Abstract
Background:
Osteochondral lesions (OCL) of the talus are a significant cause of chronic ankle pain and functional impairment, typically following trauma. Despite advancements in diagnostic imaging and surgical interventions, long-term outcomes vary, and no gold standard treatment has been established.
Methods:
This retrospective study evaluated the outcomes of n=64 patients undergoing OCL-related surgery. Inclusion criteria: an OCL of the talus, patients without OCL, with osteoarthritis, or infection were excluded. The cohort was categorized primarily based on the stage of OCL and the surgical technique used: bone marrow stimulation by retrograde or anterograde drilling and microfracturing, transplantation of autologous cancellous bone, and acellular cartilage replacement and other procedures. Postoperative outcomes were assessed using the visual analog scale (VAS), the American Orthopaedic Foot & Ankle Society (AOFAS) score, and the Foot and Ankle Outcome Score (FAOS). Statistical significance was determined using χ2 tests, with P <.05 considered significant.
Results:
A total of 97 operations were performed on 64 patients. Fifty-six percent of patients reported complete resolution of symptoms, 25% experienced partial improvement, and 19% showed no improvement. Patients aged ≤30 years had a higher success rate (62.5%) compared with older patients (45.8%, P = .227). Success rates were significantly better for patients with stage II and III lesions (50% and 59%, respectively) than for those with stage IV lesions (P = .043). Material substitution had a success rate of 44.4%, bone marrow stimulation 37.8%, and other procedures 18.8%.
Conclusion:
Surgical techniques for treating OCL of the talus provide moderate success, but a significant proportion of patients, especially those with advanced lesions, remain symptomatic.
Level of Evidence:
Level IV, retrospective case series study.

Introduction
Osteochondral lesions (OCL) of the talus are a common cause of chronic pain and dysfunction in the ankle joint. 23 These lesions, which affect both the cartilage and subchondral bone, frequently occur after trauma, such as ankle sprains or fractures. 7 But it can also arise from repetitive microtrauma, congenital factors, or metabolic disorders.2,30 The unique biomechanical environment of the ankle, where the talus bears significant weight and pressure, makes these lesions difficult to treat effectively. 37
A variety of surgical techniques have been developed to address OCL, including bone marrow stimulation (eg, microfracture), material substitution (eg, autologous spongiosa grafts or synthetic scaffolds), and osteochondral autograft transplantation. 6 However, outcomes remain variable, and no single technique has emerged as the definitive treatment. The challenges in treating OCL are compounded by the lesion's size, location, and stage, as well as patient-specific factors such as age and activity level (Figure 1).14,41 Depending on the position of the talus at the time of impact, it may be necessary to perform a malleolus osteotomy during surgery. 15 However, this does not affect the relief or weightbearing of the affected ankle.

Magnetic resonance tomography (MRT) of the ankle joint showing an osteochondral lesion of the medial talus, stage III.
This study aims to evaluate the midterm outcomes of surgical treatments for OCL of the talus, to compare and, if possible, verify the patient's subjective data with results in various scores. In the case of persistent symptoms, the question arises as to which patients will benefit from revision surgery. The study focuses on the efficacy of different surgical approaches in relation to patient age, lesion stage, and type of procedure.
Materials and Methods
This retrospective study was conducted at the University Hospital. A total of 432 ankle operations were performed between 2015 and 2018. We included and analyzed the results of 97 operations performed on 64 patients with OCL. The study was approved by the local Ethics Committee (protocol number 79/19).
A total of 64 patients (37 males, 27 females) with a median age of 30 years (range: 11-68) were included in the study. Most patients (57.8%) had trauma-induced OCL, whereas 40.6% had chronic OCL. 24 Patients without an OCL at talus, with advanced osteoarthritis or postoperative infections were excluded.
The indication for surgery was given in the case of persistent symptoms projected onto the upper ankle joint and evidence of OCL of the talus in a magnetic resonance imaging (MRI), also for revision operations. It took an average of 15 months from symptom onset to clinic presentation and another 2 months before surgery. Prior conservative treatment with physiotherapy was unsuccessful. 32 Other causes of the symptoms (instability in the case of an external ligament lesion, pilon fractures, or osteoarthritis) were ruled out beforehand.
The surgical procedure was based on the stage of damage to the OCL in computed tomography (CT) or MRI and the intraoperative situation (Figure 2). 38 There was no randomized allocation or masked assignment of patients or procedures. The surgeon determined which acellular matrix was used. For stage 1, arthroscopically supported retrograde drilling was performed, in stages 2 to 3 antegrade drilling or refixation of the fragment (osteochondral autograft), in stages 3 to 4 relining of the fragment with cancellous bone (substitution with autologous cellular material) and refixation or, in the case of fragments that appeared too small or avital, additional replacement with acellular matrix.27,29 Depending on the location of the defect, an osteotomy of the malleolus was performed with subsequent osteosynthesis using screws (Figure 3). 28

Arthroscopy of the ankle joint, osteochondral lesion of the medial talus, stage III.

