Abstract
Background:
Calcaneal lengthening osteotomy (CLO) is frequently utilized to treat painful flexible flatfoot (FF) in children. The purpose of this investigation is to analyze the impact of CLO on patient reported pain and mobility using Patient Reported Outcome Measurement Information System (PROMIS) scores in a cohort of pediatric patients treated for painful FF.
Methods:
Children aged 8-18 who underwent CLO for painful FF correction were included. Retrospective chart review for PROMIS scores of pain and mobility were collected. Preoperative PROMIS scores were compared to PROMIS scores collected within 6-12 months postoperatively. Five PROMIS points was determined to be a minimal clinically significant difference, as this is half of the SD of the PROMIS metric. Preoperative and postoperative AP/lateral talo–first metatarsal angles were collected and compared. The patients with residual pain (PROMIS >55) after CLO were evaluated, and the effect of potential factors on residual postoperative pain was assessed.
Results:
Twenty-one patients with 31 feet were included in the study, with an average age of 12.2 (range, 9-15) years at the time of surgery. Mean preoperative pain and mobility PROMIS scores were 53.6 (range, 32.2-69.6) and 42.5 (range, 25.5-56.4), respectively. Mean postoperative pain and mobility PROMIS scores were 47.1 (range, 32.0-59.0) and 48.3 (range, 31.6-61.7), respectively. Patients who received CLO had significant improvement in both pain (P = .005) and mobility (P = .017). Average pain and mobility decreased by 6.51 points and increased by 5.81 points, respectively, after CLO, both clinically significant improvements.
Conclusion:
In early follow-up, we found the use of calcaneal lengthening osteotomy used to treat children for painful idiopathic flexible flatfoot to be associated with significant improvements in pain and mobility PROMIS scores.
Level of Evidence:
Level IV, retrospective case series study.
Introduction
Flexible flatfoot (FF) is a common foot deformity found in up to 15% of children older than preschool age. Flatfeet are typically painless, but they can also be associated with pain and decreased mobility in some children, especially if associated with tendo-Achilles contracture.2,4,8,22
Initial treatment is often conservative in the form of physical therapy focusing on stretching of Achilles tendon contracture, orthotic inserts, and antiinflammatory medications to reduce pain and promote mobility.9,34 If such methods fail to achieve clinical improvement, surgical correction is considered, with calcaneal lengthening osteotomy (CLO) being the most commonly performed procedure in these patients. 19 In this procedure popularized by Mosca, 22 lengthening of the lateral column of the foot through the calcaneus results in correction of the lack of talonavicular coverage. This procedure has been shown to relieve pain and improve radiographic parameters associated with the painful flatfoot deformity. 16
Patient-reported outcome measures (PROMs) are increasingly used to determine the efficacy of orthopaedic procedures. Traditional PROMs, such as the American Orthopaedic Foot & Ankle Society (AOFAS) scores, are commonly used in pediatric populations but lack validation. For example, AOFAS scores have demonstrated significantly improved outcomes in children with painful flatfoot deformity following calcaneal lengthening osteotomy; however, their limitations include subjective clinician scoring.11,29,35 Similarly, the Oxford Ankle Foot Questionnaire, which has been validated, is often used to evaluate patient-reported outcomes in children. 32
The Patient-Reported Outcome Measurement Information System (PROMIS) represents a more advanced and versatile tool compared with traditional PROMs, particularly for chronic pediatric conditions. It allows for a quick computer adaptive survey, accommodating both patient- and proxy-reported outcomes. Several domains measured by the PROMIS system allow for a more comprehensive assessment of the outcomes of procedures and interventions and, thus, play a significant role in the field of orthopaedic surgery. These domains include pain, mobility, and upper extremity function. Developed in 2004, PROMIS has undergone extensive validation across a variety of chronic pediatric orthopaedic procedures and conditions, including ACL reconstruction, arthrogryposis, brachial plexus birth injury, Legg-Calves-Perthes disease, and talipes equinovarus.3,12,18,20,21,28,36 Recently, PROMIS was endorsed by AOFAS as a valuable outcome measure for assessing a variety of foot and ankle disorders, further underscoring its potential utility in orthopaedic practice. 13
At this time, little is currently known regarding PROMIS scores for patient-reported outcomes of calcaneal lengthening osteotomy in the treatment of painful flexible flatfoot in the pediatric population. The focus of this study is to analyze the efficacy of calcaneal lengthening osteotomy in the improvement of pain and mobility in pediatric patients suffering from painful flexible flatfoot deformities.
