Abstract
Background:
Rotational malalignment of the first metatarsal is increasingly recognized as a key feature of hallux valgus deformity, but the reliability of radiographic rotation markers remains uncertain. This study assessed the inter- and intraobserver reliability of 4 commonly used radiographic parameters: metatarsal pronation angle (MPA), tibial sesamoid position (TSP), lateral head shape (LHS), and round head sign (RH).
Methods:
In this prospective reliability study, 3 senior clinicians independently evaluated weightbearing anteroposterior and axial sesamoid radiographs of 75 hallux valgus cases on 2 occasions. Metatarsal pronation angle (MPA) was measured as a continuous variable and analyzed using intraclass correlation coefficients (ICCs). Tibial sesamoid position (TSP), lateral head shape (LHS), and round head sign (RH) were graded using ordinal scales and assessed with weighted kappa statistics (κ). Subgroup analyses evaluated whether reliability varied by deformity severity (hallux valgus angle) or increased distal metatarsal articular angle (DMAA > 10 degrees).
Results:
MPA showed excellent agreement (ICC = 0.81-0.94). TSP also demonstrated high reliability (κ = 0.88-0.98), although its value as a rotation marker is limited. LHS showed moderate to substantial agreement (κ = 0.59-0.85), whereas RH had fair to moderate reliability (κ = 0.35-0.66). RH was least reliable in mild deformities, whereas other parameters remained stable across subgroups, with slightly lower values in cases with elevated DMAA.
Conclusions:
Conventional radiographs offer reliable assessment of MPA and TSP. LHS provides acceptable reproducibility, whereas RH is less consistent. These findings support the use of selected radiographic markers and suggest that further validation against 3-dimensional imaging and standardized grading frameworks may improve consistency and clinical applicability.
Level of Evidence:
Level IV, case series.

Keywords
Introduction
Hallux valgus is a complex 3-dimensional deformity characterized by lateral deviation and external rotation (pronation) of the first metatarsal. Although metatarsal pronation has been recognized for decades, interest in this aspect has grown significantly in recent years.3,11,13
A turning point came when Okuda et al 8 demonstrated that the lateral aspect of the first metatarsal head appeared less rounded on anteroposterior (AP) radiographs following hallux valgus surgery, a finding associated with reduced recurrence. Later, the same authors concluded that metatarsal pronation is an integral component of the deformity, as supination restored the normal contour of the metatarsal head.9,13
Subsequent studies using weightbearing computed tomography (WBCT) further explored the role of metatarsal rotation. Kim et al 5 classified hallux valgus deformity into 4 distinct patterns based on metatarsal-sesamoid alignment, demonstrating that 87% of cases exhibited metatarsal pronation.
Although WBCT offers detailed 3-dimensional imaging, its use remains limited in many clinical settings and is not routinely obtained for hallux valgus assessment. To enable clinical use and future WBCT validation, it is essential to determine whether radiographic rotation markers can be applied with consistent observer agreement.
The primary aim of this study was to assess inter- and intraobserver reliability of radiographic rotational markers—including lateral head shape (LHS), round head sign (RH), tibial sesamoid position (TSP), and metatarsal pronation angle (MPA)—using standard weightbearing AP and axial sesamoid views.
Although both LHS and RH are based on visual assessment of the lateral contour of the first metatarsal head on AP radiographs, they differ in structure and focus. LHS is a multilevel, landmark-based classification incorporating features such as the lateral tubercle, whereas RH reflects the overall impression of roundness on a simplified 3-point scale.
As a secondary aim, we investigated whether observer agreement varied with the severity of hallux valgus deformity, conducting subgroup analyses based on hallux valgus angle (HVA) categorized as mild (<20 degrees), moderate (20-40 degrees), or severe (>40 degrees); and second, to explore whether the presence of an increased distal metatarsal articular angle (DMAA > 10 degrees) affected the reliability of these measurements.
Establishing the reliability of radiographic rotation markers is important because these parameters are increasingly considered in surgical planning.
Materials and Methods
Study Design
This was a prospective reliability study embedded within a larger, ongoing cohort investigating hallux valgus. The study adhered to the Declaration of Helsinki. Ethical approval was obtained from the Regional Committee for Medical and Health Research Ethics (REK, approval no. 217200) and the hospital’s data protection officer. Written informed consent was obtained from all participants.
Observers
Three senior clinicians served as observers: 2 foot and ankle surgeons from different institutions and 1 musculoskeletal radiologist from a third center—none of whom had prior routine use of the specific rotational measurements. All observers received standardized written and visual instructions outlining the measurement procedures and were masked to patient identifiers and to each other’s assessments. Measurement guides are shown in Figures 1 to 4.
