Abstract
Introduction:
Effective interventions to address health literacy gaps require both accessibility and community engagement. Proposing an intervention in a community laundromat adds a unique layer of accessibility and convenience, fostering engagement in a familiar, everyday setting. We conducted a needs assessment with laundromat patrons to provide valuable insights that can inform the work of other community health researchers. Needs assessments are an essential step for evaluating the acceptance and support of proposed community-based interventions.
Methods:
We collected survey data using quota sampling to recruit English- or Spanish-speaking patrons from four urban laundromats. We assessed laundromat usage, receptivity to a proposed intervention, reproductive knowledge, self-efficacy, and intention to seek care through descriptive analysis using STATA.
Results:
Participants (n = 60) were 38.8 years old on average, 41.2% spoke only Spanish, and 32.8% had a college degree. Most participants (96.7%) felt their health care experience needed improvement. The average reproductive knowledge score was moderate (mean 7.0, standard deviation 2.8). Areas of least awareness included knowledge on birth intervals (15.0%), folic acid purpose (8.3%), and sexually transmitted illness-related symptoms (18.3%). Significant differences between language groups were found in awareness of birth intervals (p = 0.013), fertility windows (p = 0.000), prenatal care initiation (p = 0.007), STI-related fetal risk (p = 0.027), and pregnancy spacing effects on fetal weight (p = 0.006). No differences were found in self-efficacy or intention to seek care. Participants (68.3%) were receptive to a laundromat-based intervention.
Discussion/Conclusion:
Findings from our community assessment highlight a need for improved reproductive literacy and health care experiences. Participants also shared an interest in laundromat-based and community-driven interventions.
Keywords
Introduction
Inequities in reproductive health outcomes in the United States stem from systemic factors affecting the communities where women and their families live. 1 One contributor is health literacy (HL).1,2 HL is the ability to access, comprehend, and act on health information, which is key to informed decision-making in health.3–5 Limited HL can lead to delays in seeking care, increased emergency services use, poor self-management, reduced engagement with prevention, and less trust in providers and shared decision-making. 6 Individuals most at risk for health inequities based on education, income, race, ethnicity, or age often have limited HL. 7 Gaps in health knowledge, health care access, and self-efficacy are important measures of HL, offering targets for intervention beyond the policy and quality improvement required of the health care system itself.
Local assessments have identified HL gaps as a factor affecting reproductive health outcomes, emphasizing the need for community-driven solutions. In 2018, the DC Primary Care Association reported that Washington, DC (DC), women of childbearing age identified the paucity of fertility and pregnancy knowledge as factors in delayed prenatal care. 8 The 2019 Community Health Needs Assessment (CHNA) identified health education as a primary theme for improving HL in DC. 9 Qualitative CHNA data revealed the importance of fostering dialogue so community members can express their HL needs and preferences by meeting people where they are and using trusted community spaces and culturally responsive approaches: “Information has to be disseminated at Rec Centers, at churches, at schools, and through social media….” 9
Despite increasing recognition of HL as a driver of health inequities and the importance of meeting people where they are, few studies have examined HL gaps specifically in the context of reproductive health outreach in urban community settings.10,11 Prior studies have focused largely on meeting the needs of individuals in clinical or educational settings, leaving a gap in knowledge about how to effectively reach individuals in their everyday environments. While positive outcomes as a result of health education delivered in churches, beauty salons, and barbershops have been reported in the literature,12,13 less evidence exists regarding the effectiveness and feasibility of delivering HL-focused reproductive health interventions at another well-known social hub within local communities—the laundromat.14,15 While laundromats have been used for library programs and chronic disease initiatives, they have not been studied as sites for reproductive health interventions.
Our study applies a community-based participatory research (CBPR) approach to explore laundromats as an unconventional yet promising site for reproductive health education and outreach. We draw on the Paasche-Orlow and Wolf conceptual model, which identifies factors mediating the path between HL and health outcomes: access and utilization of health care, provider–patient interaction, and self-care (Fig. 1). 16 Exploring community experiences with health care access, provider interactions, and self-care in the laundromat setting can inform the development of interventions that engage patrons by leveraging their downtime during laundry cycles. A laundromat-based intervention could expand reproductive health education by bringing information to where individuals do essential work.