Methods
This study received institutional review board approval to create a retrospective database of pediatric patients who received calcaneal lengthening osteotomy from the years 2016 to 2020. Patients were seen at a tertiary care center at the author’s institution. PROMIS surveys for pain and mobility were prospectively obtained after completing a short computer-adapted survey (average completion time: 3 minutes). Patients or caregivers and their physicians received numerical scores representing the patient’s pain and mobility at the time of the survey, specifically completed as part of standard patient intake both preoperatively and postoperatively.14,15 A retrospective chart review was then completed for PROMIS surveys of pain and mobility at both preoperative and postoperative times in patients who underwent calcaneal lengthening osteotomy to correct symptomatic flexible flatfeet.
Radiographic parameters were measured using standing anteroposterior (AP) and lateral views; however, measurements requiring the Saltzman hindfoot views were excluded as they were not collected in our cohort of flexible flatfoot. Measurements included preoperative and postoperative weightbearing AP/lateral talo–first metatarsal angles, calcaneal pitch, talonavicular uncoverage, incongruency angle as described by Ellis et al, and medial cuneiform–fifth metatarsal height (MC-5MH) as defined by Younger et al.7,37 MC-5MH was denoted as negative if the medial cuneiform was positioned plantar to the inferior part of the base of the fifth metatarsal. Similarly, incongruency angle was denoted as negative given the lateralmost point of the navicular articular surface was positioned more medially than the lateralmost point of the talar articular surface, as typically seen after surgical correction of flexible flatfoot. Such measurements were completed on each foot receiving calcaneal lengthening osteotomy and are detailed in Figure 1.
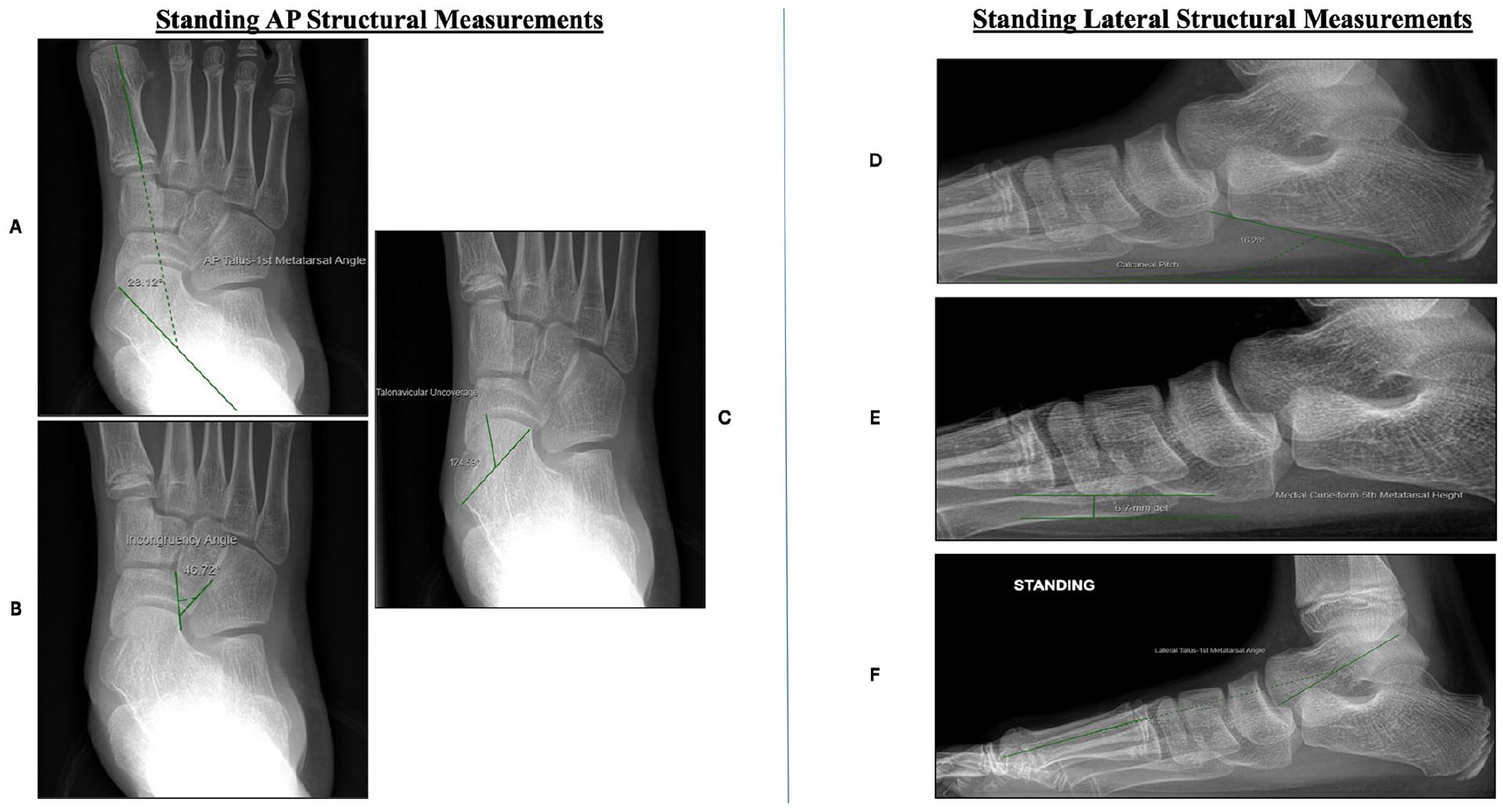
AP/lateral radiographic measurements: (A) AP talo–first metatarsal angle: measurement between the axis of the talus and the first metatarsal. (B) Incongruency angle: a line is drawn between the lateralmost articular point of the talus and the navicular, followed by another line extending from the narrowest part of the lateral talar neck to the lateralmost point of the talar articular surface. A negative angle indicates that the lateralmost point of the navicular articular surface is positioned medial