Abstract
Background:
Insertional Achilles tendinopathy (IAT) is a common cause of posterior heel pain and is often managed surgically when conservative treatment fails. Wound complications are common after Achilles surgery. Obesity is a known risk factor for such complications; however, evidence on morbid obesity (body mass index [BMI] ≥ 40) and outcomes after IAT repair is limited. This study evaluates the incidence of complications and pain relief in patients undergoing IAT surgery by BMI group.
Methods:
This is a retrospective cohort study. All patients with an established diagnosis of IAT who underwent an Achilles central splitting, detachment, debridement, and reattachment surgery between 2015 and 2023 were included. Patient demographics, surgical outcomes, and reported pain (visual analog scale for pain [VAS] scores) were collected. Patients were categorized into 2 BMI groups: <40 and ≥40. Statistical analysis included independent t test, Fisher exact, and χ2 testing.
Results:
There were 123 patients in this study, of which 90 had BMI <40 and 33 had a BMI ≥40. The mean age was 53.6 ± 10.6 years. Twenty-four had documented complications: higher in the morbidly obese group (30.3%) than in non–morbidly obese patients (15.6%, P = .077), with a significantly increased rate of wound dehiscence (24.2% vs 8.9%, P = .035; relative risk 2.72, 95% CI 1.11-6.67). VAS scores were highest in patients with BMI ≥40 compared to BMI <40 both preoperatively (P = .003) and at their final follow-up appointment (P = .006). No difference was found in change in VAS scores from preoperative to final follow-up visits (P = .818).
Conclusion:
Morbid obesity was associated with increased wound complications and higher levels of pain in this retrospective cohort undergoing IAT surgical repair. However, VAS reduction after surgery was comparable across BMI groups.
Level of Evidence:
Level III, retrospective cohort.
Introduction
The posterior heel is subject to poor blood flow and large, repetitive forces that predispose it to overuse pathology such as insertional Achilles tendinopathy (IAT). 1 Commonly described as an overuse injury, IAT accounts for more than 20% of all Achilles tendon pathology and is characterized by mobility-limiting pain, erythema, and swelling over the posterior heel.1,2 First-line treatments of IAT are conservative, including physical therapy, heel lifts, and shock wave therapy.1,2 When these treatments fail, surgery is indicated, including procedures such as simple tendon debridement, resection, reattachment with Haglund resection, and possible flexor hallucis longus tendon transfer. Complications that occur after repair include diminished wound healing, infection, deep vein thrombosis (DVT), pulmonary embolism (PE), recurrence of IAT, and tendon rupture.1,3
Multiple studies have found that inflammatory conditions such as obesity, diabetes, and autoimmune disease increase the likelihood for developing IAT.4 -6 Klein et al 4 found that patients who are overweight or obese are nearly 7 times more likely than those with a normal BMI to develop IAT. This population is growing, with 90% of Americans predicted to be overweight or obese by the year 2030. 7 Therefore, the scientific and clinical understanding of IAT in these populations is of increasing importance.
It is well documented that obesity has been associated with the development of surgical and wound healing complications. 8 In patients with primary repair of the Achilles, several large studies have found increased rates of postoperative wound complications in obese patients.7,9,10 However, there are currently only 2 existing studies examining the relationship between obesity and postoperative complications after secondary repair of the Achilles tendon for IAT with conflicting findings.11,12 Notably, multiple joint arthroplasty studies have found morbid obesity in particular to be a predictor of postoperative complications.13 -15 With the growing size of populations at increased risk for IAT and its numerous postoperative complications, more evidence is necessary to properly assess surgical risk and postoperative outcomes.
The purpose of the present study is to examine the relationship between morbid obesity, postoperative complications, and patient-reported pain scores following IAT surgical intervention. We hypothesize that morbidly obese patients undergoing IAT surgical debridement and repair will have increased rates of surgical complications as well as increased pain scores compared with those who are not morbidly obese.