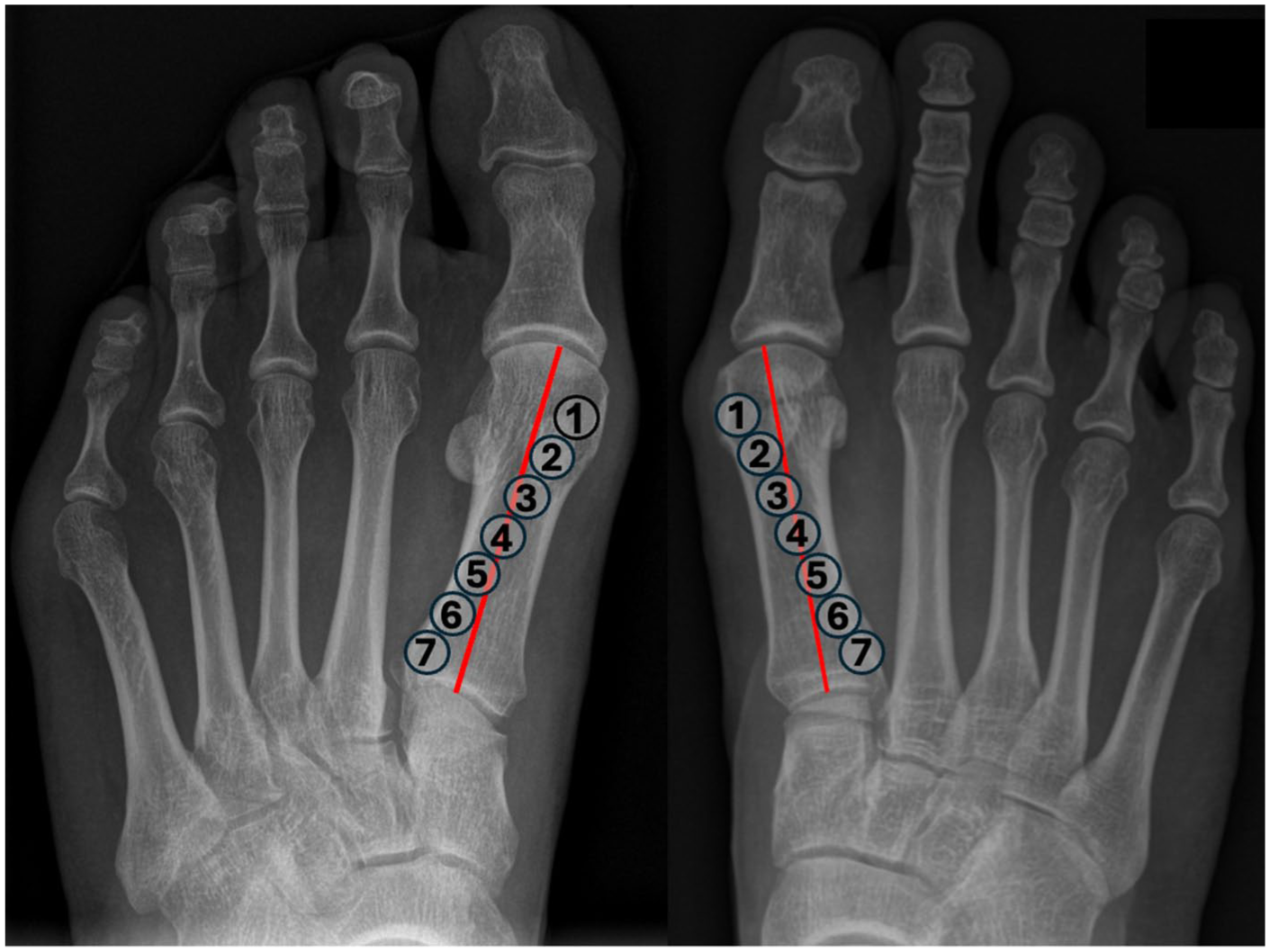
Radiographic grading of tibial sesamoid position (TSP) based on the modified Hardy and Clapham classification. A red reference line was drawn along the axis of the first metatarsal shaft. TSP was graded 1–7 based on the medial-to-lateral position of the tibial sesamoid in relation to this line, with grade 4 indicating a central location and grades 1 and 7 reflecting maximal displacement.

Axial sesamoid view demonstrating measurement of the metatarsal pronation angle (MPA). The solid line runs between the most medial and lateral points of the sesamoid grooves of the first metatarsal head. The angle is measured between this line and the horizontal plane (floor), representing the degree of pronation relative to weightbearing orientation.

Illustration of the Lateral Head Shape (LHS) classification used in this study. The grading system includes four levels (1, 2a, 2b, 3) based on the lateral contour of the first metatarsal head, reflecting progressive rounding. Illustrations were adapted by the authors based on previously published morphological frameworks, and were designed to support consistent visual grading during radiographic assessment.