to the line between the talar neck and the articular surface. (C) Talonavicular uncoverage (%): a line first drawn across the poles of the talar articular surface, followed by a line perpendicular to the medialmost point of the navicular articular surface. The angle created on the medial side is divided by 180 degrees to calculate the uncoverage percentage. (D) Calcaneal pitch: a horizontal line is drawn along the base of the foot, a second line drawn inferior to the calcaneus, connecting the calcaneal neck to the calcaneal tubercle. (E) Medial cuneiform–fifth metatarsal height: a horizontal line is drawn on the inferiormost point of the base of the fifth metatarsal, followed by another horizontal line at the inferiormost point of the medial cuneiform. The distance between these 2 points represents the height. A negative value indicates that the medial cuneiform is positioned plantar to the fifth metatarsal. (F) Lateral talo–first metatarsal angle: measurement between the axis of the talus and the first metatarsal.
Although CLO was the primary focus of this study, we also recognize that other surgical techniques exist, such as medializing calcaneal osteotomy, often used in certain patient populations. These procedures may provide additional correction in select cases; however, in our cohort of symptomatic flexible flatfeet, CLO remains a well-established procedure at our institution.
In patients who underwent a unilateral procedure, preoperative PROMIS scores for pain and mobility from the most recent visit before surgery were compared to the final postoperative PROMIS scores for pain and mobility collected within 6-12 months after surgery. In patients who received surgical correction of both feet during the study period, the preoperative PROMIS scores of the first procedure were compared to the final postoperative PROMIS scores within 6-12 months after the second procedure was performed. This method was chosen so that the preoperative pain and mobility scores of the second procedure would not be affected by the postoperative recovery process of the first procedure. During the procedure, an osteotomy is performed 1.5 to 2 cm proximal to the calcaneocuboid joint, and a tricortical allograft is placed within the space. Gastrocnemius recession or Achilles lengthening will be performed based on the intraoperative examination. If fixed supination deformity of the forefoot was present, a medial cuneiform plantarflexion osteotomy was performed.