Paasche-Orlow and Wolf conceptual model (Paasche-Orlow & Wolf, 2007) with study focus areas boxed in red emphasis.
Before intervention development and implementation, it is necessary to assess whether a laundromat-based intervention would be feasible, well-received, and aligned with community preferences and priorities.17,18 This article presents a needs assessment to measure reproductive health knowledge and evaluate community receptiveness to a proposed laundromat-based health intervention. It also provides a CBPR approach for conducting a needs assessment useful to other researchers seeking to create responsive interventions.
Materials and Methods
Research design
This study employed a CBPR design to explore reproductive health knowledge and community receptiveness to an HL intervention. We selected laundromats as recruitment sites based on prior research indicating they are trusted, frequented spaces within low-income communities—particularly among individuals who may not engage with traditional health care systems.15,19
As part of our formative work, we established a Community Advisory Board (CAB) of community members, laundromat owners, and reproductive health providers to guide the study from its inception.a The 10-member CAB met quarterly and provided feedback on recruitment strategies, participant incentives, and language for surveys, flyers, and consent forms. CAB discussions also helped identify study areas based on neighborhood-level characteristics (Supplementary Table S1) and perceived barriers to health access.20,21 Study areas identified included Wards 1, 4, 5, 7, and 8 of DC.
Instruments
Our study was informed by the Paashe-Orlow and Wolf Conceptual Model and focused on patient access and utilization of health care, patient factors of provider–patient interaction, and patient and extrinsic factors contributing to self-care (Fig. 1).
16
The 80 questions organized into six domains were drawn from validated tools and consultation with content experts (Supplementary Table S2):
Sociodemographic. We captured self-identified variables including age, place of birth, ethnicity/race, and language preference. Health Care Use/Experience. We used open-ended questions to ask about visits, care location, travel, health education, and health experiences. Reproductive Health Knowledge. We used a 15-item, 3-point Likert scale—agree, disagree, and do not know—drawn from Project DC Hope.
22
Higher scores of correct items meant greater awareness or knowledge. Laundromat Use. Selective choice response questions assessed length and reason for patronage of particular laundromats, frequency of use, distance from home, and activities engaged in during downtime. Intervention Receptivity. We used selective choice responses and open-ended questions to assess receptivity to a laundromat-based HL intervention. Self-Efficacy. We used the validated Patient-Reported Outcomes Measurement Information System (PROMIS) 15-item 5-point Likert-type scale assessing independent decision-making concerning care and confidence in performing tasks and overcoming related challenges. This tool has demonstrated good internal consistency (α = 0.94).23,24 The higher the score, the higher the perceived self-efficacy. PROMIS National Institute of Health (NIH), provided T-score cutoff points for self-efficacy—very high (>70), high (60–69), average (40–59), low (30–39), and very low (<30).23,24 Intention to Seek Care. We used a 5-point Likert-type scale, ranging from 1 (completely disagree) to 5 (completely agree), measuring attitudes toward seeking medical help with good internal consistency (α = 0.82).
25
Permission to use and translate validated survey tools was sought and granted. The survey was forward and backward translated and pretested with one English- and one Spanish-speaking individual prior to study start; results from pretesting were not included in the analysis.
Participants and recruitment
The principal investigator (PI) visited laundromats (n = 19) in selected areas with the exception of Ward 8, which did not have a laundromat. Of the seven laundromats that met the inclusion criteria (e.g., open to the public, sufficiently large), five agreed to participate in the study. From these, one laundromat from each area was selected as a recruitment site, resulting in four total study sites.
We used quota sampling to recruit laundromat patrons to achieve a representative sample across the four resulting neighborhoods. A literature review did not provide comparable estimates to support a formal power analysis, due to the lack of existing data on this specific population and setting. Additionally, power-based sample size calculations were not required given the descriptive nature of this needs assessment. Instead, to determine our sample size, we followed the “rules of thumb” for pilot studies when there is no prior information upon which to base the sample size and established a minimum sample size of 60 participants.26,27 Consultation with two biostatisticians further supported this target sample size, which was deemed sufficient to identify meaningful patterns in the data due to the study’s descriptive nature.28,29 Quotas were then set to ensure a comparable representation from each site (approximately 14–16 participants per location) to reflect neighborhood-level diversity and local context. We did not stratify by demographic characteristics due to the exploratory nature of the study.
