Abstract
Background:
First tarsometatarsal (TMT) arthrodesis is a surgical option for moderate to severe hallux valgus, particularly in the setting of first-ray instability. The use of a supplemental intermetatarsal screw (IMS) has emerged as a technique intended to enhance transverse plane stability and may help maintain correction; however, limited clinical data exist regarding its radiographic and complication profile. This study compared radiographic correction, maintenance of alignment, and postoperative complications following TMT arthrodesis with vs without IMS fixation.
Methods:
A retrospective review was performed of adult patients who underwent first TMT arthrodesis for hallux valgus from 2013 to 2023 at a tertiary academic center. Patients undergoing additional midfoot fusion or with <6-month follow-up were excluded. Patients were grouped by whether supplemental IMS fixation was used, which was determined at surgeon discretion. Demographic, operative, and clinical data were recorded. Radiographic measurements included intermetatarsal angle (IMA) and relative first metatarsal (MT) length preoperatively, immediately postoperatively, and at latest follow-up.
Results:
Eighty-nine patients met criteria (51 IMS; 38 no IMS). Baseline demographics and comorbidities were similar between groups. Immediately postoperatively, the IMS cohort demonstrated a smaller IMA (5.8 vs 7.8 degrees, P = .010), which persisted at latest follow-up (7.3 vs 9.3 degrees, P = .015). The IMS group demonstrated a greater reduction in IMA from preoperative to final follow-up (6.9 vs 3.9 degrees, P = .001). Relative first MT length remained greater in the IMS cohort across all time points (P ≤ .045) but change‑score (Postop-Preop) differences in length were not statistically significant. Complication rates, including nonunion (2.0% vs 2.6%), revision surgery (9.8% vs 18.4%), and hardware-related complications (7.8% vs 2.6%), did not differ significantly between groups (P > .05).
Conclusion:
Supplemental IMS fixation in first tarsometatarsal arthrodesis for hallux valgus was associated with greater maintenance of radiographic correction without observed differences in complication rates. These findings support IMS augmentation as a potential adjunct in appropriately selected patients.
Level of Evidence:
Level III, retrospective review.

Introduction
