Abstract
Introduction
The current model of perinatal care in the United States is inadequate to meet the needs of pregnant capable individuals and is in crisis; it can neither sufficiently avert harm, nor does it promote joy and connection. The failures of the current system are disproportionately borne by Black and Indigenous communities as demonstrated by deep inequities in maternal morbidity and mortality in the United States, which continues to experience the highest rates of maternal mortality compared “to” similar countries. 1 Most of these maternal deaths are preventable. 2–4 These same communities are incredible sources of wisdom, insight, resilience, community, and joy. There are deep structural and social inequities, including racism and other forms of discrimination, that impact access to, utilization of, and quality of perinatal care. 5 Perinatal care models must be reimagined to meet the critical health needs of pregnant capable individuals and their families, address the root causes of inequities, prevent adverse outcomes, and create opportunities for joy and thriving. Recognizing the urgency of this perinatal crisis, the first Georgetown University Reimagining Perinatal Care to Promote Health Equity Symposium was held on March 19–20, 2025 in Washington, DC and convened over 50 perinatal health, policy, and reproductive justice experts.
The symposium fostered collaboration between early-career educators, scholars, researchers, legal experts, clinicians, and colleagues from community-based organizations with a focus on leveraging their expertise and radical imagination to reimagine and strategize on transformative models of perinatal care. The symposium consisted of a public panel discussion and collaborative small groups with plans for dissemination via this Special Issue. Amid the constrained financial and charged sociopolitical backdrop of Washington, DC, we cultivated an environment of collective care and mutual respect, developed trust and new relationships, and initiated conversations to spark future collaboration opportunities that advance perinatal health research.
The 2025 Georgetown University Symposium revealed both challenges and opportunities for community-driven, innovative solutions to developing and implementing a transformative model of perinatal care. Rather than accepting incremental reform to a fundamentally broken health care system, panelists envisioned this opportune time for a radical reimagination rooted in reproductive justice, health equity, interdisciplinary engagement, and community support. We identified next steps for moving out