Two academic institution research team members, at least one identifying as a Hispanic woman fluent in Spanish/English, held recruitment windows of 2–4 h on different days and times of the week to capture a diversity of patrons and evaluate laundromat patron flow. Recruitment took place between October 2021 and March 2022 and continued until 14–16 participants from each laundromat completed surveys.
Eligibility
Participants were eligible if they met the following: (1) identified as women or persons assigned female at birth (women), (2) over 18 years old, (3) Spanish- and/or English-speaking, and (4) living in DC. In our design, we did not set an age cap, recognizing that in matriarchal, cross-generational communities, older women play a role in passing health knowledge to younger generations. 30 This intergenerational information exchange was stressed by CAB members as essential in fostering widespread understanding of reproductive health.31–33 The study was limited to languages in which our team had linguistic and cultural expertise. We focused on recruiting local residents to ensure that participants were likely to be engaged with locally based services, which would better capture the experiences of women navigating local health care systems. This ensured cultural relevance and maximized the study’s potential to identify concerns within the communities served by the laundromats.
Data collection
Once consented, participants were verbally offered either an English or Spanish version of the survey. They were also offered the option to complete the survey on paper or electronically via QR code. Study team members were available to read aloud questions or notate responses as needed. Surveys took 30–45 min to complete; participants were incentivized with a $15 gift card. After each recruitment period, team members completed a postrecruitment form to examine procedures, laundromat attendance, data collection procedures, and team member–participant dynamics. We used this information to assess protocol adherence and study reliability. The PI audited data collection procedures to enhance the dependability, confirmability, and credibility of findings. The authors’ university institutional review board approved all procedures.
Data analysis
We conducted descriptive analysis using STATA 17.0. 34 Based on descriptive analysis results, a chi-square test was used to compare reproductive knowledge scores across language groups. We used the HealthMeasures Scoring Service to calculate T-scores and standard errors (SE). 35 The population mean was defined as 50 (standard deviation [SD] = 10). We ran t-tests, with corresponding Shapiro–Wilk and Breusch–Pagan/Cook–Weisberg tests. Due to links shown in the literature between level of education and HL, we also ran t-tests between self-efficacy and level of education (i.e., high school or less versus more than high school). We analyzed intent to seek care scores with the nonparametric equivalent, Kruskal–Wallis.
Team members from the academic institution (R.M.-B., N.D., K.R.) independently read open-ended survey responses, coding responses to create categories in an inductive process. 36 We met regularly to discuss discrepancies and ensure reliability. 37 Once categories were established, team members independently reexamined open-ended responses to assess patterns across surveys. CAB members reviewed final themes prior to finalization.
Results
Sociodemographics
Of 123 patrons approached, 84 expressed interest and were screened for inclusion. After exclusions due to age (n = 3), language (n = 3), and place of residence (n = 12), 66 patrons provided consent (53.7%). Of these, four did not submit electronic surveys, and two did not complete paper surveys due to time constraints. The final sample consisted of 60 participants; 38 participants completed surveys in English and 22 completed surveys in Spanish. Most participants chose paper surveys (n = 54), and several submitted electronic surveys (n = 6). Demographic characteristics by site are found in Table 1. Participants’ ages ranged from 18–71 years, with a mean age of 38.8. Nineteen participants had a college or university degree. Half of participants were from the United States and approximately one-third were from Spanish-speaking countries of Central America and the Caribbean (Table 1).
Sample Demographics (n = 60)

Hispanic America: Includes Spanish-speaking countries of Central America and the Caribbean.
Data do not sum to n = 60 or 100% because some participants were born in the United States.
Health care use/experience
Of the 85% of participants who reported using health care in the past 12 months, most sought care for routine checkups (76.5%) or obstetric/gynecological care (58.8%). There were no differences in health care use and experience between participants attending different laundromats. English-speaking participants were statistically more likely to report health care use in the past 12 months than Spanish-speaking participants (χ2(1) = 18.29, p = 0.000). Participants most commonly used public transport to travel to health care appointments, with over one-third utilizing this method. Other modes of transportation included taxis/Uber (23.3%), privately owned vehicles (21.7%), walking (21.7%), or having family/friends drive (20.0%). Two participants mentioned having their transportation costs covered by insurance.