Methods
Institutional review board approval was obtained. A retrospective review of collected data was performed on patients undergoing surgery for IAT by 4 fellowship-trained foot and ankle orthopaedic surgeons from December 1, 2015, to December 1, 2023. STROBE cohort reporting guidelines were used. 16 Those >18 years of age who had undergone surgical correction of IAT as initially identified by Current Procedural Terminology (CPT) code 27654 with electronic medical record documentation of IAT correction were eligible for study inclusion. Exclusion criteria included a history of previous surgery to the Achilles of the affected extremity and a history of cancer or other immunocompromised status.
Patient demographics, surgical and postoperative outcomes, and patient-reported outcomes data were collected via a review of the electronic medical record. A history of diabetes, smoking status, human immunodeficiency virus, blood thinners use, and peripheral artery disease, were recorded. Wound complications were also documented by reviewing postoperative clinic visits. This included wound dehiscence, superficial wound complications that simply required antibiotics and local wound care, as well as deeper infections that required more invasive treatment. Additional complications included DVT, recurrence of heel pain (defined as redevelopment of heel pain at 6 months), and any need for revision surgery. Visual analog scale for pain (VAS), scored 0 to 10, was administered at preoperative and postoperative follow-up clinic visits. Included patients were divided into groups based on a body mass index (BMI) according to the WHO obesity classifications: BMI <30, those in obesity class I (30-34.9) and Class II (35-39.9), and those meeting obesity class III (above 40) criteria. 17 Those with BMI <30, in obesity class I and class II were grouped together (group 1) to examine morbid obesity (group 2) directly to those without morbid obesity.
Operative Procedure and Recovery Protocol
After the induction of general anesthesia, patients were placed prone on the operating room table. All bony prominences were well padded, and a tourniquet was applied to the operative extremity. Patients received the appropriate perioperative antibiotics. The patient’s operative extremity is prepped and sterile draped in accordance with hospital policy. A midline incision over the Achilles tendon is utilized. This incision is marked out and is approximately 6 cm in length and directly midline over the Achilles tendon and insertion. Skin is incised sharply, and blunt dissection is used until the paratenon is identified. The paratenon is sharply divided and preserved to be repaired at the conclusion of the procedure. The Achilles tendon is then centrally split, and care is taken to elevate the tendon flaps off the insertion site and preserve as much tendon attachment as possible medially and laterally. The tendon flaps are then debrided of any unhealthy tendon. A posterior resection of the superior aspect of the calcaneus (Haglund deformity) is performed under fluoroscopic guidance ensuring appropriate level of resection. Posterior insertional spurs are also removed. After debridement of the Achilles tendon and removal of the Haglund deformity, the tendon is then reattached using 3 bioabsorbable suture anchors.
Postoperatively, patients were plantarflexed, immobilized in a splint, and made nonweightbearing. At 2 weeks they were placed in a boot with heel lifts and made full weightbearing. At 6 weeks, heel lifts are weaned with a goal of flat foot weightbearing at 9 weeks. Patients are taken out of the boot 1 week later. DVT prophylaxis was prescribed for 2 weeks or until weightbearing. Between the 4 different surgeons and over the course of 8 years, there were slight variations in operative procedure and recovery protocol.
Statistical Analysis
Patient demographic data were analyzed with general descriptive statistics. Fisher exact and χ2 tests were used to assess categorical data, including operative procedures and postoperative complications. All continuous data was tested for normality. Mean VAS pain scores were compared between BMI cohorts using an independent samples t test. A priori power analysis was calculated with an alpha level of .05 and power of 0.8. Based upon an established complication rate of 5% for the surgery and an expected complication rate of 25% in those with BMI ≥40, necessary sample sizes are 85 patients with BMI <40 and 28 patients with BMI ≥40, respectively.1,18 All other analyses were conducted with SPSS software version 27.0 (IBM Corp).
