Abstract
Research Type:
Level 3 - Retrospective cohort study, Case-control study, Meta-analysis of Level 3 studies
Introduction/Purpose:
With total ankle arthroplasty (TAA) emerging as a prevalent treatment for advanced ankle arthritis, continual reevaluation of outcomes are critical. Current evidence associating smoking with increased rates of postoperative complications is robust, however, the literature remains inconclusive for TAA. The purpose of this study is to analyze the impact of preoperative smoking on the outcomes of TAA.
Methods:
The Nationwide Readmissions Database (NRD) was queried from 2016 to 2020 to identify 29,705 patients undergoing primary elective TAA. Patients were divided into two cohorts based on their preoperative smoking status, with 7,526 (25.3%) being active smokers at the time of surgery. Preoperative demographics, comorbidities, postoperative outcomes, cost of admission, and total length of stay (LOS) were analyzed between cohorts.
Multivariate regression analyses were conducted to identify independent predictors of postoperative outcomes other than preoperative smoking status.
Results:
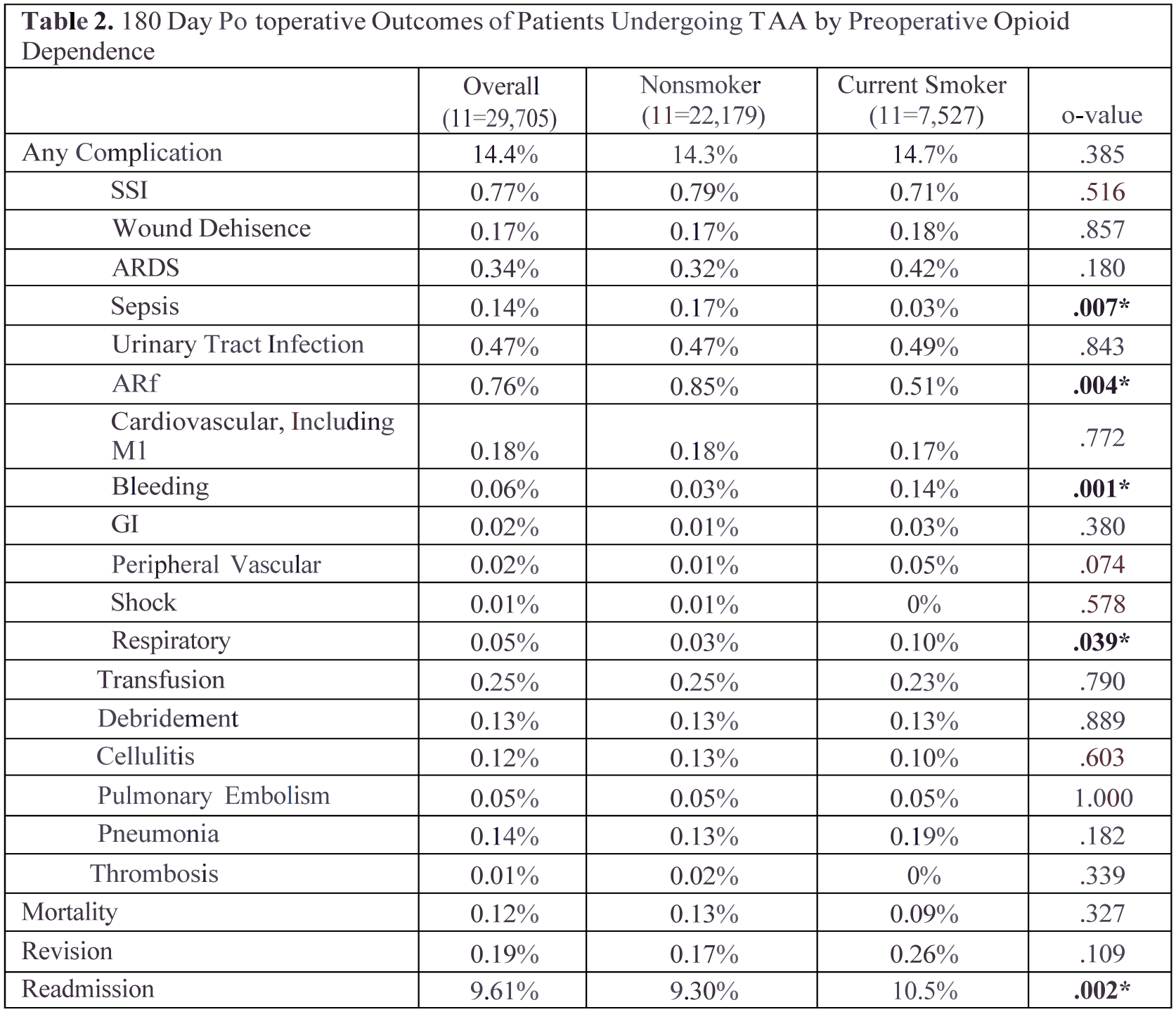
The cohort was majority male (54.2%) with mean age of 65.14 (range 17-90) years, and Charlson-Deyo Comorbidity Index (CCI) score of 0.65 (range 0-12). Active smokers were statistically significantly older (Smoker=66.75, Nonsmoker=64.6), more likely to be male (Smoker=58.81%, nonsmoker=52.66%), and had higher rates of comorbidity as measured by CCI score (Smoker=0.79, Nonsmoker=0.60). Multivariable regression showed that preoperative active smoking status was predictive of increased risk of intraoperative or postoperative bleeding (Odds Ratio [OR]=5.309), readmission (OR=1.149), and adverse discharge (OR=1.067). This analysis found active smokers to be at a decreased risk of sepsis (OR=0.163) and ARF (OR=0.451). Additionally, it was found that preoperative active smoking status was significantly predictive of over a $400 increase in total cost of admission (b=412.51).
Conclusion:
Active smokers undergoing TAA face a higher risk of intraoperative or postoperative bleeding, readmission, adverse discharge, and greater healthcare costs compared to non-smoking patients. Interestingly, active smokers have a lower risk of sepsis and acute renal failure, signaling potential areas for future research.