Abstract
Research Type:
Level 3 - Retrospective cohort study, Case-control study, Meta-analysis of Level 3 studies
Introduction/Purpose:
Insertional Achilles Tendinopathy (IAT) is a challenging pathology that often resists conservative treatments. While traditional open surgical approaches effectively address IAT, they are associated with complications such as wound healing delays, infections, and prolonged recovery. This study evaluates the outcomes of a Minimally Invasive Surgical (MIS) technique employing an arthroscopic-assisted double-row repair compared to traditional open double-row repair, assessing its potential benefits in reducing postoperative morbidity and improving recovery.
Methods:
67 patients with insertional Achilles tendinopathy were followed prospectively from June 2021 to January 2024, with 24 completed with MIS and 43 completed with a standard open incision. The MIS procedure utilized a percutaneous double-row Achilles tendon repair combined with endoscopic calcaneoplasty to address Haglund's deformity. Patient demographics, comorbidities, and postoperative complications were recorded. Comparative preoperative and final follow-up data included Patient-Reported Outcomes Measurement Information System Physical Function (PROMIS PF) and Foot and Ankle Ability Measure (FAAM). Statistical comparisons were performed using two-tailed, paired t-tests, with p< 0.05 considered statistically significant.
Results:
Mean follow-up time was 2.5 years (range 1.0-3.5) for MIS patients and 1.3 years (range 1.0-2.0) for open patients. The MIS group demonstrated a statistically significant improvement in preoperative (26.6) to postoperative (55.7) PROMIS PF scores compared to the open repair group (33.1 to 51.3; p=0.005). Average FAAM scores improved preoperatively to postoperatively in MIS patients (28.4 to 83.9; p< 0.001) and open patients (24.5 to 85.4; p< 0.001). There was no statistically significant difference in the change in FAAM scores from preoperative to postoperative assessments between the MIS group and the open group (p=0.492). The reported complication rate was 0% (n=0) among MIS patients and 11.6% (n=5) among open patients: 4 required wound care, 1 required surgical debridement. No correlation found between wound complications and BMI.
Conclusion:
The MIS Achilles technique significantly improves outcomes for patients with Insertional Achilles Tendinopathy compared to traditional open repair. Patients undergoing the MIS procedure demonstrated reduced wound complications and improved PROMIS physical function metrics. These findings underscore the MIS approach as an alternative to open surgery, offering improved functional outcomes while minimizing postoperative complications.
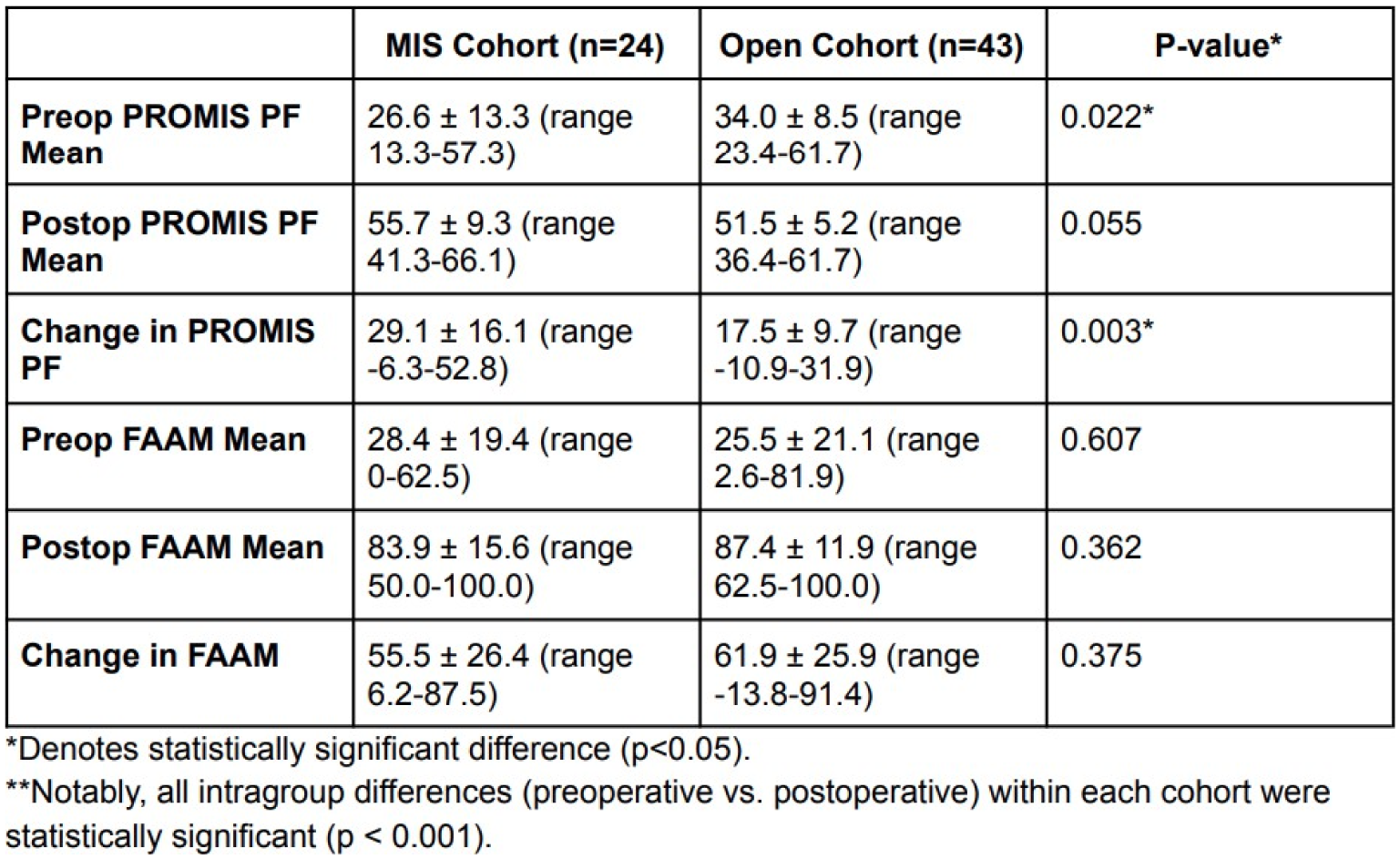
Table 1: Preoperative and Postoperative Patient-Reported Outcomes
Comparison of preoperative and postoperative functional outcomes between MIS and open Achilles repair groups, measured by PROMIS PF and FAAM scores. Statistical significance was assessed using preoperative to postoperative differences between MIS and open repair groups.