work forward that includes the concurrent urgent needs to work within existing systems and frameworks, and to move beyond limiting paradigms (See Fig. 1): (1) adapt existing systems while reimagining what is possible, (2) engage in policy advocacy alongside community organizing, (3) integrate individual healing practices within larger systems of care and communal healing, (4) shift from models of shared ownership to liberatory frameworks, (5) expand beyond collaborations and committing to mutuality and care, (6) create sustainable infrastructures and build trustworthy and restful spaces, (7) labor together while also rooting out efforts in joy, resilience, and healing traditions, (8) move from community partnerships to community led endeavors that center the wisdom of lived experiences. These actions can collectively transform our perinatal care system to one that centers on human dignity and the right to thrive.
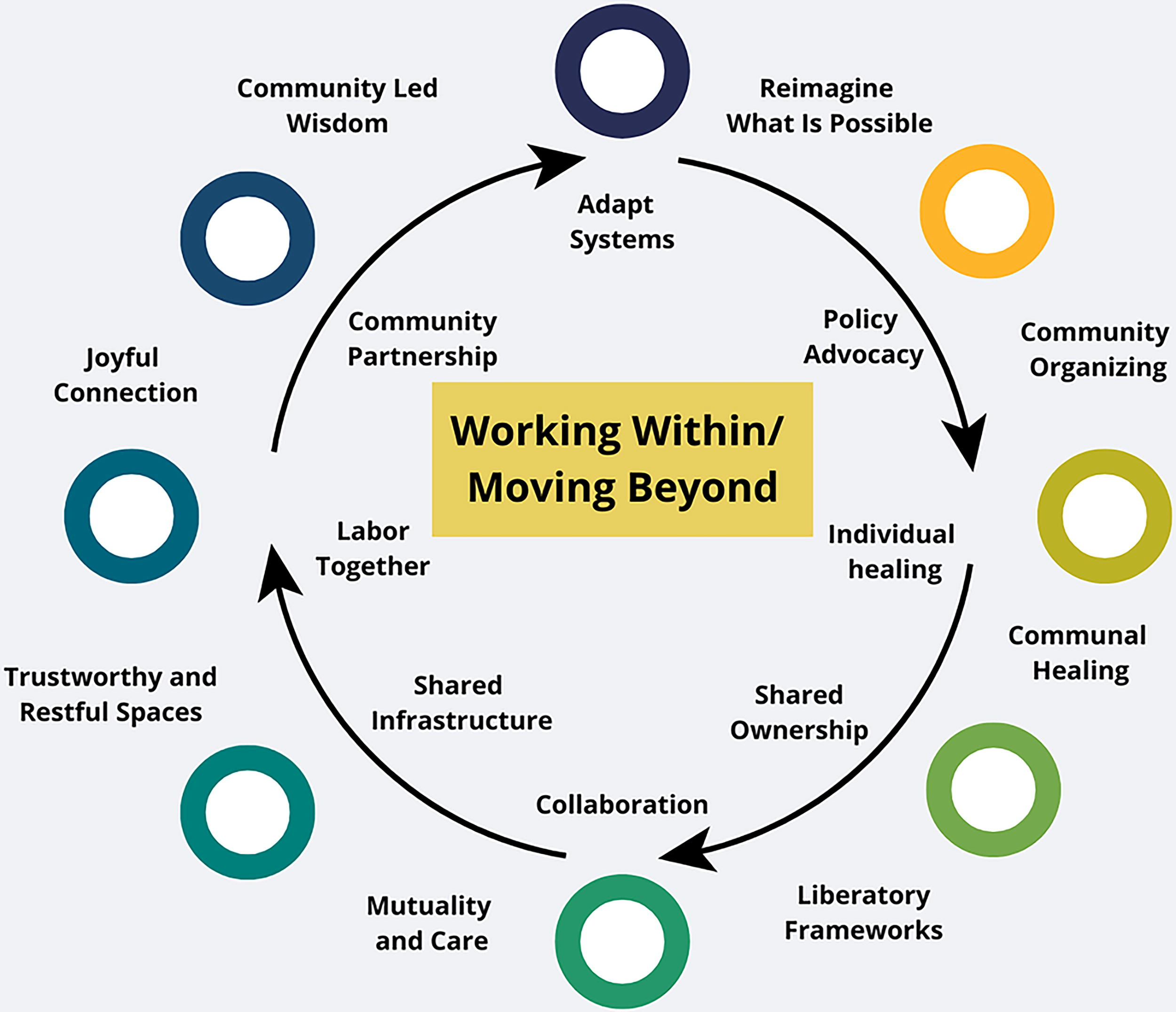
Framework for working within/moving beyond.
We wanted to ensure that the generated ideas, content, and collaborative work would be widely disseminated. In collaboration with Dr. Monica McLemore, Editor in Chief of Health Equity, we proposed a special issue that was enthusiastically welcomed. Our team of seven guest editors across medicine, midwifery, and public health have worked to shape an issue that bridges research, practice, policy, and the arts to promote progress toward advancing equity in perinatal care. The Health Equity special issue on Reimagining Perinatal Care to Promote Health Equity features many original and review articles, perspectives, and creative submissions.
Panel Discussion: Reimagining Perinatal Care to Promote Health Equity
The panel discussion brought together two health equity researchers, an obstetrician/reproductive justice advocate, and a reproductive justice legal expert to address an uncomfortable truth: our current perinatal health services are failing communities most in need, who continue to face unprecedented threats. The 90-minute hybrid (in-person and Zoom) panel discussion was moderated by Dr. Christina X. Marea (Assistant Professor, Georgetown University Berkley School of Nursing) and included Dr. Rachel Hardeman (Center for Anti-Racism Research for Health Equity, University of Minnesota), Dr. Natalie Hernandez-Green (Center for Maternal Health Equity, Morehouse School of Medicine), Dr. Jamila Perritt (Physicians for Reproductive Health), and Professor Sonia Canzater (O’Neill Institute, Georgetown University Law). The panel discussion is summarized across six themes found in Table 1.