Hallux valgus is among the most common forefoot deformities requiring surgical correction.1,2 First tarsometatarsal (TMT) arthrodesis, including the Lapidus procedure, is commonly performed for moderate to severe deformities or in the presence of first-ray instability.3,4 Despite high rates of deformity correction and patient satisfaction, complications such as nonunion, recurrence, and loss of correction remain concerns, particularly in cases with residual intercuneiform instability.3,5,6
To address persistent instability between the first and second metatarsals, the use of an intermetatarsal screw (IMS) has been introduced as an adjunct to TMT arthrodesis (Figure 1).7 -9 Biomechanical and clinical data suggest that an IMS enhances stabilization of the first-second metatarsal interval, which may help preserve correction and lower recurrence rates.8,10,11 However, the addition of an IMS also increases hardware load and soft tissue dissection, which may elevate the risk of complications such as nerve irritation, hardware failure, or iatrogenic joint violation. 12
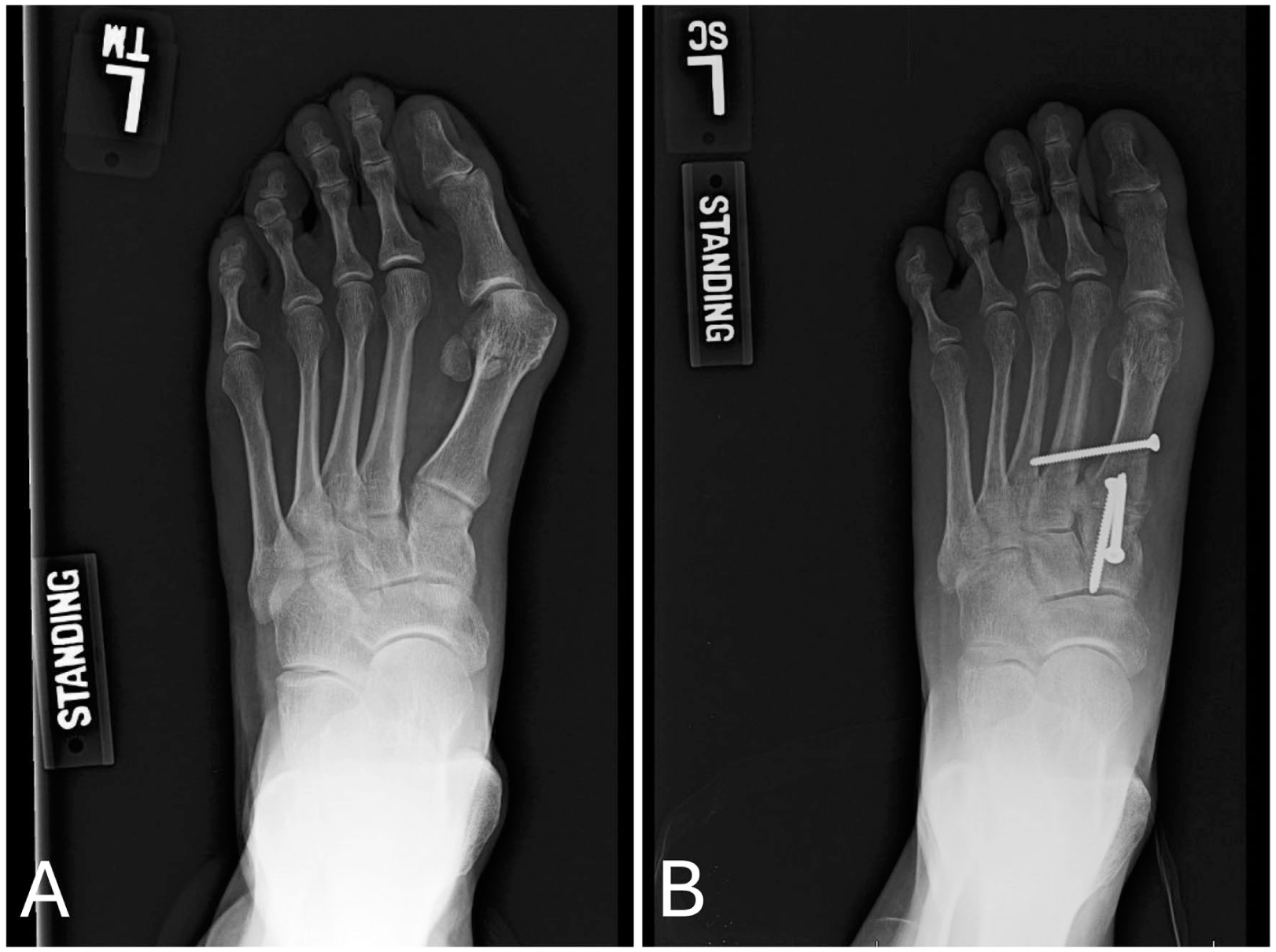
Preoperative (A) and postoperative (B) weightbearing anteroposterior radiographs demonstrating correction of hallux valgus following first tarsometatarsal (TMT) arthrodesis with intermetatarsal screw (IMS) fixation.
Although previous studies have demonstrated enhanced construct rigidity with IMS fixation,4,7,8,10,11,13 limited clinical data exist regarding its radiographic and clinical outcomes. The purpose of this study was to compare radiographic outcomes, complication rates, and clinical characteristics of patients undergoing hallux valgus correction with and without IMS fixation in first TMT arthrodesis. We hypothesized that the addition of an IMS would improve maintenance of intermetatarsal correction without increasing postoperative complication rates.
Methods
Study Design, Setting, and Participants
Following institutional review board approval, a retrospective review was conducted to identify patients who underwent first TMT arthrodesis from 2013 to 2023 at a tertiary academic medical center. Patients were identified using Current Procedural Terminology (CPT) codes 28740 and 28297. Patients were excluded who underwent fusion of rays 2 through 5, fusion involving the intermediate cuneiform, or had less than 6 months of follow-up.
Demographic and clinical variables were recorded, including age, sex, body mass index, American Society of Anesthesiologists score, tobacco use, diabetes, peripheral vascular disease, intravenous drug use, and duration of clinical follow-up. Operative variables noted were laterality, fixation method (screw-only or plate-assisted), and use of an IMS, which was determined at surgeon discretion (Figure 1). Time to full weightbearing was also recorded.