Results
A total of 123 patients (89 female) who received surgical treatment for insertional Achilles tendinopathy with or without Haglund deformity resection were included in this study. Group 1 (BMI < 40) consisted of 90 patients (58 female) and group 2 (BMI ≥ 40) had 33 patients (31 female). Mean BMI for the entire cohort was 34.5 ± 7.7. The mean BMI was 30.9 (95% CI 29.82-31.95) for group 1 and 44.5 (95% CI 43.24-45.80) for group 2 (P < .001). The mean age of all patients was 53.6 (95% CI 51.75-55.54) years. Mean age of groups 1 and 2 were 54.8 (95% CI 52.4-57.1) and 50.6 (95% CI 47.58-53.63) years, respectively (P = .055). A total of 25 patients (20.3%) had diabetes or prediabetes. Specifically, 18 (20.0%) in group 1 and 7 (21.2%) in group 2 (P = .779). The 95% CI for mean follow-up time was 9.68 to 13.37 months for the entire cohort, 8.66 to 13.13 months for group 1, and 9.99 to 16.51 months for group 2 (P = .263). All descriptive characteristics can be found in Table 1.
Descriptive Characteristics of Study Population by BMI.

Abbreviations: BMI, body mass index; HbA1c, glycated hemoglobin.
Five different complications were collected: wound dehiscence, recurrence, DVT/PE, traumatic injury/anchor failure, and revision surgery offered. The complication rate for all patients was 19.5% (24/123). When patients were classified into either morbidly obese (BMI ≥ 40) or not morbidly obese (BMI < 40), overall, complication rates were 30.3% vs 15.6%, respectively (P = .077). There were 8 cases (8.9%) of wound dehiscence in those without morbid obesity and 8 cases (24.2%) in those with morbid obesity (P = .035). Only 2 patients (2.2%) with BMI <40 had traumatic injury/anchor failure, whereas 2 (6.1%) with BMI ≥40 had the same complication (P = .573). No morbidly obese patients and only 1 (1.1%) non–morbidly obese patient had recurrence (P > .99). Revision was offered to zero morbidly obese and 5 (5.6%) non–morbidly obese patients (P = .323). Two (6.1%) morbidly obese patients had a DVT or PE whereas only 1 (1.1%) non–morbidly obese patient had DVT or PE (P = .175). See Table 2.
Complication Rates by BMI Group.

Abbreviations: BMI, body mass index; DVT, deep vein thrombosis; PE, pulmonary embolism; RR, relative risk.
VAS pain scores, scored 0 to 10, were collected from preoperative and final follow-up appointments. Scores ranged from 0 to 10. The mean preoperative pain scores were 5.38 (95% CI 4.78-5.88) for group 1 and 7.09 (95% CI 4.71-6.45) for group 2 (P = .003). The mean final follow-up pain scores were 2.39 (95% CI 1.86-3.30) for group 1 and 3.94 (95% CI 2.83-5.05) for group 2 (P = .006). Mean difference in pain scores were −2.99 (95% CI −3.68 to −2.3) for group 1 and −3.15 (95% CI −4.55 to −1.75) for group 2 (P = .818). Data provided in Figure 1 and Table 3.
