Abstract
Background:
Hallux valgus (HV) is a common forefoot deformity associated with pain, gait impairment, and reduced quality of life. Minimally invasive chevron-Akin (MICA) osteotomy provides reliable correction with low reported recurrence. However, when combined with distal minimally invasive metatarsal osteotomies (DMMOs) for coexistent metatarsalgia, altered forefoot biomechanics may increase recurrence risk. No prior study has directly compared outcomes between isolated MICA and combined MICA+DMMO. The primary objective was to compare radiographic recurrence at 12 months, with secondary objectives including patient-reported outcomes, pain, and complications. We hypothesized that MICA+DMMO would be associated with higher radiographic recurrence.
Methods:
This retrospective comparative cohort study included 121 consecutive patients undergoing minimally invasive HV correction at 2 high-volume centres between 2019 and 2024, with a minimum 12-month follow-up. Sixty patients underwent MICA alone and 61 underwent MICA+DMMO (second-fourth metatarsals). Outcomes included radiographic angles (hallux valgus angle [HVA], intermetatarsal angle), Patient-Reported Outcomes Measurement Information System [PROMIS] physical function and pain interference, visual analogue scale (VAS) pain, and complications. Recurrence was defined as HVA >20 degrees.
Results:
Baseline demographics and deformity severity were comparable between groups. Both cohorts achieved significant early correction. At 12 months, mean HVA was lower following MICA alone (14.9 ± 3.8 degrees) compared with MICA+DMMO (17.7 ± 4.7 degrees; mean difference 2.8 degrees, 95% CI 1.0-4.6; P = .003). Radiographic recurrence occurred in 11.7% of MICA patients vs 47.5% of MICA+DMMO patients (absolute risk difference 35.8%, 95% CI 20.6-50.9; P < .0001). PROMIS physical function improved substantially in both groups, with greater 12-month improvement in the MICA+DMMO cohort (mean change 36.6 vs 29.8 points; mean difference 6.8, 95% CI 4.1-9.5; P < .0001), exceeding minimal clinically important difference thresholds. PROMIS pain interference decreased by more than 30 points in both groups, with no between-group difference. VAS pain improved similarly to a mean of 1.4 at final follow-up. Overall complication rates were comparable (15%).
Conclusion:
Both isolated MICA and combined MICA+DMMO were associated with radiographic correction and clinically significant improvements in pain and function at 12 months. However, the addition of DMMO is associated with a substantially higher rate of radiographic recurrence at 12 months despite greater functional gains; these findings should be interpreted as short-term observational associations rather than causal evidence. Further prospective studies are warranted to clarify the long-term biomechanical impact of combined procedures.
Level of Evidence:
Level III, retrospective comparative study.
Keywords
Introduction
Hallux valgus (HV) is one of the most common forefoot deformities, affecting up to 23% of adults and more than one-third of the elderly population, with a marked female predominance.1 -3 The deformity is associated with pain, impaired gait, difficulty with footwear, and reduced quality of life. 4 Surgical correction remains the gold standard for symptomatic cases unresponsive to conservative measures, yet recurrence remains a major concern, with reported rates ranging from 10% to more than 30% depending on the surgical technique, patient factors, and the radiographic criteria used.5 -7 Recognized risk factors for recurrence include higher preoperative hallux valgus angle (HVA) and intermetatarsal angle (IMA), sesamoid malposition, residual deformity, and insufficient soft tissue balancing.8 -10
Minimally invasive surgery (MIS) has gained popularity in the management of HV in recent years because of its reduced soft tissue disruption, faster rehabilitation, and favorable cosmetic results compared with open procedures.11 -13 Among MIS techniques, the minimally invasive chevron and Akin (MICA) osteotomy particularly in its third- and fourth-generation iterations has demonstrated excellent short- and midterm outcomes, including significant radiographic correction, improved patient-reported outcomes, and low rates of symptomatic recurrence.14 -17 However, reported radiographic recurrence rates after MICA range from 3.3% to 17% in severe deformities, depending on preoperative severity and follow-up duration.15,17,18
The distal minimally invasive metatarsal osteotomy (DMMO) is widely used to treat central metatarsalgia by overloaded metatarsal heads while preserving joint mobility.19 -21 When combined with MICA, DMMO can address coexisting HV and metatarsalgia in a single stage, potentially avoiding multiple surgeries and improving overall forefoot load distribution. 22 However, performing DMMO concurrently with HV correction may alter first ray biomechanics by allowing lateral translation of the lesser metatarsal heads, which could destabilize the corrected first metatarsal and predispose to HV recurrence. 23
Our previously published work demonstrated that combined MICA and DMMO procedures yield substantial improvements in radiographic alignment and patient-reported outcomes at 12 months but are associated with a high rate (75%) of mild radiographic recurrence (HVA > 20 degrees). 23 Although this recurrence was largely radiographic and did not correspond to diminished functional scores or patient satisfaction, the findings underscore the need to determine whether DMMO contributes to increased recurrence risk.