Inclusion criteria for this analysis focused on pediatric patients between the ages of 8 and 18 years with a diagnosis of painful flexible flatfeet with minimum 6 months’ follow-up since the procedure. Eight years was determined to be the minimum age of inclusion for the pediatric patients in this study because, prior to this age, the medial longitudinal arch is not fully developed, and surgical correction of flatfeet is often not considered. Exclusion criteria included disorders that affect mobility such as neuromuscular pathology, prior surgical intervention that may potentially affect mobility, previous surgical correction of the flatfeet before undergoing calcaneal lengthening osteotomy, or any rigid flatfoot deformities ranging from idiopathic to other pathologies including tarsal coalition.
Statistical analysis included paired t tests between preoperative and postoperative PROMIS scores and talo–first metatarsal angles using SPSS 27. PROMIS scores from the most recent preoperative follow-up were used in the preoperative score category and were compared to PROMIS scores collected from final follow-up visits 6-12 months after surgery. Paired t test was used to compare the means of these 2 groups, and P <.05 was used to determine statistical significance. The average score for all PROMIS domains is 50 of 100, with a SD of 10. The minimal clinically important difference (MCID) will be determined by a difference of 5 PROMIS points, as this is half of the SD of the PROMIS metric. This aligns with the methodology of the distribution-based approach to determining the MCID of a scoring system, as outlined by Rai et al. 26 Residual pain after the procedure will be evaluated by determining the number of patients with postoperative pain PROMIS scores >55 at the time of final follow-up 6-12 months after surgery.
Results
A total of 31 feet in 21 patients matched the inclusion criteria. Of these patients, 10 received surgery on both feet in different surgical settings, and 11 received unilateral procedures. Nineteen of the 31 feet underwent medial cuneiform osteotomy at the time of CLO. Twenty-three feet underwent gastrocnemius recession, with an additional 5 receiving Achilles tendon lengthening. Of the 21 patients, 4 (19%) displayed residual pain; this was specifically observed in 5 feet (16%), between 6 and 12 months of follow-up as a complication. Otherwise, none of the 31 feet were found to have wound complications reported in the electronic medical records after receiving CLO or any other concurrent procedures.
The average age of the patients was 12.24 years at the time of surgery (range, 9-15). Patient demographic information is detailed in Supplemental Table S1. Table 1 includes a summary of the preoperative and postoperative PROMIS scores for both pain and mobility. The average preoperative pain PROMIS score improved significantly from 53.63 (SD = 8.48) to 47.12 (SD = 9.00, P = .005) at 6-12 months’ follow-up whereas the average preoperative mobility PROMIS score improved significantly from 42.50 (SD = 6.66) to 48.31 (SD = 9.04, P = .017). The magnitude of improvement in both pain and mobility scores (reduction of 6.51 points in pain and improvement of 5.81 points in mobility) was greater than the minimum clinically significant amount for PROMIS scores and are considered clinically significant. Table 2 displays mean postoperative pain and mobility PROMIS scores based on each patient’s final follow-up period within the 6-12-month time frame. Six patients were grouped in the 6-8-month group, followed by 7 in the 8-10-month group and 8 in the 10-12-month group. Gradual increase in mobility scores with decline in pain scores can be observed. Four patients (19%) reported residual pain at the time of final follow-up between 6 and 12 months.
Mean Pre- and Postoperative PROMIS Scores for Pain and Mobility (N = 21). a

Abbreviation: PROMIS, Patient-Reported Outcome Measurement Information System.
Postoperative PROMIS scores are taken from final follow-up 6-12 months after surgery.
Bolded P value represents statistical significance.
Summary of Mean Pain and Mobility PROMIS Scores at Each Final Follow-up Interval Between 6 and 12 Months After Surgery.

Abbreviation: PROMIS, Patient-Reported Outcome Measurement Information System.
Table 3 displays the comparison between preoperative and postoperative AP/lateral structural measurements in all 31 feet. A statistically significant improvement was found in AP talo–first metatarsal angles after CLO (P < .001). There was also a statistically significant improvement in talonavicular uncoverage percentage, incongruency angle, calcaneal pitch angle, and medial cuneiform–fifth metatarsal height (P < .001).
