Abstract
This is a visual representation of the abstract.
Introduction
Tarsometatarsal (TMT) joint injuries, or injuries to the Lisfranc joint complex, account for approximately 0.5% of all fractures, with a reported incidence of 9.2 per 100,000 person-years.7,18,45 A series published in 1989 reported that up to 40% of TMT injuries were missed on initial radiographs, 39 which can subsequently result in substantial morbidity for patients. The genesis of these injuries can involve a range of mechanisms, from high-energy trauma such as a motor vehicle accident (MVA) or crush injury to low-energy indirect trauma such as twisting on a plantarflexed foot seen in sporting settings. 57
Background
The TMT joint complex supports the transverse arch of the foot and consists of the articulations between the 3 cuneiforms (C1-C3), 5 metatarsals (MT1-MT5), and the cuboid. The midfoot complex is supported by weaker dorsal, stronger interosseous, and strongest plantar ligaments.13,26 The term “Lisfranc ligament” refers to a key ligamentous complex traversing from the plantar aspect of the MT2 base to C1, with dorsal, interosseous, and plantar components. 26 The stability of the articular complex is provided by a combination of osseous and ligamentous anatomy, with the “keystone effect” of the recessed second TMT joint and Lisfranc ligament of particular importance. 51
Injury to the midfoot can involve a combination of bony or ligamentous injuries with varying involvement of the TMT complex. 18 The natural history of this spectrum of conditions is well understood. If unstable injuries are untreated, patients will likely sustain progressive midfoot collapse and arthrosis, which may require shoe modification, orthoses, or, ultimately, surgery. 36 High-energy fracture-dislocations such as those in polytrauma patients have guarded outcomes despite optimal surgical management.29,50 Lower-energy injuries have a better prognosis, but are more often missed or underdiagnosed as the radiographic and clinical signs are more subtle 33 and may require weightbearing or 3-dimensional imaging modalities to establish the diagnosis. 58
One of the difficulties in deciphering the literature on this topic is understanding where patients in a particular study fall on the spectrum of TMT injuries. The currently accepted treatment method across this diverse range of injuries is either open reduction and internal fixation (ORIF) or primary arthrodesis.34,38 If internal fixation is used, consensus has been reached in the literature regarding the need for near-anatomic or anatomic reduction in treating these injuries.
Several series have demonstrated that the quality of reduction is a key factor in predicting a positive patient outcome.29,34,35 Early recommendations to use wire fixation alone did not produce satisfactory results. 32 Although most authors agree there is a need to maintain accurate reduction with stable fixation, the optimal fixation construct has yet to be defined.
Currently used options for fixation of TMT joint injuries include rigid devices such as transarticular screws (TAS), articular bridging plates (ABP), or a combination of both plates and screws. 35 Recently, flexible devices such as suture buttons or fiber tape have also been investigated.14,41 In theory, flexible devices are appealing as they minimize damage to articular cartilage, avoid the potential for broken screws, and obviate the need for hardware removal. These devices aim to re-create the native biomechanics of the ligamentous complex. In vivo animal models have demonstrated that complete immobilization of a ligament may be detrimental to healing and compromise its mechanical properties. 56 Flexible fixation constructs are well-established for syndesmotic injuries and have become more commonly used, with reports of superior results when compared to traditional screw fixation.10,25,37,46 In Lisfranc injuries, this is not established.
When interpreting the literature on Lisfranc injuries, a substantial challenge is separating high-energy fracture/dislocations and lower-energy (mainly ligamentous) injuries. Most clinical series on TMT joint injuries study severe fracture/dislocations or a spectrum of injuries.2,17,29,34 The literature on lower-energy injuries is scant in comparison. 60 In addition, there are numerous classification systems described for tarsometatarsal injuries, but none are universally accepted.18,39 Finally, there is heterogeneity in the outcome measures used to evaluate Lisfranc injuries, and many utilized the American Orthopaedic Foot & Ankle Society (AOFAS) midfoot score, which as a clinician-based outcome measure has insufficient reliability and validity compared to validated PROMS. 30
In this review, we performed a systematic literature search focusing on the different fixation constructs used in ORIF and examined the contemporary evidence to help guide treatment pathways for this heterogeneous group of injuries.