To our knowledge, no prior study has directly compared recurrence rates between patients undergoing isolated MICA and those undergoing combined MICA and DMMO for HV correction. The primary objective of this study was to compare the rate of radiographic recurrence, defined as a HVA >20 degrees at 12 months, between patients undergoing isolated MICA osteotomy and those treated with combined MICA and DMMOs. Secondary objectives included patient-reported outcomes (Patient-Reported Outcomes Measurement Information System [PROMIS] physical function and pain interference), visual analogue scale (VAS) pain scores, and procedure-related complications. We hypothesized that the addition of DMMO to MICA would be associated with a higher rate of radiographic recurrence, potentially related to altered forefoot biomechanics.
Materials and Methods
Study Design and Setting
This was a retrospective comparative cohort study conducted at 2 high-volume foot and ankle surgery centres specializing in minimally invasive forefoot procedures: Assuta Medical Centre (Tel Aviv, Israel) and St Anna medical center (Lucerne, Switzerland). Institutional review board (IRB) approval was obtained before study initiation (AMC 0087-25). All procedures were performed by fellowship-trained foot and ankle surgeons experienced in MICA and DMMO techniques.
Patient Selection
We reviewed the records of adult patients (≥18 years) who underwent minimally invasive hallux valgus correction between January 2019 and December 2024 with a minimum of 12 months’ clinical and radiographic follow-up. Two cohorts were identified: MICA-alone group patients who underwent isolated MICA osteotomy, with or without concomitant Akin osteotomy, for symptomatic HV. The second group identified was MICA+DMMO group patients who underwent MICA combined with DMMO of the second, third, and fourth metatarsals for HV and concurrent central metatarsalgia.
Inclusion criteria were symptomatic HV of any severity unresponsive to ≥6 months of conservative management (shoe modifications, orthoses, activity modification, and analgesia). For the MICA+DMMO group those with a clinical diagnosis of central metatarsalgia with plantar tenderness under the lesser metatarsal heads were included. Exclusion criteria were prior forefoot surgery of any kind on the index foot, Charcot arthropathy or inflammatory arthropathy affecting foot alignment (except stable rheumatoid or psoriatic arthritis), neuromuscular disorders affecting forefoot stability, and less than 12 months of follow-up.
Surgical Techniques
Minimally invasive chevron-Akin
All MICA procedures followed the fourth-generation technique described by Redfern and Vernois,18,19 involving a percutaneous straight first metatarsal osteotomy fixed with 2 screws (one 4.0-mm beveled screw and a second 3.0- or 4.0-mm beveled screw according to surgeon preference). An Akin osteotomy was performed based on intraoperative assessment of residual hallux valgus interphalangeal joint.
Distal minimally invasive metatarsal osteotomy
DMMO was performed through small dorsal incisions without internal fixation, targeting decompression of overloaded central metatarsals while maintaining metatarsophalangeal joint mobility. Osteotomies were made at approximately 45 degrees to the long axis of the metatarsal shaft, allowing controlled shortening and elevation, as described by Vernois and Redfern.16,18,19
Postoperative protocol
All patients were permitted immediate full weightbearing in a rigid postoperative shoe for 6 weeks. This was followed by a transition to comfortable athletic footwear and a structured physiotherapy program focusing on range-of-motion restoration, gait training, and gradual return to activities.
Outcome Measures
Radiographic assessment
Weightbearing anteroposterior radiographs were obtained preoperatively and at 3 and 12 months postoperatively. Measurements included the HVA and intermetatarsal angle (IMA), performed independently by two fellowship-trained foot and ankle surgeons using standardized techniques. In cases of significant discrepancy, a third independent fellowship-trained surgeon masked to group allocation provided the definitive measurement. Radiographic recurrence was defined a priori as HVA >20 degrees at final follow-up. 23
Radiographic reliability analysis
To assess the reliability of radiographic measurements, inter- and intra-observer agreement was evaluated for HVA and IMA. Measurements were independently performed by 2 fellowship-trained foot and ankle surgeons. Intra-observer reliability was assessed by repeat measurements performed by the same observers after a minimum washout period. Reliability was quantified using the intraclass correlation coefficient (ICC) with a 2-way random effects model and absolute agreement. ICC values were interpreted according to standard thresholds, with values >0.75 considered good and >0.90 considered excellent reliability.
Clinical outcomes
Patient-reported outcomes were assessed using the Patient-Reported Outcomes Measurement Information System (PROMIS) domains of physical function, pain interference. PROMIS questionnaires were administered electronically using validated local language versions, in accordance with PROMIS guidelines. Scores were collected preoperatively and at 3 and 12 months postoperatively. Minimal clinically important difference (MCID) thresholds were defined as 4.5 to 6.0 points for physical function and pain interference and 1 point for pain intensity, based on established orthopaedic literature. Pain severity was additionally assessed using a 10-point VAS, reflecting average pain during daily activities. Procedure related complications including nonunion, infection, nerve injury, and hardware-related symptoms were prospectively recorded.