Comparison Between Preoperative and Postoperative Structural Measurements in All 31 Feet That Underwent CLO
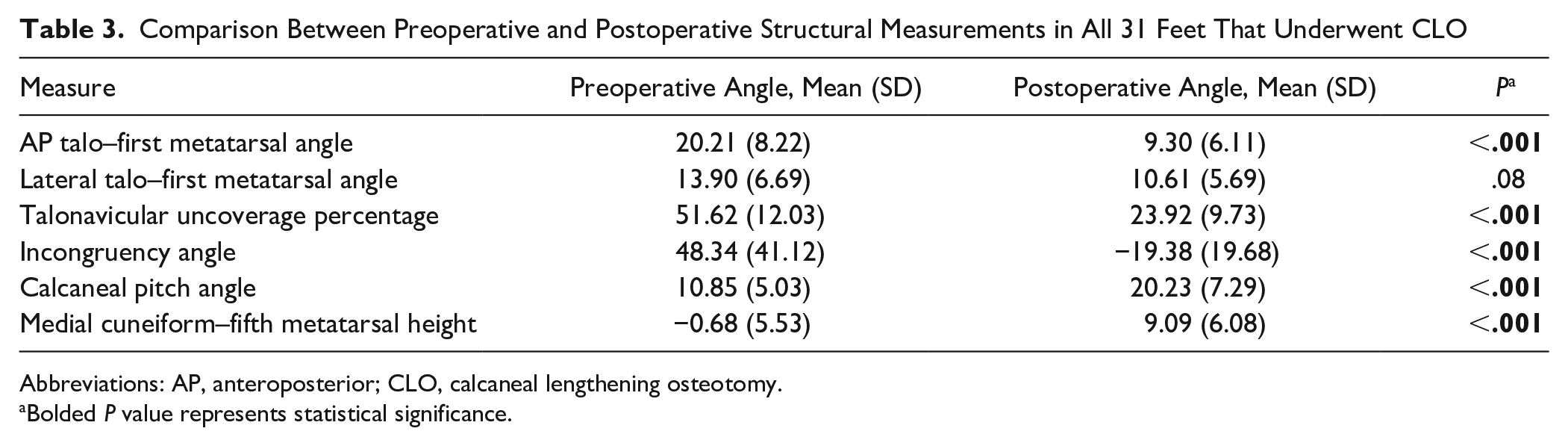
Abbreviations: AP, anteroposterior; CLO, calcaneal lengthening osteotomy.
Bolded P value represents statistical significance.
Table 4 provides detailed demographic and management data for the 5 feet with ongoing pain. Additionally, it includes a comparison of preoperative and postoperative PROMIS scores and radiographic measurements, including AP/lateral talo–first metatarsal angles, talonavicular uncoverage percentage, calcaneal pitch, incongruency angle, and MC-5MH. Table 5 displays the comparison between preoperative and postoperative radiographic measurements and pain PROMIS scores, age, and BMI in the 4 patients with residual postoperative pain and 17 patients with satisfactory postoperative pain. A clinically significant difference was found between preoperative pain PROMIS scores, with the residual pain group having a mean preoperative PROMIS score that was 7.04 points greater than the mean preoperative pain score of the satisfactory postoperative pain group. Analysis of postoperative pain PROMIS scores showed a significant difference of 12.7 points, with a greater pain score in the residual pain group (P = .007).
Comparisons Between the 5 Residual Pain Cases Observed in Our Cohort. a

Abbreviations: AP, anteroposterior; MC-5MH, medial cuneiform–fifth metatarsal height; MCO, medial cuneiform osteotomy, PROMIS, Patient-Reported Outcome Measurement Information System.
Cases 4 and 5 represent the same patient requiring bilateral symptomatic flatfoot correction.
Comparison of the Patients With Satisfactory Postoperative Pain PROMIS Scores and Those With Residual Pain (PROMIS Score >55) After CLO

Abbreviations: AP, anteroposterior; BMI, body mass index; CLO, calcaneal lengthening osteotomy; MC-5MH, medial cuneiform–fifth metatarsal height; MCO, medial cuneiform osteotomy; PROMIS, Patient-Reported Outcome Measurement Information System.
Bolded P value represents statistical significance.
Table 6 compares preoperative and postoperative radiographic measurements and PROMIS scores between patients undergoing isolated CLO and those requiring a combination of MCO with CLO. Figure 2 demonstrates pre- and postoperative radiographs between those underoing isolated CLO and those requiring a combination of MCO and CLO. Of the total cohort, 19 of 31 feet (61.3%) underwent the combined MCO and CLO procedure. The average preoperative MC-5MH was significantly greater in patients undergoing the isolated CLO procedure (1.96) compared with those undergoing the combined procedure (−2.34; P = .03). Otherwise, no other significant differences were observed in radiographic measurements or PROMIS scores between the 2 groups.