The majority of participants reported that their health care experience needed improvement (96.7%). Analysis of open-ended responses revealed an inability to get an appointment or long wait times as the most common areas needing improvement; some also mentioned providers lacking attentiveness or an understanding of patient concerns. One participant wished that providers “were nicer… that they understood people as they were and that they treated us [the patient] well” (60-year-old, English-speaking participant). Another felt that providers were not particularly communicative and that “they should try to evaluate what one says to learn/understand what the patient needs” (38-year-old, Spanish-speaking participant).
The most common sources of information on reproductive health were providers (e.g., midwives, nurses, and physicians; 53.3%), the internet (53.3%), and family (50.0%). Twice as many Spanish than English-language participants mentioned television as a source of information.
Laundromat use
Nearly all participants were repeat laundromat patrons (93.3%). Among repeat patrons, 62.5% visited weekly and 25% visited biweekly. Distance, convenience, or accessibility motivated participants to choose a particular laundromat (41.7%). Half of the participants attended a laundromat within a 10-minute walk of their home, and several participants visited on the same day and time. Downtime was spent scrolling or playing on phones (45.0%), reading (20.0%), or simply waiting/relaxing (16.7%). Observations during recruitment showed most patrons, both participants and non-participants, spent downtime outside of laundry tasks on their phones.
Intervention receptivity
Most participants reported they would be interested in receiving information on reproductive health while waiting at the laundromat (68.3%). There were no significant differences between Spanish and English language speakers in receptivity (χ2(3) = 4.69, p = 0.196). In open-ended responses, participants explained that having this information delivered while they were at the laundromat would be convenient and important:
I am usually not doing much while waiting [and] it’s a convenient place to [be] educated about healthcare without actively seeking it (24-year-old, English-speaking participant).
A small group of participants stated that their willingness to participate in an intervention would depend on whether privacy was needed (5.0%) and the time/day of the presentation (10.0%). Among the eight participants who shared they would decline to engage with an intervention, “not needing the information” or “a good relationship with [their] physician” were cited as reasons; three of these participants had private insurance and were visiting the laundromat this one time.
Reproductive health knowledge
Participants demonstrated moderate knowledge of reproductive health knowledge-based items drawn from project DC-HOPE (Table 2). There were statistically significant differences between language groups. English-speaking participants were more likely to demonstrate awareness of recommended birth intervals (χ2(1) = 6.13, p = 0.013), fertility windows (χ2(1) = 18.37, p = 0.000), recommended initiation for prenatal care (χ2(1) = 7.18, p = 0.007), and newborn risk when born to a mother with an STI (χ2(1) = 4.87, p = 0.027) (Table 2). Spanish-speaking participants had a statistically significantly higher chance of knowing the association between pregnancy spacing and fetal weight (χ2(1) = 7.52, p = 0.006). There were no significant differences between groups for any other knowledge items. Half of the participants knew when fertility windows occurred, and a majority knew prenatal care was needed even in the absence of complications (Table 2). Knowing the reason for taking prenatal vitamins containing folic acid was the area of least awareness (8.3%).