Sample Size Calculation
A formal a priori sample size calculation was performed for the primary endpoint of radiographic recurrence at 12 months. Published series have reported recurrence rates after MICA ranging between 10% and 25%.14,15,17,21 In contrast, our pilot data demonstrated a recurrence rate of approximately 75% in the MICA+DMMO cohort. 23 Assuming a 25% recurrence rate following MICA alone vs 75% after MICA+DMMO, the study was powered to detect this 50% absolute difference, considered clinically significant. Using a 2-sided test for independent proportions with α = 0.05% and 80% power, the required sample size was 48 patients per group. To provide adequate power not only for the primary endpoint but also for secondary outcomes (eg, PROMIS domains with moderate effect sizes), we expanded the final target enrolment to 60 and 61 patients per group (total N = 121). This adjustment also allowed for potential loss to follow-up and improved the generalizability of the findings.
Statistical Analysis
Participants were classified into 2 groups (No DMMO; DMMO 2-3-4) and assessed at baseline (T0), 3 months (T3), and 12 months (T12). Continuous outcomes included IMA, HVA, PROMIS domains (physical function, pain interference, pain intensity), and VAS.
Normality of each outcome measure at each time point was assessed using the Shapiro-Wilk test. Although some variables deviated from a normal distribution, results are reported as mean and SD to allow consistent presentation and facilitate comparison across outcomes and time points. Between-group comparisons at each time point were performed using independent samples t tests, and categorical variables were compared using the χ2 or Fisher exact test, as appropriate. Statistical significance was set at P <.05.
To account for baseline differences, absolute change (Δ) from baseline and percentage change were also calculated for each participant: Δt = Y − Y0, %Δt = 100 × (Yt − Y0)/Y0, where Yt represents the outcome at follow-up (T3 or T12) and Y0 is the baseline value. The original and the derived variables were compared between groups using the Mann-Whitney U test
No loss to follow-up occurred during the study period.
All statistical tests were 2-sided, with a significance threshold of P <.05. Analyses were performed in R, version 4.5.0 (R Foundation for Statistical Computing).
Results
A total of 121 patients were included: 60 in the No DMMO group and 61 in the DMMO 2-3-4 group. The mean age was 52.0 ± 13.6 years, with no significant difference between groups (53.3 vs 50.9 years, 95% CI 49.6-54.5, P = .303). The majority of patients were female (83.5%), with a similar sex distribution across groups (P = .632).
The mean BMI for the entire cohort was 26.5 ± 3.3, with no significant between-group difference (26.3 vs 26.6, 95% CI 21.4-28.3, P = .507). Most patients were nonsmokers (88.4%), with comparable smoking rates in the 2 groups (13.3% vs 9.8%, P = .583) (Table 1).
Baseline Demographic and Clinical Characteristics. a
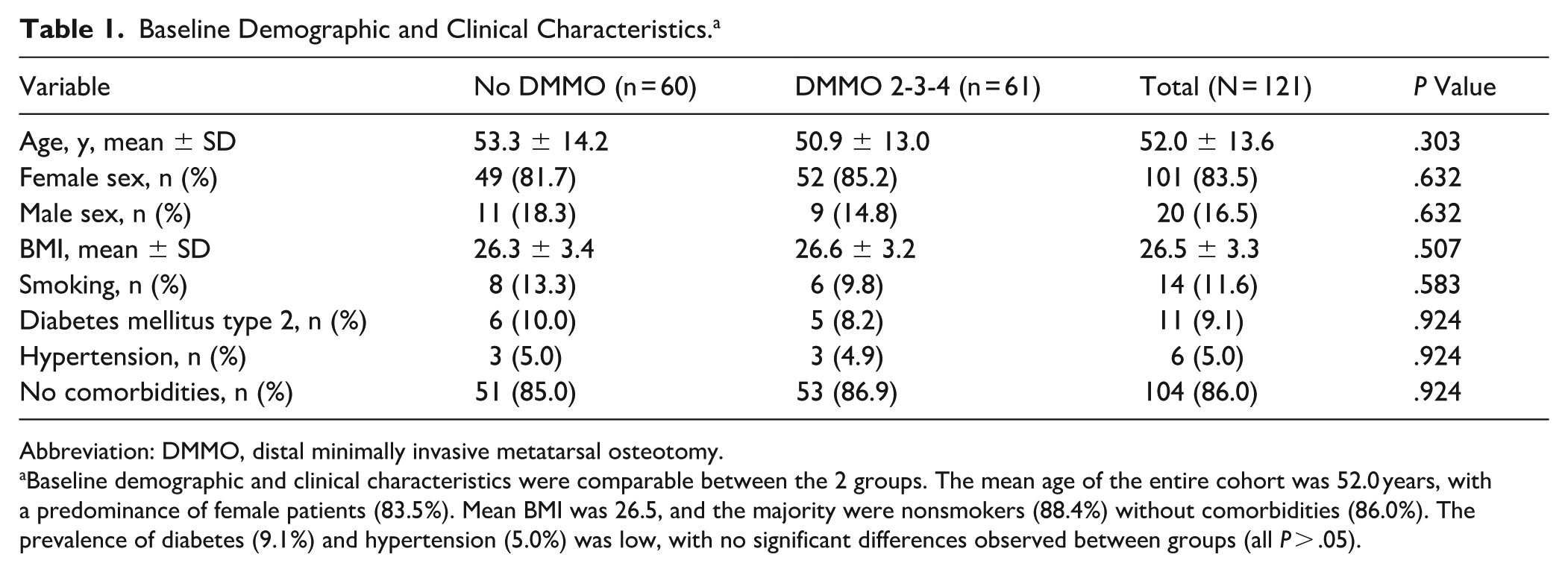
Abbreviation: DMMO, distal minimally invasive metatarsal osteotomy.
