Abstract
Background:
First metatarsophalangeal (MTP) joint fusion is a common surgical procedure to treat hallux rigidus and malalignment at the MTP joint. Nonunion after first MTP arthrodesis can cause continued pain and limitation in function. The present study aims to provide a single-site analysis of nonunion risk factors after first MTP fusion. We hypothesized that diabetes, smoking, and a body mass index (BMI) ≥30 are associated with increased risk of nonunion.
Methods:
This is a retrospective cohort study. All patients who underwent first MTP fusion performed by 3 orthopaedic foot and ankle surgeons between September 20, 2013, and September 20, 2023, were included. Patient demographics, comorbidities, intraoperative medications, and postoperative complications were collected. Relationships to nonunion were evaluated using the multivariable logistic regression (a < 0.05) and both odds ratio (OR) and adjusted odds ratio (aOR) were calculated.
Results:
A total of 417 patients (450 feet) were included. Average BMI was 27.94 ± 6.79. There were 25 nonunions, which did not statistically differ in sex or age. Per-patient models identified idiopathic peripheral neuropathy and bilateral surgeries as independent predictors, with BMI ≥30 showing a trend toward significance. Diagnosis of peripheral neuropathy was subdivided into diabetic and idiopathic peripheral neuropathy, with increased nonunion rates in the idiopathic group. Osteoporosis, bisphosphonate use, and smoking history showed no statistical difference in nonunion rates. BMI and diabetes showed statistical differences with univariate logistic regression but were deemed insignificant on multivariate analysis.
Conclusion:
In this single-institution cohort, idiopathic peripheral neuropathy and bilateral MTP fusions were associated with higher odds of nonunion; findings for BMI ≥30 and diabetes should be interpreted prudently, given the limited events and wide CIs.
Level of Evidence:
Level III, retrospective cohort study.
Introduction
First metatarsophalangeal (MTP) joint arthrodesis is a common surgical procedure to treat severe hallux rigidus and malalignment of the MTP joint. It is often indicated after conservative treatment measures have failed. MTP arthrodesis is typically performed by debriding articular surfaces through the subchondral bone plate, and stabilizing in an appropriate functional position with orthopaedic hardware. This procedure is effective, with reported success rates of approximately 90% and revision rates ranging from 0 to 11%. 1
The highest reported complication is nonunion, which is defined by lack of sufficient osseous bridging at the arthrodesis site on radiographs. A review of 2818 patients reported non-union rates of approximately 5.4%. 2 Smoking, elevated body mass index (BMI), and diabetes mellitus with and without associated neuropathy have all been shown to impair bone healing and increase risk for nonunion after first MTP arthrodesis.3 -7 Other factors, such as osteoporosis, have been associated with nonunion after other non-MTP arthrodesis orthopaedic surgeries.8,9
Patient BMI >30 has been linked to various bone healing complications, including lower bone density and a higher likelihood of fracture. Additionally, patients with increased BMI are at a higher likelihood of developing diabetes and excessive inflammation, both of which impact bone healing.10 -13 An obese BMI has previously been linked to increased risk of nonunion in ankle fusions and hallux valgus corrections.14,15 However, studies specifically examining first MTP arthrodesis have found no correlation of obesity with nonunion.16,17
To date, there are conflicting results in the literature regarding the risks for nonunion after first MTP arthrodesis. This may be attributed in part to standardized studies with limited sample sizes, or large databases without standardized single institutional technique. The present study aims to provide an expansive single-site analysis of risk factors for nonunion after primary first MTP arthrodesis to clarify previously reported associations in the literature. We hypothesized that diabetes, smoking, and a BMI greater than 30 would be significant risk factors in the development of nonunion.
Methods
Following IRB approval, a retrospective review of prospectively collected outcomes data was conducted for all patients undergoing MTP arthrodesis by 3 foot and ankle fellowship-trained orthopaedic surgeons from September 20, 2013, to September 20, 2023. Included patients were identified by Current Procedural Terminology (CPT) code 28750: metatarsophalangeal arthrodesis of the great toe. All patients without confirmed electronic record of primary first MTP arthrodesis or postoperative follow-up were excluded. Data were collected and analyzed both by foot and by patient.
