Abstract
Research Type:
Level 4 – Case series
Introduction/Purpose:
Subtalar arthrodesis is a commonly performed procedure by orthopaedic foot & ankle specialists, most often indicated in the setting of primary subtalar arthritis, post-traumatic subtalar arthritis, deformity correction, or talocalcaneal coalitions. Numerous techniques and fixation constructs have been described for primary subtalar arthrodesis with generally favorable union rates and other patient outcomes. However, many of these techniques pose challenges to the surgeon such as unfavorable patient/surgeon positioning, difficult instrumentation/screw trajectories, high reliance upon fluoroscopy, and/or difficulty manipulating subtalar alignment and instrumenting simultaneously. A crossed screw construct, as described here, aims to minimize certain challenges encountered with other subtalar arthrodesis constructs while achieving the same standard of excellent union rates and low complication rates.
Methods:
A retrospective review was performed for patients who underwent subtalar arthrodesis between January 2017 and December 2022 with any of four foot and ankle surgeons at a single institution. Immediate post-operative radiographs were screened for the crossed screw construct, and patients were eligible for inclusion if primary subtalar arthrodesis was performed for diagnoses of primary subtalar arthritis, post-traumatic subtalar arthritis, post-infectious subtalar arthritis, hindfoot deformity correction, or talocalcaneal coalition. Patients were excluded for a primary diagnosis of Charcot arthropathy, simultaneous/previous ankle or other hindfoot arthrodesis, simultaneous/previous total ankle arthroplasty, simultaneous calcaneal osteotomy, or less than 6 months of follow up. Ninety-nine feet in 96 patients ultimately met inclusion criteria. Demographic data, smoking status, and comorbidities were collected for each patient included. Post-operative data including length of clinical and radiographic follow up, radiographic union, symptomatic malunion, infection, symptomatic hardware, fracture, talar AVN, and secondary procedures were collected and analyzed.
Results:
The average age of patients included was 51.5 years with an average of 26 months of radiographic follow up. Of the 99 subtalar crossed screw arthrodesis procedures included, radiographic union occurred in 95.9% and only 2 patients (2.02%) underwent reoperation for nonunion. Two patients with concern of radiographic nonunion during the follow up period had evidence of partial bridging on subsequent imaging and did not require revision surgery.
Symptomatic hardware was noted in 7 patients (7.07%) with 5 patients (5.05%) ultimately requiring hardware removal. The overall rate of secondary surgery for the group was 14.14% with other reasons including deep infection (1.01%), malunion (3.03%), and symptomatic adjacent joint arthrosis (3.03%). No cases of talar AVN were noted during the follow up period.
Conclusion:
A crossed screw subtalar arthrodesis construct, as described here, provides successful outcomes with regards to high rates of union and low complication rates. Hardware removal rates with this construct are lower than many reported constructs for subtalar arthrodesis while avoiding a posterior heel incision, decreasing reliance on fluoroscopy by utilizing palpable anatomic landmarks, and providing easier screw trajectories for instrumentation in the supine position.
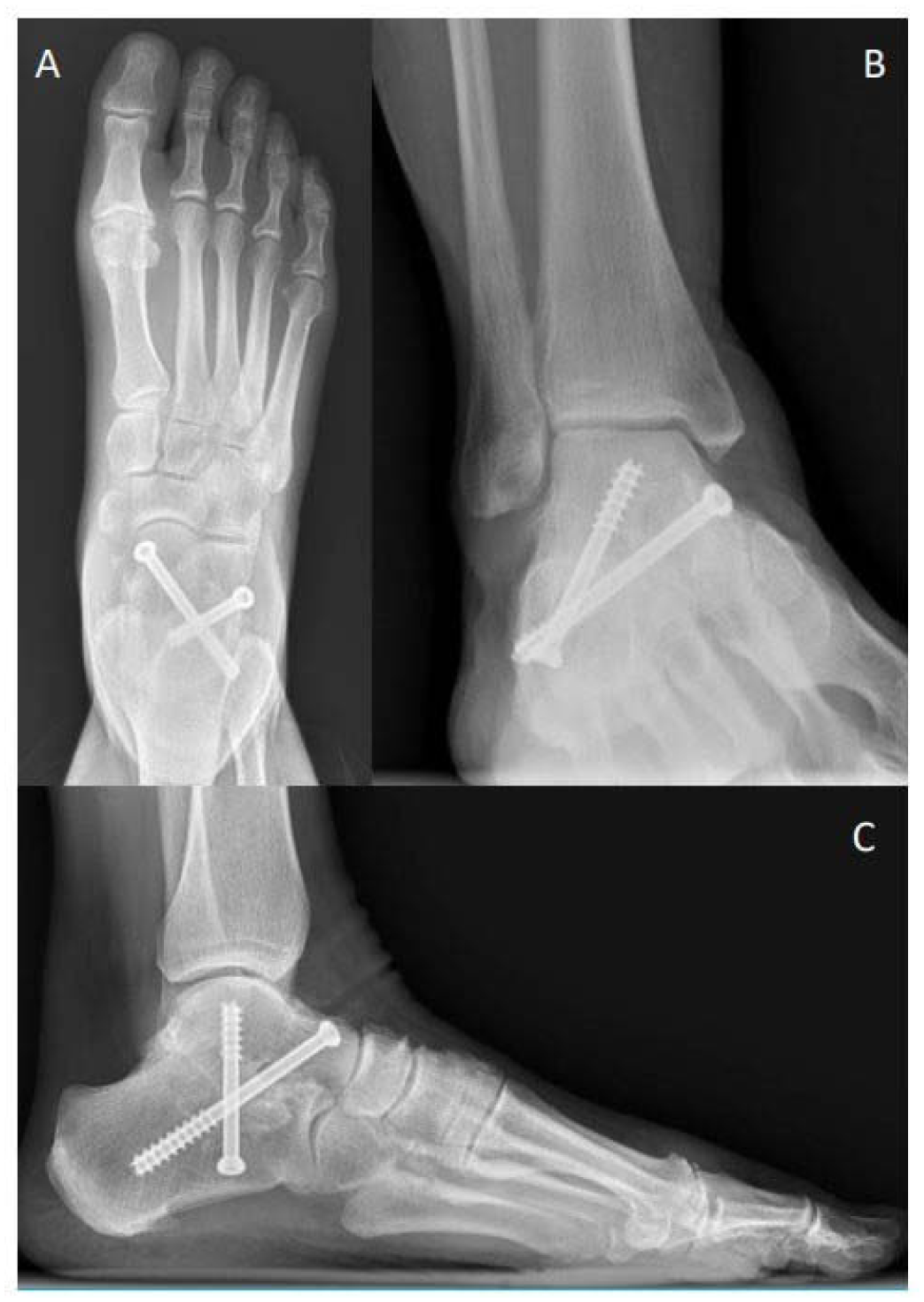
Post-operative radiographs of subtalar arthrodesis crossed screw construct
Figure 1. Post-operative AP foot (A), ankle oblique (B), and lateral (C) radiographs demonstrating a crossed screw subtalar construct with a dorsal to plantar screw from the dorsomedial talar neck into the posterolateral calcaneus as well as the second screw starting on the plantar lateral calcaneus in the midline aimed into the medial talar dome.