Themes from Panel Discussion on Reimagining Perinatal Care to Promote Health Equity
The historical and community context of care
Dr. Jamila Perritt, president and CEO of Physicians for Reproductive Health, began with a foundational challenge to how we understand health care’s relationship to history and community. Her opening remarks reminded the audience that the United States has a “deep commitment to an ahistorical context.” She shared how dangerous pretenses that past and present exist in isolation is a systemic problem that contributes to perinatal health inequities.
Dr. Perritt argued that this disconnection is deliberate. It enables medical education to systematically separate practitioners from the communities they serve. Students move through years of training (undergraduate studies in one city, medical school in another, residency elsewhere) without ever being required to understand the communities they will serve. It prevents them from grappling with the complicated relationships those communities have with medical institutions. The result is a health care system that treats patients as isolated individuals and health care providers as assets, disconnecting both groups from the support systems that sustain them.
Community-centered innovations
Dr. Natalie Hernandez-Green, Associate Professor and Founding Executive Director of the Center for Maternal Health Equity at Morehouse School of Medicine, presented solutions and shared a hopeful vision of how community-engaged clinical care and research can improve care and confront structural inequities. Dr. Hernandez-Green works in Georgia where many women and birthing individuals lack access to reproductive health care and maternal mortality rates remain among the nation’s highest. The Center’s work is anchored in a set of guiding principles that redefine maternal health equity. First, it adopts a life course perspective, emphasizing that achieving equity requires interventions that begin well before pregnancy and extend across the lifespan. Second, it is rooted in co-creation with communities, ensuring that those most affected, particularly Black women and birthing individuals, shape the solutions designed to serve them. This participatory approach disrupts conventional research paradigms that have too often excluded or exploited marginalized populations.
Most significantly, the Center’s VOICE program (Verbalizing Options to Integrate Community Peri and Postnatal Support and Resources to achieve Equity) trains women from affected communities as doulas, patient navigators, community health workers, and lactation peer support specialists. 6 By recognizing this work as skilled labor and ensuring fair compensation, the program promotes both workforce development and economic empowerment. Graduates connect families to culturally relevant, vetted resources that address social determinants of health such as housing, food security, and transportation. This comprehensive approach reflects a broader paradigm shift in maternal health that situates health equity within the social, structural, and economic realities that shape individuals’ lives. Dr. Hernandez-Green emphasized that equitable care requires systems that value community expertise, dismantle structural barriers, and treat social conditions as integral to health and well-being.
Legal and policy challenges
Professor Sonia Canzater from Georgetown Law Center’s O’Neill Institute brought attention to the rapidly shifting legal landscape affecting reproductive health care. Her remarks highlighted how policy changes create real-time challenges for clinicians trying to navigate an increasingly hostile environment, and put patients at risk. The rollback of affirmative action in academic admissions threatens to reduce diversity in health profession training programs, potentially limiting the number of health care clinicians who return to serve marginalized communities. Equally concerning are recent changes to federal protections for reproductive health care clinicians. The revocation of executive orders that clarified clinicians’ protections under emergency care laws Emergency Medical Treatment and Active Labor Act has created deliberate ambiguity, upending the provision of reproductive health care through uncertainty rather than outright prohibition. Yet, Professor Canzater identified an opportunity within the crisis. Professional organizations can step up to provide guidance and support for their members, creating spaces for community and protection.
Structural racism as root cause
Dr. Rachel Hardeman, founding Director of the Center for Antiracism Research for Health Equity at the University of Minnesota, brought the conversation full circle by naming structural racism as the root cause of health inequities and illuminating the systems that sustain them. Rather than centering despair, Dr. Hardeman framed the conversation as grounds for hope shaped by radical imagination—a concept rooted in Black radical thought and the visionary work of scholars such as Robin D.G. Kelley—the courage to ask “what if” in spaces where power can be leveraged for transformation. She challenged the group to think beyond traditional academic and clinical boundaries, urging attention to how state-level policy, financial innovation, and community partnership can collectively advance justice-centered care. In doing so, Dr. Hardeman reminded the audience that antiracism in health is not only a research agenda but a moral mandate—one that demands both imagination and action.