Illustration of the Round Head (RH) classification used in this study. The three-point scale (1–3) reflects progressive lateral roundness of the first metatarsal head. Illustrations were adapted from previously published visual frameworks to support consistent radiographic grading.
Participants
A total of 75 patients were included, selected consecutively from a prospectively collected cohort undergoing radiographic evaluation for hallux valgus between 2021 and 2024. Radiographic hallux valgus was defined as a hallux valgus angle (HVA) >15 degrees and intermetatarsal angle (IMA) >9 degrees, in accordance with established diagnostic criteria. 1 Only patients with a complete set of weightbearing anteroposterior (AP) and axial sesamoid view radiographs of acceptable quality were considered.
Inclusion criteria
Adults with clinically and radiographically confirmed hallux valgus
Availability of weightbearing AP and axial sesamoid view radiographs
Exclusion criteria
Kellgren & Lawrence grade >2 (moderate to severe osteoarthritis of the first metatarsophalangeal joint)
Prior surgery or trauma involving the first ray
Inadequate radiographic quality, including insufficient weightbearing or poor visualization of the sesamoid sulci. Given the known technical challenges associated with obtaining high-quality axial images—particularly in the presence of forefoot malalignment—images were accepted if both medial and lateral sulcus contours were reasonably discernible.
Radiographic Technique and Measurements
Four rotational parameters were evaluated on weightbearing radiographs: LHS, RH, TSP, and MPA (Figures 1-4). LHS and RH were assessed on AP radiographs using ordinal classification systems based on the lateral contour of the first metatarsal head. As described in the Introduction, LHS is a structured, multilevel system based on discrete anatomic features, whereas RH reflects a simplified visual impression of roundness.
The RH sign was evaluated on a 3-point scale (1-3), where higher values indicated greater lateral head roundness. This visual classification was based on the grading system described by Wu and Lam, which builds on the work of Yamaguchi et al.16,17
LHS was scored using a 4-level scale (1, 2a, 2b, 3), adapted by the authors based on established morphologic patterns and visual references from prior literature. The classification was conceptually based on the association between metatarsal pronation and lateral head roundness described by Okuda et al, 8 and visually informed by illustrations from the PROMO Surgical Technique Guide by Wagner and Wagner. 15 All illustrations used in this study were redrawn by the authors based on these published visual frameworks.
TSP was graded 1 to 7 based on the Hardy and Clapham classification. 4
MPA was measured on axial sesamoid view radiographs as the angle between a line parallel to the floor and a line connecting the lateral border of the lateral sesamoid sulcus to the medial border of the medial sesamoid sulcus.
Weightbearing axial forefoot radiographs were obtained with the hallux dorsiflexed to approximately 30 degrees, in line with the positioning described by Siebert et al, 12 who proposed that this replicates the position of maximal sesamoid engagement during the toe-off phase of gait. Beam direction was aligned toward the metatarsal heads, as recommended by Wagner and Wagner, to enhance visualization of the sesamoid sulci. 13 Measurements were performed manually using PACS software tools.
All HVA and DMAA measurements were performed manually by the first author. Each angle was measured multiple times, and the most consistent value was used in the analyses. DMAA was dichotomized at 10 degrees, consistent with common clinical practice and prior publications. 6
Measurement Procedure
Each observer independently evaluated all radiographs twice, with a minimum interval of 3 weeks between sessions to minimize recall bias. Observers were masked to their previous measurements and to the results of the other raters.
Consideration of DMAA
Within our research group, it was discussed that an increased distal metatarsal articular angle (DMAA > 10 degrees) could reflect either a true morphologic variant or a surrogate marker of rotational malalignment. As a result, all participants were included regardless of DMAA status, and a subgroup analysis was performed to assess whether elevated DMAA affected measurement reliability.
Severity Stratification
Hallux valgus severity was classified based on the hallux valgus angle (HVA) as follows:
Mild: HVA <20 degrees
Moderate: HVA 20-40 degrees
Severe: HVA >40 degrees
Statistical Analysis
Reliability of continuous variables (MPA) was assessed using the intraclass correlation coefficient (ICC), calculated with a 2-way random effects model for absolute agreement of single measurements [ICC(2, 1)]. Ordinal variables (LHS, TSP, LHS, RH) were evaluated using Cohen weighted kappa. Quadratic weights were applied for LHS and TSP to reflect their graded severity scales, whereas linear weights were used for LHS and RH because of their simpler ordinal structures. Interobserver and intraobserver reliability were analyzed separately for each measurement round. Interpretation thresholds for ICC and kappa followed standard guidelines: <0.20 (slight), 0.21 to 0.40 (fair), 0.41 to 0.60 (moderate), 0.61 to 0.80 (substantial), and 0.81 to 1.00 (almost perfect).