Clinical outcomes recorded were the incidence of infection requiring treatment, symptomatic nerve irritation or injury, implant failure, implant removal, nonunion, and revision surgery. Nonunion was defined radiographically as the absence of bridging trabeculae across the arthrodesis site and clinically by persistent pain or hardware failure prompting reoperation at or beyond 6 months postoperatively. 14 In addition, variation in IMS fixation by surgeon was reviewed to provide context for potential differences in surgical technique (Supplemental Table S1). All variables were collected via retrospective review of the electronic medical record.
Postoperatively, all patients were immobilized in a posterior splint and subsequently transitioned to a controlled ankle-foot walking boot. Progression of weightbearing followed a standardized institutional protocol, with advancement based on clinical and radiographic assessment at the discretion of the treating surgeon. Full weightbearing was typically permitted between 6 and 8 weeks postoperatively.
Radiographic Measurements
Radiographic parameters were measured preoperatively, immediately postoperatively, and at latest follow-up, and included the intermetatarsal angle (IMA) between the first and second ray, as well as the relative first MT length.
The IMA was measured on standardized weightbearing anteroposterior radiographs as the angle formed by the longitudinal axes of the first and second metatarsals (Figure 2). Each axis was defined by a line drawn through the midpoints of the diaphysis of the respective metatarsal shafts, consistent with the method described by Coughlin and Mann.13,15 Smaller postoperative and follow-up IMA values reflected greater correction and maintenance of alignment following arthrodesis. A normal IMA was considered ≤9 degrees, consistent with standard radiographic criteria for hallux valgus. 2

Method for measuring the intermetatarsal angle (IMA) on weightbearing anteroposterior radiographs. The angle is formed by lines drawn along the longitudinal axes of the first and second metatarsal shafts.
Relative first MT length was measured using a method previously described by Morton 16 (Figure 2). A line was drawn along the longitudinal axis of the second metatarsal, with a perpendicular line at the apex of the second metatarsal head. A parallel line was then drawn at the apex of the first metatarsal head, and the distance between these lines was recorded. Negative values indicated that the first metatarsal apex was proximal to the second (Figure 3).

Method for measuring relative first metatarsal length (protrusion) on weightbearing anteroposterior radiographs. A line was drawn along the longitudinal axis of the second metatarsal, with a perpendicular line at the apex of the second metatarsal head. A parallel line was then drawn at the apex of the first metatarsal head. The distance between these lines represents the relative metatarsal length.
All radiographic measurements were obtained using Picture Archiving and Communication System (PACS) digital tools by a single reviewer and verified by a fellowship-trained foot and ankle orthopaedic surgeon. Changes in IMA and first MT length were calculated across time points (preoperatively, immediately postoperatively, latest follow-up) to assess maintenance of correction.
Statistical Analyses
Descriptive statistics were generated to characterize the study population. Categorical variables are presented as counts and percentages and were compared using χ2 or Fisher exact test, as appropriate. Continuous variables are reported as means with SDs and were compared using independent t tests. The threshold for statistical significance was defined as a 2-sided P value of ≤ .05. All statistical analyses were performed using IBM SPSS Statistics (version 31.0.0.0).
Results
Of 311 patients identified using CPT codes 28740 and 28297, 89 patients who underwent first TMT arthrodesis for hallux valgus met inclusion criteria, of which 51 (57.3%) received an intermetatarsal screw (IMS) and 38 (42.7%) did not. The mean age of this cohort was 50.1 years (range: 18-76 years), and the mean duration of follow-up was 487.7 days (range 180-2244 days). This cohort was predominantly female (75.3%). Baseline demographic and clinical characteristics were similar between groups (Table 1). There were no statistically significant differences in age (P = .235), sex (P = .234), body mass index (P = .129), diabetes (P = .362), tobacco use (P = .546), peripheral vascular disease (P = .060), intravenous drug use (P = .326), American Society of Anesthesiologists classification (P = .178), or duration of follow-up (P = .694) (Table 1).
Baseline Demographic and Clinical Characteristics of Patients Who Underwent Hallux Valgus Correction With and Without Intermetatarsal Screw Fixation.