The primary outcome included the association of nonunion with risk factors such as diabetes, obesity, smoking, peripheral neuropathy, osteoporosis, bisphosphonate use, and wound complications. Preoperative patient demographics, intraoperative information, and postoperative outcomes were collected on a review of the electronic medical record. Preoperative demographics included sex, BMI, smoking status, diabetes, diabetic peripheral neuropathy, idiopathic peripheral neuropathy, bisphosphonate use, and osteoporosis. Diabetic and peripheral neuropathy status was confirmed by preexisting diagnosis within the electronic medical record. Diabetic peripheral neuropathy was noted if the chart contained diagnoses of peripheral neuropathy and diabetes, whereas idiopathic peripheral neuropathy was recorded if there was no preexisting diabetes diagnosis and no other underlying cause of neuropathy.
Postoperative outcome data collected included diagnosis of nonunion, bone stimulator use, and wound complications. All nonunion diagnoses were confirmed by radiographic findings in postoperative follow-up. Bone stimulator use was recorded if a bone stimulator was prescribed by their respective surgeon for the purpose of avoiding nonunion if delayed healing was observed approaching the 6-month postoperative mark. Any occurrence of wound dehiscence, superficial infection, deep infection with return to the operating room, or signs of abnormal healing with suspicion for infection were recorded as a wound complication. Superficial complications included cases where patients were prescribed antibiotics for wound dehiscence or other clinical signs of infection. Deep complications solely included cases where infection of the hardware was suspected with return to the operating room.
Operative Technique
The first MTP joint was approached from a dorsal incision, unless there was a previously performed medial approach, which was then utilized. Dissection was carried down through skin to the EHL tendon, which was retracted laterally. The capsule was incised, and medial and lateral collateral ligaments were released to allow exposure of the metatarsal head articular surface and base of the proximal phalanx. The articular surfaces were denuded of cartilage down to bleeding bone with the use of rongeurs, curettes, and/or reamers. After irrigation, a 2.0-mm drill bit was used to make several fenestrations through the subchondral bone. The joint was reduced to an appropriate position and fixed in place with a Kirschner (K)-wire. An MTP fusion plate was pinned into place, centered dorsally over the joint, with position confirmed on fluoroscopy. Locking screws were placed distally within the proximal phalanx, followed by a nonlocking screw placed eccentrically to allow for compression across the arthrodesis site. Additional locking screws were placed proximally, and K-wires removed. A 4.0-mm partially threaded cannulated screw was drilled and placed from the medial proximal phalanx to the lateral metatarsal neck to supplement compression. Hemostasis was achieved, and incisions were irrigated and closed in a layered fashion. Dressings were placed, and patients were instructed to heel-weightbear in a postoperative shoe.
Statistical Analysis
Patient demographic data were analyzed with general descriptive statistics. A univariate analysis was conducted with odds ratio (OR) calculated. Using a conservative model, variables with P <.1 and/or deemed clinically relevant were entered into a multivariate binary logistic model. Adjusted odds ratio (aOR) was then calculated. The number of variables used in the multivariate testing were limited to maintain recommendations of 10 events-per-variable in logistic regression. 18 All analyses were conducted with SPSS software version 31 (IBM Corporation).
Results
A total of 434 patients were originally collected for evaluation, with 8 exclusions due to prior MTP fusion and 9 with no follow-up documentation. A final total of 417 patients (326 female) were included that underwent primary first MTP arthrodesis by 3 orthopaedic foot and ankle surgeons. Within this cohort, 450 feet were included, with 36 patients receiving fusions on both feet at different time points.
Per-Patient Results
Of the 417 patients, there were 25 nonunions (6.00%) and 33 wound complications (7.9%) identified. Of the 25 nonunions, 16 were female (64.0%). The mean BMI of this cohort was 27.94 ± 6.79 and the mean follow-up time was 12.69 ± 11.42 months (Table 1). Thirty-six (8.6%) underwent 2 separate MTP fusions for bilateral intervention, of which 5 experienced a nonunion (OR 2.911, 95% CI 1.022-8.289, P = .045) (Table 2). The population with a BMI of 30 or greater (n = 136) had 13 nonunions, resulting in a univariate OR of 2.369 (95% CI 1.051-5.342, P = .038). There were 34 patients with diabetes, resulting in 4 nonunions and producing a univariate OR of 2.298 (95% CI 0.741-7.131, P = .15). The OR for the association between patients with any history of smoking (n = 132) and nonunion was 1.760 (95% CI 0.776-3.989, P = .176).
Demographics of per-patient population by union status.