Baseline demographic and clinical characteristics were comparable between the 2 groups. The mean age of the entire cohort was 52.0 years, with a predominance of female patients (83.5%). Mean BMI was 26.5, and the majority were nonsmokers (88.4%) without comorbidities (86.0%). The prevalence of diabetes (9.1%) and hypertension (5.0%) was low, with no significant differences observed between groups (all P > .05).
Comorbidities were uncommon, and their distribution was balanced between groups. Diabetes mellitus type 2 was present in 9.1% overall (10.0% vs 8.2%), hypertension in 5.0% (5.0% vs 4.9%), and the majority of patients (86.0%) reported no comorbidities. No significant between-group differences were observed for any baseline characteristic (P > .05 for all). No loss to follow-up occurred during the study period (Table 1).
The mean preoperative IMA was 13.7 ± 1.3 degrees overall, with no significant difference between groups (13.9 vs 13.6 degrees, 95% CI 12-16, P = .098). Similarly, the mean HVA was 35.7 ± 5.0 degrees, comparable between groups (35.8 vs 35.7 degrees, 95% CI 26-44, P = .864) (Table 2, Figure 1).
Radiographic and Clinical Outcomes. a

Abbreviations: DMMO, distal minimally invasive metatarsal osteotomy; HVA, hallux valgus angle; IMA, intermetatarsal angle; PROMIS, Patient-Reported Outcomes Measurement Information System; VAS, visual analogue scale.
Both groups demonstrated substantial improvements in PROMIS physical function, pain interference, and VAS pain scores over the 12-month follow-up. PROMIS physical function improved beyond the MCID in both groups, with the DMMO cohort showing significantly greater functional gains at 12 months. PROMIS pain interference decreased markedly in both groups, exceeding the MCID, with no significant differences between cohorts. VAS pain scores improved similarly, reaching near-complete pain relief at 12 months in both groups. Overall, these findings highlight robust clinical benefits in both groups, with superior long-term functional outcomes in patients undergoing combined MICA+DMMO.

Intermetatarsal angle (IMA) and hallux valgus angle (HVA) changes over time. Both groups showed significant radiographic correction of IMA and HVA after surgery. At 3 months, correction was comparable between groups; however, by 12 months, the DMMO group demonstrated a higher mean HVA and a significantly greater recurrence rate compared with the No DMMO group, whereas IMA remained stable in both.
Radiographic measurements demonstrated good to excellent inter- and intra-observer reliability. Inter-observer ICC was 0.86 for HVA and 0.83 for IMA, whereas intra-observer ICC was 0.90 for HVA and 0.88 for IMA.
Baseline PROMIS physical function scores averaged 41.9 ± 6.2, with slightly higher values in the No DMMO group (42.9 vs 40.9, 95% CI 32-45, P = .163). PROMIS pain interference scores were 63.9 ± 2.5 overall, with the DMMO group showing significantly lower scores compared with the No DMMO group (63.4 vs 64.4, 95% CI 62-74, P = .044). VAS pain scores at baseline were also comparable, with a mean of 6.6 ± 0.9, and no between-group difference (6.5 vs 6.7, 95% CI 5-8, P = .309) (Table 2, Figure 1).
Radiographic analysis demonstrated a significant reduction in IMA following surgery in both groups. At baseline, mean IMA was 13.9 ± 1.4 degrees in the No DMMO group and 13.6 ± 1.2 degrees in the DMMO 2-3-4 group (95% CI 11-16, P = .098). At 3 months, IMA improved to 8.5 ± 0.9 degrees and 8.4 ± 0.7 degrees, respectively, with no significant difference between groups (95% CI 7-9, P = .351). At 12 months, mean IMA was 8.9 ± 0.9 degrees in the No DMMO group and 8.5 ± 0.9 degrees in the DMMO group, a statistically significant difference (95% CI 7-10, P = .026). The absolute reduction in IMA from baseline to 3 months averaged −5.4 ± 1.5 degrees and −5.2 ± 1.3 degrees, 95% CI −4 to −6; P = .198), whereas from baseline to 12 months it was −5.0 ± 1.3 degrees and −5.1 ± 1.4 degrees (95% CI −4 to −6, P = .801), respectively (Table 2, Figures 1–3).

