Abstract
Introduction
Health and health care inequities are persistent and pervasive across a wide range of conditions and outcomes. Racism is recognized as a root cause of racial health inequities. 1–3 Structural racism is embedded in systems, laws, policies (both written and unwritten), and entrenched practices and beliefs that produce, condone, and perpetuate widespread unfair treatment and oppression of people of color, leading to adverse health consequences. 4 Eliminating health and health care inequities requires a structured, intentional approach with engaged leadership and strategic alignment, to build capacity for change.
Anti-racism training for health care professionals has been recommended as one path to advance health equity 3,5 although evidence is lacking for what anti-racism training modalities have shown effectiveness. Some institutions have introduced curricula or workshops on structural racism for health professions students and clinicians. 6–11 Evidence suggests that such training is beneficial. 12,13 However, notable gaps remain in the literature. First, relatively few anti-racism interventions have been implemented and evaluated, and most existing efforts focus on clinicians, trainees, and students within academic medical education systems. 14–16 A 2021 review by Hassen et al. of anti-racism interventions in health care settings found that only 5 of 37 articles presented interventions that were evaluated or in the process of being evaluated, and all were in outpatient settings. 17 Second, few interventions have been designed to promote structural or systems-level change to address racism. 17 Notable exceptions include Mass General Brigham, 18 University of Pennsylvania Health, 19 and Boston Medical Center, 20 each of whom has engaged in system-level strategies to address racism.
Addressing these gaps is essential because patient care and outcomes are shaped not only by clinicians, but also by operational and administrative leaders who make up the broader ecosystem in which care is delivered and patients’ experiences and outcomes are shaped. This paper describes how an inaugural health equity department within an academic health system built capacity to dismantle racism, highlighting key strategies, challenges, and lessons learned. The work provides a potential model for other health systems seeking to advance health equity.
Methods
Setting
University of California San Diego (UCSD) Health, the care delivery arm of an academic health system with 14,000 employees, collaborates closely with the UCSD Schools of Medicine, Public Health, and Pharmacy. In response to student advocacy during the coronavirus disease 2019 pandemic and the murder of George Floyd, an anti-racism task force was launched in 2021 with representation from the health system and all three schools. In 2022, the Department of Health Equity was established, led by a physician and nationally recognized health equity researcher (first author, C.W.C.) who reports directly to the Chief Executive Officer.
Overview
We conducted a series of activities to build capacity to address structural racism guided by Dr. Camara Phyllis Jones’ “National Campaign Against Racism,” which emphasizes three tasks: (1) name racism, (2) identify how it operates, and (3) organize and strategize to act.
14
Name racism: Racism is defined as a system of structuring opportunity and assigning value based on the social interpretation of how one looks (what we call “race”) that unfairly disadvantages some individuals and communities, unfairly advantages other individuals and communities, and harms everyone through the waste of human resources.
21
Identify how racism operates: Racism operates through structures, policies, practices, norms, and values, which are elements of decision-making and create opportunities for intervention.
Organize and strategize to act: Establishing structures and partnerships to sustain anti-racism action.
Rationale
Our content and modalities drew upon prior research and expert recommendations showing that:
Racism, not race, drives racial health inequities; yet, it is rarely named in medicine or medical literature.
22,23
Most health systems lack education and training for its staff on the impact of racism, despite available curricula and educational tools education.
6–8,12,15,29
Anti-racism training has demonstrated value,
12
particularly when it incorporates facilitated discussions on race and racism.
16
Activities
Figure 1 provides a timeline and overview of activities.