The question of power
The symposium’s panelists addressed questions of power—how it operates, who holds it, and how it must be redistributed for meaningful change to occur. Their response centered on how health service provision’s power dynamics are built into everything from research questions to patient positioning during examinations, yet these dynamics are rarely acknowledged or discussed. The conversation revealed different approaches to engaging with institutional power. Some panelists spoke of working “inside” systems while others focused on community organizing and movement building.
Redefining access and care
One of the symposium’s most important contributions was its insistence on redefining fundamental concepts like “access” and “care.” As multiple panelists noted, having insurance does not equal having access to care. This was likened to having access to a building’s roof—it could mean having stairs unlocked or being handed “a grappling hook and some bungee cords.” Both technically provide access, but only one is meaningful. In Washington DC, one of the most insured cities in the country, the closure of maternity hospitals east of the Anacostia River means that geography, not insurance status, determines whether residents can actually receive care when and where they need it. True access is being able to walk down the street to see a clinician who knows you, your family, and your community context. It means caring relationships built over time, rooted in community understanding rather than brief clinical encounters focused on efficiency and volume.
Panel discussion conclusion
The panel discussion concluded with panelists sharing beautiful examples of the work that sustains their vision for transformed health care. To achieve this vision, they recommended recognizing the expertise of our communities and valuing their lived experiences as legitimate data. Supporting the next generation of reproductive justice advocates is also essential to mitigating threats to health care access.
Proceedings from Collaborative Writing Groups
In convening 50 health equity scholars, clinicians, and community activists, we established eight collaborative writing groups. Each group consisted of six to eight participants who shared ideas and expertise surrounding their topic of interest (see Table 2) and developed a plan for disseminating results from our discussions and further research and collaboration opportunities. The topics of interest were selected based on: (1) participant expertise, (2) greatest potential for transformation, and (3) an intentional expansive approach to transforming perinatal care consistent with the reimagining theme.
Collaborative Writing Group Topics
Applying midwifery philosophy to research: Implications for equity
Led by Christina X. Marea and Mimi Bhatt, and included Katie DePalma, Melicia Escobar, and Katie Page.
The idea of midwifery as a scientific discipline sparked our collaborative writing group’s dialogue on midwifery-led research and the application of midwifery philosophy to research design, methods, analysis, and dissemination. The application of midwifery philosophy to research represents a fundamental shift from traditional biomedical research paradigms toward more holistic, relationship-centered approaches to knowledge generation. Midwifery research embraces a “doing with,” approach which emphasizes partnership, witnessing, and accompaniment throughout the research process. This approach recognizes that pregnancy and childbearing are normally physiological processes with profound personal and communal meaning. A midwifery philosophy challenges researchers to re-evaluate default assumptions of normalcy while maintaining vigilant attention to deviations, mirroring the midwifery practice of judicious application of our expertise. The research design must honor multiple ways of knowing and being, while embracing embodied inquiry and community-defined outcomes. Midwifery philosophy emphasizes relational continuity, requiring researchers to invest time in knowing and being known by participants, creating space for radical imagination and acceptance of socially sanctioned expressions of both joy and pain. We discussed how this approach is inherently emancipatory, recognizing the interconnection between health and social experiences while focusing on individual and community resilience. Critical to this framework is the integration of reproductive justice principles, intersectionality, and decolonizing methodologies. We seek to pursue research that addresses the vertical integrity (or lack thereof) of existing systems of care while maintaining laterally oriented power dynamics that honor participant self-determination and cocreation.
Centering liberation-partnering across the African diaspora to reimagine perinatal care
Led by Lauren Arrington and Kanika Harris, and included Tanay Lynn Harris, Natalie Hernandez-Green, and Ebony Marcelle.
