Abstract
Research Type:
Level 4 – Case series
Introduction/Purpose:
While surgeons can generally assure patients of positive outcomes following acute Achilles tendon repair, specific evidence-based benchmarks for early recovery counseling remain limited. Preoperative discussions about recovery expectations are critical for patient satisfaction but often lack concrete milestones. This gap between clinical experience and evidence-based guidance creates uncertainty for both providers and patients.
Particularly during the crucial early rehabilitation phase, patients seek clear recovery targets to gauge their progress. While long-term outcomes are generally favorable, the intermediate recovery phase (4-6 months) represents a critical psychological and functional transition period for patients. This study aims to provide concrete, patient-centered recovery targets that surgeons can confidently discuss during preoperative consultation based on comprehensive patient-reported outcome measures.
Methods:
From a prospectively collected institutional database (2017-2021), we identified 330 open Achilles repairs aged >18, of which 174 (52.7%) Haglund's deformity and 32 (9.7%) chronic tendinitis cases were excluded. 124 acute ruptures were analyzed, of which 101 patients completed pre-operative and 6-month follow-up (82% follow-up rate) questionnaires. All patients underwent standardized surgical repair (giftbox or modified Krakow repair) less than 6 weeks from injury and went through similar rehabilitation protocols. We assessed comprehensive recovery domains including function (FAAM ADL and Sports), pain (10-point VAS), physical and mental health (PROMIS- PH and MH), and patient satisfaction measures (Global Rating of Change (GRC)).
Results:
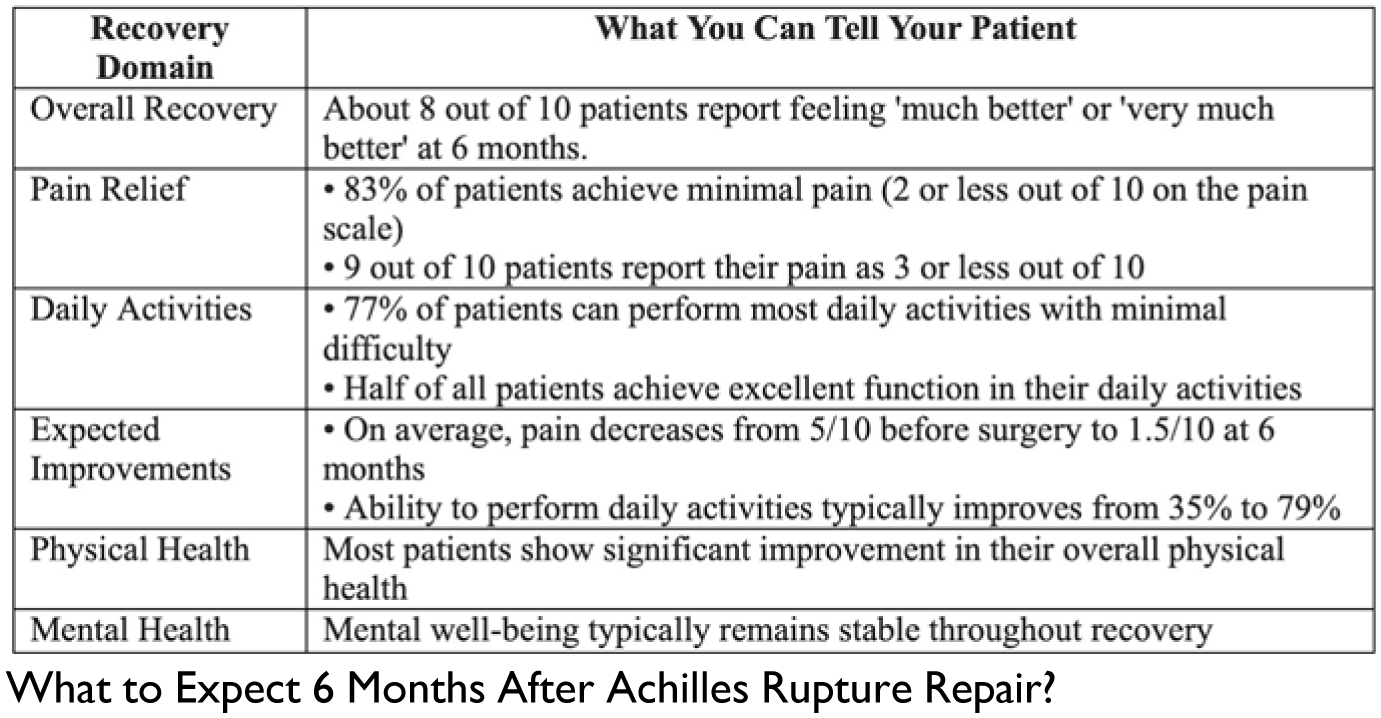
The cohort included 101 patients (78 males, 23 females), mean age 38.6 years (range: 19-71), mean BMI 28.9 ± 5.8 kg/m². At 6-month follow-up, 81% reported feeling 'much' or 'very much' better according to the GRC. Patients demonstrated significant functional gains, with FAAM ADL scores improving from 35.4 to 79.2 (p < 0.001), with 77% achieving good functional outcomes (FAAM ADL ≥70). Pain resolution was excellent, with mean VAS scores decreasing from 4.9 to 1.5 (p < 0.001), and 83% achieving minimal pain (VAS ≤2). Physical health showed significant improvement (PROMIS PH: 11.9 to 14.6, p< 0.001), while mental health scores remained stable (PROMIS MH: 14.6 to 14.7, p=0.42).
Conclusion:
Based on our institutional evidence, this study provides surgeons with evidence-based counseling benchmarks: at 6 months post-surgery, over 80% of patients report significant improvement, with most achieving minimal pain (VAS ≤2) and good functional outcomes (FAAM ADL ≥70). This can translate to an ability to safely advance patients to higher activity levels and progress through early and focused rehabilitation. These consistent improvements across measured domains, combined with high satisfaction rates, demonstrate the procedure's reliability in achieving positive patient outcomes and provide specific