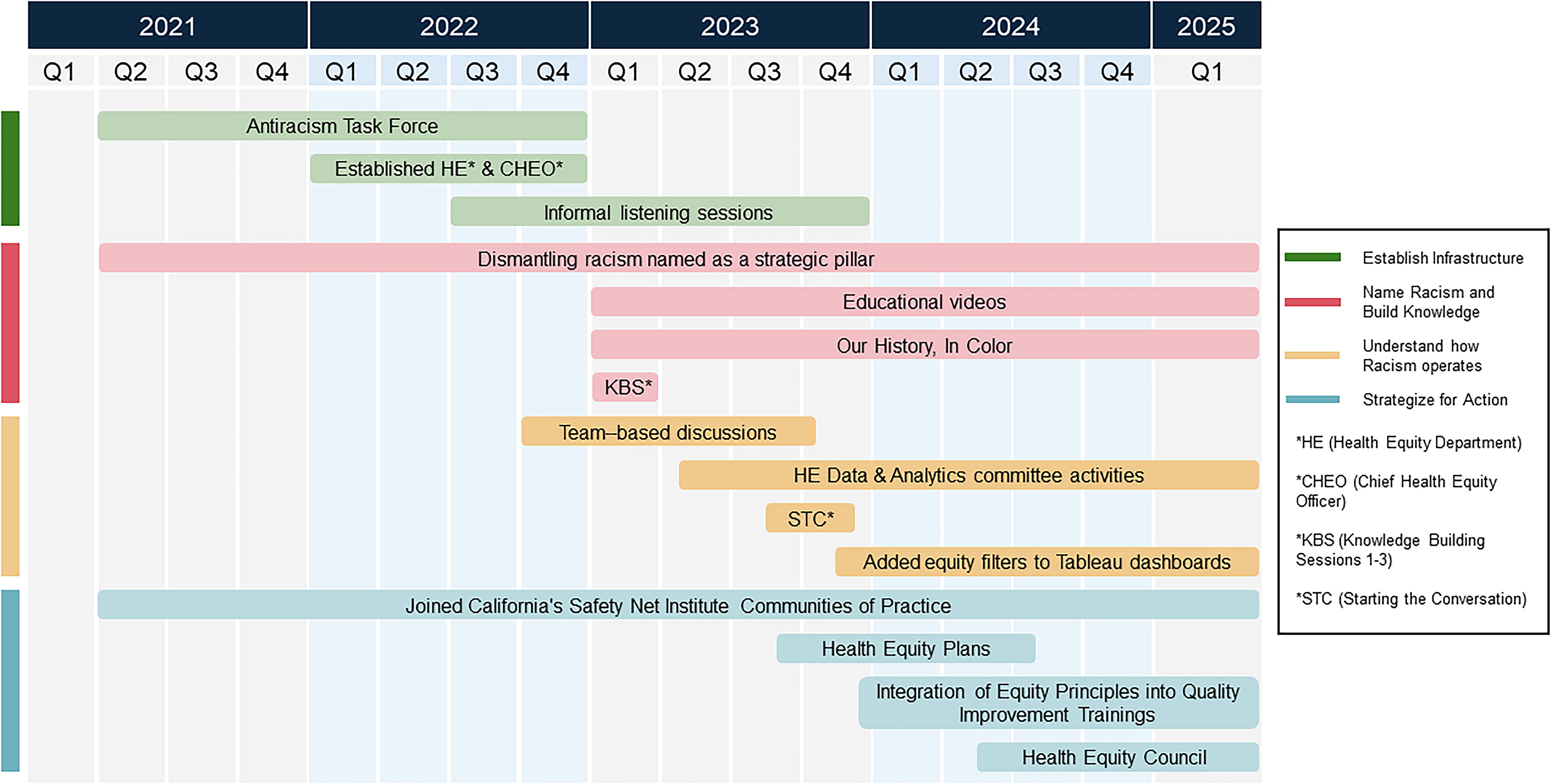
Overview of capacity-building activities.
Our efforts were designed to: 1 educate and build skills, 2 shift perspectives, 3 build collaborative partnerships, and 5 influence policy. To achieve these aims, we used multiple modalities, including didactic teaching, experiential learning, video messages, newsletters, facilitated group discussions, action planning, policy development, and participation in a racial equity community of practice.
Results
Naming racism and building knowledge
UCSD Health named “Dismantling Structural Racism” a strategic priority, embedding it into the organizational framework alongside core goals for quality, experience, culture, access, and efficiency. We used Dr. Jones’ definition of racism 21 to guide our work.
