Abstract
Research Type
Level 5 - Case report, Expert opinion, Personal observation
Introduction/Purpose
Achieving stable fixation with adequate interfragmentary compression is critical for successful fracture repair and arthrodesis. We have previously demonstrated that angling locking screws away from the fracture or joint line improves compression and contact area in foam bone surrogates; however, the interaction between screw angulation and insertion sequence has not been fully defined or validated in cadaver bone. This study aimed to elucidate how varying screw insertion orders and angulations can maximize interfragmentary compression and enhance fixation stability.
Methods
Two experimental sets were conducted. In the first experiment, Sawbones samples were plated according to manufacturer guidelines using a four hole plate (2 locking, one non-locking compression, and a final locking screw) and assigned to one of four conditions: (1) all screws angled 30° away from the fracture, (2) first two locking screws inserted perpendicular followed by two screws angled 30°, (3) first two locking screws angled 30° with the remaining two perpendicular, and (4) all screws inserted perpendicular to the plate (0° angulation). Interfragmentary compression and contact area were quantified using TekScan Evolution pressure-sensitive film, with data analyzed via one-way ANOVA and Tukey post hoc comparisons. In the second experiment, paired cadaver specimens underwent a 2nd tarsometarsal fusion procedure to validate the Sawbones findings under a clinically relevant setting. This experiment leveraged similar experimental procedures, using pressure sensing film to measure compression and contact area.
Results
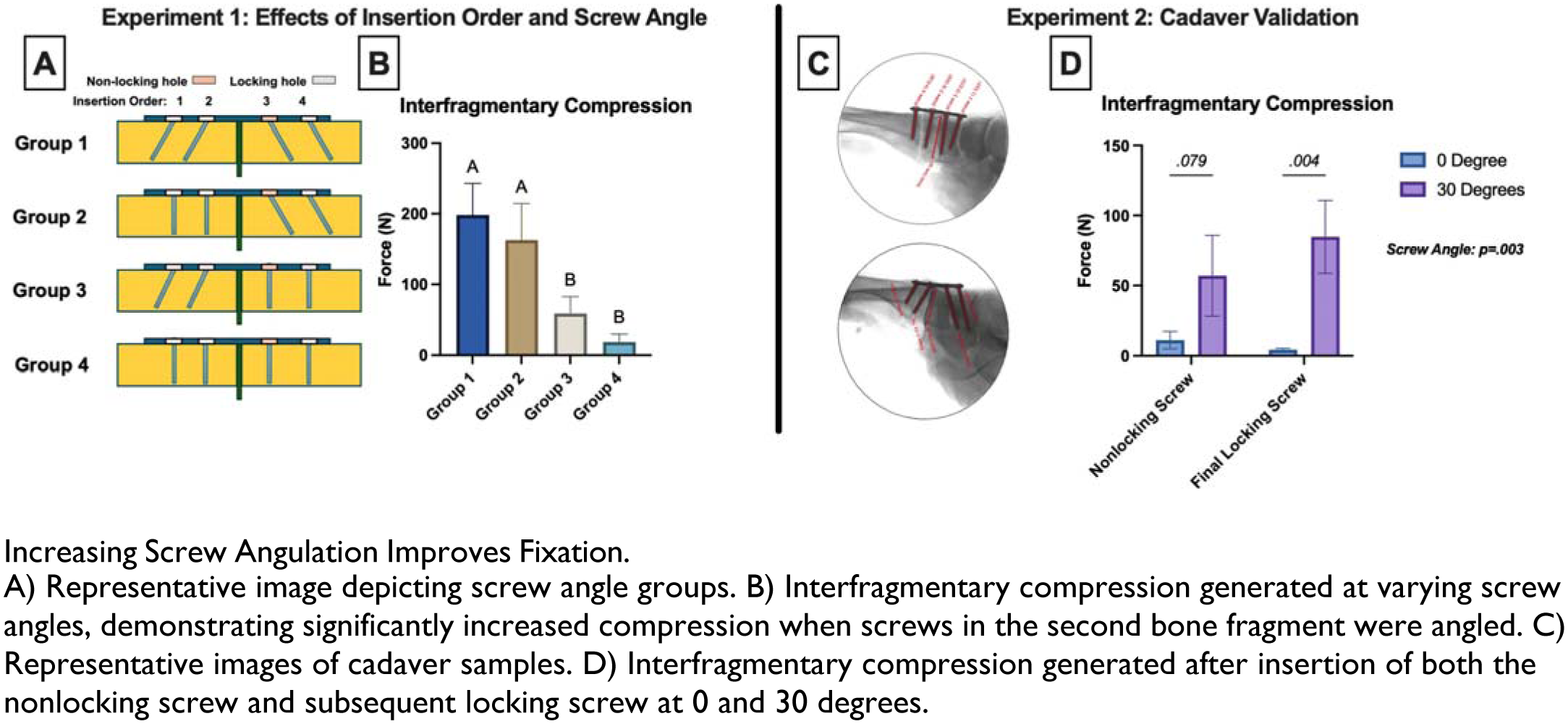
Interfragmentary compression increased significantly with screw angulation (p < 0.001). Notably, significant improvements in compression were observed only when the screws in the second bone fragment were inserted at an angle (conditions 1 and 2, p < 0.001). Likewise, contact area was enhanced, with Group 1 exhibiting a 2.9-fold increase compared to Group 4 (p = 0.01). In cadaver specimens, the insertion of screws at 30° away from the fracture line yielded a marked and significant increase in interfragmentary compression (p = 0.003) and contact area (p < 0.001), corroborating the Sawbones model.
Conclusion
Securing the plate to the first bone fragment followed by the strategic angulation of screws in the second fragment significantly enhances interfragmentary compression (19.3x) and contact area (3.2x). The study demonstrates that directing screw angulation specifically within the second bone fragment is the primary driver of improved fixation stability. These findings advocate for the use of plates that accommodate greater angulation, thereby enabling this targeted approach. By focusing on screw angulation in the second fragment, surgeons may achieve superior biomechanical outcomes, which in turn can lead to improved clinical results in fracture repair and arthrodesis.