Radiographs following MICA+DMMO bunion correction. (A, top and bottom)-Immediate postop (B, top and bottom) 12 months after surgery. The immediate postoperative radiograph (A), obtained following a MICA procedure combined with DMMO of the second, third, and fourth metatarsals, demonstrates excellent correction of both the intermetatarsal angle (IMA) and the hallux valgus angle (HVA). However, at the 1-year follow-up (B), an increase in the HVA is observed, indicating a recurrence of the deformity. DMMO, distal minimally invasive metatarsal osteotomy; MICA, minimally invasive chevron-Akin.
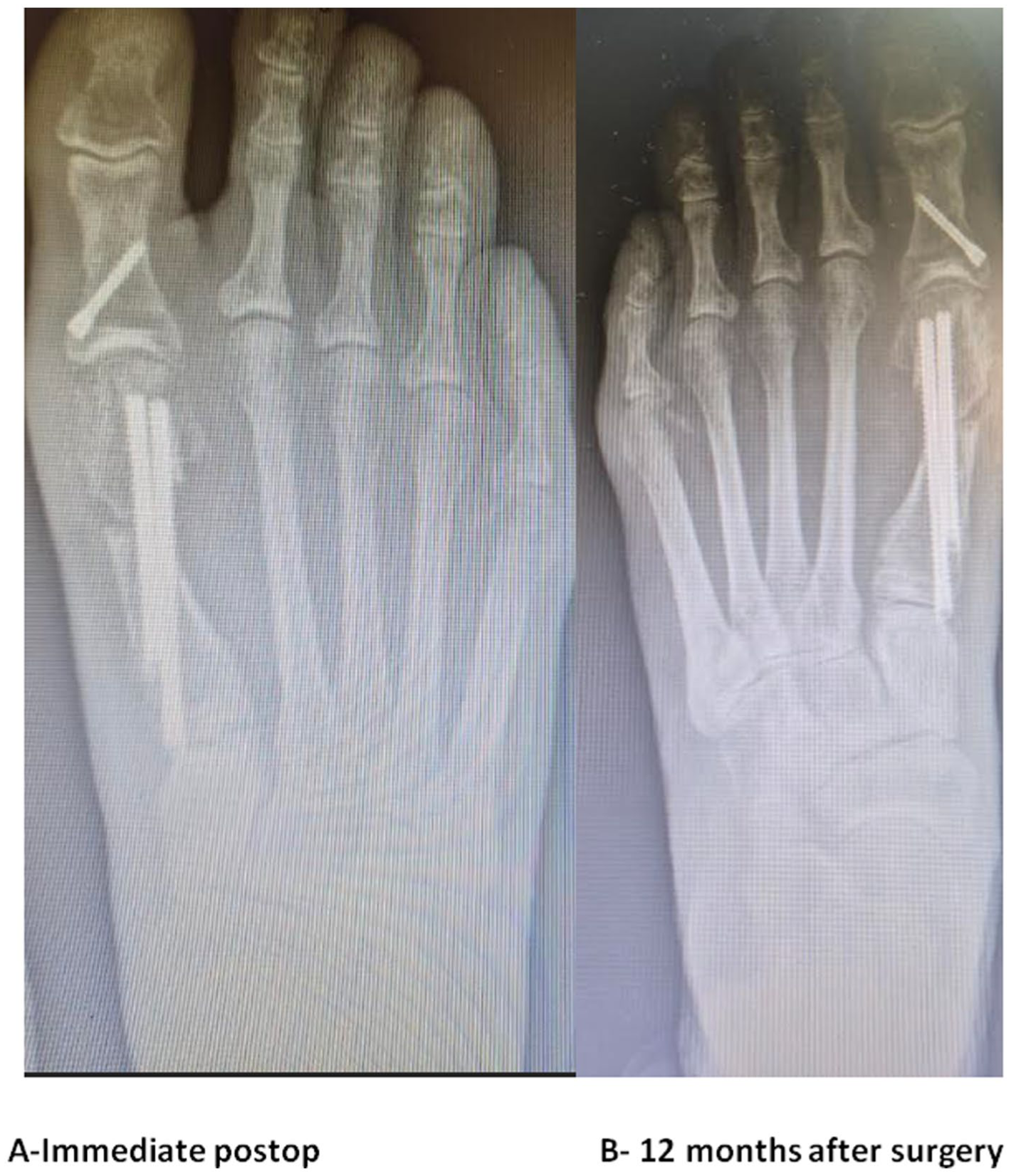
Radiographs following MICA bunion correction: (A) Immediate postop (B)- 12 months after surgery. The immediate postoperative radiograph (A), obtained following a MICA procedure, demonstrates excellent correction of both the intermetatarsal angle (IMA) and the hallux valgus angle (HVA). At the 1-year follow-up (B), the correction is maintained.