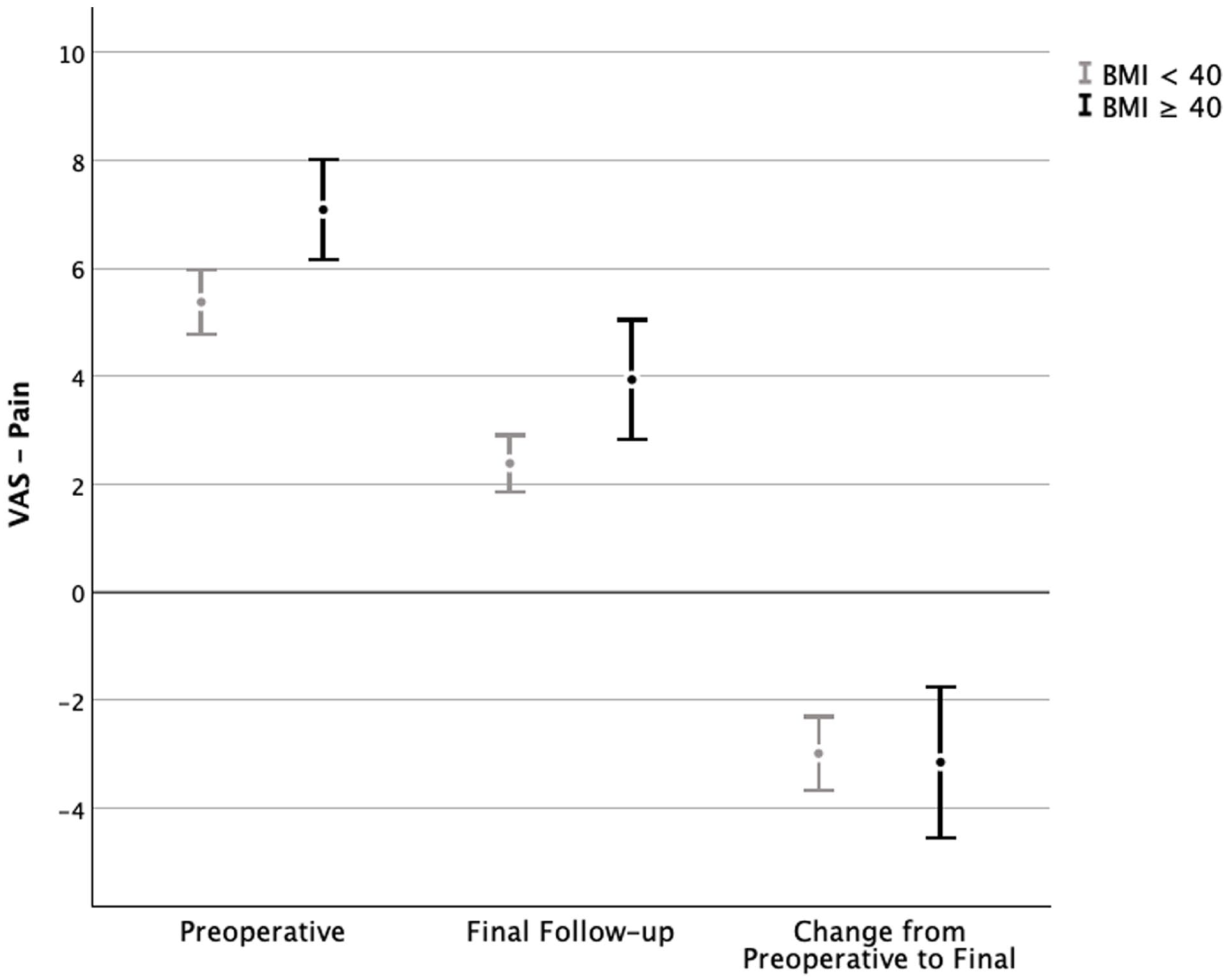
VAS pain scores by BMI group. The figure displays 95% CIs for VAS pain scores preoperatively, at the final follow-up appointment, and the change between the two.
VAS Pain Scores by BMI Group.

Abbreviations: BMI, body mass index; VAS, visual analog scale.
Discussion
This retrospective study analyzed 123 patients who underwent surgical IAT repair to investigate the association between BMI, postoperative complications, and patient-reported pain scores. Notably, patients with morbid obesity had higher wound dehiscence compared to those with lower BMI (24.2% vs 8.9%, P = .035, RR 2.72, 95% CI 1.11-6.67). Although overall complication rates did not reach statistical significance (P = .077), there was a clinically notable 2‑fold differential (30.3% vs 15.6%). No significant differences were observed in recurrence, DVT/PE, anchor failure, or revision surgery.