Literature Search
A literature search of electronic databases was carried out on April 16, 2024. We searched PubMed, Ovid EMBASE, and Ovid MEDLINE. We narrowed the scope of the search to the last 10 years to provide the most relevant articles. We searched using the following key terms: Lisfranc, midfoot, tarsometatarsal, plate, screw, fixation, and ORIF. Boolean operators were used where appropriate. We included studies on adult patients, in the English language, that included data on TMT fixation with any construct. We included review, systematic review, and meta-analysis articles. We excluded articles on pediatric patients, case reports, or those on Lisfranc primary arthrodesis. All articles were screened using the article title and abstract for suitability.
Search Results
Our search yielded a total of 36 articles. These are listed in Table 1. Our literature search yielded 15 retrospective cohort studies, 1 prospective study, and no randomized controlled trials. There were also 10 review articles and 6 meta-analyses. The remaining articles were biomechanical or surgical technique papers. This demonstrates that the number of high-quality trials in this space is lacking.
Literature search results. A search was carried out for the past 10 years using key terms on PubMed, MEDLINE and EMBASE.

Methods of Fixation
Rigid Fixation
Transarticular screws (TAS)
Transarticular fixation with Kirshner wires (K-wires) was historically used to stabilize injury to the TMT joints. 6 However, early reports of K-wire fixation were met with unacceptably high failure rates.18,39 Lee et al 36 subsequently examined the biomechanical stability of 3 rigid stabilization constructs. In a cadaveric model, these authors sectioned the ligaments of the first through fifth TMT joints. They then applied fixation with one of 3 constructs: (1) K-wires across all 3 columns, (2) transarticular screws across the medial and intermediate columns with K-wires across the lateral column, and (3) transarticular screws across all TMT joints. They then tested load to failure and found that K-wire fixation had a significantly lower load to failure compared with transarticular screws. They also reported that the group with fixation only across the first through third TMT joints did not fail earlier than the group with fixation across all TMTs. The authors concluded that fixation with only K-wires was inadequate and that it is possible that only the 3 medial TMT joints require rigid stabilization. These biomechanical data have formed the basis for many modern fixation techniques. 36
Alberta et al 4 reported their cadaveric results comparing TAS to ABP with nonlocking semitubular plates across the first and second TMT joints. Load to failure was similar for each group. However, there was less articular cartilage disruption in the ABP group compared with the TAS group, and the authors therefore recommended bridge plating as a viable alternative to transarticular screws. 4 In another cadaveric TAS model, the original articular injury caused by screw fixation increased by 1.44 times when 2 weeks of simulated weightbearing were cycled, because of motion of the screw at the articular surface. The second metatarsal (M2) showed the greatest increase (1.54-fold, P = .0047), whereas the first (M1) showed the least (1.35-fold, P = .0083). 15
There was only a single study identified in our search in the past 10 years directly examining a cohort of TAS patients. We therefore looked further into the past at Kuo et al, 32 who reported their experience treating 92 patients with open reduction and TAS over 7 years. Despite a loss to follow-up rate of 48%, they followed their patients for an average of 52 months (range 13-114 months). The mean American Orthopaedic Foot & Ankle Society (AOFAS) midfoot score was 77 points (range 40-100), considered to be an average to good result. Six patients (12.5%) required subsequent midfoot arthrodesis. In this study, the major determinant of outcome was anatomic reduction (P = .05), and purely ligamentous injuries showed a trend for worse outcomes in this series. 32
Park et al 42 published a retrospective series of 31 patients over 6 years. In this series, percutaneous reduction was achieved in purely ligamentous injuries with a pointed reduction clamp, and then medial to lateral fixation was undertaken using two 2.7-mm cortical screws. One patient required midfoot arthrodesis (3.2%), and 7 patients had screw breakage (22.6%). Body mass index was significantly higher in patients with broken screws. The authors concluded that 2.7-mm percutaneous cortical screw fixation is a viable option for treating these injuries in nonobese patients. 42
In 2022, Engelmann et al 17 performed a systematic review and meta-analysis of Lisfranc fixation comparing TAS to ABP. Only 4 studies were included in this analysis, and the authors excluded studies that did not have direct comparison groups. This analysis concluded that ABP had lower rates of post-traumatic osteoarthritis (OR 0.45, 95% CI 0.22-0.94, P = .03) and better AOFAS midfoot scores than TAS fixation (mean difference 7.08, 95% CI 1.50-12.66, P = .01). In this study, there were no differences in hardware removal, secondary arthrodesis, or postoperative infection rates. 17 In addition, a recent systematic review has suggested that TAS constructs placed percutaneously may lead to nonanatomic reduction. 52
Articular bridge plating
In 2003, Schildhauer and Sangeorzan were the first to propose a temporary bridge plating technique in the midfoot for fracture-dislocation injuries of the TMT joints. 49 Articular bridge plating is typically performed dorsally across the TMT joints, with some variability for the first TMT joint where plates may be placed medial or plantar (Figure 1). ABP can maintain length and does not violate the articular cartilage. It is also useful in the setting of the comminution of metatarsal bases. One of the initial difficulties with this technique was the limited space for screw placement, leading to the development of midfoot-specific implants with variable angle locking screw options. An illustrative case of an ABP technique with an additional “Lisfranc screw” from the base of the second metatarsal to the medial cuneiform is shown in Figure 1.
