Abstract

Introduction
Tumors of the foot and ankle are uncommon, comprising about 4% of musculoskeletal tumors; most lesions in this region are benign and arise from soft tissues. 7 Among bones, the distal fibula ranks third. 7 Aneurysmal bone cyst (ABC) typically affects patients in the first 2 decades of life and arises in the metaphysis of long bones, as well as in the posterior elements of vertebral bodies, forming lytic, expansile lesions with poorly defined margins. 7
Distal fibular tumors are surgically challenging because they may compromise ankle stability through syndesmotic involvement and can affect the distal fibular physis in children. 6 Reported treatments include curettage/graft, resection/ankle arthrodesis, reconstruction with allograft/ipsilateral proximal fibula, free fibular grafts, and subperiosteal resection. 3
In 1995, Babhulkar et al 2 described a sliding cortical graft from the ipsilateral fibula to restore ankle stability after autologous fibular harvest; in 1999, Rizzo et al 9 reported a similar approach for reconstruction following tumor resection. These less-invasive methods avoid ankle or syndesmotic arthrodesis but do not ensure preservation of fibular length or rotational alignment. Segmental resection can disrupt the spatial orientation of the lateral malleolus, potentially causing pain and instability.
We implemented a modification: intralesional resection while preserving the medial cortex of the lateral malleolus along its entire length to maintain rotational alignment and fibular length. This aims to preserve malleolar orientation and reduce instability and chronic pain. We describe the technique and report functional outcomes in 2 cases.
Indications and Contraindications
Indications: Localized lateral malleolar neoplasms in which intralesional resection is feasible and the medial cortex can be preserved without compromising prognosis
Contraindications: Malignant neoplasms, lesions requiring en bloc resection or removal of the medial cortex, intra-articular extension, or extensive soft-tissue involvement
Technique
Classic Babhulkar et al 2 Technique (Figure 1): (1) subperiosteal exposure of the fibula, (2) preparation of a sliding graft in the anteroposterior plane, and (3) distal advancement and fitting to restore malleolar position and fibular length. Rizzo et al 9 adapted the method for oncologic resections using a metaphyseal graft around the defect. Neither approach specifically addresses potential loss of fibular length or rotational alignment, which can result in ankle malalignment.

Babhulkar et al2 technic schematic illustration. (A) Subperiosteal fibular exposition. (B) Graft preparation in the anteroposterior plane. (C) Distal sliding and graft engaging to restore normal length and positioning of the malleolus.
Modified Procedure
Step A: Intralesional resection without creating a segmental defect, with preservation of the medial cortex to maintain rotational alignment and fibular length; curettage and adjuvant electrocautery of the preserved cortex (Figure 2).
Step B: Preparation of a graft from the proximal ipsilateral approximately 40 mm longer than the defect, providing an overlap of 20 mm on each side of the noninvolved bone (Figure 3).
Step C: Distal sliding and fixation with plate and screws, which we prefer to screws alone to enhance lateral support and rotational control in this reconstruction (Figure 4).

Schematic figure of step A of the surgical modification.

Schematic figure of step B of surgical modification.

Schematic figure of step C of the surgical modification.
Case 1
A 17-year-old male adolescent presented with 12 months of lateral ankle pain and swelling after a soccer match. Radiographs showed an expansile lytic distal fibular lesion, and MRI demonstrated fluid-fluid levels consistent with ABC (Figure 5). Biopsy confirmed the diagnosis. The modified technique was performed (Figure 6). Postoperatively, the patient used an orthopaedic boot for 6 weeks, followed by physiotherapy. At 6 months, he had returned to normal activities with clear graft consolidation and no evidence of local recurrence (Figure 7). Functional scores were American Orthopaedic Foot & Ankle Society (AOFAS) ankle-hindfoot score 97/100 and Musculoskeletal Tumor Society Rating Scale (MSTS) score 23/30 (76.5%). At 2 years, the scores remained stable (AOFAS 98/100 and MSTS 23/30 [76.5%]) without recurrence or implant/graft failure.8,10

(A) Initial radiograph showing lytic and insufflative lesion of the right lateral malleolus. (B) Fluid-fluid level observed on ankle MRI with T1-weighted images in the sagittal and axial planes. MRI, magnetic resonance imaging.

Intraoperative images of case 1. (A) Dissection of the lesion. (B) Appearance of the distal fibula bed after resection, curettage, and local adjuvant treatment with cautery. (C) Surgical specimen and graft from the proximal fibula. (D) Final appearance after graft fixation with a locking plate.