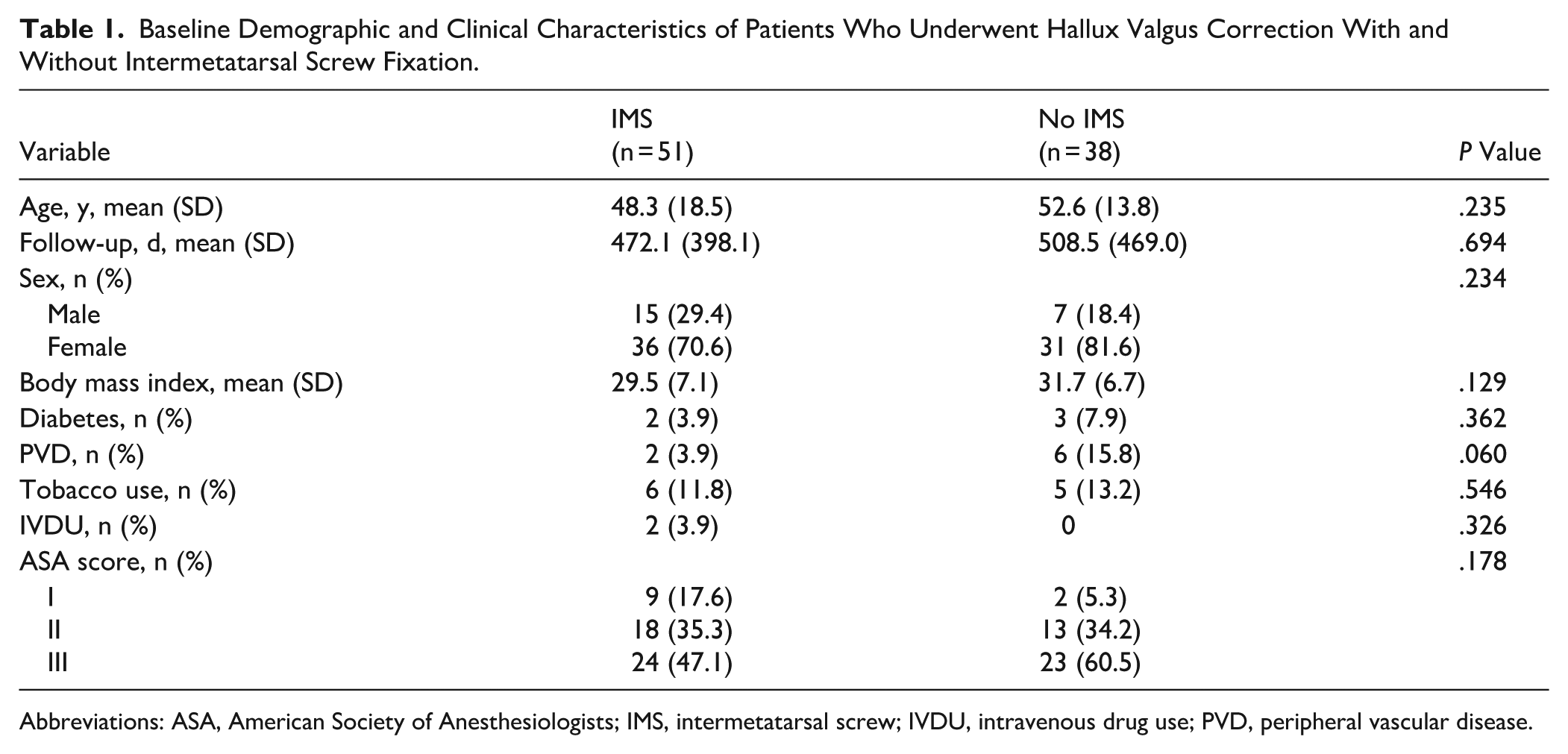
Abbreviations: ASA, American Society of Anesthesiologists; IMS, intermetatarsal screw; IVDU, intravenous drug use; PVD, peripheral vascular disease.
Operative and rehabilitation characteristics are presented in Table 2. Plate fixation was used more frequently in cases without supplemental IMS fixation (31.6% vs 13.7%, P = .042) (Table 2). Time to full weightbearing did not differ significantly between groups (47.3 vs 47.7 days, P = .943) (Table 2).