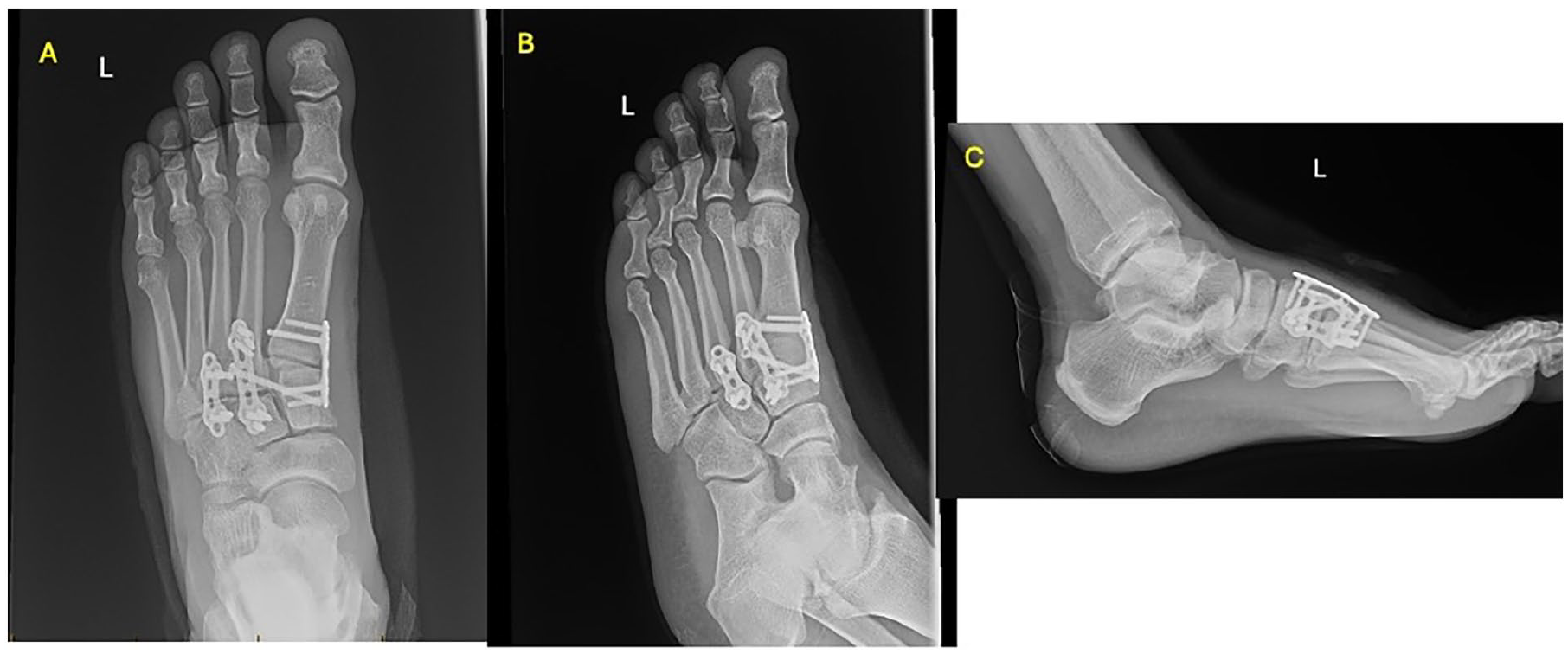
A 35-year-old man was treated with open reduction, internal fixation for a Lisfranc injury sustained in a motorcycle accident. Postoperative radiographs are shown (A-C). He underwent dorsal bridge plating of TMT joints 1-3. After reduction, a screw is placed from the base of the second metatarsal to medial cuneiform to maintain reduction between rays and protect the Lisfranc ligament.
