Abstract
Research Type:
Level 3 - Retrospective cohort study, Case-control study, Meta-analysis of Level 3 studies
Introduction/ Purpose:
Post-operative swelling (POS) is a significant concern in forefoot surgery, potentially contributing to complications such as persistent pain, stiffness, or wound breakdown. Accurate assessment of swelling could improve post-operative monitoring and guide rehabilitation. Traditional volumetric methods, such as water displacement or optoelectronic techniques, require additional equipment and can be impractical in routine clinical settings. Cone-beam weightbearing CT (WBCT) is increasingly used for pre- and post-operative radiographic evaluation, offering a potential opportunistic approach for swelling assessment without added technical burden.
However, its role in quantifying soft tissue changes post-surgery remains unexplored. This study aimed to evaluate post-operative edema using WBCT in patients undergoing forefoot surgery. We hypothesized that swelling would increase from pre-op to 1 month post-op, followed by a decrease at 3 months.
Methods:
This IRB-approved, retrospective, single-center, paired comparative study included 29 feet with available WBCT imaging pre-operatively, at 1 month, and at 3 months post-operatively. Surgery consisted of a mini-open Chevron osteotomy, with 17.2% undergoing additional lesser toe realignment via percutaneous osteotomy and 58.6% undergoing distal metatarsal metaphyseal osteotomies (DMMO) of the 2nd-4th metatarsals. CubeVue software (CurveBeamAI, Hatfield, PA, USA) was used for standard Hallux Valgus (HV) measurements, including first metatarsophalangeal (MPA), sesamoid rotation (SRA), and intermetatarsal (IMA) angles. Slicer 3D (slicer.org) was used to segment bone and soft tissue volumes, with soft tissue (ST) defined by a Hounsfield Unit (HU) threshold of -500 to +500 and bone and soft tissue (BST) by -500 to +3000. Normality was assessed using the Shapiro-Wilk test. Friedman’s test was used for repeated-measures comparisons, with post-hoc pairwise analyses performed using Nemenyi’s test. Significance was set at α=0.05.
Results:
Mean age was 58.5 ± 14.2 years. Preoperative IMA, HVA, and SRA were 14.52 ± 2.16, 29.1 ± 7.92, and 25 ± 9.98, respectively. Soft tissue (ST) volume increased by 9.25% (95% CI 6.37–12.14) at 1 month, then decreased by - 4.02% (95% CI -6.7 to -1.33) at 3 months (overall change: 4.58%, 95% CI 1.88–7.28, p < 0.001). Volume increase was highest in DMMO cases (12.4% ± 7.6) vs. toe realignment (5.3% ± 2.7) and isolated 1st ray (4.3% ± 6.2, p = 0.02). At 3 months, patients with IMA ≥ 14° had a significantly greater soft tissue volume increase at whilst those < 14° had a volume decrease (3.7 ± 4.75 vs. -1.31 ± 7.98, p = 0.046).
Conclusion:
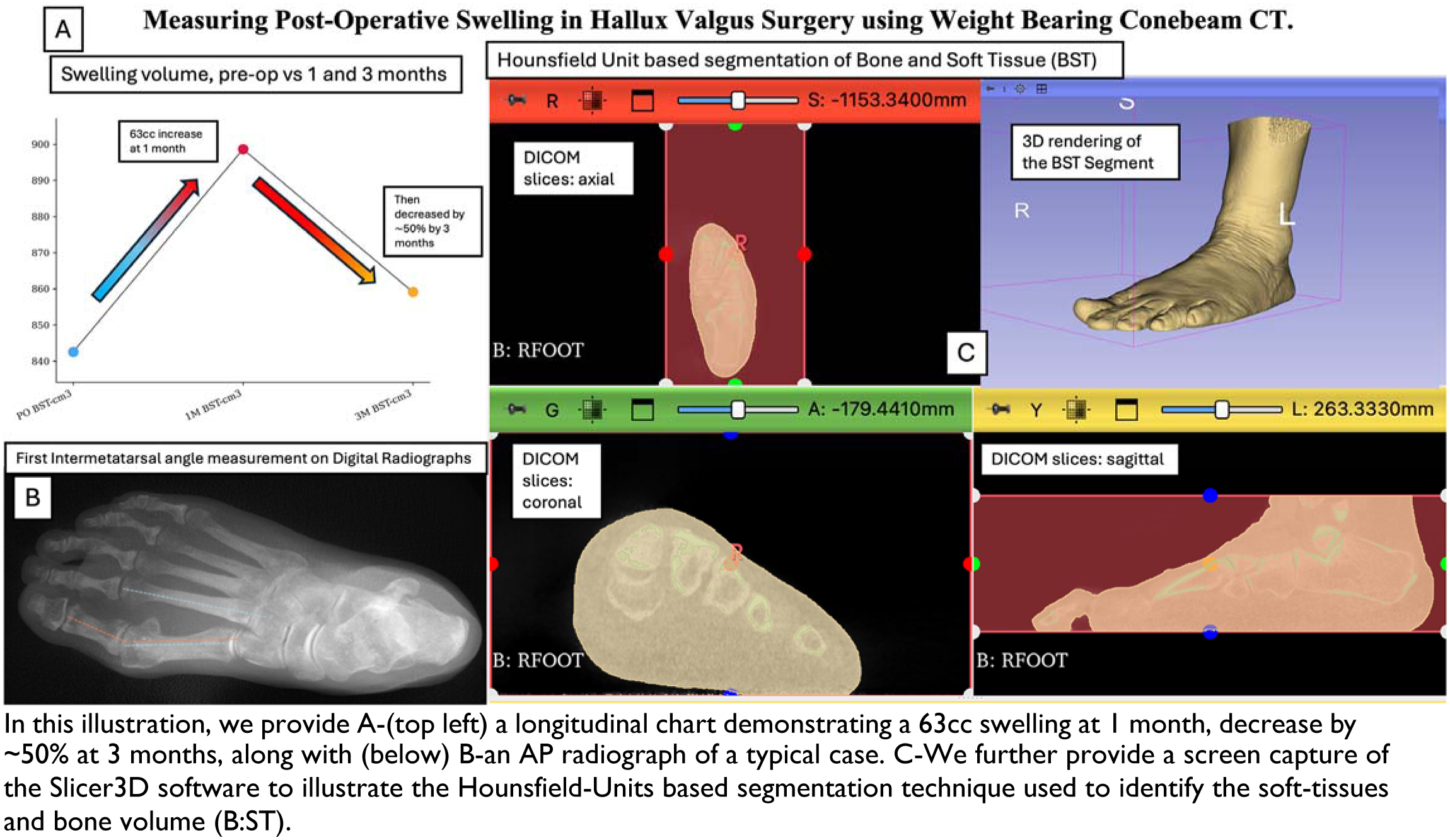
WBCT-based soft tissue volume measurements showed a significant 69 cm³ increase at 1 month, followed by an ∼50% decrease at 3 months. Swelling was greater in combined 1st ray + DMMO cases than in isolated 1st ray cases. At 3 months, cases with IMA >14° had more residual swelling than IMA < 14°. These findings align with prior literature. Compared to optical methods, WBCT enables objective swelling assessment without additional devices or radiation exposure when already used for follow-up. This opportunistic use may improve post-operative monitoring in forefoot surgery.