The centering liberation interest group is advancing collective action to confront the unjust and preventable perinatal morbidity and mortality disproportionately affecting Black communities globally. Our collaborative writing group focused on the group care model as an effective platform for liberatory care, which recognizes that fighting injustice is a necessary step to achieve health and well-being. 7 Drawing lessons from movements that circumvent oppressive paradigms, we amplify the wisdom, expertise, and dedication of the global majority. These movements include codevelopment, South-to-South partnerships, and African diasporic collaboration. 8–10 Our work is grounded in a radical reimagining of a just and liberated future and seeks to establish a liberatory framework for antioppressive, anticolonial, and antiracist collaboration to improve perinatal care and outcomes for Black birthing individuals. While not all members were able to attend the symposium, the voices and commitments of colleagues, including Nafisa Jidawi, Rose Aka James, Jyesha Wren, and Debrah Lewis, were present in spirit and continue to guide this collective effort.
Abortion access post-Dobbs
Led by Meghan Eagan-Torkko and Monica McLemore, and included Mara Evans, Karen Grace, Signey Olson, and Rebecca Reingold.
In the aftermath of the overturning of Roe v. Wade, our collaborative writing group’s conversation focused around the power dynamics of bodily autonomy, particularly in light of the historically “normal” role of midwives in providing abortion care. Rather than framing this shift solely as a change in medical practice, dialogue explores it as a strategic reassertion of power structures that have long perpetuated systemic harm. Specifically, there are opportunities to use this destabilization of harmful systems to re-establish a person-centered, community-based approach to comprehensive sexual and reproductive care, including abortion. We examine the historical displacement of midwives and the deliberate centering of physicians as gatekeepers of reproductive care. By illuminating these dynamics, we open a broader conversation about the path forward and the future of liberatory, community-centered models of care.
Additional conversations were specifically grounded in workforce initiatives and institutional challenges in balancing care provision and training needs. This group prioritized team-based care and innovations and recommended that transdisciplinary roles be developed that include community members and individuals served as patients.
Legislative, policy, regulatory, and payer issues in perinatal care
Led by Emma Clark and Sonia Canzater, and included Lastacia Coleman, Allyson Crays, Kionna Henderson, and Kathryn Lee.
As our understanding of perinatal care interventions that advance health equity continues to deepen, the accompanying legislative, policy, regulatory, and payer frameworks must evolve in tandem. These frameworks are often the determining factor in whether promising interventions—such as doula support, birth center care, or equitable reimbursement for midwifery services—become widely available and transformative for health outcomes. Without enabling environments, even the most efficacious interventions face significant barriers to adoption and scale. Building such environments requires a strong evidence base that speaks directly to policy makers, regulators, and payers, including Medicaid and Medicare, to justify investment through mechanisms such as policy change, regulatory reform, or financial coverage of services. Yet, the complexity of health systems can make generating this type of actionable evidence particularly challenging, especially when it must be framed to overcome perceived risks or disruption of the status quo. Our collaborative writing group explored how this barrier might be addressed by leveraging large existing datasets [e.g., Centers for Disease Control’s WONDER, Pregnancy Risk Assessment Monitoring Systems (PRAMS), and National Vital Statistics System, the Centers for Medicare and Medicaid Services Transformed Medicaid Statistical Information System (T-MSIS) Analytic Files] to examine state-level variations in the adoption of promising or proven perinatal interventions and their association with key outcomes. For example, analyzing the impact of Medicaid reimbursement parity for certified nurse–midwives and certified midwives relative to physicians in birth services provides a powerful opportunity to demonstrate both feasibility and correlate it with specific birth outcomes of interest like low-risk cesarean births among nulliparous individuals. Ultimately, this evidence-driven approach can inform the scale-up of equity-focused solutions that reimagine perinatal care for the future.
Dyadic postpartum models of care
Led by Ashley Gresh and Noelene Jeffers, and included Erica Eliason, Laura Lazzari, Michelle Roett, Karen A. Scott, and Sola Stamm.