In 2014, Stern and Assal 53 reported their experience in a retrospective cohort of 15 patients in whom they treated Lisfranc injuries with dorsal plating alone without any trans-articular screws. If the lateral column needed to be stabilized, this was performed with K-wires. All hardware was removed 4 months after surgery. At a follow-up of 1 year, the mean reported AOFAS midfoot score was 85 points (range, 78-92). This technique maintained radiographic reduction in all patients without any instances of hardware failure. Two patients had delayed wound healing, but there were no cases of infection or unexpected secondary surgery. The follow-up was not long enough in this series to evaluate for secondary arthrosis and arthrodesis. 53
Abbasian et al 1 subsequently reviewed their series of 58 patients who underwent a combination of TAS and ABP, all with routine hardware removal. The authors compared subgroups of purely ligamentous and osseous injuries. They reported no difference between the 2 injury patterns regarding PROMs and complications. Good outcomes were obtained in both groups, with a mean AOFAS midfoot score of 84 in the ligamentous group (range 27-100) and 85 (range 45-100) in the osseous group (P = .34). The authors concluded that primary arthrodesis was not routinely justified in ligamentous injuries. 1
In 2016, Van Koperen et al 55 were the first to describe the routine use of locking bridge plates for Lisfranc injuries. In their series of 36 patients, 21 were treated with ABP using locking plates. In the other 13 patients, K-wires or transarticular screws or a combination were used. When comparing patients treated with locking ABP to those without, there were no significant differences in AOFAS midfoot scores. There were similar hardware removal and complication rates. The authors postulated that longer follow-up (their series involved a mean follow-up of 21 months) might reveal any differences in TMT arthrosis potentially caused by violating the joint with transarticular screws. 55
Similarly, Davey et al 12 reviewed 37 patients over an 8-year period who underwent ABP for a combination of osseous and ligamentous injuries. At medium-term follow-up, 85.6% (32/37) of patients were satisfied and had good functional outcomes. More than half of the patients (56.7%) underwent subsequent plate removal, with hardware removal planned in another 10.8% at publication. There were no significant differences in reported AOFAS scores and residual pain levels between those who underwent ABP removal and those who elected not to have their plates follow-up (P = .664 and P = .909, respectively). The mean AOFAS midfoot score in this series was 77.4 ± 23.8, consistent with other published series on ABP. 12
Lisfranc-specific plating
In recent years, specific plating systems have been designed for Lisfranc injuries. These overcome one of the issues noted with ABP techniques, in that TMT bridging plates do not provide stability between columns. Lisfranc-specific plates are designed to span across TMT joints and also the medial and middle columns of the foot. These typically have “h-shaped” or “diamond” configurations (Figure 2). Ho et al 21 reported their results of a cadaveric model comparing a novel Lisfranc-specific diamond plate to TAS. They observed no significant difference in load to failure (absolute force or cyclical loading) or joint displacement between these 2 groups. Of note, the authors reported that with cyclical loading, both the TAS and Lisfranc-specific plating constructs failed at loads well above physiological levels. 21 These spanning plates represent an alternative to traditional 2- or 3-plate techniques. Our literature search did not identify clinical series comparing these devices to traditional TAS or ABP methods.

“Lisfranc-specific” plating device. Preoperative radiographs (A, B) of a patient with a tarsometatarsal fracture/dislocation demonstrate clear base of second metatarsal fracture, with Lisfranc diastasis and dorsal subluxation of the joints. This patient was treated with a bridge plating technique using a diamond shaped plate that spans the first and second rays, and due to residual instability, an additional plate spanning the third TMT joint (C, D).