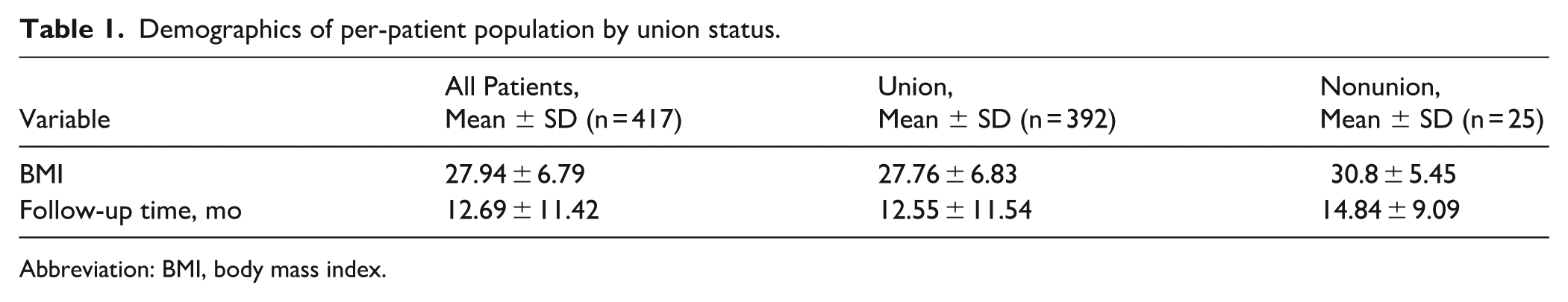
Abbreviation: BMI, body mass index.
Statistical Analysis of Risk Factors Associated With Nonunion Within the Per-Patient Population.

Abbreviation: BMI, body mass index.
Statistically significant (P < .05).
Diagnosis of any type of peripheral neuropathy (n = 21) was associated with nonunion with a univariate OR of 5.875 (95% CI 1.955-17.655, P = .002). The presence of diabetic peripheral neuropathy (n = 5) resulted in a univariate OR of 4.042 (95% CI 0.435-37.578, P = .22). The association between idiopathic peripheral neuropathy (n = 16) and nonunion produced a univariate OR of 6.032 (95% CI 1.792-20.306, P = .004).
Regarding wound complications, 29 (7.0%) patients had a superficial healing complication. Of those, 2 went to nonunion (OR 1.176, 95% CI 0.263-5.252, P = .832). Four (1.0%) patients had a deep infection requiring debridement in the operating room, with none developing nonunion (P = .999).
There were 33 patients with a diagnosis of osteoporosis, of which 1 went on to nonunion (OR 0.469, 95% CI 0.061-3.579, P = .465). There were 10 patients on bisphosphonate therapy with none progressing to nonunion (P = .999).
A multivariate analysis was performed to determine significance after controlling for other predictors. Variables included were the presence of bilateral MTP fusions, a BMI greater than 30, and a diagnosis of idiopathic peripheral neuropathy. Separate bilateral fusions produced an adjusted OR of 3.442 (95% CI 1.171-10.121, P = .025). A BMI greater than 30 showed an adjusted OR of 2.238 (95% CI 0.976-5.132, P = .057), and an aOR of 6.794 was observed for diagnosis of idiopathic peripheral neuropathy (95% CI 1.937-23.826, P = .003).
Per-Foot Results
The per-foot cohort produced similar demographics to the per-patient (Table 3). Of the 450 feet included, there were 149 with a BMI of 30 or greater, 13 which progressed to nonunion, resulting in a univariate OR of 2.302 (95% CI 1.023-5.178, P = .044) (Table 4). There were 36 feet with a prior diagnosis of diabetes, with 4 progressing to nonunion and producing a univariate OR of 2.339 (95% CI 0.757-7.229, P = .140). There were 11 nonunions that occurred within the 139 feet with prior history of smoking (OR 1.823, 95% CI 0.806-4.125, P = .149).
Demographics of Per-Foot Population by Union Status.

Abbreviation: BMI, body mass index.
Statistical Analysis of Risk Factors Associated With Nonunion Within the Per-Foot Population.

Abbreviation: BMI, body mass index.
Statistically significant (P < .05).
Prior diagnosis of peripheral neuropathy was noted in 21 feet, where 5 nonunions were observed (OR 6.391, 95% CI 2.127-19.197, P < .001). Once stratified, there were 5 feet with a prior diagnosis of diabetic peripheral neuropathy and 1 that progressed to nonunion, resulting in a univariate OR of 4.385 (95% CI 0.472-40.766, P = .194). Prior diagnosis of idiopathic peripheral neuropathy was observed in 16 feet, which produced 4 nonunions and a univariate OR of 6.556 (95% CI 1.948-22.062, P = .002).
Within the 33 feet (7.3%) that experienced postoperative wound complications, 29 (6.4%) were superficial, developing 2 nonunions (OR 1.282, 95% CI 0.287-5.725, P = .745). Four deep infection complications requiring return to the operating room were observed, with none progressing to nonunion (P = .999).
