Abstract
Research Type:
Level 4 – Case series
Introduction/Purpose:
Arthrodesis of the first metatarsophalangeal (1MTP) joint is a recognized surgical option for managing hallux valgus (HV), particularly in patients with severe, recurrent, or arthritic deformities. Clinical studies have shown that it can provide marked pain relief and functional improvement, but one key objective of HV surgery is forefoot narrowing, achieved by reducing the intermetatarsal angle (IMA). Despite evidence that 1MTP fusion can decrease the IMA, the magnitude of this correction remains uncertain, with published results varying widely. This variability likely stems from heterogeneous inclusion criteria and differences in HV severity. Therefore, this study aimed to quantify the change in IMA after 1MTP fusion in patients with strict radiographic HV criteria, and to identify factors predictive of greater correction.
Methods:
This retrospective cohort study identified 87 consecutive adult patients (mean age 69 years) who underwent 1MTP arthrodesis for HV at a single institution. Inclusion criteria required a hallux valgus angle (HVA) >20°, an intermetatarsal angle (IMA) >11°, and at least six months of radiographic follow-up. Exclusion criteria included concurrent midfoot arthrodesis, second metatarsal osteotomy, hallux interphalangeal joint fusion, traumatic deformity, nonunion, or insufficient follow-up imaging. Surgical indications encompassed severe primary HV (n=63), arthritic HV (n=8), or recurrent HV (n=16). Demographic data (age, sex, body mass index) and surgical indication were recorded from medical charts. Pre- and postoperative radiographs were evaluated for HVA, IMA, medial sesamoid position, foot width, and metatarsus adductus angle, the latter included to assess its effect on IMA correction. Bivariate analyses and linear regression were performed to identify demographic and radiographic predictors of IMA correction.
Results:
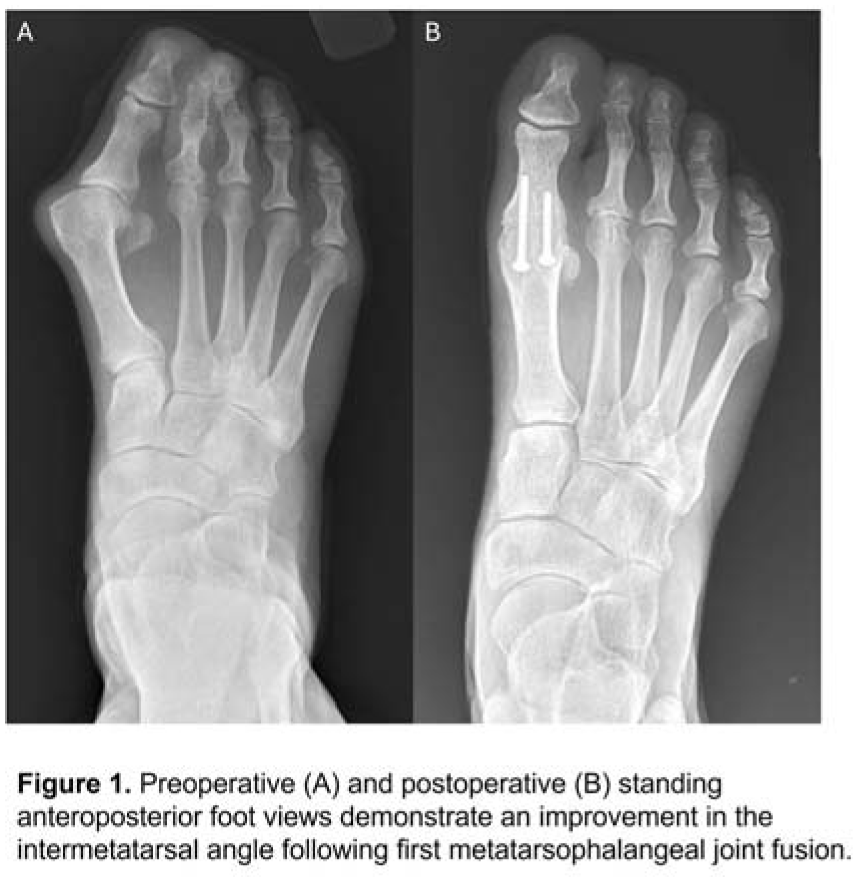
Among the 87 patients, the mean preoperative IMA improved from 15.2° to 10.1° (p <.0001, Figure 1), and the HVA from 36.2° to 14.2° (p <.0001). Foot width was reduced by 5 mm, and median sesamoid position improved from 7 to 5. Patients with preoperative IMA ≥15° had greater correction (6.3°) than those with IMA < 15° (4.0°, p<.0001). Overall, 69% reached a final IMA below 11°, and 88.5% were under 13° (1 SD above the mean, Figure 2). In multivariate analysis, older age, higher preoperative IMA, larger HVA reduction, and severe or recurrent HV were associated with greater IMA reduction, whereas arthritic HV showed less improvement. Metatarsus adductus did not significantly affect outcomes. Each degree of HVA correction yielded 0.14° of IMA improvement.
Conclusion:
In this radiographically defined hallux valgus cohort, fusion of the first metatarsophalangeal joint achieved an average 5° reduction in the intermetatarsal angle. Notably, older patients, those presenting with higher baseline angles, and individuals undergoing more substantial hallux valgus angle correction realized the greatest improvements, whereas degenerative changes limited correction magnitude. Although nearly half of patients with moderate to severe IMAs did not reach the 11° threshold, the vast majority remained within an acceptable range, and no additional operations were needed. Ultimately, further interventions for additional forefoot narrowing should be tailored to each patient’s specific clinical circumstances.