Comparison Between Patients Undergoing CLO and Those Who Underwent Both CLO and MCO

Abbreviations: AP, anteroposterior; CLO, calcaneal lengthening osteotomy; MCO, medial cuneiform osteotomy; PROMIS, Patient-Reported Outcome Measurement Information System.
Bolded P value represents statistical significance.

Pre- and postoperative calcaneal lengthening osteotomy vs calcaneal lengthening osteotomy + medial cuneiform osteotomy radiographs.
Discussion
We present the first study investigating the outcomes of calcaneal lengthening osteotomy for the treatment of symptomatic flexible flatfeet in pediatric patients using PROMIS metrics and found clinically and statistically significant improvement in pain and mobility and all radiographic parameters.
Since being popularized by Mosca, 22 CLO has been shown to result in improved radiographic and clinical outcomes in children with painful FF. Several studies have previously investigated the efficacy of the procedure in pediatric patients with FF utilizing other metrics than the PROMIS system to measure pain specifically. Akimau and Flowers 1 found significant improvement in pain after CLO in pediatric patients with FF using the VAS (visual analog scale) system with a mean follow-up of 4.5 years in 12 pediatric patients (20 feet). Additionally, Sterian and Ulici investigated the efficacy of CLO in pain alleviation for FF using the Wong-Baker Pain Scale. 30 Their study analyzed 21 procedures in pediatric patients and found significantly alleviated pain at the 12-month follow-up by comparing pain scores before and after surgery. 30
In addition to pain, specific investigation of mobility improvement after CLO for painful FF has been studied to a lesser degree. De Luna et al 5 explored the ability of CLO to improve mobility in 14 pediatric patients (26 feet) with painful FF using the Foot and Ankle Disability Index (FADI) scoring system, which examines mobility by asking patients to rate their ability to walk, squat, ascend/descend stairs, engage in recreational activities, and perform daily activities at home. Their analysis found a statistically significant improvement in mean Foot and Ankle Disability Index scores after CLO was performed, indicating an improvement in mobility as a result of the procedure. 5
Although pain and mobility have each been individually explored as an outcome of CLO for symptomatic FF, several studies have investigated the efficacy of the procedure by using scoring systems that take both pain and mobility into account. One such metric is the American Orthopaedic Foot & Ankle Society (AOFAS) scoring system. De Luna et al 5 found a statistically significant AOFAS score improvement following CLO in their study in addition to Foot and Ankle Disability Index scores as described above, with their 14 patients on average reporting good outcomes (AOFAS scores > 90). Viegas 35 explored AOFAS scoring after CLO for pediatric painful FF as well in 17 patients (34 feet) and found that on average, patients experienced fair results at a 3-month follow-up (AOFAS score 80-90), with further improvement to good results by the final follow-up (AOFAS scores > 90). In a study of 15 pediatric patients (20 feet) with painful FF, Nejib and Delpont 24 found 13 patients experienced good outcomes (AOFAS scores > 90) after CLO with a mean follow up of 8.3 years. Importantly, they noted 7 patients experienced residual pain after the procedure, highlighting the possibility that further conservative management or potentially additional surgical intervention may be necessary after CLO for optimal management of the deformity.
In a more recent study, DeFrancesco et al 6 assessed the radiographic alignment and PROs of flatfoot reconstruction following CLO, alongside additional procedures including medial side soft tissue procedures, medial cuneiform plantar flexion osteotomy, and medializing calcaneal osteotomy. Once utilizing PROMIS score data, DeFrancesco et al found 75% patients (18/24) achieved the minimally clinically important difference estimated at 3 for the pediatric pain interference domain.6,33 Radiographically, they found statistically significant improvement in all structural measurements including AP/lateral talus–first metatarsal angle, talonavicular uncoverage, incongruency angle, MC-5MH, and hindfoot moment arm (P < .0001). 6 In similar fashion, our work demonstrated statistically significant improvement in all radiographic parameters. Such findings indicate radiographic improvement in those undergoing CLO for FF, specifically improving forefoot adduction, talar head coverage, and arch height.