To further explore category-level uncertainty, cumulative link mixed models (CLMMs) were also fitted for TSP and LHS. These analyses confirmed high agreement for TSP and revealed greater observer variability for LHS, supporting the use of weighted kappa as the primary metric; detailed results are presented in Supplementary Table 1.
Subgroup analyses were performed based on hallux valgus severity (mild, moderate, severe) and DMAA category (≤10 degrees vs >10 degrees). Simplified random-effects structures were used when model singularity occurred. An a priori power calculation indicated that 72 participants were required to detect an ICC of 0.75 with 80% power at α = 0.05, assuming 3 raters and 2 repeated measurements. All analyses were conducted in R (version 4.5.0) using the irr, ordinal, lme4, flextable, and officer packages.
Results
Sample Characteristics
A total of 75 feet were included (63 women, 12 men), with a mean age of 50.1 years (SD 11.3; range 19-73). Radiographs represented 34 right feet (45.3%) and 41 left feet (54.7%). The mean hallux valgus angle (HVA) was 23.7 degrees (SD 7.8), intermetatarsal angle (IMA) 11.3 degrees (SD 2.8), and distal metatarsal articular angle (DMAA) 9.9 degrees (SD 4.3). Based on HVA, 29 feet (38.7%) were classified as mild (<20 degrees), 42 (56.0%) as moderate (20-40 degrees), and 4 (5.3%) as severe (>40 degrees). An increased DMAA (>10 degrees) was present in 25 feet (33%).
Interobserver Reliability
Interobserver reliability for the metatarsal pronation angle (MPA) was good to excellent, with intraclass correlation coefficients (ICCs) of 0.823 and 0.875 in rounds 1 and 2, respectively. Tibial sesamoid position (TSP) demonstrated almost perfect agreement (κ = 0.90 and 0.94). Lateral head shape (LHS) showed substantial agreement in round 1 (κ = 0.68) and moderate agreement in round 2 (κ = 0.59). The round head sign (RH) demonstrated moderate agreement in round 1 (κ = 0.43) and fair agreement in round 2 (κ = 0.35). Full results, including pairwise kappas and mean agreement values, are shown in Table 1.
Interobserver Reliability per Parameter and Round.

Abbreviations: ICC, intraclass correlation coefficient; LHS, lateral head shape; MPA, metatarsal pronation angle; RH, round head sign; TSP, tibial sesamoid position.
Intraobserver Reliability