Recommendations from the anti-racism task force that preceded the health equity department, and informal listening sessions with leaders and staff, confirmed the need to begin with education on structural racism and its impact on health and health equity.
Knowledge building sessions
The health equity team facilitated three 90-min knowledge-building sessions held over zoom and recorded. Topics covered included racial equity and anti-racism, creating brave and accountable spaces for racial equity dialogue, and unpacking power, privilege, and bias. Each session included didactic content and break-out groups for discussion.
An average of 382 leaders participated in the sessions, with postsession survey response rates exceeding 80%. These sessions were well-received: 90% of respondents reported shifts in previously held views, and 97% said they would recommend them. Representative comments highlighted the sessions’ value and the need for continued skills building and leadership modeling.
“EXCELLENT training. One of the best I have seen. Inclusive, fun and worth repeating and sharing as often as possible, to the widest audience.”
“I appreciated the breakdown between safe, brave, and accountable spaces. I think the way it was explained makes it more actionable for folks.”
“While I appreciate the material and presentation, I do not feel I can take action. More time and training would be needed. I feel too under informed at this point but more training is going to help but also how to bring this to my team would also help.”
“Great information. Loved the sessions. I didn’t see my CAO [Chief Administrative Officer] attending and noticed she was in the room next to me having meetings. I think this should be required for everyone to attend.”
Engagement in the knowledge-building sessions was incorporated into the fiscal year 2024 leadership incentive plan, making participation a defined expectation for all director-level and above leaders.
Video education series
To reinforce key concepts from the sessions, the health equity team produced short (<6 min) practical, action-oriented videos, which were posted on our departmental website and directly shared.
Topics included:
Why we Lead with Race. What is Structural Racism. 4 Strategies to Dismantle Structural Racism. Understanding Privilege. Unpacking Privilege, Power Hierarchies, and Bias. How to Talk About Race at Work. Creating Brave and Accountable Spaces for Racial Equity.
Our history in color
To challenge norms, counter biases, and foster a more inclusive culture, the health equity team launched a monthly series called Our History in Color—a collection of one-page spotlights highlighting the contributions of people of color to medicine and science. Shared to all-staff across the health system and the three health professions schools, the series has featured 33 individuals to date (see example- Fig. 2). Though no formal evaluation is conducted, this initiative has received much unsolicited positive feedback. Team members have expressed appreciation for seeing individuals with whom they identify and have found the content culturally affirming and educational. Representative comments include:

Our history, in color.
“Thank you for this remarkable moving story, and for sharing our hidden histories of injustice and discrimination. Knowing and remembering facilitate change.”
“I LOVE this publication. I learned so many wonderful things. Thank you, Health Equity team, for all you do to help our community learn and grow.”
“I really wanted to thank you for writing this issue of Our History In Color. Both my partner and I are Asian American and in the field of psychology. We didn’t know this story behind AAPA, about the Sue’s, and found this both moving/encouraging and bittersweet-that even with the time that’s passed, we often have felt the weight about the limited research and mental health resources for racio-ethnic minorities and specific groups, i.e., Asian Americans. The journey continues, and the story matters.
Policy development
Finally, based on recommendations from the anti-racism task force, the health equity team led the development of a new health system policy, including the development of educational materials on how to handle patients who display racist and discriminatory behavior toward staff.
Understanding how racism operates
Facilitated team discussions
To complement didactic knowledge-building sessions, a member of the health equity department facilitated over 25 primarily in-person (though several occurred via zoom) team-based discussions, lasting 90 min, based on Dr. Camara Jones’ TEDx talk, Allegories on Race and Racism. 30 The talk contains 4 allegories (stories): (1) Japanese lanterns: Colored Perceptions (of race); (2) Dual Reality (of privilege): A restaurant saga 31 ; (3) Levels of racism: a gardener’s tale 32 ; and (4) Life on a Conveyor Belt: Moving to action. 33
After watching each allegory, the facilitator stopped the video and guided participants through structured questions, encouraging personal reflection and identifying examples of where they perceived racism within the health system. Commonly cited examples related to medicaid acceptance, diversity in leadership, language access and interpretive services for limited English proficiency patients, and inclusivity of marketing materials. These 90-min sessions used an engaging, innovative format to deepen understanding, improve comfort, and build skills needed to discuss racism-key for dismantling structural racism. Approximately 1,800 individuals participated; 92% reported feeling comfortable to engage in the discussions, and 89% would recommend the activity.