Preoperative HVA was comparable between groups, with mean values of 35.8 ± 5.2 degrees in the No DMMO group and 35.7 ± 4.9 degrees in the DMMO 2-3-4 group (95% CI 27-45, P = .864). At 3 months, both groups demonstrated substantial correction, with mean HVA reduced to 12.9 and 12.6 degrees, respectively (95% CI 10-16, P = .466). At 12 months, however, the No DMMO cohort maintained lower mean HVA (14.9 ± 3.8 degrees) compared with the DMMO group (17.7 ± 4.7 degrees), representing a significant difference (95% CI 12-24, P = .003). The absolute change in HVA from baseline to 3 months was similar between groups (−22.9 vs −23.1 degrees, 95% CI −20 to −32; P = .793), but by 12 months the correction was greater in the No DMMO group (−20.8 vs −18.0 degrees, 95% CI −20 to −35; P = .008). Radiographically, none of the patients in either group demonstrated HVA >20 degrees at 3 months. At 12 months, however, recurrence defined as HVA >20 degrees was significantly more frequent in the DMMO group (47.5%) compared with the No DMMO group (11.7%) (P < .0001) (Table 2, Figures 1–3).
Preoperative PROMIS function scores were similar between groups, averaging 42.9 ± 7.0 in the No DMMO cohort and 40.9 ± 5.3 in the DMMO 2-3-4 group (95% CI 32-55, P = .163, Cohen d = −0.323). At 3 months, both groups demonstrated substantial improvement, with mean scores of 60.5 and 58.5, respectively (95% CI 49-70, P = .069). By 12 months, however, the DMMO group exhibited significantly higher function scores (77.5 ± 4.9) compared with the No DMMO group (72.7 ± 3.0, P < .0001). Absolute change from baseline to 3 months was nearly identical (17.6 in both groups, 95% CI 14-32, P = .975), whereas at 12 months, patients in the DMMO group demonstrated a greater improvement (36.6 vs 29.8, 95% CI 25-49, P < .0001, Cohen d = 1.179). Both groups demonstrated improvements in PROMIS function scores that exceeded the minimal clinically important difference (MCID) of 4 to 6 points (Table 2, Figure 4).

PROMIS function and VAS changes over time. Both groups demonstrated marked improvements in PROMIS function and VAS pain scores over time. Functional gains were greater in the DMMO group at 12 months, exceeding the MCID, whereas pain reduction (VAS score) was similar between groups, highlighting strong clinical improvement regardless of recurrence. PROMIS, Patient-Reported Outcomes Measurement Information System; VAS, visual analogue scale.
Baseline PROMIS pain interference scores were slightly higher in the No DMMO group (64.4 ± 2.7) compared with the DMMO 2-3-4 group (63.4 ± 2.3), a difference that reached statistical significance (95% CI 59-70, P = .044, Cohen d = −0.399). At 3 months, both groups demonstrated marked improvement, with mean scores decreasing to 51.4 ± 2.3 and 50.6 ± 2.6, respectively, with no significant difference between groups (95% CI 48-56, P = .154, Cohen d = −0.326). By 12 months, continued improvement was observed, with mean scores of 33.0 ± 2.1 in the No DMMO cohort and 32.7 ± 2.4 in the DMMO group (95% CI 28-40, P = .699, Cohen d = −0.133). Absolute change from baseline to 3 months was similar between groups (−13.0 ± 2.2 vs −12.8 ± 2.3, 95% CI −10 to −23, P = .599, Cohen d for change = 0.089), as was the change at 12 months (−31.4 ± 1.9 vs −30.7 ± 2.1, 95% CI −29 to −42, P = .217, Cohen d for change = 0.349). The reductions in PROMIS pain interference scores in both groups substantially exceeded the MCID of 4 to 6 points (Table 2).
Preoperative VAS pain scores were similar between groups, averaging 6.5 ± 1.0 in the No DMMO cohort and 6.7 ± 0.8 in the DMMO 2-3-4 group (95% CI 6-9, P = .309). At 3 months, both groups demonstrated marked pain reduction, although mean VAS was slightly lower in the No DMMO group (4.2 ± 0.7 vs 4.4 ± 0.8, 95% CI 3-6, P = .047). By 12 months, mean VAS had further improved to 1.4 ± 0.6 in both groups, with no significant difference (95% CI 1-3, P = .773). Absolute change from baseline to 3 months (−2.3 ± 1.0 in both groups, 95% CI −4 to −1, P = .886) and to 12 months (−5.1 ± 1.0 vs −5.3 ± 1.1, 95% CI −6 to −4, P = .595) was comparable (Table 2, Figure 4).