The postpartum period is an opportune time to address acute complications associated with pregnancy and birth and to partner with patients and their given and chosen families in establishing the foundation for long-term health and well-being through preventive support and care. Our collaborative writing group discussed the immense physical and mental health risks in the first 12 months postpartum. Over half (53%) of all maternal deaths in the United States occur between 7 and 365 days postpartum, making the postpartum period one of the most dangerous phases of the perinatal continuum. 5 Unresolved pregnancy complications such as hypertensive disorders of pregnancy, gestational diabetes, and mood and anxiety disorders are likely to persist past 12 months postpartum if not effectively addressed and supported by sustained, coordinated care beyond the postpartum period. 11,12 The postpartum period is a critical window of time in which short-term recovery intersects with long-term health trajectories. Our discussion centered on the understanding that for many birthing individuals and families, the postpartum period is a missed opportunity characterized by low utilization, mistimed intervention, and fragmented, stigmatizing care. 13 Dyadic postpartum care models (integrating care for both the postpartum person and infant) could potentially offer a transformative approach to postpartum care; however, to date, there has not been a national landscape analysis examining implemented dyadic postpartum care models, as existing research has been limited to small-scale pilots, regional initiatives, and specific patient populations. We conceived a research study focused on understanding how dyadic care is delivered, sustained, and experienced in diverse clinical and community settings. We agreed to focus on this knowledge gap so that we can explore the breadth of approaches, identify common barriers and facilitators, and elevate the voices of patients, providers, partners, and caregivers engaged in this model of care. This comprehensive and inclusive perspective is essential to inform future policy, advance equitable models of care, and ensure that dyadic approaches are both scalable and responsive to the needs of historically marginalized communities.
Perinatal mental health: Whole person and community integrated care for screening and service delivery
Led by Rebecca Shasanmi-Ellis and Amittia Parker, and included Katie Daily, Theodora Danylevich, Mara Evans, Tanay Harris, Natalie Hernandez-Green, Roxanne Mirabal-Beltran, Bayyinah Mohammed, Charis Suh, and Veronica X. Vela.
Perinatal mental health concerns are among the leading causes of maternal mortality from pregnancy through one year postpartum. 14 Suicide, homicide, and overdose—many of which are preventable—are the primary causes of death. 15 We brainstormed ways that a reimagined approach to perinatal mental health care delivery can address maternal mortality and better align with community needs. We discussed opportunities for enhancing the standardization, collaboration, and implementation of mental health education and screening to ensure early detection and timely support. For example, what are the perspectives and recommendations of providers engaged in perinatal and pediatric care, including community health workers and doulas, regarding critical gaps in perinatal mental health care? How can whole person care (physical, mental, social, and spiritual) and engagement within communities at high risk for perinatal mental health concerns also identify these critical gaps? 16 Through narrative analysis and case study vignettes, our group began to develop recommendations for clinical practice, public health education, and policy to seek coordinated, integrated, and person-centered perinatal mental health care.
Harm reduction approaches to perinatal substance use disorder
Led by Elizabeth G. Muñoz, and included Bre Calhoun, Briana Kramer, Sara Paiva, and Nicole Warren.
Substance use disorder (SUD) disproportionately affects historically oppressed pregnant and postpartum individuals, many of whom face inadequate treatment due to stigma and discrimination. In response to the punitive policies targeting pregnant individuals that increased in number after the Dobbs decision and the broader marginalization of this population within institutional systems, their protection has become an urgent concern. 17 Notably, pregnancy remains one of the few contexts where carceral approaches are expanding instead of being scaled back. 17 During the first year after the Dobbs decision, substance use-related charges were present in the majority of cases brought against pregnant individuals, making this offense in pregnancy more common than abortion-related charges. 17 We recommended harm reduction as the best evidence-based approach to caring for pregnant and postpartum individuals with SUD. 18 We discussed the need to examine and develop evidence-based policies and guidelines with actionable strategies at the individual and system levels that promote equitable, nonpunitive care among pregnant and postpartum individuals with SUD. Immediate actionable policy and care recommendations were discussed, such as the elimination of universal drug testing during pregnancy, use of nonbiased and person-first language around substance use, and encouragement among patients with SUD to create a personal harm reduction plan.
Perinatal community-based participatory research: Moving from performative to principled
Led by Kelly Bower, Heather Bradford, and Roxanne Mirabal-Beltran, and included Jess Angelson, Alexia Dunn Amore, Kelley Robinson, Rebecca Shasanmi-Ellis, Dawn Sherman, and Ellen Solis.