Reproductive Knowledge Scores Overall and Across Language Groups
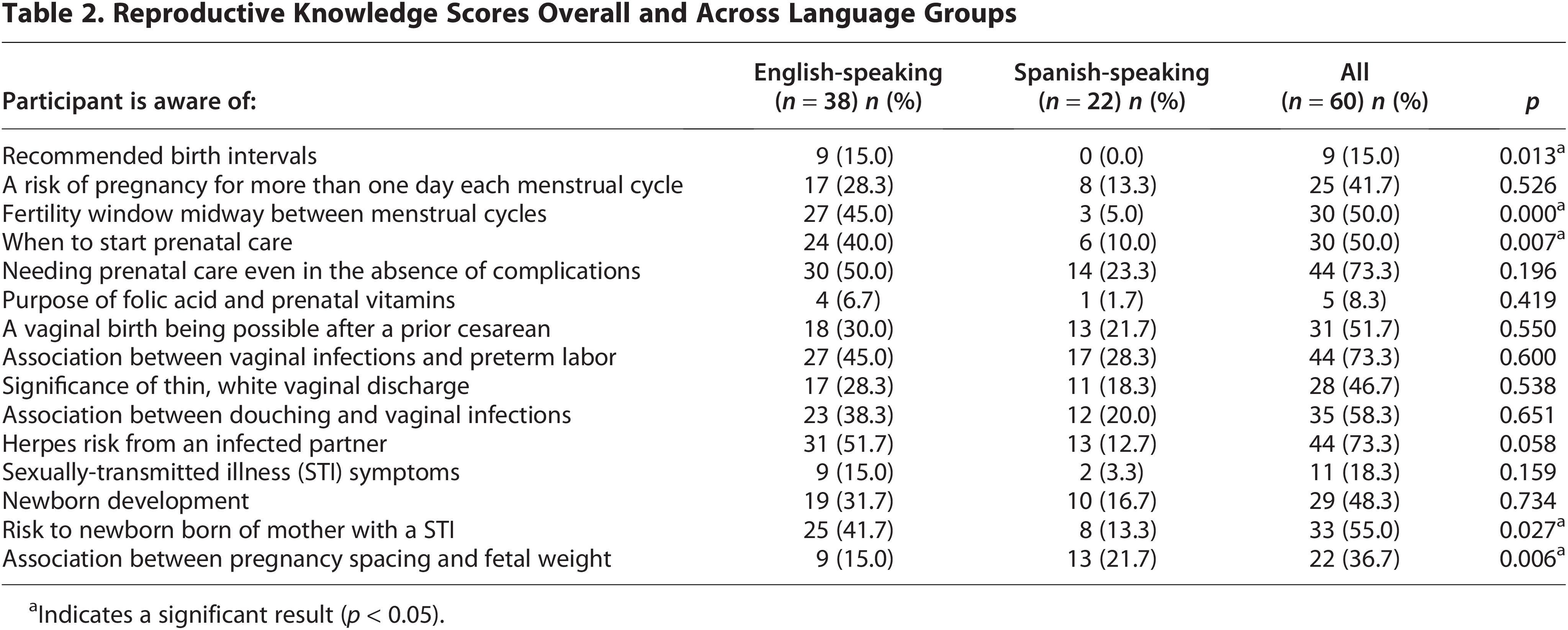
Indicates a significant result (p < 0.05).
Self-Efficacy and intention to seek care
More than half of the participants expressed self-efficacy to make autonomous reproductive decisions, solve problems, and seek care either fairly often or very often. About one-third of participants shared they would “very often” be able to find a reproductive health care provider if needed, even if it were difficult; 23.7% participants responded they could do so “fairly often.” Similarly, most participants (62.7%) responded that they could “fairly often” and “very often” find a way to procure their desired birth control even if someone disagreed with their decision.
Reproductive health self-efficacy scores were averaged for our sample with a total mean score of 50.0 (SD 1.2) (Table 3). Self-efficacy scores were normally distributed (p = 0.322) and homoscedastic (p = 0.261), meeting t-test assumptions. There were no significant differences in self-efficacy scores between Spanish and English-speaking participants (t(57) = 0.908, p = 0.368), and both groups expressed average self-efficacy (Table 3). Participants with primary or secondary education had significantly lower self-efficacy compared to those with college or higher (t(55) = −2.656, p = 0.010). Participants’ intention to seek care scores also reflected the general population mean with a mean score of 48.9 (SD 1.6) (Table 3). There were no significant differences in intention to seek care scores between Spanish and English-speaking participants (χ2(1) = .624, p = 0.430) (Table 3).
Self-Efficacy and Intention to Seek Care Scores Overall and across Language Groups

One participant did not answer the self-efficacy questionnaire.
SD, standard deviation; SE, standard error.
Discussion
Research indicates a correlation between low HL and poor health outcomes, particularly in underserved communities living with health inequities. 38 Our study represents a critical first step in gauging community need and interest in a laundromat-based HL intervention. Participants demonstrated moderate reproductive health knowledge, with significant gaps in awareness around fertility windows, recommended birth intervals, and the role of folic acid in prenatal care, underscoring a need for additional information.30,39
Our findings support partnering with laundromats as sites for outreach as most patrons lived within walking distance, allowing for HL content to be tailored to community needs. Patrons reported visiting on specific days, also creating an opportunity for follow-up engagement. Though laundromats have served as sites for reading-focused literacy programs, research on partnering with laundromats for health-related interventions is limited,b with existing literature focused on business metrics rather than research-driven data. 40 The high level of interest expressed by laundromat patrons in receiving health information while waiting presents an innovative opportunity for health outreach—one with potential to reach underserved populations with tailored health education in a comfortable and nonstigmatized environment.