Participant comments highlighted the sessions’ impact, emphasizing the importance of engaging in discussions about racism, authentic leadership support, psychological safety, and trust among coworkers when discussing sensitive topics.
“Extremely engaging and informative session. At no point did it feel forced or difficult. Expectations and norms were set and allowed participants to thoroughly feel safe to engage. Best session I have ever attended in this subject matter.”
“As an employee who believes in the strategic mission of UC San Diego Health to break down systemic racism, I was disheartened to hear the various views from organizational leaders that are in direct opposition of these goals. Clearly, the health equity team needs more support to truly integrate structures and processes and a mechanism to overcome internal barriers otherwise the well-intended program will become a victim of the systemic racism they hope to address.”
“I would like this to be a more frequent conversation. We have had a lot of experiences in our department within my 8 years here however, this is the first time we have had a conversation. I would also like the university to identify ways to get all staff to participate.”
“Very uncomfortable and not appropriate conversation for the workplace. I did not feel like it was a “safe place to speak openly.” Why should I open up when anything I say in this department is held against me. The morale and trust between employees and management needs to be stronger in order for this activity to be a successful interaction.”
Starting the conversation
In response to feedback that the facilitated discussions on structural racism did not allow enough time to explore its links to bias, team communication, and patient interactions—and at the Radiology service-line director’s request—the health equity team developed Starting the Conversation, a 6-week pilot within Radiology. The program combined didactic learning and coaching, providing participants with practical tools and skills to address racism as a health barrier. It included four group sessions with all eight team members together and optional individual sessions for people seeking additional support to apply these concepts in practice. Three people choose to also have individual sessions. The learning objectives are outlined in Table 1.
“Starting the Conversation” Pilot Program Sessions and Learning Objectives
Pre- and post-program evaluations from eight pilot participants showed increases in those strongly agreeing they:
Understand the impact of racism and bias on health outcomes (from 50% to 85.7%) Recognize their own biases and how they influence health care decisions (from 25% to 85%) Feel confident discussing issues related to racism, bias, privilege, health equity, and health disparities (from 12.5% to 28.5%).
Open-ended feedback reflected the program’s value, usefulness of tools, benefit of coaching, and a desire for more practice time.
“Overall, the content and execution were on point, I do believe we all grew a little through this work.”
“Provided great tools to help engage and navigate these conversations.”
“Coaching has helped improve framing discussion in a way that puts the audience at ease and makes it easier to relate to.”
“May have been helpful to practice scenarios in small groups and receive real time feedback on what worked/what could be improved.”
Health equity data and analytics committee
Data and stories offer critical insight into how racism operates. To support this, we prioritized building a data infrastructure to identify health inequities key metrics for tracking progress in advancing health equity. We established a Health Equity Data and Analytics Committee to lead the development of this infrastructure. This committee provides strategic direction, oversight, and visibility into equity indicators within our patient population. This committee developed data standards, mapped national sexual orientation and gender identity (SOGI) standards for demographic data collection to our data capture tools, and made improvements to race, ethnicity, and SOGI categories in our electronic health record (EHR). We also made changes within our EHR to improve capture and tracking of preferred language and interpretive services use.