Operative Characteristics and Postoperative Rehabilitation of Patients Who Underwent Hallux Valgus Correction With and Without Intermetatarsal Screw Fixation.

Abbreviations: IMS, intermetatarsal screw; WB, weightbearing.
Boldface indicates statistical significance (P < .05).
Radiographic outcomes are summarized in Table 3. Preoperatively, the mean IMA was comparable between groups (14.2 vs 13.3 degrees, P = .299). Immediately postoperatively, patients treated with IMS fixation demonstrated a smaller IMA (5.8 vs 7.8 degrees, P = .010) (Table 3). This difference persisted at latest follow-up (7.3 vs 9.3 degrees, P = .015). The change in IMA from pre- to postoperative and from pre- to final follow-up was significantly greater in the IMS group (8.4 vs 5.5 degrees, P = .002; and 6.9 vs 3.9 degrees, P = .001, respectively) (Table 3).
Radiographic Outcomes Before and After Hallux Valgus Correction in Patients With and Without Intermetatarsal Screw Fixation.

Abbreviations: Δ, change; FU, follow-up; IMA, intermetatarsal angle; IMS, intermetatarsal screw; MT, metatarsal; postop, postoperative; preop, preoperative.
Boldface indicates statistical significance (P < .05).
Relative first MT length was consistently greater in the IMS group at all time points (Table 3). Preoperatively, the relative first MT length was −1.4 mm in the IMS group and −3.0 mm in the no-IMS group (P = .045). This relationship persisted both immediately postoperatively (−1.8 mm vs −3.6 mm, P = .014) and at latest follow-up (−1.6 mm vs −4.0 mm, P = .003) (Table 3).
Postoperative complications are shown in Table 4. There were no statistically significant differences in rates of infection (0% vs 2.6%, P = .427), nerve injury (15.7% vs 21.1%, P = .514), nonunion (2.0% vs 2.6%, P = .674), revision surgery (9.8% vs 18.4%, P = .239), implant failure (7.8% vs 2.6%, P = .285), or implant removal (9.8% vs 7.9%, P = .531) between patients with and without IMS fixation (Table 4).
Postoperative Complications in Patients With and Without Intermetatarsal Screw Fixation for Correction of Hallux Valgus.
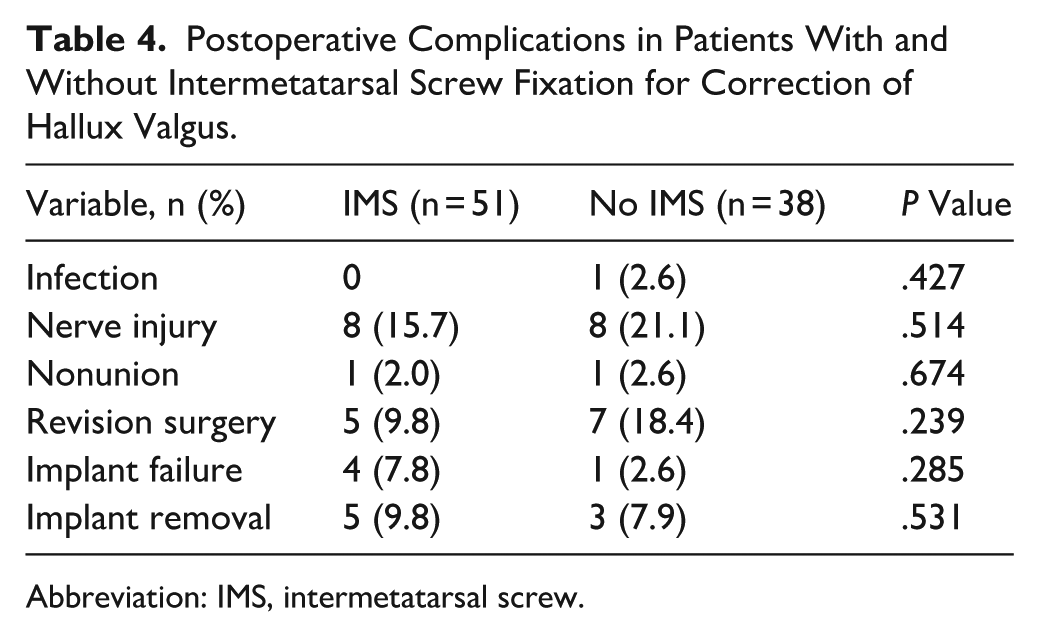
Abbreviation: IMS, intermetatarsal screw.