Our collaborative writing group represented voices from community-based organizations (CBOs), researchers with expertise in perinatal community-engaged research (CEnR) and community-based participatory research (CBPR), and others interested in the topic. We shared our experiences in conducting perinatal CEnR as well as CBPR, the gold standard of CEnR. We lauded how CBPR study designs ensure the research benefits are adequately returned to the community, emphasize equal ownership, cocreation and learning, and actionable results to bring about social change, and can address disparities in perinatal outcomes. 19,20 However, the term CBPR has become a common buzz phrase in research, often overstating the actual level of community engagement. We discussed how some communities of study may not be served by research that is performative rather than principled. We reimagined the use of words around this topic and whether “participatory” should be replaced by “partnerships” to more directly reflect engagement expectations. 21–23
We also reflected on specific challenges to attaining the gold standard CBPR study design. For example, when grants are developed and submitted to fund the research, the principal investigator is maintaining a salary, but the CBO and community advisory board (CAB) members are often not paid for their time and expertise during the pre-award period. In addition, when grants are administered by academic institutions, the academic financial processes often create unnecessary compensation burdens for CAB members, like difficulty accessing and navigating payment systems. What value does a check hold for a CAB member who does not have a checking account to cash it? We brainstormed redesign opportunities for community partner compensation practices to ensure they are adequate, equitable and fair, flexible, and transparent. 24 We also discussed the institutional support needed to conduct CBPR. Could we generate a best practice guide to perinatal CBPR within the current constraints of academia and funding? We aspired to conduct a mixed-methods study to capture the perspectives of study participants, CBOs, CAB members, and researchers on best practices of CBPR, including how to avoid overburdening CBOs with formative work, maintain and compensate community engagement between funding opportunities, and build sustainability and transparency into perinatal CBPR. We also sought to explore academic institutional frameworks that facilitate CBPR within the confines of faculty advancement, promotion, and tenure. Altogether, we proposed the need to find creative solutions to address perinatal health inequities through the use of perinatal CBPR that conveys respect, values the needs and expertise of the community partners, and promotes sustainability and transparency.
What Have We Lost and Possibilities We Reimagine
At the conclusion of the 2-day symposium we engaged in a small group reflection activity for collective grieving of the individual and collective harms we experience as a result of the current administration, and to vision how we redefine success and move with integrity and radical reimagination. Through structured discussions, participants documented impacts and strategies for forward progression with hope and community resilience.
First, we asked the groups to reflect on what losses they were experiencing. Participants reported experiences of policy changes as “disruption and theft” through systematic dismantling of systems that promoted well-being and equity. The administration’s strategy of flooding the zone created existential threats to marginalized populations: Black and Latine communities, LGBTQ+ individuals, disabled individuals, immigrants, women, and those with reproductive capacity. The impacts manifested at individual, institutional, and structural levels. Daily processing of ongoing attacks depleted our cognitive bandwidth and capacity. Federal research funding on health equity and community-engaged research centering structurally excluded groups was abruptly cancelled and deemed “unscientific.” These attacks impact us as individuals whose identities and lived experiences are being simultaneously attacked and erased as websites and databases are stolen from the public domain. Funding cuts threatened and continue to threaten our research and clinical practices, employment, and staff. The current undermining of public health and research funding and infrastructure affect our mental health and require ongoing cognitive and emotional labor to process, respond to, and compartmentalize. Individuals, institutions, and movement spaces reveal their underlying values and the extent to which they will capitulate or remain silent in the face of demands to erase equity work.
