Abstract
Research Type:
Level 3 - Retrospective cohort study, Case-control study, Meta-analysis of Level 3 studies
Introduction/Purpose:
Periarticular soft tissue envelope and soft tissue thickness have been found to be associated with increased risk of infection and surgical complications in primary total knee arthroplasty. Prior investigation of the soft tissue envelope in regards to total ankle arthroplasty (TAA) includes only one retrospective study of 197 patients that did not find correlation between soft tissue envelope around the ankle joint and wound complications. Multiple studies have found worse survivorship in patients who have undergone TAA with a larger body mass index (BMI). The purpose of this study was to investigate the relationship between soft tissue envelope of the ankle and calf and perioperative complications in TAA patients.
Methods:
This was a retrospective study of 124 patients who underwent primary TAA at a single academic institution between December 2015 to May 2024. Preoperative anteroposterior (AP) and lateral radiographs were analyzed for the following soft tissue measurements: thickness at the joint (STT), 10cm above the joint (STT10), 15cm above the joint (STT15), and thickness anterior to the joint. Complications analyzed were infection or wound complications, perioperative fracture, hardware loosening, dislocation, deep vein thrombosis, chronic pain requiring narcotics, and postoperative stiffness. A Point Biserial Correlation was calculated to understand if there was correlation between the patient’s preoperative soft tissue envelope and the incidence of complications.
Results:
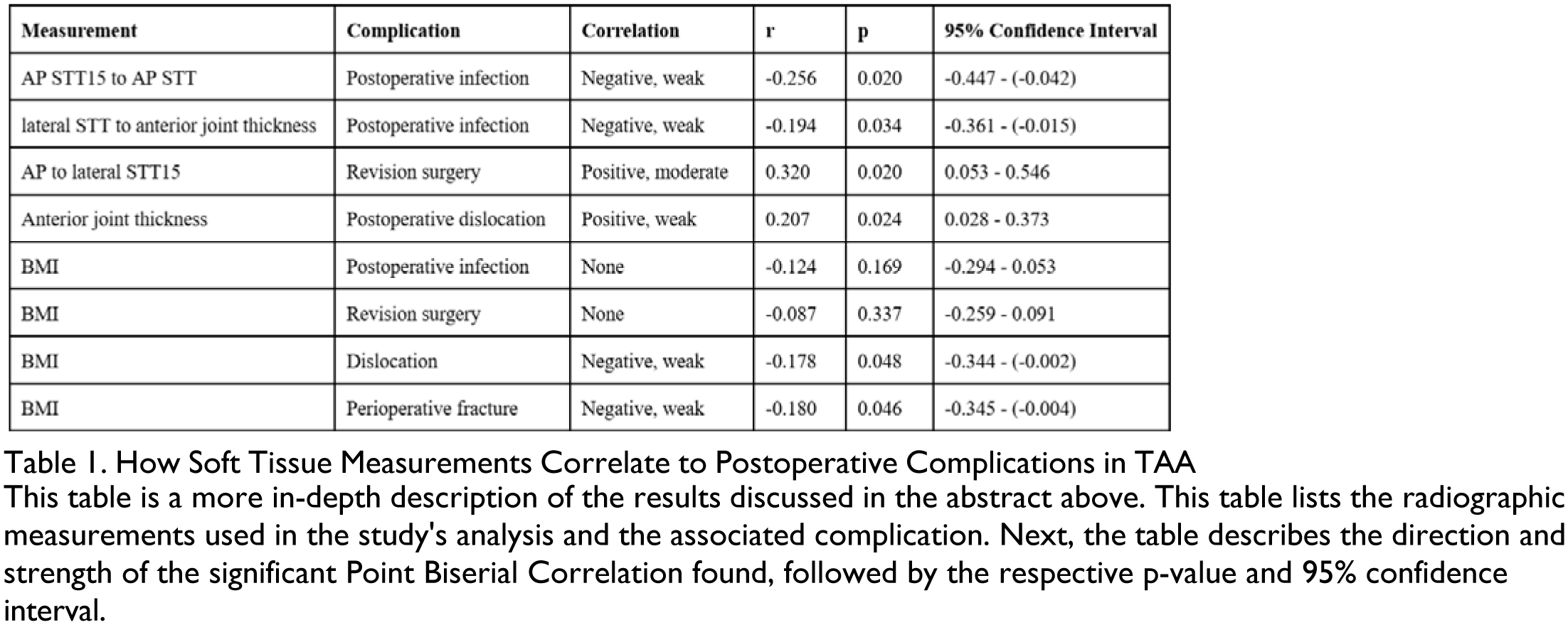
Postoperative infection was found to weakly and negatively correlate with the following ratios: AP STT15 to AP STT (r=-0.256, p=0.020) and lateral STT to anterior joint thickness (r=-0.194, p=0.034). The ratio between AP and lateral STT15 was found to moderately and positively correlate with revision surgery (r=0.320, p=0.020). Anterior joint thickness was found to weakly and positively correlate with postoperative dislocation (r=0.207, p=0.024). BMI was not found to correlate with postoperative infection or revision surgery (r=-0.124, p=0.169 and r=-0.087, p=0.337). BMI was found to weakly and negatively correlate with dislocation and perioperative fractures (r=-0.178, p=0.048 and r=-0.180, p=0.046). See Table 1 for detailed results.
Conclusion:
Patients in this cohort demonstrated that soft tissue envelope is a better predictor of postoperative infection, dislocation, and revision surgery than BMI. Patients’ soft tissue envelope may be an important risk factor for complications after TAA. Measurements corresponding to a patient’s preoperative soft tissue envelope at the calf and at the ankle may be an underutilized tool to assess potential risks associated with primary total ankle arthroplasty.