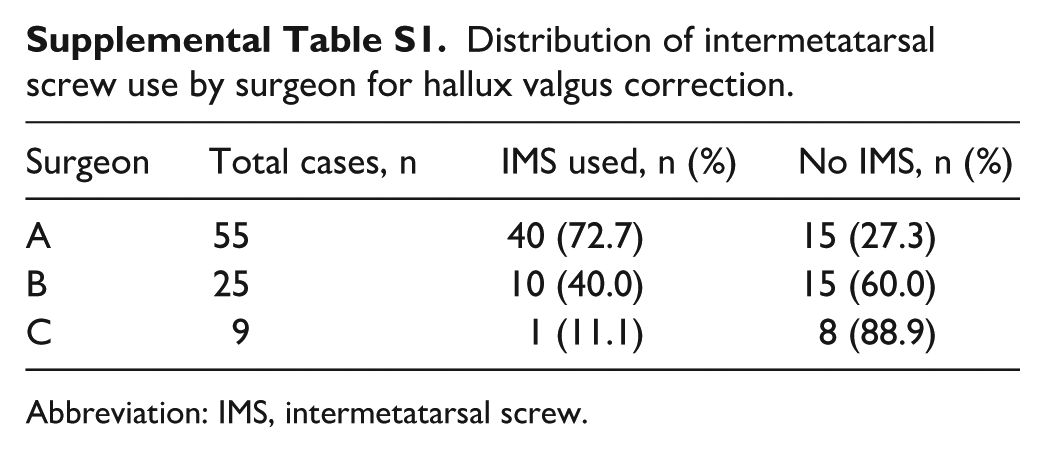
Surgeon-specific use of IMS fixation is summarized in Supplemental Table S1. Surgeon A used an IMS in 72.7% of cases, surgeon B in 40.0% of cases, and surgeon C in 11.1% of cases.
Discussion
In this retrospective study of patients who underwent first TMT arthrodesis for hallux valgus, supplemental IMS fixation was associated with greater initial correction of the IMA and improved maintenance of alignment at latest follow-up, without an increase in postoperative complications. These associations provide observational evidence that IMS augmentation may be linked to greater transverse plane stability and improved maintenance of correction, although surgeon‑level practice patterns and fixation construct differences could confound these associations. Although further investigation is warranted, IMS fixation appears to be a viable adjunct in appropriately selected patients undergoing first TMT arthrodesis for hallux valgus.
Prior investigation has demonstrated that transverse fixation across the first and second metatarsal bases can increase construct rigidity and limit intermetatarsal splay under load.7,11,17 Consistent with this, Jones et al 17 compared first TMT arthrodesis with vs without a first-second metatarsal base screw and found greater initial IMA correction (11.6 vs 7.8 degrees) and better maintenance at 1 year (change 0.5 vs 2.3 degrees) in the screw cohort. Notably, IMS placement in the Jones et al 17 study was guided by a standardized intraoperative criterion, whereas in our cohort, the decision to use IMS was made at surgeon discretion, representing a methodological difference between the studies. To contrast, Scheele et al 10 observed greater initial hallux valgus angle (HVA) reduction with intermetatarsal fusion plus a stabilization screw, but no difference in IMA/HVA or recurrence at final follow-up compared with isolated TMT arthrodesis. Taken together, these findings suggest that supplemental first-second ray stabilization may enhance initial alignment and maintain correction, although consistent long-term benefit has not been definitively demonstrated.
In this study, relative first MT length was greater in the IMS cohort at all time points. Although fixation technique variation may contribute, this finding could reflect improved first-ray stability and resistance to shortening during correction.18,19 Because shorter relative first-ray length is associated with metatarsalgia,20,21 preservation of first-ray length may be another way IMS augmentation confers clinical benefit. However, previous work has suggested that sagittal plane alignment and overall first-ray mechanics may play a greater clinical role than length alone. 22 Thus, although IMS fixation may assist in maintaining first-ray length, a factor linked to forefoot biomechanics, its clinical significance warrants further investigation.