There were 35 feet with a prior diagnosis of osteoporosis, where 1 progressed to nonunion (OR 0.479, 95% CI 0.063-3.651, P = .478). Of the 11 feet on bisphosphonate therapy, none progressed to nonunion (P = .999). Sixty-nine feet had eventual bilateral MTP fusions, with 5 developing nonunion. This resulted in an OR of 1.41 (95% CI 0.511-3.893, P = .507).
Multivariate analysis was repeated within the per-foot cohort, using BMI ≥30, idiopathic peripheral neuropathy, and bilateral surgeries as variables. This produced adjusted ORs of 2.187 (95% CI 0.960-4.983, P = .062) for obesity, 6.817 (95% CI 1.946-23.885, P = .003) for idiopathic peripheral neuropathy, and 1.652 (95% CI 0.581-4.696, P = .346) for bilateral surgeries.
Of note, there were 16 feet prescribed bone stimulators because of observed delayed bone bridging, and 11 (68.8%) ultimately developed nonunion as verified by imaging.
Discussion
We hypothesized that diabetes, smoking, and BMI ≥30 would be significant risk factors for nonunion; in adjusted analyses, idiopathic peripheral neuropathy and bilateral surgeries were significant predictors, BMI ≥30 showed a trend, and diabetes/smoking were not identified as significant factors. There was no association between wound healing complications and nonunion.
Within this study, 6.0% of patients experienced nonunion, which aligns with findings by Roukis, 2 that found a nonunion rate of 5.4% in a retrospective cohort of 2818 patients. However, the present study’s nonunion rate is lower than studies reported by Molloy et al, 19 Füssenich et al, 20 and Weber et al, 16 which ranged from 9.2% to 23.5% in cohorts of 153 patients or less.
Weigelt et al 17 analyzed 165 patients for risk factors associated with MTP fusion, noting increased risk of nonunion in patients with a diagnosis of diabetes (OR = 7.4). Kachooei et al 4 further showed an increased risk of nonunion in diabetic patients within 378 feet undergoing MTP fusion. Interestingly, smaller studies evaluating MTP fusion risk factors, such as Molloy et al 19 and Reardon et al, 21 did not identify a significant relationship between nonunion and diabetes, although both were limited by small sample sizes and low diabetic representation. The present study did not find a statistically significant association between diabetes and nonunion, though diabetes was more prevalent among nonunion cases (7.5% vs 16%), likely reflecting limited power.
Diabetic peripheral neuropathy was explored for its established relationship with increased nonunion rates. Prior work by Shibuya et al 6 looked at 165 diabetic patients undergoing MTP fusion. Among the 42 patients that experienced bone healing complications, 26 had diabetic peripheral neuropathy. Additionally, they reported 44% of neuropathic patients experienced bone healing complications in comparison to only 15% in those that did not have concurrent peripheral neuropathy. Anderson et al 3 further substantiated this by looking at 76 diabetic patients undergoing MTP fusion, concluding that two-thirds of the diabetic patients with peripheral neuropathy experienced complications and had significant increased risk for malunion or nonunion. Within our study, peripheral neuropathy was associated with increased risk of nonunion (OR 5.875, 95% CI 1.955-17.655); however, it did not reach statistical significance. This was likely underpowered, with only 1 patient with diabetic neuropathy experiencing nonunion. Notably, this is the first study to find idiopathic peripheral neuropathy as an independent predictor of nonunion (aOR 6.032, 95% CI 1.792-20.306). Our review of a large cohort finds that a prior diagnosis of neuropathy, specifically, idiopathic peripheral neuropathy, is an important risk factor for nonunion following MTP arthrodesis.
Smoking status was also evaluated in the present study, with conflicting findings in prior literature. In 2013, Patel et al 5 conducted a literature review of 17 studies that had evaluated smoking as a risk factor for union complications in nonspinal orthopaedic surgeries. Contrastingly, 13 concluded smoking had a significant negative effect on bone healing. A study by Younger et al 22 in 2019 found a similar relationship between smoking and nonunion through analysis of 2301 foot and ankle fusions performed on 1320 patients. Another study by Allport et al 23 evaluating 381 joints undergoing midfoot or hindfoot arthrodesis reported that smoking had a relative risk of 5.81 for nonunion. However, Weber et al 16 found no association between smoking and nonunion rates after MTP arthrodesis within 153 patients. Other, smaller studies evaluating smoking and nonunion after MTP arthrodesis came to similar conclusions.17,19,20,24 However, a study by West et al 25 observed delayed union rates in smokers vs nonsmokers at the 12-week time point. The present study is the largest study, to our knowledge, evaluating nonunion risk after first MTP arthrodesis and validates previous findings that smoking does not increase risk of nonunion after first MTP arthrodesis. However, further research is warranted to understand how smoking affects MTP arthrodesis differently from other lower extremity fusions.