Next, we asked participants to lean into their hope and imagination to consider what our work could look like. We expressed a shared commitment to be ready with more equitable visions and actions to rebuild our health and research ecosystems as more equitable, joyful, and caring spaces. We also asked individuals how we can measure success and advancement in promoting health equity. Participants affirmed the importance of focusing on community relationships and pairing on economic justice with reproductive justice. Participants will center liberatory frameworks, redefining responsibility and shared ownership and investing in more interprofessional collaborations to dismantle systems of power and better uplift marginalized voices. There were robust discussions about how we redefine our relationships with our work and the importance of balancing our wellness and roles as caregivers personally and professionally with productivity and ongoing action. In order to work collaboratively and move forward, participants noted that by protecting communications, establishing trust, taking rest, and sharing moments with one another is important to create a sustainable and joyful community. Rooting efforts in sharing joy, resilience, healing traditions, resources, and skillsets will also help create spaces where meaningful, transformative work can thrive.
Where Do We Go From Here? Next Steps
The perinatal period is crucial for the health and well-being of pregnant capable individuals, infants, families, and communities. As one of the highest periods of health system contact points, it is a key time to influence health across the lifespan. However, there are deep structural and social inequities, including racism and other forms of discrimination, that impact access to, utilization of, and quality of perinatal care. To address the root causes of these inequities and provide care that not only allows pregnant capable individuals to survive but thrive, perinatal care models must be reimagined.
The conversations to advance these steps will continue beyond this single event, carried forward by perinatal health and reproductive justice leaders who refuse to accept ahistorical frameworks and the deep structural and social inequities and discrimination that negatively impact perinatal care. In addition to generating innovative solutions, symposium participants came away from the 2-day dialogue with new collaborative relationships and a stronger sense of mutual trust and collective care that will advance perinatal health research and health policy advocacy. This collective conversation represents not just a professional obligation, but a love and thirst for a future we have yet to fully imagine but know our perinatal care health system and pregnant capable individuals deserve. We have received grant funding and plans are underway to host the 2nd annual symposium in 2026 so that we can continue to advance our efforts to reimagine and transform perinatal care.
Footnotes
Acknowledgments
The authors sincerely thank their symposium sponsors, including the Georgetown University (GU) Berkley School of Nursing, the Georgetown-Howard Universities Center for Clinical and Translational Science, the O’Neill Institute for National & Global Health Law, the GU Gender + Justice Initiative, the GU Center for Health Equity, and the GU Women & Gender Studies. They also appreciate those who participated in and contributed to the symposium, including Alexia Dunn Amore, Jess Angelson, Bre Calhoun, Sonia Canzater, Lastacia Coleman, Allyson Crays, Katie Daily, Theodora Danylevich, Katie DePalma, Melicia Escobar, Mara Evans, Karen Grace, Rachel R. Hardeman, Tanay Lynn Harris, Kionna Henderson, Briana Kramer, Laura Lazzari, Kathryn Lee, Ebony Marcelle, Bayyinah Mohammed, Sara Paiva, Signey Olson, Katie Page, Jamila Perritt, Rebecca Reingold, Kelley Robinson, Michelle Roett, Dawn Sherman, Ellen Solis, Sola Stamm, Veronica X. Vela, and Nicole Warren. They used Claude AI to assist with cleaning audio transcriptions from the event.
Authors’ Contributions
Conceptualization: C.X.M., L.A., H.M.B., and M.M. Writing—original draft preparation: H.M.B., L.A., C.X.M., C.S., A.K., N.H.G., M.B., K.B., E.C., M.E.T., R.S.E., A.G., K.H., N.J., R.M.B., E.G.M., A.P., K.A.S., E.E., and C.X.M. Writing—review and editing: H.M.B., L.A., C.X.M., C.S., A.K., N.H.G., M.B., K.B., E.C., M.E.T., R.S.E., A.G., K.H., N.J., R.M.B., E.G.M., A.P., K.A.S., E.E., M.M., and C.X.M. Funding acquisition: C.X.M., L.A., and H.M.B. Supervision: H.M.B. Visualization: C.X.M.
Author Disclosure Statement
No competing financial interests exist.
Funding Information
This publication was supported in part by the National Center for Advancing Translational Sciences of the National Institutes of Health under Award Number KL2TR001432, as well as the Susan H. Mayer Endowed Professorship in Health Equity and the Mary L. and Raymond T. Holden Endowed Professorship for Maternal and Infant Health. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Funders had no role in the writing of this article.
Appendix
Abbreviations Used