MPA showed excellent intraobserver reliability across all 3 observers, with ICCs ranging from 0.813 to 0.942. TSP demonstrated almost perfect agreement (κ = 0.881-0.976). LHS showed substantial agreement (κ = 0.678-0.782), whereas RH yielded moderate intraobserver reliability (κ = 0.487-0.623). Detailed results are presented in Table 2.
Intraobserver Reliability by Parameter and Observer.
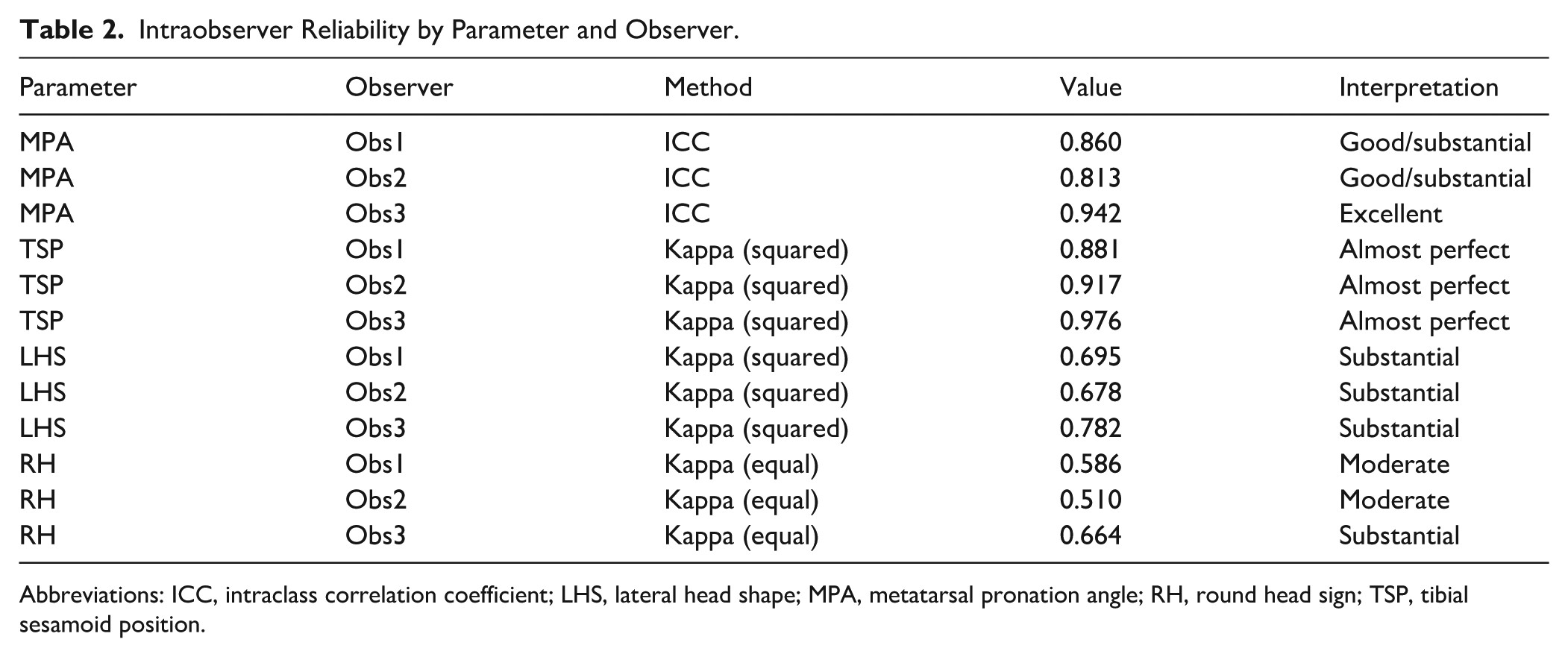
Abbreviations: ICC, intraclass correlation coefficient; LHS, lateral head shape; MPA, metatarsal pronation angle; RH, round head sign; TSP, tibial sesamoid position.
Subgroup Analyses: HVA Severity
When stratified by deformity severity, MPA maintained good to excellent interobserver reliability across all HVA categories (ICC: 0.86 [mild], 0.81 [moderate], 0.82 [severe]). TSP showed almost perfect agreement in mild and moderate groups (κ = 0.86 and 0.87), but estimates for the severe group could not be calculated because of the small sample size. LHS reliability ranged from moderate to substantial (κ = 0.55-0.71), with the lowest agreement observed in the mild group. RH showed the poorest performance, with κ values ranging from 0.14 (mild) to 0.38 (moderate), suggesting reduced consistency in less pronounced deformities. Summary values represent mean agreement across observer pairs. See Table 3 for full results.
Interobserver Reliability per Marker and HVA Group (Round 1).

Abbreviations: HVA, hallux valgus angle; ICC, intraclass correlation coefficient; LHS, lateral head shape; MPA, metatarsal pronation angle; RH, round head sign; TSP, tibial sesamoid position.
Subgroup Analyses: DMAA
Observer agreement was slightly higher in cases with a normal or low DMAA (≤10 degrees) compared to those with elevated DMAA (>10 degrees). MPA demonstrated greater consistency in the low-DMAA group (ICC = 0.853 vs 0.804), as did TSP (κ = 0.941 vs 0.910), LHS (κ = 0.635 vs 0.583), and RH (κ = 0.365 vs 0.280). These results indicate slightly lower interobserver agreement in the presence of elevated DMAA, particularly for visually graded markers. However, this observational finding should be interpreted with caution, as multiple confounding factors may influence measurement consistency. Full data are presented in Table 4.
Interobserver Reliability per Marker and DMAA Group (Round 1).
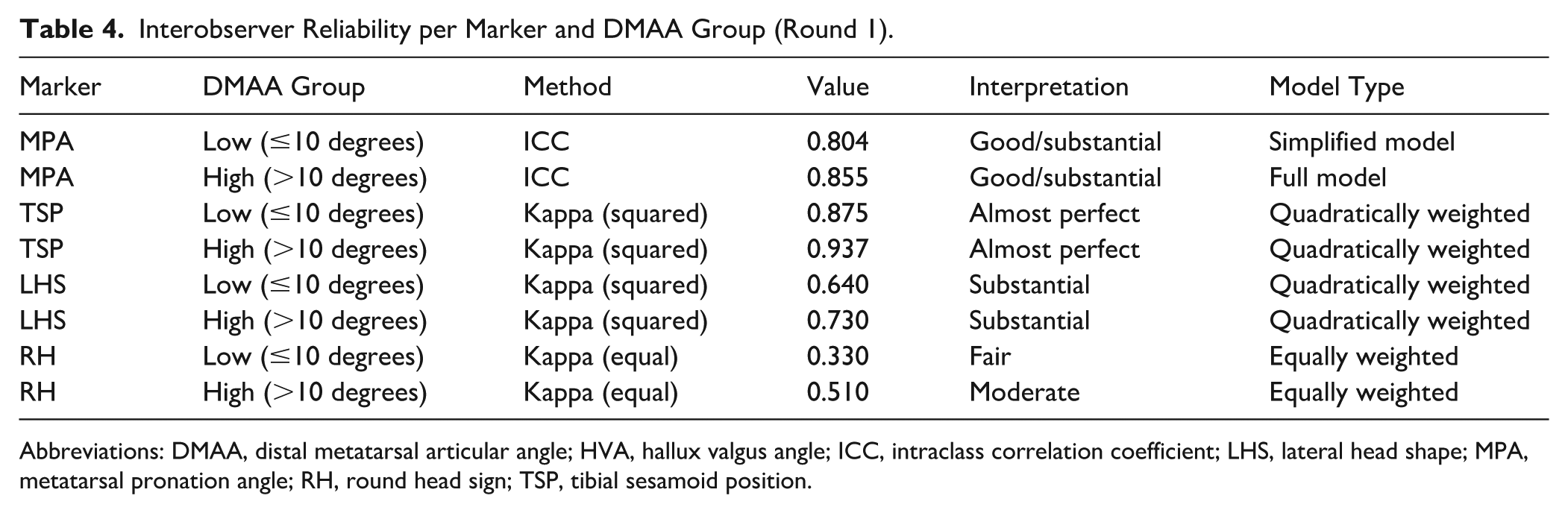
Abbreviations: DMAA, distal metatarsal articular angle; HVA, hallux valgus angle; ICC, intraclass correlation coefficient; LHS, lateral head shape; MPA, metatarsal pronation angle; RH, round head sign; TSP, tibial sesamoid position.