Complications were reported in 15% of the overall cohort, with no significant difference between groups (P = .807). The most frequent issues included hardware removal for symptomatic screw prominence (8 cases in total, 4 in each group, 6%) and transient neuropathy (6 cases in total, 3 in each group, 5%), both of which resolved without long-term sequelae. Nonunion was observed only in the DMMO group, affecting 4 patients (1 metatarsal in each patient). Non-union was observed in 1 metatarsal in each of 4 patients, representing a total of 4 cases out of 183 DMMO procedures performed (2.2%). Three of these patients remained asymptomatic and required no further intervention, whereas in 1 case revision surgery was necessary to address the nonunion. Superficial wound infection occurred in 2 patients (1%), 1 from each group, and responded well to oral antibiotics and local care (Table 3).
Postoperative Complications. a

Abbreviation: DMMO, distal minimally invasive metatarsal osteotomy.
Complications were observed in 15% of the overall cohort, with no significant difference between the No DMMO and DMMO groups. The most frequent events were hardware removal due to screw prominence (6.7% vs 6.6%) and transient neuropathy (6.7% vs 3.3%).
Four of 183 DMMOs.
Discussion
This comparative cohort study provides direct evidence comparing isolated MICA with combined MICA and DMMO in the management of hallux valgus with or without associated central metatarsalgia. Although both techniques achieved meaningful radiographic correction and clinically significant improvements in PROMIS and VAS outcomes exceeding established MCID thresholds, our findings add an important nuance to the existing literature. Specifically, although the addition of DMMO was associated with greater functional improvement, it was also associated with a substantially higher rate of radiographic recurrence. These results highlight a clinically relevant trade-off that should inform surgical decision making when considering combined procedures (Figure 2).
Although both groups achieved similar early correction, differences emerged at 12 months. Mean HVA was significantly higher in the DMMO group (17.7 vs 14.9 degrees), despite neither exceeding 20 degrees on average. Crucially, nearly half of patients in the DMMO cohort (47.5%) developed radiographic recurrence (HVA > 20 degrees) compared with only 11.7% in the MICA-alone group. Recurrence of HV after surgery remains a major concern, with rates in the literature ranging from 10% to >30% depending on technique and definitions used.4 -6 Biomechanically, performing DMMOs across the central metatarsals may alter load distribution and destabilize the first ray, thereby predisposing to recurrence, as has been suggested in prior clinical and experimental reports.17 -19,23
A previous study by Genuth et al 23 reported a radiographic recurrence rate (HVA > 20 degrees) in 75% of patients treated with combined MICA and DMMO. This study’s findings demonstrate similar trends, although with somewhat lower recurrence rates. The differences may be attributable to sample size, as our previous series (Genuth et al 23 ) included 100 patients in the MICA+DMMO group, whereas the present study analysed 61 patients, which may have influenced the observed proportions.
Despite higher recurrence, PROMIS physical function scores were significantly better in the DMMO group at 12 months (77.5 vs 72.7). The mean improvement of 36.6 points compared with 29.8 in the MICA-alone cohort far surpassed the MCID of 4 to 6 points. 19 Similarly, PROMIS pain interference decreased by more than 30 points in both groups, exceeding MCID thresholds, without between-group differences. These findings highlight the paradox of radiographic recurrence without deterioration in patient-reported outcomes, a phenomenon consistent with prior MIS series reporting discordance between radiographic and clinical recurrence.14,16,17,23
The greater improvement in function and pain observed in the MICA+DMMO group may reflect the greater symptom burden these patients experienced preoperatively. By addressing both hallux valgus and central metatarsalgia, the combined procedure likely provides a more meaningful functional benefit for those who are more limited at baseline.
Although nearly half of the patients in the DMMO group demonstrated mild radiographic recurrence at 12 months, this did not translate into inferior functional or pain outcomes. On the contrary, both PROMIS function and pain interference scores improved well beyond the MCID in both groups, with the DMMO cohort showing superior functional gains. This apparent discordance highlights that for many patients, improved function and pain relief are likely more meaningful than the cosmetic appearance of a perfectly straight toe.
Complication rates fall within the ranges previously reported in the literature and similar between groups.10 -12 Hardware prominence and transient neuropathy were the most frequent issues, both resolving without sequelae. Non-union occurred only in the DMMO group (2%), confined to lesser metatarsals. Three of these patients remained asymptomatic and required no further intervention, whereas in 1 case revision surgery was necessary to address the nonunion. This corresponds to a low overall rate, consistent with previously published reports on the procedure. 17 Superficial infection occurred in 1% of cases, treated successfully with oral antibiotics.