The committee enhanced our quality, safety, and patient experience dashboards by adding equity “filters,” to enable data stratification. The Chief Health Equity Officer introduced the REAL GAPSSTM—Race, Ethnicity, Age, Language, Gender, Ability, Payor, Sexual Orientation, and Social needs and resources Framework for Health Equity—to help team members consider multiple inequity indicators. We also developed new equity dashboards, including one for Social Determinants of Health that tracks screening completions, domain-specific completion rates, and the percentage of patients at risk for unmet social needs. Additional dashboards for readmissions, discharges, and patient experience enable us to monitor and address inequities over time.
Strategizing for action
To advance racial health equity and address inequities, we conducted several activities.
Racial equity community of practice
Five representatives from UC San Diego Health—including staff from the Health Equity, Quality, and Information Services departments participated in the California Health Care Safety Net Institute’s inaugural 18-month Racial Equity Community of Practice (CoP, 2021–2023), with over 70 leaders across 12 public health systems. Grounded in the Leading for Equity Framework and Liberatory Design, 34 the CoP used action learning and coaching from the National Equity Project. Our team’s initial readiness assessment of our CoP team revealed knowledge gaps around structural racism and its connection to health equity, prompting a stronger focus on education at our institution.
Now in its second 18-month cycle (2023–2025), the CoP emphasizes implementation. Teams identify specific equity challenges, collect data, and design solutions. Bi-monthly action-learning sessions are supplemented by cross-system interest groups focused on equity in quality and language access.
Health equity plan development
As part of the FY24 leaders’ incentive goals, each leader created a department-specific health equity plan. A total of 174 plans were developed with coaching support from the health equity team, using a recognized equity framework 35 aligned with Lean Six Sigma’s A3 problem-solving method. 36 The health equity team reviewed all plans, identified key themes, and mapped them to organizational goal areas—quality, access, efficiency, culture, and experience. We shared written summaries and insights with executive leaders and presented them system-wide.
Top cross-cutting themes included:
Improving language access Expanding care for vulnerable populations (e.g., immigrants, refugees, low-income-groups) Addressing social determinants of health Enhancing equity in leadership and professional development opportunities
Review of the plans revealed that many leaders struggled to articulate clear problem statements and understand root causes from an equity lens, limiting their ability to identify effective and sustainable solutions. In response, the Health Equity and Transformational Health teams partnered to integrate equity principles into the organization’s quality improvement trainings. Health equity staff co-facilitated system-wide workshops that guided leaders through structured problem-solving and process improvement methods to address inequities in patient care. This approach supports leaders in building requisite skills to develop equity-centered solutions and improve health for all patients. The review also surfaced opportunities to identify system-level equity priorities and strengthen the infrastructure needed to advance health equity.
System-wide health equity council
Building on these insights, we launched a Health Equity Council to set health equity priorities, advise on metrics, monitor progress, and remove barriers. Co-chaired by the Chief Health Equity Officer and Chief Quality and Safety Officer, the Council includes 26 members from 20 departments, service lines, and centers across the health system and health professions schools. The Council, which meets monthly, reports to the Executive Committee of the health system and provides ongoing guidance on advancing health equity across the system.
Discussion
Challenges and solutions
A key challenge we faced was limited and often inaccurate understandings of racism among leaders and staff. Many viewed racism solely as interpersonal—typically between Black and white individuals—and questioned its relevance in a politically progressive state like California. This narrow view obscured racism’s broader impact on health inequities. To address this, the health equity team provided education on the three levels of racism: structural, interpersonal, and internalized. 32 By emphasizing structural racism 37 —embedded in systems, policies, and practices and lacking a clear perpetrator—the team shifted conversations from individual behaviors to systemic barriers. This reframing reduced the shame and blame often associated with discussions of interpersonal racism and enabled more productive dialogue about change.
Another challenge emerged when untrained leaders chose to facilitate their team’s “Allegories on Race and Racism” discussions instead of using experienced health equity facilitators. Though infrequent, these discussions went poorly. Some staff, especially from minoritized groups, felt unheard, while others felt blamed or shamed. Debriefs revealed that these facilitators: dominated discussions, strayed off-topic, failed to read the “community agreements” and focused on interpersonal rather than structural racism—often triggering negative emotional reactions and undermining psychological safety.