Six-month postoperative radiograph demonstrating good ankle alignment, with no signs of local recurrence and remodeling of the donor area.
Case 2
A 14-year-old male adolescent reported 6 months of right ankle pain. Radiographs showed an expansile metaphyseal distal fibular lesion sparing the epiphysis (Figure 8). Biopsy confirmed ABC. The same modified technique and postoperative protocol were used. At 6 months, he had returned to usual and sports activities without limitation; radiographs confirmed graft consolidation and absence of recurrence (Figure 9). Functional scores at 2-year follow-up were AOFAS 100/100 and MSTS 27/30 (90.0%).8,10
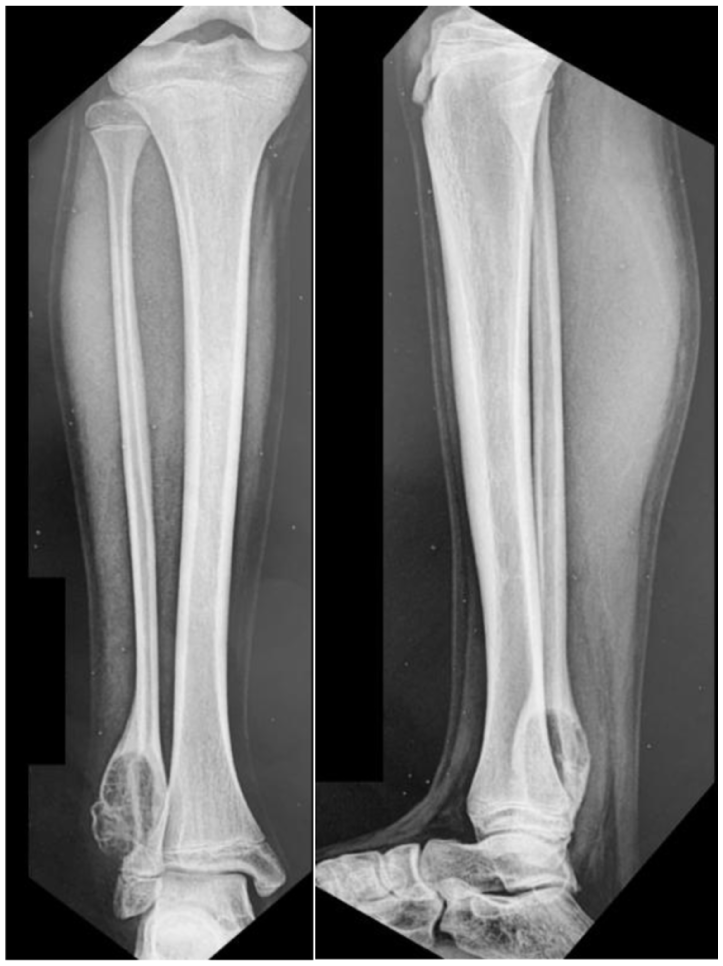
Initial radiograph showing a lytic, insufflating lesion in the distal metaphysis of the fibula without involvement of the epiphysis.

Six-month postoperative radiograph demonstrating good ankle alignment, with no signs of local recurrence and remodeling of the donor area.
Complications
No clinically relevant complications occurred in these 2 cases. Theoretical risks include premature physeal closure and angular deformity in skeletally immature patients. General surgical risks include neurovascular injury, surgical site infection, implant failure, nonunion or delayed union, joint instability, and tumor recurrence. Rotational malalignment and fibular shortening remain potential complications if anatomic alignment is not meticulously preserved.
Discussion
Surgery for lateral malleolar tumors must balance oncologic safety with preservation of ankle biomechanics and, in children, the growth plate. Unlike the classic ipsilateral sliding fibular grafts described by Babhulkar et al 2 and by Rizzo et al, 9 our modification intentionally preserves the medial cortex of the distal fibula so that rotational alignment and fibular length are maintained while the lateral shell is reconstructed with an ipsilateral advancing graft. Resection of the lateral malleolus can cause anterolateral tibiotalar instability. Lampasi et al 4 reported 9 pediatric distal fibular ABCs treated with curettage plus adjuvancy, resection with autograft, or resection with allograft; with mean 11-year follow-up, AOFAS scores were excellent/good, and growth, alignment, stability, and remodeling were acceptable across methods.
We favored a lateral plate over screws alone to add temporary lateral support and permit earlier partial weight-bearing. Although Misaghi et al 5 showed lag screws can match plate-and-screw stiffness for certain fractures, there are no specific studies evaluating this comparison in the context of fixation over allograft. We are not confident that screw fixation provides the same degree of rotational stability as plate fixation in this type of reconstruction.
The present modification explicitly maintains the medial cortex to preserve rotational alignment and fibular length. Advantages include avoiding contralateral donor morbidity and dependence on bone banks, using standard fixation hardware, and obviating ankle or syndesmotic arthrodesis. In both cases, graft integration, satisfactory ankle alignment, and timely return to activities were achieved without recurrence or instability at short-term follow-up.
We would consider this even in children <10 years, with syndesmotic fixation to reduce valgus risk. The preserved medial cortex acts as a structural column maintaining metaphyseal-epiphyseal alignment. Although not previously detailed, the closest analogue is Abuhassan et al, 1 who showed subperiosteal intercalary resection, preserving only a small distal segment and employing syndesmotic fixation, yet still showing rapid periosteal new bone formation in a young child without grafting or an intact medial cortex, highlighting pediatric regenerative capacity and the biomechanical benefit of preserving the medial cortex when feasible.
The fibular strut allograft is acknowledged as an excellent option in settings with well-established bone banks and donation programs, offering lower donor-site morbidity and useful reinforcement of the distal fibula. However, in many regions, cultural nonacceptance, limited availability, or high cost restrict allograft use. In these circumstances, an autograft remains a feasible and effective reconstructive alternative.
Conclusion
This modified technique preserves the medial cortex, maintains fibular length and rotational alignment, and provides stable reconstruction. It may be particularly useful when an allograft is unavailable or culturally unacceptable and when intralesional resection allows the medial cortex to be preserved. Given the rarity of these tumors, further studies are warranted to validate indications, refine technique, and confirm long-term outcomes.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251403480 – Supplemental material for Modified Sliding Fibular Graft for Aneurysmal Bone Cyst of the Lateral Malleolus: Technique and Two-Case Series
Supplemental material, sj-pdf-1-fao-10.1177_24730114251403480 for Modified Sliding Fibular Graft for Aneurysmal Bone Cyst of the Lateral Malleolus: Technique and Two-Case Series by Filipe Marques de Oliveira, Mariana Vendramin Mateussi, Jairo Greco Garcia, Marcelo de Toledo Petrilli, Dan Carai Maia Viola and Reynaldo Jesus-Garcia Filho in Foot & Ankle Orthopaedics
Footnotes
Ethical Considerations
This study was approved by the Research Ethics Committee of Universidade Federal de São Paulo (UNIFESP) under protocol 7.481.760.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