Discussion
This prospective study assessed the reliability of 4 radiographic markers for evaluating first metatarsal rotation in hallux valgus. MPA and TSP showed excellent reproducibility, supporting their clinical applicability. In contrast, morphology-based signs—LHS and RH—were less consistent, particularly in severe deformities or when DMAA was elevated.
Although we acknowledge that correlation with 3-dimensional imaging would enhance validity, our primary aim was to assess reproducibility across observers. Establishing reliability is a necessary step before broader validation, particularly for emerging radiographic markers such as MPA, LHS, and RH. Our results for MPA align closely with those of Siebert et al, 12 who demonstrated excellent agreement between MPA and WBCT-derived rotation measures (ICC = 0.986) in a cohort with primarily mild deformities. By including a broader spectrum of hallux valgus severity and assessing the influence of elevated DMAA—an aspect not previously explored—we extend these findings and support the clinical applicability of MPA across varying anatomic presentations.
Subgroup findings confirmed that MPA and TSP remained highly reliable across deformity severity and DMAA categories, whereas RH showed lower agreement in mild deformities and a slight decline with increasing DMAA.
We performed subgroup analyses to explore whether measurement reproducibility varied with increasing DMAA, particularly for visually graded markers such as LHS and RH. Although the potential relationship between DMAA and metatarsal rotation remains debated in the literature, our findings suggest that elevated DMAA had limited impact on interobserver agreement.
The 4 markers reflect different anatomic levels and are assessed across 2 imaging planes (AP and axial views). MPA, assessed on axial sesamoid views, directly captures coronal rotation at the level of the sesamoid grooves. 12 Although this view is not routinely included in standard hallux valgus protocols, our findings—and those of Siebert et al—suggest it offers the most consistent radiographic assessment of first metatarsal rotation. Wider adoption of axial sesamoid imaging in routine preoperative evaluation may therefore improve rotational assessment, particularly where access to WBCT is limited. TSP remains a reliable ordinal tool but serves as an indirect marker of rotation. As Kim et al 5 demonstrated using WBCT, apparent sesamoid alignment on AP views may be misleading—so-called pseudo-sesamoid subluxation—seen in 25% of pronated metatarsals. In contrast, LHS and RH reflect surface morphology on AP images and may be affected by projection, rotation, and osteophytes. 17
The use of head shape as a pronation surrogate has both biomechanical and historical grounding. Eustace et al 3 first described lateral contour changes with increasing pronation, later adopted by Okuda et al 8 and Wagner and Wagner. 13 We adapted these into a standardized reference guide inspired by the PROMO technique, providing the first empirical test of its reliability. 15 Although LHS proved more reproducible than RH, the moderate agreement for both—particularly in mild deformities—highlights the difficulty of grading subtle morphologic features. In our study, LHS directed attention to specific landmarks such as the lateral tubercle, whereas RH relied more on global shape perception, which may explain its lower agreement despite a simpler grading scale.
Wu and Lam evaluated RH and inferior tuberosity position—equivalent to our RH and LHS—on weightbearing AP radiographs, reporting moderate agreement. 16 The inclusion of both pre- and postoperative images may partly explain their lower reliability, as surgical changes can obscure morphology. Del Vecchio et al 2 later reported poor agreement for RH (κ = 0.225; ICC = 0.389), concluding the method was too subjective for clinical use. Our study builds on this by applying a standardized visual reference and demonstrating improved reproducibility using masked, repeated assessments and axial imaging.