Osteotomy of the medial malleolus, acellular matrix (CaReS-1S Arthro Kinetics Biotechnology GmbH, Krems, Austria) on medial talus.
The classification into subgroups depends on the surgical procedure and the stage of the damage.
Patients underwent one of the following procedures:
Material substitution: This involved autologous spongiosa grafts or synthetic scaffolds such as autologous matrix-induced chondrogenesis.4,20
Bone marrow stimulation: Techniques included microfracture, retrograde drilling, and antegrade drilling, aiming to stimulate endogenous cartilage regeneration. 1
Other procedures: These included debridement, synovectomy, and cartilage smoothing, typically reserved for smaller or less severe lesions. 12
A minimum follow-up of 24 months was ensured to allow for the evaluation of midterm outcomes. The follow-up period ranged from 2 to 5 years, with a mean follow-up time of 3 years (SD = 1.58). At the time of follow-up, the outcomes were evaluated using the visual analog scale (VAS), American Orthopaedic Foot & Ankle Society (AOFAS) score, and the Foot and Ankle Outcome Score (FAOS). 3 The subjective information was additionally verified by a clinical examination, cross-sectional imaging (ie, MRI) and the Short Physical Performance Battery (SPPB) test. The clinical parameters include pain, symptoms, quality of life, sports ability, daily function, and alignment. The success of the operation was defined depending on the remaining symptoms. If the symptoms were alleviated, this was considered a partial success. Patients were not fully satisfied with their condition. If there were still functional disorders and persistent complaints, or if a new operation was performed, the previous operation was rated as unsuccessful. If subjective symptoms persisted, a further MRI scan was ordered. If the MRI findings correlated with the symptoms, various treatment options (conservative, revision surgery) were discussed. χ2 tests were used to assess statistical significance, with P <.05 considered significant.
Results
General Outcomes
The success of the operation and the possible need for further surgery were assessed using the clinical parameters and compared with the results of the VAS, AOFAS, FAOS, and SPPB scores. Except for the SPPB, the other valid scores can be used to assess the symptoms of OCL. Patients subjectively rated the success of the procedure based on their assessment of pain, function, strength, stability, and quality of life.
Of the 64 patients, 56% experienced complete resolution of symptoms, 25% showed partial improvement, and 19% remained symptomatic postoperatively. Patients who underwent a single surgery had a significantly higher success rate (63%) compared to those who had multiple surgeries (43%, P = .017) (Table 1).
Outcomes by Number of Surgeries (Patient Rating [PROMs]).

Abbreviation: PROMs, patient-reported outcome measures.
Influence of Lesion Stage
Patients with stage II and III lesions had significantly better outcomes (50% and 59% success rates, respectively) compared to those with stage IV lesions (P = .043). Stage I lesions were less common (n=3) and partially associated with worse outcomes, but the number of patients in this subgroup was too small to draw statistically robust conclusions. (Table 2).
Surgical Success by OCL Stage (Patient Rating [PROMs]).

Abbreviations: OCL, osteochondral lesions; PROMs, patient-reported outcome measures.
Age-Related Outcomes
Younger patients (≤30 years, mean age 22.3 years) had a higher success rate (62.5%) compared with older patients (45.8%, mean age 45 years), although this difference was not statistically significant (P = .227) (Table 3).
Surgical Success by Age Group (Patient Rating [PROMs]).