To address this, the health equity team debriefed with the facilitators and offered psychological support to team members negatively affected by these sessions. We also developed a facilitator training specific to this activity, which was required for leaders wishing to lead these discussions. In addition, a skilled facilitator from the health equity team was available to co-lead the discussions.
A key ongoing challenge is sustaining long-term commitment to anti-racism amid competing priorities and a shifting political climate. Like many systems, UCSD Health faces increasing patient volumes, clinical space constraints, and low reimbursement for publicly insured patients. Financial pressures are intensified by proposed changes to Medicaid/Medi-Cal and research funding—factors that strain leadership bandwidth and force decisions that may result in a de-prioritization of some equity efforts.
National attacks on diversity, equity, and inclusion (DEI) efforts have further complicated the work. Political rhetoric and federal actions that conflate DEI with health equity have caused some institutions to pause or abandon efforts entirely. The growing reluctance to use terms like “racism” and “equity” in federally funded settings also undermines progress. Still, sustained leadership engagement remains essential to dismantle the structural barriers that prevent equitable health outcomes.
In response, UCSD Health implemented several strategies to maintain focus. First, the executive team has reaffirmed its commitment to addressing systems, policies, and practices that contribute to inequitable patient outcomes. Equity filters are integrated into quality and patient experience dashboards, and equity metrics are tracked to facilitate quality improvement.
Second, ongoing education on structural and social drivers of health is embedded into annual orientation and coaching for employees and leaders, reinforcing equity as foundational to our mission.
Third, the health equity team has developed communication guidance to help leaders articulate the organization’s health equity efforts. This messaging is reinforced via CEO-led town halls for all staff, and meetings with health system leadership.
Finally, UCSD Health tracks and shares its progress. Annual health equity reports, internal updates, and regular recognition of individuals and teams advancing this work help to sustain engagement and accountability.
Limitations and strengths
We lack outcome data demonstrating reductions in health inequities. Our activities were not part of a single intervention that can be evaluated holistically or formally. However, the content was evidence-based and aligned with recommended best practices. We followed recommended strategies by: (1) incorporating explicit, shared anti-racism language; (2) securing leadership commitment to organizational change; (3) using experienced facilitators to conduct training; and (4) linking anti-racism work to broader systems of power. 5,17
Moreover, no consensus currently exists on the most effective methods, tools, or outcomes for evaluating anti-racism initiatives 15 and there is no established “gold standard” for delivering such education. Our anti-racism education and training methods (e.g., facilitated discussions, monthly series) were chosen to maximize feasibility, impact and team member engagement.
A major strength was our system-wide approach that engaging both clinicians and non-clinicians using multiple modalities. Similar to us, other health systems have implemented anti-racism education and efforts to promote organizational culture change. 18–20 Some have used Dr. Camara Jones allegories on race and racism and offered optional facilitated discussions for their staff 18 and have leveraged the power of stories to engage their staff in dialogue about racism. 19 One organization also developed a patient code of conduct (similar to the policy we developed) that outlines how to manage patients who display racist, discriminatory, or hostile behaviors toward staff. 18 Another health system also enhanced their data infrastructure to identify and address disparities in patient care outcomes. 20 While other health systems have undertaken important efforts to address racism as a structural determinant of health, UCSD Health’s approach is unique in its organization-wide scope and the breadth of activities implemented to build knowledge, skills, and accountability to confront racism across multiple levels of the organization.
Conclusion
UCSD Health demonstrates that building health system leaders’ capacity to address structural racism- through education and skill-building, action planning, and perspective shifts/culture change-can yield measurable benefits and add value, as reflected in process outcomes and participant feedback. Success factors include naming racism explicitly as an organizational priority, building supportive infrastructure, holding leaders accountable, using varied educational approaches, and leveraging data for ongoing improvement. With an experienced team applying theory and evidence, UCSD Health offers a replicable model grounded in practical, sustainable, and system-integrated strategies.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
Funding Information
No funding was received for this article.
Appendix
Abbreviations Used