Dynamic Fixation
A potential drawback of all TAS and ABP techniques is that there is hardware spanning a mobile joint. Many surgeons therefore agree that such hardware should be routinely removed, adding both cost and risk. 19 That said, this notion was recently challenged during the COVID-19 pandemic, when patients could not access hospitals for elective hardware removal. Recent literature from the United Kingdom suggests that bridging plate retention may be acceptable. A retrospective cohort study examined 85 patients from a level 1 trauma center where hardware removal was not routinely offered to patients. Hardware was removed only as needed; the authors did not specify the specific reasons for removal. 40 The authors reported a 21% hardware removal rate, more likely in female patients. In addition, 9.4% of this cohort went on to have secondary arthrodesis. A systematic review 48 also suggests that this hardware-retention approach may be safe, but this approach lacks prospective clinical data.
As the debate regarding the removal of hardware evolves, flexible fixation is a new alternative for surgeons seeking to avoid planned secondary surgery in patients with Lisfranc injuries. The different flexible constructs are detailed below.
Suture button devices
Suture button devices have recently been used to stabilize the Lisfranc articulation. Ahmed et al 3 examined the biomechanical stability of these devices in a cadaveric model that did not include sectioning of the ligaments. These authors reported that although a suture button construct showed 1 mm greater diastasis (P < .001) than a single screw under physiologic loads, there was no difference between constructs in load to failure. 3 Meanwhile, Panchbhavi et al 41 performed a cadaveric study in which the ligaments of the midfoot were sectioned. The authors compared a suture button device from C1-MT2 to a similarly placed single 3.5-mm cannulated screw. They found that both techniques were effective at limiting displacement compared with an unfixed injury and that there was no significant difference between the constructs. The authors concluded that a suture button is an acceptable alternative to screw fixation. Notably, this study was sponsored by the manufacturer of the suture button device. 41 Another biomechanical study by Pelt and colleagues demonstrated that both suture-button and screw fixation constructs restrained motion at the Lisfranc complex without a significant difference between the two constructs. 43
Regarding clinical data with this technique, Cho et al 8 published a retrospective series of 63 patients comprising 32 TAS and 31 suture button cases. At the 6-month review prior to screw removal, there was a significant improvement in AOFAS midfoot score in the suture button group compared to the TAS group; however, at 12 months, there was no difference in clinical or radiologic outcomes. Of note, this study included pedobarographic data which demonstrated increased plantar pressure at the first MT head just before screw removal. 8
A small retrospective series (12 cases) of elite athletes treated with a suture button device for purely ligamentous Lisfranc injuries demonstrated encouraging results with early return to full weightbearing at 4 weeks postoperatively and return to full competition at 12-16 weeks, without major complications. Minimum follow-up in this series was 2 years. 54
Cottom et al 11 published a larger retrospective series of 84 patients with purely ligamentous injuries. They performed suture button fixation from MT2-C1 and 4.0-mm cannulated screw fixation from C1 to C2. Minimum follow-up was 3 years. The authors reported that this hybrid fixation/suture button fixation technique was associated with promising AOFAS midfoot scores (mean 90.64, range 78-100). Meanwhile, the mean VAS score improved from 8.4 to 1.3. The mean preoperative step-off between the base of the second metatarsal and the intermediate cuneiform improved from 3.15 mm preoperatively to 0.43 mm at final follow-up. No suture buttons failed or needed to be removed. Nine patients (11%) had removal of the intercuneiform cannulated screw for “loosening or residual pain.” 11
Finally, a 2023 systematic review of 11 studies concluded that the suture button device is comparable to traditional screw fixation with regard to both clinical and radiographic results (AOFAS midfoot scores, VAS, return to function, and radiographic reduction). 9
Ligament reinforcement technique
Responding to concerns about the amount of articular cartilage violated and the potential for latent diastasis due to “creep” with a suture button device, the most recent evolution in flexible fixation has been the use of a ligament reinforcement technique (LRT) with suture tape.
This technique involves passing the suture tape from the second metatarsal base to the medial cuneiform. The construct is secured with a metallic suture button on MT2 and an interference screw within C1. In addition, an extension of the construct to include an “over-the-top” reinforcement from C1 to C2 has been described.23,31 LRT can also be combined with the plating of individual TMT joints if required. A potential advantage of this technique over the suture button technique is the smaller-diameter drill hole required to pass the implant, saving approximately 2 mm of articular cartilage.14,16 A case example can be seen in Figure 3 (C and D, isolated LRT; E and F, LRT in combination with plating).