Abbreviation: PROMs, patient-reported outcome measures.
Comparison of Surgical Techniques
In the 97 operations, cellular and/or acellular material was substituted 36 times. Transplantation of autologous spongiosa was performed 14 times and acellular materials were substituted 22 times (15 times CaReS-1S, 7 times Chondro-Glide from Geistlich).
Bone marrow stimulation was performed in 45 of the 97 procedures, and other procedures such as synovectomy were performed 16 times. Material substitution and bone marrow stimulation had similar success rates (44.4% and 37.8%, respectively), while other procedures, such as debridement, were less successful (18.8%). There was no significant difference between material substitution and bone marrow stimulation (P = .435) (Table 4). Substitution of acellular materials had a success rate of 50%, and substitution of cellular materials alone had a success rate of 36.7%. No significant relationship was found (χ2 = 0.797, P = .671).
Surgical Technique Success Rates (Patient Rating [PROMs]).
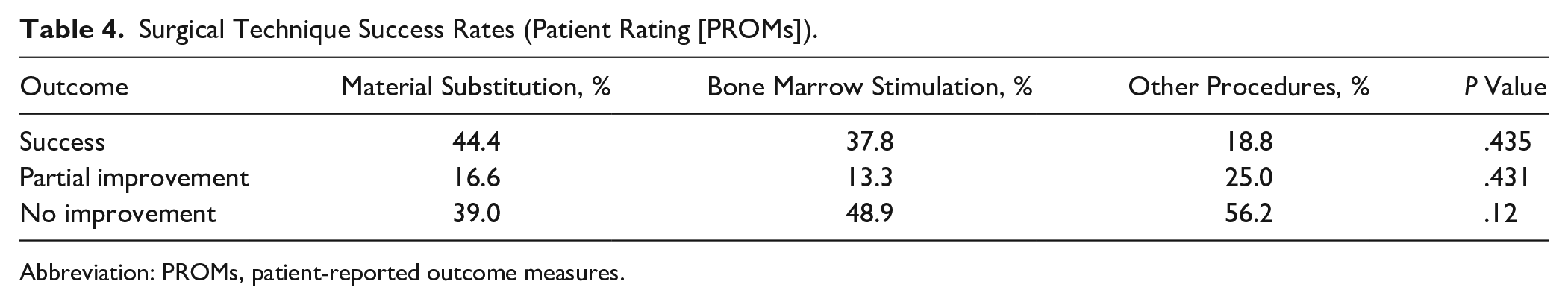
Abbreviation: PROMs, patient-reported outcome measures.
Comparison of Single and Multiple Operations
Of the 64 patients in the collective, 43 cases of OCL were cured after a single surgery. The success rate was 63%. Twenty-one patients continued to have problems and required multiple operations (2-5 times). The success rate decreased from 63% for single surgeries to 43% for multiple operations (P = .017).
Of the total 33 multiple operations, 25 involved a change of procedure and 8 involved the same procedure. Overall, reoperation improved the outcome in 51.5% of cases (27.3% success, 24.2% improvement only). No success was achieved in 48.5% of cases.
Discussion
This study provides valuable insights into the effectiveness of different surgical techniques for treating OCL of the talus, particularly when analyzing variables such as patient age, lesion stage, and type of surgery performed. Our findings demonstrate that while many patients benefit from surgery, a substantial portion continues to experience symptoms, especially in more advanced stages.
Impact of Surgical Techniques
Surgical interventions for OCL of the talus, including material substitution and bone marrow stimulation, have shown varying degrees of success. In our study, material substitution demonstrated a success rate of 44.4%, whereas bone marrow stimulation yielded a slightly lower success rate of 37.8%. These results are consistent with previous reports in the literature, which suggest that although these methods can be effective, they often fail to restore the full biomechanical integrity of the talar cartilage, particularly in larger or more advanced lesions.9,35
The use of autologous spongiosa grafts and synthetic materials, such as autologous matrix-induced chondrogenesis, is a popular approach for larger defects. 18 However, success with this technique is often limited by the extent of the lesion and the quality of the surrounding tissue. 13 Microfracture, a widely used form of bone marrow stimulation, has been shown to yield favorable outcomes in smaller lesions, but long-term results are less promising, especially in athletes and those with higher functional demands.16,21 Studies have also indicated that microfracture alone may not be sufficient for lesions larger than 1.5 cm2, where other surgical techniques, such as osteochondral autografts or allografts, may be more appropriate.11,40
Influence of Lesion Stage on Outcomes
The stage of the OCL is a critical factor influencing surgical outcomes. In our study, patients with stage II and III lesions had significantly better results (50% and 59% success rates, respectively) compared with those with stage IV lesions, where success was only 15% (P = .043). These findings align with previous research that emphasizes the importance of early detection and intervention.5,26 Advanced-stage lesions, such as those in stage IV, are often associated with subchondral bone involvement, larger defect sizes, and increased joint instability, all of which reduce the chances of successful cartilage regeneration following surgery.31,36
The results suggest that surgical intervention is most effective when performed in the earlier stages of OCL, before the lesion progresses to the point where surrounding structures are compromised. 16 This underscores the importance of accurate staging, which can be accomplished using advanced imaging modalities like MRI and CT scans. 34 Our study supports the use of these imaging tools not only for diagnosis but also for monitoring the progression of the lesion postoperatively (Figures 4 and 5). 19

Magnetic resonance imaging scan (T2-weighted, coronal view) of the ankle joint at 4-year follow-up shows osteochondral lesion of the medial talus, stage III.