Notably, IMS fixation did not demonstrate any statistically significant differences in postoperative complications. Complication rates, including infection, nerve symptoms, hardware-related complications, nonunion, and reoperation, were comparable between groups. Prior studies report nonunion in 3.3% to 12%,5,23-25 infection in 2.3% to 7%, 26 and hardware removal in up to 15%, 27 which aligns with the rates observed in this cohort. These findings suggest that IMS augmentation can be used safely as an adjunct to the Lapidus procedure.
In addition to radiographic parameters, this study evaluated clinical outcomes, providing a more comprehensive assessment of deformity correction. As the modified Lapidus procedure continues to evolve, defining indications for adjunctive fixation techniques remains an important area of study. Future studies incorporating patient-reported outcomes and longer-term follow-up will be important to better define which patients may benefit most from supplemental fixation in hallux valgus correction.
Limitations
This study has limitations that should be considered when interpreting these findings, including those inherent to its retrospective design. Because this was a retrospective study with a fixed available sample and no a priori power calculation, the study may be underpowered to detect small between-group differences, and the results should be interpreted within this context. Similarly, multiple comparisons were performed across time points and outcomes without formal multiplicity adjustment (for P value level “significance”); thus, results should be interpreted as exploratory. Radiographic measurements were performed by a single reviewer, although verified by a fellowship-trained foot and ankle orthopaedic surgeon. However, interobserver reliability was not assessed. Clinical follow-up duration varied, and longer-term assessment may better capture complications such as recurrence and symptomatic hardware removal. In addition, differences in surgeon technique and implant constructs, including compression strategy and plate configuration, were not controlled and may have influenced the observed radiographic and clinical outcomes. This study did not capture specific surgical indications for first TMT arthrodesis, including the presence or severity of clinical first-ray instability. As a result, some patients in this cohort may have had relatively modest radiographic deformity at baseline. Furthermore, the heterogeneity in preoperative IMA values may reflect real-world variation in surgeon practice patterns rather than a single, standardized indication for Lapidus arthrodesis at this institution. This cohort was limited to procedures identified by CPT codes specific to first TMT arthrodesis (28740 and 28297). As a result, the study does not capture the full volume of hallux valgus correction procedures performed at our institution during this time frame. Because Morton’s method may underestimate relative first metatarsal length in cases of transverse plane deformity, 28 the ability to detect subtle changes in metatarsal length may be limited, although all measurements were performed using a standardized technique applied uniformly to both cohorts.
Conclusion
Supplemental IMS fixation in first TMT arthrodesis for hallux valgus was associated with greater maintenance of radiographic correction without observed differences in complication rates. These findings support IMS augmentation as a potential adjunct in appropriately selected patients.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251413242 – Supplemental material for Radiographic and Clinical Outcomes of Intermetatarsal Screw Fixation in First Tarsometatarsal Arthrodesis for Hallux Valgus
Supplemental material, sj-pdf-1-fao-10.1177_24730114251413242 for Radiographic and Clinical Outcomes of Intermetatarsal Screw Fixation in First Tarsometatarsal Arthrodesis for Hallux Valgus by Ashley N. Kimbel, Robin M. Litten, Allison D. Desforges, Robert W. Rutz and Michael D. Johnson in Foot & Ankle Orthopaedics
Footnotes
Appendix
Distribution of intermetatarsal screw use by surgeon for hallux valgus correction.
| Surgeon | Total cases, n | IMS used, n (%) | No IMS, n (%) |
|---|---|---|---|
| A | 55 | 40 (72.7) | 15 (27.3) |
| B | 25 | 10 (40.0) | 15 (60.0) |
| C | 9 | 1 (11.1) | 8 (88.9) |
Abbreviation: IMS, intermetatarsal screw.
Ethical Considerations
Ethical approval for this study was sought and deemed exempt by the University of Alabama at Birmingham Institutional Review Board (IRB 300011914) because this retrospective review of existing medical records posed minimal risk and met criteria for exemption.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