Flexible fixation construct for Lisfranc injuries. T2-weighted (A) axial and (B) coronal images demonstrating hyperintensity in the second TMT and rupture of the Lisfranc ligament. In the purely ligamentous injury, the InternalBrace device can be used either as a standalone device (C, D) or in combination with plates spanning the TMT joints (E, F).
LRT has been evaluated biomechanically and compared to other fixation constructs.22,31 Hopkins et al 22 examined the mechanical properties of 3 fixation constructs in a purely ligamentous sawbones model. In this industry-sponsored study, the load to failure of a screw, suture button, and ligament reinforcement technique were examined. The authors found that load to failure was highest for the screw, whereas the suture button and LRT constructs were similar but lower than the screw. The authors noted that all 3 constructs were suitable for protected weightbearing. Meanwhile, Koroneos et al 31 examined the MT2-C1-C2 LRT construct (suture tape fixation as described above) and compared it to a C1-MT1 + C1-MT2 TAS in a cadaveric series of 16 feet. They found that under cyclical loading, the LRT showed equal stability to TAS. However, the screw construct used in this cadaveric model replicated the path of the LRT (ie, C1-C2 and C1-MT2) and, as such, probably does not reflect modern surgical technique. In addition, it should be noted that the models used in these series are only a biomechanical reflection of purely ligamentous injuries, and not fractures or dislocations.
Presently, the only clinical series published on LRT is from Hoskins et al, 24 who recently reported their early results in a pilot study of the LRT. Their retrospective series included 15 patients with an average follow-up of 7.3 months (range 1-15 months) with either purely ligamentous or minor avulsion injuries. They reported no revision surgery and no loss of fixation. In this series, the patients commenced full weightbearing at an average of 6.6 weeks and returned to work at an average of 14.1 weeks.
As described in the cadaveric study by Koroneos et al23,31 the ligament reconstruction reinforcement technique can be used to address not only C1-MT2 but also C1-C2 instability (see Figure 3, C and D). However, prospective clinical evaluation of this construct is not yet available in the published literature.
Table 2 summarizes the advantages and disadvantages of each of the fixation constructs discussed.
Summary of 4 Fixation Constructions for Open Reduction Internal Fixation of Tarsometatarsal (Lisfranc) Injuries.

Comparative Clinical Studies
Transarticular Screws vs Bridge Plating
Lau et al 35 reported a retrospective comparative study of a cohort of 62 high-energy trauma patients undergoing TMT stabilization by either screws, plates, or a combination of both. The patients in the dorsal plating group in this study all underwent transarticular MC-2MT screw fixation of the Lisfranc articulation. The primary outcomes in this study were radiographic, and no difference was noted when comparing fixation constructs. However, the patients who underwent a combination of plates and screws tended to have a nonanatomic reduction, and these patients showed significantly higher rates of TMT arthritis at final follow-up as measured by Kellgren-Lawrence grade. The authors surprisingly found that the plate fixation group tended to produce a more planus foot, as measured by the Meary angle. 35 In a follow-up study on the same cohort of patients, 34 the authors assessed functional outcomes using the AOFAS midfoot score and Foot Function Index. They found no difference in functional outcomes when comparing fixation constructs and instead found that the quality of anatomic reduction was the best predictor of patient outcome. 34
Meanwhile, Kirzner et al 29 published a series of 108 patients from a level 1 trauma center with comparisons between 38 patients who underwent fixation with TAS, 45 with ABP, and 25 with both TAS and ABP. The majority of these were high-energy injuries, including open injuries in 18% of cases. The authors reported better AOFAS midfoot scores (82.5 vs 71.1 vs 63.3, P < .001) and Manchester-Oxford Foot Questionnaire scores (25.6 vs 38.1 vs 45.5, P < .001) in the ABP group compared with either TAS or a combination technique. In this study, all treatment groups lost reduction over time; however, the rate of this was decreased in the ABP group. For all types of fixation, the authors noted that injuries requiring 3-column fixation performed worse on patient-reported outcome scores. As noted in other studies, the quality of reduction was a key determinant of functional outcome. Similar to Lau et al, 34 the authors acknowledge that in all patient groups, TAS was used across the Lisfranc joint, and in some cases in the plating group intercuneiform screws were also used.