Wagner et al developed a radiographic method for assessing first metatarsal rotation—termed medial column internal rotation—based on the lateral head contour seen on weightbearing AP views. Their method, conceptually aligned with our LHS classification, showed substantial reliability (κ = 0.79; ICC = 0.85) and 85% diagnostic accuracy compared with WBCT. 14 Unlike their study, which likely included surgeons familiar with rotational assessment, our senior observers had no prior experience with these specific markers, yet achieved consistent results.
Moreover, we stratified reliability across deformity severity and DMAA to explore whether these anatomic factors influenced measurement consistency.
Reproducible assessment of metatarsal rotation is clinically relevant, particularly when considering derotational osteotomy. Among the evaluated markers, MPA offers a consistent and practical tool that may support surgical planning and help stratify recurrence risk. While not a replacement for WBCT, conventional radiographs remain the most accessible modality in routine care. In contrast, visual markers such as LHS and RH may require further refinement before broader clinical application.
Although Siebert et al 12 demonstrated excellent agreement between MPA and WBCT-derived rotation measures, our study extends these findings by confirming high reliability of MPA across a broader range of deformity severity. This supports its use as a robust and reproducible marker even in more complex cases, where conventional radiographs remain the most practical tool. In most clinical settings, weightbearing axial views are not routinely included in the radiographic workup for hallux valgus, and surgical planning often depends on subjective AP-based assessments such as the round head sign. Our findings suggest that structured parameters like MPA may offer a more consistent and anatomically grounded alternative. Given its reproducibility and potential clinical value, wider adoption of axial sesamoid imaging in routine preoperative evaluation should be considered—particularly where access to WBCT is limited.
Overall, our findings emphasize the importance of selecting rotation markers that are both anatomically meaningful and reproducible in clinical practice. Although Wagner et al demonstrated promising reliability for a morphology-based marker, other studies such as that of Mansur et al 7 have raised concerns about the anatomic validity of head shape assessments, showing only weak correlation with axial rotation on CT. This highlights the need for continued refinement of radiographic rotation measures and supports the use of structured, image-plane–specific parameters such as MPA in routine assessment of hallux valgus.
Limitations
Although this study provides robust data on inter- and intraobserver reliability, several limitations should be considered. First, all assessments were based on standardized weightbearing radiographs; no 3-dimensional imaging such as WBCT was available for comparison. Although MPA has demonstrated strong concordance with WBCT, the anatomic validity of TSP, LHS, and RH remains uncertain, as existing studies offer conflicting evidence.5,12,14,17
Second, although patients with moderate to severe osteoarthritis were excluded, we acknowledge that milder degenerative changes—such as osteophyte formation—may still influence visual interpretation of head shape or sesamoid position.
Third, our analyses were limited to preoperative imaging. Whether similar reliability can be achieved postoperatively remains unclear, particularly as implants, altered anatomy, or soft tissue changes may obscure key landmarks. As Prusmetikul et al 10 showed, reproducibility of markers such as sesamoid position and head shape may decline after surgical correction.
Fourth, relatively few severe cases were included, limiting generalizability in that subgroup. This likely reflects the technical challenges of obtaining high-quality axial views in advanced deformities, which may reduce inclusion eligibility in this population.
Fifth, although none of the observers had prior experience with these specific measurements, they were all senior clinicians. Although this reflects conditions typical for early adoption in specialized practice, future studies may benefit from including raters with varying levels of training to further assess generalizability.
Finally, although a standardized visual guide likely improved consistency, it may have constrained interpretation in borderline cases where grading remains subjective. Although WBCT provides superior 3-dimensional visualization, the reproducibility of rotation measurements on 3D imaging remains uncertain, and no standardized protocols have been established. Although access to WBCT has increased, it is still not routinely used in the assessment of typical hallux valgus—one of the most common forefoot deformities treated in orthopaedic practice.
Given the added infrastructure, personnel demands, and uncertain benefit in routine cases, conventional radiography remains a practical and reliable tool in everyday clinical evaluation.
Future Directions
Future research should aim to validate radiographic rotation markers—particularly LHS and RH—against WBCT, including assessments across the full deformity spectrum and in postoperative cases. Artificial intelligence–assisted image analysis may further enhance reproducibility, especially for morphology-based systems prone to observer variability. Standardizing terminology—for example, aligning “lateral head shape” with descriptors like “inferior tuberosity position,” “lateral contour,” or “medial column rotation”—could also improve clarity and consistency. Although LHS is not yet widely established, it integrates prior morphologic concepts and may serve as a practical, anatomically grounded term for future clinical and research use.
Furthermore, although Wagner et al 14 reported high reliability for a morphology-based rotation marker conceptually similar to our LHS classification, our findings suggest more modest agreement when the system is applied independently and without prior training. Several other head shape and roundness classifications have also been introduced without formal validation, which may contribute to inconsistent interpretation and highlight the need for objective, reproducible reference standards in future research.