Pain outcomes also varied by BMI class. Morbidly obese patients demonstrated a statistically significant increase in preoperative VAS scores compared to those with a BMI <40. Despite these differences, the magnitude of change from preoperative to final postoperative VAS was similar across both groups, suggesting comparable improvement in pain following surgery.
To date, only 2 prior studies have evaluated BMI in relation to postoperative complications and outcomes following IAT repair. A study by Ptak and Rigby 11 found no differences in overall complication rates across BMI groups in a cohort of 78 patients but did not report outcomes for specific complications, such as wound issues. Morrissette et al, 12 in a larger cohort of 370 patients, identified a significant increase in wound complications in patients with BMI ≥30, although no differences were observed between obesity classes. The current study corroborates these findings, highlighting a clear association between morbid obesity and wound dehiscence.
Despite limited literature regarding IAT, the association between obesity and wound complications is well-documented in literature regarding primary Achilles repair. Burrus et al 7 and Dombrowski et al 19 were both large studies that analyzed national datasets and reported significantly increased odds of wound complications in obese patients (odds ratios 2.1 and 3.2, respectively). Similarly, Trivedi et al 10 noted an elevated risk (odds ratio 1.7) of 30-day postoperative complications in obese patients. Conversely, other, smaller studies have identified different risk factors, such as tobacco use, steroid use, and age, as stronger predictors of wound issues, underscoring the multifactorial nature of postoperative healing.20,21
The present study also contributes novel insights into pain outcomes in this population. Morbid obesity was associated with higher pain scores both pre- and postoperatively, consistent with prior literature linking obesity to greater pain severity in chronic and postsurgical settings.22,23 However, data on chronic pain outcomes following foot and ankle surgeries in obese populations remain limited, indicating an important area for future research.
This study has several limitations. As a retrospective cohort design, it is subject to inherent biases, has a relatively short mean follow‑up (~11.5 months), and lacks validated functional outcome measures such as the Foot Function Index (FFI), or 12-Item Short Form Health Survey (SF-12).24,25 The inclusion of 4 different surgeons over 8 years introduces variability in technique, potentially affecting outcomes and limiting internal validity, although this may enhance generalizability. Some analyses, particularly those evaluating more rare complications, may have been underpowered to detect statistically significant differences.
Importantly, although obesity was linked to increased wound complications, this should not be interpreted as a contraindication to surgery. Ubillus et al 8 highlights that foot and ankle pain may limit weight loss efforts, and surgery may provide meaningful relief and functional improvement. Rather than excluding morbidly obese patients, heightened preoperative counseling and perioperative vigilance are warranted.
Conclusion
This study adds to the limited literature evaluating surgical outcomes in morbidly obese patients undergoing insertional Achilles tendinopathy repair. Although these patients experienced increased rates of wound dehiscence and reported higher pain scores, their relative improvement in pain was comparable to that of non–morbidly obese individuals. Morbid obesity should not preclude surgical intervention, but both patients and surgeons should be aware of the elevated risks for wound complications and, possibly, higher levels of pain. Future prospective studies with larger sample sizes and validated functional outcome measures are needed to further clarify these associations.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251413603 – Supplemental material for Association of Morbid Obesity (BMI ≥40) With Postoperative Complications and Pain After Insertional Achilles Tendinopathy Achilles Splitting Surgical Treatment
Supplemental material, sj-pdf-1-fao-10.1177_24730114251413603 for Association of Morbid Obesity (BMI ≥40) With Postoperative Complications and Pain After Insertional Achilles Tendinopathy Achilles Splitting Surgical Treatment by Charles C. Hower, Wesley J. Manz, Param J. Desai, Rishin J. Kadakia and Jason T. Bariteau in Foot & Ankle Orthopaedics
Footnotes
Ethical Considerations
The study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethics Committee of Emory University (no. 00000652) on August 3, 2020, with the need for written informed consent waived.
Consent to Participate
Not Applicable
Consent for Publication
Not Applicable
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