Finally, Herbosa et al 20 retrospectively reviewed their hospital database and identified 70 patients (47 TAS and 23 ABP) who underwent Lisfranc fixation. Their data showed that clinical outcomes were equivalent and that the plating group demonstrated higher wound complications. A cost analysis of care demonstrated higher implant costs associated with the ABP method. 20
A Note on the Role of Primary Arthrodesis
Although not the primary focus of this review, we must acknowledge that primary arthrodesis (PA) is an accepted and common treatment option for Lisfranc injuries (Figure 4). PA has been reported to be superior to ORIF in the case of purely ligamentous injuries. Ly and Coetzee published a randomized controlled trial comparing ORIF to PA in 41 patients. At 2 years postoperatively, the PA group had higher AOFAS midfoot scores (P < .005). Five patients in the ORIF group had subsequent pain and were converted to arthrodesis. 38 One criticism of this article is that in the ORIF group, fixation was purely by transarticular screws that were left in place while patients were allowed to progress weightbearing. Subsequent studies examining this topic have produced conclusions both supporting and opposing this seminal study.27,28,44,47 Kirzner et al 28 examined the role of primary arthrodesis in a retrospective cohort of high-energy trauma patients and found that the primary arthrodesis group had superior patient-reported outcome scores (PROMs). 28 However, both Rammelt et al 47 and Joseph et al 27 have published recent studies that report superior outcomes with ORIF. Systematic reviews and meta-analyses on this topic have again been conflicting as well.2,5,59

A 45-year-old female patient was treated with primary arthrodesis of tarsometatarsal joints 1-3 after diagnosis of midfoot arthritis following from a missed Lisfranc injury 9 months prior. Postoperative radiographs demonstrate the (A) dorsoplantar, (B) oblique, and (C) lateral projections. The TMT joints were compressed with headless screws and then bridged here with a plantar Lapidus plate and dorsal plates for TMT joints 2 and 3.
In the authors’ clinical practice, the indications for ORIF are acute injuries <6 weeks, including both fracture/dislocations of the TMT joints and purely ligamentous Lisfranc injuries. The decision to stabilize with ABP or LRT construct depends on the injury pattern. We routinely remove bridge plates at approximately 4 months after the index procedure. Primary arthrodesis is considered when patients have severe fracture-dislocations (such as those requiring closed reduction and wiring as a temporizing measure) or severely comminuted injuries. It is also considered for chronic (>6 weeks) injuries as well as for elderly patients or patients with preexisting arthrosis.
Conclusion
In this review, we performed a literature search of English-language articles on the treatment of Lisfranc injuries over the past decade. The studies cover a heterogeneous group of patients encompassing high- and low-energy injuries. The optimal fixation construct for these injuries remains elusive. Several investigators have moved away from traditional fixation methods such as K-wires and transarticular screws toward articular bridge plates and flexible constructs. All examined constructs provide reasonable clinical results. The trend toward flexible fixation may have appeal because of decreased articular violation and less need for hardware removal. However, high-quality comparative clinical data are lacking.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251352519 – Supplemental material for Outcomes in Open Reduction and Internal Fixation of Tarsometatarsal (Lisfranc) Injuries: A Contemporary Review of Fixation Constructs
Supplemental material, sj-pdf-1-fao-10.1177_24730114251352519 for Outcomes in Open Reduction and Internal Fixation of Tarsometatarsal (Lisfranc) Injuries: A Contemporary Review of Fixation Constructs by Adrian J. Talia, Sasha Roshan-Zamir and David W. Shepherd in Foot & Ankle Orthopaedics
Footnotes
Ethical Approval
Ethical approval was not sought for the present study.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: David W. Shepherd, BSc(Hons), MBBS, FRACS (Orth.), FAOrthA, reports consultancy with Stryker: total ankle replacement proctor surgeon and symposium speaker; invited presenter at Arthrex Symposium 2023, delivered talk on Lis Franc management, but no contractual arrangement with Arthrex. Disclosure forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