Conclusion
This study showed that MPA and TSP can be measured with excellent reliability on weightbearing radiographs. MPA remained the most consistent marker across deformity severities and DMAA levels. Given its reproducibility, MPA may help guide surgical planning in hallux valgus. However, as axial sesamoid views are not routinely obtained, broader implementation will require consistent imaging protocols.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251371723 – Supplemental material for Metatarsal Pronation on Radiographs: A Prospective Reliability Study of Visual Rotation Markers in Hallux Valgus
Supplemental material, sj-pdf-1-fao-10.1177_24730114251371723 for Metatarsal Pronation on Radiographs: A Prospective Reliability Study of Visual Rotation Markers in Hallux Valgus by Mikaela Engarås Hamre, Lise Benedikte Wendt Ræder, Martin Okelsrud Riiser, Peter Franz Schubert and Marius Molund in Foot & Ankle Orthopaedics
Footnotes
Appendix
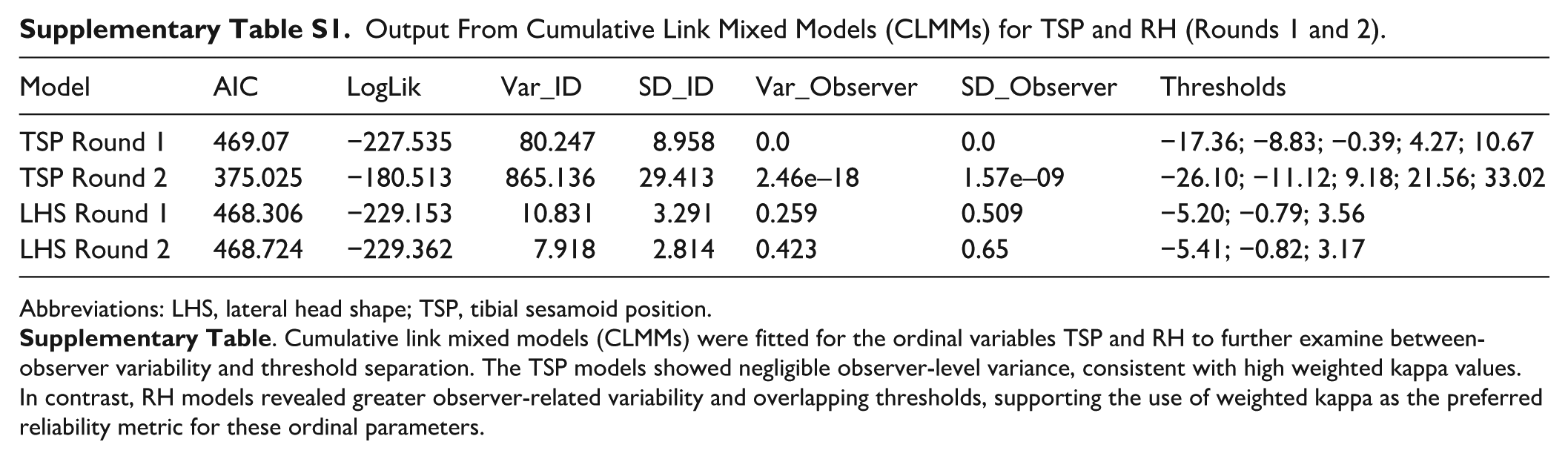
Output From Cumulative Link Mixed Models (CLMMs) for TSP and RH (Rounds 1 and 2).
| Model | AIC | LogLik | Var_ID | SD_ID | Var_Observer | SD_Observer | Thresholds |
|---|---|---|---|---|---|---|---|
| TSP Round 1 | 469.07 | −227.535 | 80.247 | 8.958 | 0.0 | 0.0 | −17.36; −8.83; −0.39; 4.27; 10.67 |
| TSP Round 2 | 375.025 | −180.513 | 865.136 | 29.413 | 2.46e–18 | 1.57e–09 | −26.10; −11.12; 9.18; 21.56; 33.02 |
| LHS Round 1 | 468.306 | −229.153 | 10.831 | 3.291 | 0.259 | 0.509 | −5.20; −0.79; 3.56 |
| LHS Round 2 | 468.724 | −229.362 | 7.918 | 2.814 | 0.423 | 0.65 | −5.41; −0.82; 3.17 |
Abbreviations: LHS, lateral head shape; TSP, tibial sesamoid position.
Ethical Approval
Ethical approval for this study was obtained from the Regional Committee for Medical and Health Research Ethics (REK, approval no. 217200) and the Østfold Hospital Trust Data Protection Officer. Written informed consent was obtained from all participants. The study adhered to the Declaration of Helsinki.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