The present study identified that a BMI ≥30 significantly increases the risk of nonunion on univariate testing. However, with multivariate analysis, obesity was not found to be an independent predictor, suggesting idiopathic peripheral neuropathy and bilateral surgeries may be confounders. Previous literature has found conflicting results regarding MTP arthrodesis nonunion and BMI. Weber et al 16 and Weigelt et al 17 found no association in their cohorts of 153 and 165 patients, respectively. However, West et al 25 found lower rates of union at 12 weeks in a larger cohort of 305 patients. BMI ≥30 has been linked to bone healing complications, lower bone density, and increased risk of fractures, diabetes, and other inflammatory pathologies.10 -13 Elevated BMI has been found to increase risk of nonunion both in the ankle and in hallux valgus corrections.14,15
To the authors’ knowledge, there have been no studies examining the role wound healing complications play in the development of nonunion after first MTP arthrodesis. However, there have been multiple studies examining this relationship in fractures. Infection alters the biologic healing process, and prior studies have found that 30% to 40% of patients with long-bone nonunion after fracture had an associated infection.25 -27 This greatly contrasts with the present study, which found no association between wound healing complications and nonunion. Notably, no patients that developed nonunion experienced a deep infection requiring reoperation, limiting the power of this observation. The present study may suggest that wound healing complications play less of a role in the development of nonunion in MTP arthrodesis than in long-bone fractures.
Patients with MTP arthrodesis performed in each foot on separate occasions were found to be independent predictors of nonunion when controlled for other factors. Prior studies on MTP arthrodesis have found increased risk of nonunion with prior ipsilateral nonunion; however, there are currently no studies examining the association of contralateral surgeries with nonunion.28,29 Patients with bilateral surgeries likely have an inherent, yet-to-be identified, difference in their etiology or severity of pathology requiring surgeries in both feet that may be contributing to the increased risk of nonunion.
An incidental finding of the present study was the observation that of the 16 patients prescribed bone stimulators after delayed healing, 11 eventually developed nonunion. Bone stimulator use has continued to grow as a therapeutic option to reduce nonunion rates and promote healing across the fusion site. Although stimulator use has been studied in tibia and fibula nonunions, higher level evidence is lacking in the foot and ankle, particularly in the forefoot.30 -32 The small number of patients prescribed bone stimulators in the present study limits us from drawing further conclusions. However, this does suggest that further research is needed to assess their efficacy.
There are various limitations that should be noted within the study. This is a retrospective study with inherent limitations, and no a priori power analysis was conducted. Patient follow-up varied as only those with no follow-up were excluded. Additionally, no patient-reported outcomes were analyzed. Lastly, with only 25 documented nonunions, it is possible that some confounding variables may not show true significance within our multivariate modeling.
Conclusion
In conclusion, within this single institution cohort, nonunion occurred in 6.0% of patients; idiopathic peripheral neuropathy and bilateral surgeries were associated with higher odds of nonunion, whereas BMI ≥30 showed a trend and diabetes/smoking were not significant after adjustment. Despite the large size of the patient cohort evaluated in our study, the findings should be interpreted cautiously, given the relatively limited number of nonunion events.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251413590 – Supplemental material for Metatarsophalangeal Arthrodesis: Risk Factors for Nonunion in a 10-Year Retrospective Cohort
Supplemental material, sj-pdf-1-fao-10.1177_24730114251413590 for Metatarsophalangeal Arthrodesis: Risk Factors for Nonunion in a 10-Year Retrospective Cohort by Caroline M. Dingler, Charles C. Hower, Kevin T. Kane, Alicia G. Edwards, Rishin J. Kadakia and Jason T. Bariteau in Foot & Ankle Orthopaedics
Footnotes
Ethical Considerations
Approval for this study was granted under institutional review board committee review.
Informed Consent
A waiver of informed consent was also obtained from the institutional review board.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Rishin J. Kadakia, MD, reports disclosures related to manuscript of consultant for Enovis. Jason T. Bariteau, MD, reports general disclosures of consultant Seaspine, DJO; royalties from DJO; and stocks in Restore3d and Stridelink. Disclosure forms for all authors are available online.
Data Availability Statement
The data sets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