This study has several limitations. First, the retrospective design is prone to selection bias; to mitigate this, we included consecutive patients from 2 high-volume centres and applied strict inclusion and exclusion criteria to minimize confounding. Second, the 12-month follow-up may underestimate late recurrence or complications; however, all patients had complete clinical and radiographic data through 1 year, providing reliable short-term outcomes, and ongoing follow-up is planned. Third, recurrence was defined radiographically (HVA > 20 degrees), which may not always correlate with clinical symptoms; to address this, we complemented radiographic assessment with validated PROMIS domains and VAS scores, demonstrating that functional outcomes remained robust even in cases of mild radiographic recurrence. Fourth, although the sample size was adequate for detecting between-group differences in recurrence, subgroup analyses (such as patients with severe deformities or comorbidities) may have been underpowered; we attempted to minimize this by conducting power calculations a priori and ensuring balanced baseline characteristics between groups. Fifth, radiographic evaluation relied on weightbearing radiographs, to reduce interobserver variability, measurements were performed independently by 2 fellowship-trained surgeons with a third review in case of disagreement. Although radiographic measurements demonstrated good to excellent reliability, some degree of measurement variability is inherent to angular assessment on weightbearing radiographs and may have influenced absolute values. Finally, it is possible that patients who underwent combined MICA and DMMO represented more severe or technically demanding cases, 24 potentially predisposing them to higher recurrence rates; we sought to account for this by reporting detailed baseline deformity parameters, which did not differ significantly between groups, and by standardizing surgical technique across both centres. This study reflects a real-world cohort of day-to-day hallux valgus patients rather than a highly selected subgroup. As such, we did not stratify exclusively by deformity severity, which enhances the generalizability of the findings but limits conclusions regarding outcomes in severe cases specifically. Further studies focusing on patients with higher baseline deformity will be necessary to determine whether the recurrence rate is disproportionately elevated among those undergoing combined MICA and DMMO.
Several potential sources of bias were considered in the design and analysis of this study. To reduce selection bias, consecutive patients were included from 2 high-volume foot and ankle centres, and standardized surgical techniques and postoperative protocols were applied. Measurement bias was minimized through standardized acquisition of weightbearing radiographs and uniform administration of patient-reported outcome measures at predefined time points. Confounding by indication is an inherent limitation, as patients undergoing combined MICA and DMMO presented with concomitant central metatarsalgia and potentially greater baseline symptom burden, which may have influenced preoperative functional scores. This study was designed as a comparative cohort analysis with a prespecified primary endpoint of radiographic recurrence, and the sample size was powered accordingly; therefore, adjusted multivariable analyses were not performed.
The findings suggest that although combined MICA and DMMO can optimize functional outcomes and address concomitant metatarsalgia, it carries a substantially higher risk of radiographic recurrence. Surgeons must carefully weight these trade-offs and consider patient-specific pathology before selecting combined procedures. Future prospective studies with long-term follow-up are needed to clarify the biomechanical effects of DMMO on first ray stability and whether adjunctive techniques can mitigate recurrence risk.
Conclusion
Both isolated MICA and combined MICA+DMMO yield meaningful clinical improvement in hallux valgus, with PROMIS pain and function gains exceeding MCID thresholds. Although the combined procedure produced slightly better functional outcomes, it was associated with a markedly higher radiographic recurrence rate compared with MICA alone. Notably, mild recurrence did not correlate with worse patient-reported outcomes at 12 months, underscoring the dissociation between radiographic alignment and functional recovery. These results highlight a trade-off when adding DMMO: potential functional benefit at the expense of reduced first-ray stability and increased recurrence risk. Surgical selection should therefore be individualized. Further long-term studies are needed to clarify the biomechanical impact of DMMO and to explore techniques that may reduce recurrence while maintaining functional gains.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114261420163 – Supplemental material for Recurrence and Function After Minimally Invasive Hallux Valgus Correction: A Dual-Centre Retrospective Comparative Cohort Study of MICA Alone vs MICA+DMMO
Supplemental material, sj-pdf-1-fao-10.1177_24730114261420163 for Recurrence and Function After Minimally Invasive Hallux Valgus Correction: A Dual-Centre Retrospective Comparative Cohort Study of MICA Alone vs MICA+DMMO by Gil Genuth, Nadav Moses, Chris Brown, Peter Stavrou and Lukas D. Iselin in Foot & Ankle Orthopaedics
Footnotes
Ethical Considerations
Ethical approval for this study was obtained from Assuta Medical Centre, Tel Aviv, Israel (approval no. AMC 0087-25).
Author Contributions
G.G. and L.I. were primarily responsible for patient care, surgical procedures, data collection, and manuscript preparation. N.M. assisted in several surgical cases and contributed to manuscript editing. P.S. and C.B. served as mentors to the primary surgeons (G.G. and L.I.) and were actively involved in their surgical training.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Data Availability Statement
Data generated or analysed during this study are not publicly available due to patient confidentiality but are available from the corresponding author upon reasonable request.
Declaration of Generative AI and AI-Assisted Technologies in the Writing Process
During the preparation of this work, the authors used chat and ask AI in order to correct spelling and language errors. After using this tool/service, the authors reviewed and edited the content as needed and takes full responsibility for the content of the publication
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