Magnetic resonance imaging scan (T1-weighted, sagittal view) of the ankle joint at 4-year follow-up shows osteochondral lesion of the medial talus, stage III.
Age-Related Outcomes
Age plays a significant role in the success of surgical interventions for OCL. In our study, younger patients (≤30 years) had a higher success rate (62.5%) compared with older patients (45.8%), though, importantly, the difference was not statistically significant (P = .227). This trend is consistent with findings from other studies, which suggest that younger individuals have better regenerative capacity, leading to improved outcomes after cartilage repair procedures.33,40 The greater regenerative potential in younger patients may be due to the increased number and activity of mesenchymal stem cells in the bone marrow, which are crucial for cartilage repair.34,39 However, older patients may experience less favorable outcomes because of age-related degeneration of the cartilage and subchondral bone, which can impair the healing process. In such cases, more aggressive interventions, such as osteochondral autograft transplantation or the use of advanced biomaterials, may help achieve satisfactory results. 25
Comparison of Single vs Multiple Surgeries
Patients who underwent multiple surgeries were less likely to experience successful outcomes compared to those who had a single surgery. Our data showed that success rates dropped from 63% in single surgeries to 43% in patients who had multiple surgeries (P = .017). This decline in success may be attributable to several factors, including the formation of scar tissue, reduced joint space, and the impact of repeated surgical trauma on the surrounding tissues. 22 The literature supports this finding, as multiple surgeries are often associated with diminished outcomes, particularly in cases where revision surgeries involve the same technique.10,30 In our study, many patients who underwent revision surgeries had switched from one technique to another, such as moving from microfracture to material substitution, in an attempt to improve outcomes. However, the results suggest that even with a change in technique, the cumulative damage from repeated interventions reduces the likelihood of a successful outcome. 17
Limitations
Although this study provides valuable insights into the progress results of OCL treatments, there are several limitations that should be noted. First, the retrospective nature of the study introduces potential biases, such as selection bias, and limits the ability to control for confounding variables, such as variations in postoperative rehabilitation protocols. 8 Additionally, the sample size is relatively small, which may limit the generalizability of the findings to a broader population. Another limitation is the lack of long-term follow-up for the patients. Although we were able to assess outcomes up to several years postoperatively, a more extended follow-up period would be ideal for evaluating the durability of the surgical interventions, particularly for techniques like bone marrow stimulation and material substitution, which may deteriorate over time. 9 Furthermore, the study did not include a control group of patients who received conservative management, which could have provided valuable insights into the effectiveness of surgical intervention compared to nonsurgical approaches.
Conclusion
The results of this study highlight the challenges of treating OCL of the talus, particularly in advanced-stage lesions. Although surgical techniques like bone marrow stimulation and material substitution can provide symptom relief for many patients, a significant portion remains symptomatic postoperatively. The results of the study show a trend in treatment. Patients <30 years of age with OCL stages II and III may benefit most from surgery. The best results we had were achieved with bone stimulation in combination with autologous matrix-induced chondrogenesis.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251329378 – Supplemental material for Midterm Outcomes and Surgical Approaches for Osteochondral Lesions of the Talus
Supplemental material, sj-pdf-1-fao-10.1177_24730114251329378 for Midterm Outcomes and Surgical Approaches for Osteochondral Lesions of the Talus by Christoph Biehl, Carina Fritzsche, Nike Walter, Lotta Biehl, Thaqif El Khassawna, Christian Heiss and Markus Rupp in Foot & Ankle Orthopaedics
Footnotes
Ethical Approval
The study was conducted in accordance with the guidelines of the Declaration of Helsinki and approved by the local ethics committee at Justus Liebig University (protocol number 79/19) on May 8, 2019. This retrospective study was conducted at the University Hospital of Giessen.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of Data and Materials
The data sets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
