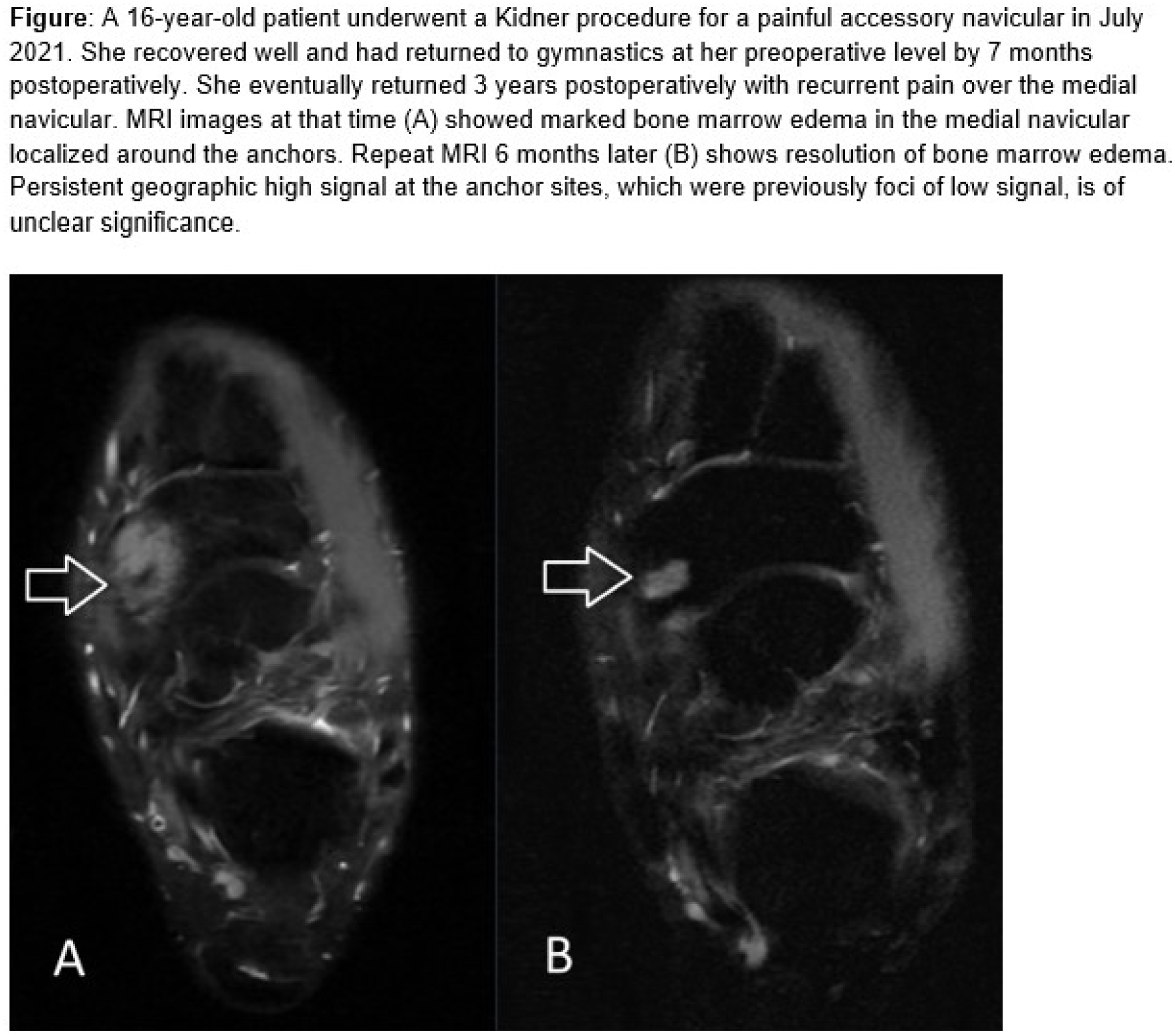
Abstract
Research Type:
Level 3 - Retrospective cohort study, Case-control study, Meta-analysis of Level 3 studies
Introduction/Purpose:
Bioresorbable orthopedic implants have proliferated in recent years, including suture anchors, soft tissue scaffolds, and screws. One such device is a bioresorbable polymer suture anchor (the SonicAnchor™ [Stryker, Michigan, USA]). This anchor utilizes ultrasonic technology to liquefy the anchor tip, allowing it to interdigitate with surrounding cancellous bone. With its small 2.5 mm footprint and high pull-out strength, it has become popular in foot and ankle procedures. Although there are reports in the literature of inflammatory reactions to various bioresorbable implants, there are no reports on complications associated with use of this particular anchor. At our institution, we have anecdotally noticed late inflammatory reactions in the bone surrounding these anchors.
Therefore, we aimed to identify and characterize complications associated with this bioresorbable suture anchor.
Methods:
We conducted a retrospective review of foot and ankle procedures utilizing the bioresorbable anchor, using a prospectively-collected foot and ankle registry. A total of 62 patients underwent foot and ankle surgery with at least one of these implants between November 2018 and January 2023. In this cohort, 42 (68%) were female. Chart review was performed to identify complications, specifically pain with bone marrow edema (BME) surrounding the anchor(s), as detected on magnetic resonance imaging (MRI). The primary diagnoses of patients included ankle instability (n=22), insertional Achilles tendinitis (n=16), flatfoot/accessory navicular (n=9), ankle fracture (n=8), and other conditions (n=7). Patients were also classified according to their level of physical activity: inactive, recreational, or collegiate. Patients with and without BME were compared to each other using two sample t-tests for continuous variables and Pearson chi square tests for categorical variables.
Results:
Of the 62 patients who received a bioresorbable anchor, 20 (32%) developed an inflammatory response, identified at a mean of 27 months postoperatively. Of the 20 patients who had anchor-associated BME on MRI, 4 (20%) were identified ≤1 year postoperatively; the remaining 16 (80%) were identified more than 2 years postoperatively. There was no significant difference in age and BMI between groups (Table). Anchor-associated BME was identified more often in female patients (p=0.047). Primary diagnosis was associated with occurrence of BME, with a diagnosis of ankle fracture more common in the BME group (p = 0.039). No significant association was found between physical activity level and development of BME. All but 3 cases (15%) of late BME resolved with nonoperative treatment.
Conclusion:
Nearly one third of the patients who underwent foot and ankle surgery with the bioresorbable anchor developed an inflammatory response. Female sex was the only significant predictor of BME. Although most symptoms resolved within a few months of nonoperative treatment, not all did. Caution should be exercised when using bioresorbable anchors. We recommend avoiding their use particularly in young, athletic female patients.