An intervention in laundromats could be particularly beneficial to Spanish speakers. Although Spanish-speaking participants demonstrated similar levels of self-efficacy and intention to seek care to English-speaking participants, they were significantly less likely to report recent health care use, underscoring potential challenges in navigating the health care system. Camargo et al. reported that among Hispanic women, language barriers, misunderstanding, and mistrust are significant obstacles to prenatal care access. 30 Their study highlights how familial and social networks facilitate early access to prenatal care. Similarly, our study found a significant difference in prenatal care knowledge between Spanish- and English-speaking participants. We propose that a community-informed and laundromat-based intervention could guide Spanish-speaking patrons and their support networks toward timely and culturally competent care. A laundromat-based approach promoting better understanding of available services, such as bilingual or culturally-concordant providers, could bridge gaps, facilitate trust, and improve the likelihood of timely prenatal care entry.41–43
Our study has limitations, including its community-specific approach, making reproducibility challenging. Participants may have also been distracted when completing surveys during the limited time between laundry loads. However, these limitations are also some of its notable strengths. The engagement of the CAB throughout the study’s development and implementation ensured that the survey was tailored to the community, and the option to have surveys read to participants during downtime improved accessibility by eliminating literacy requirements.
The results of our assessment support the need to improve HL among laundromat patrons and should inform the content and modality of future HL interventions. Improving HL has the potential to augment patient agency in health care decisions, enabling better communication with providers and supporting shared decision-making. 44 One area of needed exploration is assessing the best and most acceptable methods of delivering information (e.g., digital kiosks, videos accessed through QR codes, pamphlets, community health workers), as well as evaluating the impact of such methods on self-efficacy and intention to seek care.
Conclusions
Research on laundromats as sites for community-based interventions is limited, but our results highlight their potential for disseminating health education in communities with health care access barriers and distrust due to systemic biases. Our study contributes to the literature on CBPR-driven health interventions, highlighting the importance of codeveloping programs that are grounded in community input, which is critical for achieving meaningful and sustainable outcomes that connect communities to local resources.45–47 This approach aligns with existing literature on the importance of community-specific interventions and the need for community assessments to design health initiatives that address the self-identified needs of underserved communities.12,13,15,38,48
Authors’ Contributions
Conceptualization: R.M.-B.; methodology: R.M.-B.; data analysis: R.M.-B., K.R., N.D.; writing—original draft preparation: R.M.-B., K.R., N.D.; writing—review and editing: R.M.-B., A.P.T., K.H., A.H.H.-d.-M.; Funding acquisition: R.M.-B.; and supervision: R.M.-B.
Footnotes
Acknowledgments
The authors acknowledge CAB members—Ra Amin, Marialuz Castro, Jane Lole, Rene McCray, Quiana Mitchem, Laura Spagna, Tiffany Tyler, Myron Ward, and Laura Worby—for informing and guiding our decisions along each step of the project. The authors thank the participants and laundromat owners of Wards 1, 4, 5, and 7 for their time and receptiveness to our work. The authors are appreciative of Drs. Jane Fall-Dickson, Linda Gallo, and Laura Linnan for their mentorship. We would additionally like to acknowledge Drs. Haijun Wang and Nancy Crowell for their biostatiscal support. R.M.-B. was a participant in the 2023 National League of Nursing (NLN) Scholarly Writing Retreat, sponsored by the NLN Chamberlain College of Nursing Center for the Advancement of the Science of Nursing Education.
Author Disclosure Statement
No competing financial interests exist.
Funding Information
This work was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health under Grant KL2TR001432. This information or content and conclusions are those of the authors and should not be construed as the official position or policy of, nor should any endorsements be inferred by, HRSA, HHS, the National Institutes of Health, or the United States government.
Supplemental Material
Abbreviations
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