Using PROMIS scores, we found significant improvement in pain and mobility after CLO in children with symptomatic flatfeet. Four patients (19%) in our study reported residual pain (PROMIS score > 55) at the final follow-up, which indicates that although CLO improves the pain associated with flexible flatfeet, residual pain can be seen in a moderate percentage of the patients. Although the calcaneal lengthening osteotomy is a relatively safe procedure and has been associated with generally positive clinical outcomes in a series of studies, it is not without complications and potential negative outcomes. Several studies have previously sourced residual pain following CLO secondary to hindfoot valgus, nerve palsies, malunion, nonunion, calcaneocuboid subluxation, and calcaneonavicular subluxation.6,9,10,23,25
A systematic review conducted by Lima and Volpon analyzed 8 studies and found residual pain in 17.2% of the patients. 17 Our findings agree with this study by demonstrating that residual pain may be present after the procedure in a small group of patients. We did not find any effect of severity of preoperative or postoperative deformity or BMI on the presence or absence of postoperative pain. We found that the group with residual postoperative pain tended to have more pain before surgery, although the difference did not reach statistical significance in our study. Radiographically, our study also demonstrated no statistical significance in both preoperative and postoperative measurements. Furthermore, we found that 3 of the 5 feet had residual pain closer to the 6-month follow-up period. Given their limited follow-up time, persistent pain may be accounted by not entirely reaching the recovery potential for the full range of motion and activity. This is similar to the findings of other studies in orthopaedic literature demonstrating the amount of preoperative pain as a factor in predicting postoperative pain.27,31 Consequently, more research is needed to understand the risk factors for complications including residual pain after surgery for idiopathic flatfeet.
With increasing use of PROMIS scores in orthopaedics, we report the first study using PROMIS scores in treatment of children with symptomatic flatfoot deformity. Important limitations to consider include retrospective design, limited sample size, single institution focus, and discrepancy of time points when PROMIS scores were recorded for each patient. Additionally, our postoperative follow-up period ranged from 6 to 12 months, meaning our outcomes would fall within the early postoperative period and subsequently do not entirely represent long-term outcomes of symptomatic FF managed with CLO.
Conclusion
We found clinically and statistically significant improvement in patient-reported outcomes for both mobility and pain after CLO for painful flexible flatfeet in pediatric patients. Ultimately, these results suggest that CLO can improve pain and mobility in children presenting with symptomatic flexible flatfeet. Future studies may benefit from incorporating PROMIS scores when examining the outcomes of CLO in nonidiopathic flatfoot deformities, as well as in evaluating other procedures used in the treatment of other foot deformities in children.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251318733 – Supplemental material for Early Patient-Reported Outcomes Following Calcaneal Lengthening Osteotomy for Symptomatic Flexible Flatfoot
Supplemental material, sj-pdf-1-fao-10.1177_24730114251318733 for Early Patient-Reported Outcomes Following Calcaneal Lengthening Osteotomy for Symptomatic Flexible Flatfoot by Rohit Siddabattula, Matthew William, Daniel E. Pereira, Jason L. Cummings and Pooya Hosseinzadeh in Foot & Ankle Orthopaedics
Footnotes
Appendix
Patient Demographics and Procedure Characteristics.

| Characteristic | Value |
|---|---|
| Age, y, median (minimum-maximum) | 12 (9-15) |
| Gender | |
| Male,, n (%) | 11 (52.38) |
| Female, n (%) | 10 (47.62) |
| Race, n (%) | |
| White | 15 (71.43) |
| Black or African American | 5 (23.81) |
| American Indian/Alaska Native | 1 (4.76) |
| Height, cm, median (minimum-maximum) | 158 (138-183) |
| Weight, kg, median (minimum-maximum) | 52 (32-109) |
| Weight > 50 kg, n (%) | 11 (52.38) |
| Patients with a unilateral calcaneal lengthening osteotomy, n (%) | 11 (52.38) |
| Patients with a bilateral calcaneal lengthening osteotomy, n (%) | 10 (47.62) |
Ethical Approval
Ethical approval for this study was obtained from the Washington University in St. Louis Institutional Review Board (ID: 202010235).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
