Abstract
Background:
Ankle fractures are a common injury treated by orthopaedic surgeons. Unstable, displaced ankle fractures are often fixed with open reduction internal fixation (ORIF) using different implant constructs at various cost. No study to date has looked at transparency in ankle implant costs to surgeon behavior. Our surgeons self-identified that the biggest barrier for lowering implant cost was the lack of cost transparency. This was a surgeon-led-study to evaluate whether increased transparency in implant costs affected surgeon behavior.
Methods:
Monthly operative logs from December 2021 to September 2022 were reviewed at our level 1 trauma center for operative fixation of ankle fractures. The cost data of each fixation construct was reported to trauma-trained surgeons at the end of each month from March 2022 to June 2022. Average costs of implants were compared before and after education. A linear mixed model was used to explore what factors were associated with changes in costs. Surgeons also participated in a poststudy survey.
Results:
The implant costs of 110 ankle fracture fixations were reviewed over the period before education (n = 60), during education (n = 30), and after education (n = 20). The mean implant cost difference for unimalleolar fractures was −$204.80 (P = .68), whereas the mean cost difference for bimalleolar fractures was −$9.82 (P = .98). Trimalleolar fractures had a mean cost difference of +$94.47 (P = .84). Linear mixed model demonstrated fracture pattern as the only factor significantly associated with implant costs (P < .01). Post-education surgeon survey revealed that 6 of 7 surgeons felt that monthly updates affected their implant selection. However, only 2 surgeons demonstrated a change in practice with decreased implant costs during the study.
Conclusion:
The majority of surgeons self-reported being influenced by the implant cost education, but the detected change in implant cost was only observed in less than one-third of surgeons. Our results suggest implant selection and related costs are not influenced by increased cost transparency education alone.
Level of Evidence:
Level III, case control study.
Introduction
Ankle fractures account for 9% of the fractures in the world, making them a common fracture orthopaedic surgeons see in practice. 4 Open reduction internal fixation (ORIF) of unstable, displaced ankle fractures remains the standard mode of treatment, with approximately 25% of ankle fractures requiring surgical care.4,12 There are many different types of implants used by orthopaedic surgeons to fix ankle fractures, which vary in cost. 2 Even for similar fracture patterns, surgeon choice can account for nearly a 3.5-fold difference between the lowest and highest cost surgeons. 2 Studies have shown the costs of orthopaedic implants account for a large portion of spending during orthopaedic procedures, even accounting for up to 87% of the cost. 10 In fact, direct costs of ankle fractures can cost patients and the health care system up to $19,555 per patient. 3 Surgeons therefore directly influence the costs for patients by the implants they choose. 6 With the rising costs of health care in the United States, physicians are being held accountable for decreasing cost spending. 9 However, surgeons are often not provided the cost of implants and incorrectly underestimate the cost of a variety of different implants, which may limit their ability to reduce spending.7,11
At our own site, surgeons agreed that lack of information on implant cost was the main barrier to enacting change. To date, there is no known study that examines the transparency of ankle implant cost to surgeons and how this affects their implant choice behavior. Thus, we designed an observational study that allowed surgeons to review the costs of their utilized ankle implants monthly to determine if increased cost transparency resulted in a change in practice. Our hypothesis was that increased transparency would change surgeon behavior regarding ankle implant selection and lead to a decrease in implant costs.
Methods
Institutional review board (IRB) approval was obtained for this observational study. Eight hospital-employed trauma-trained orthopaedic surgeons, one of whom was foot and ankle trained, at our level 1 trauma center were informed of participation in this study and informed of the costs of common ankle implants prior to the start of the study. From March 2022 to June 2022, each orthopaedic surgeon was informed of their average ankle implant cost, as well as a breakdown of the price of each implant they used, for each patient who underwent ORIF of ankle fractures (Current Procedural Terminology codes 27766, 27769, 27792, 27814, 27822, and 27823). We did not include syndesmotic injuries because our surgeons, as well as others, make syndesmotic implant choice based on multiple factors other than cost alone.
Cost was calculated using implant information and their associated cost from our internal implant data base. Our health care institution has an implant contract that dictates 90% of our implants used must be made by Synthes, with the other 10% made by Stryker, Zimmer, and Smith and Nephew. We did not include drill bits, used-not implanted, wasted implants, or implants used for syndesmotic fixation in our total cost per patient. This was presented to them in a bar graph and table format at the monthly department meeting. The surgeons were provided with their individual cases, as well as the cases of their peers. Electronic medical records were reviewed for demographic information and fracture pattern (unimalleolar vs bimalleolar vs trimalleolar ankle fracture).
Chart review was then performed for patients who underwent ORIF of ankle fractures between December 2022 and February 2022 for cost analysis before the cost education intervention and July 2022 to September 2022 for cost analysis after the education intervention. We wanted to evaluate if there was a change in surgeon behavior, would that change be sustained after the intervention was completed. Demographic information, fracture pattern, implant information, and their associated cost from our internal implant database were gathered. Again, drill bits, used-not implanted, wasted implants, or implants used to fix syndesmotic injuries were not included in the total cost per patient.
Study data were assembled and maintained on Microsoft Excel on a secure hospital server (Microsoft Corporation, Redmond, WA). Means, frequencies, and percentages were calculated for patient demographics and fracture patterns within our population study. Cases from December 2022 to March 2022 were compared to those in July 2022 to September 2022 for direct analysis of before and after the cost education intervention.
A linear mixed model was utilized to determine factors associated with cost (SAS 9.4) (SAS Institute, Cary, NC). The factors included in the model were association (before and after education), fracture pattern (unimalleolar, bimalleolar, trimalleolar), the interaction of association and fracture pattern, provider, and the interaction of provider and fracture pattern. It also included the following patient characteristics; age, body mass index (BMI), gender, diabetes, current smoking status, osteoporosis, and American Society of Anesthesiologists Classification (ASA). Finally, we included month to adjust for any changes in cost simply associated with inflation over time. For regression analysis, cases from December 2022 to March 2022 were included in the before cost education category and cases from April 2022 to September 2022 were included in the after-education period because of surgeons being aware of costs during these times. Two providers were excluded from the analysis because they did not have at least 1 of each level of the same fracture pattern in the before and after education periods. Statistical significance was set at a P value of <.05.
At the end of the education period, participating surgeons completed a survey on Qualtrics (Qualtrics Company, Seattle, WA). They were asked to rank their agreement with various statements concerning how they believed monthly cost updates changed their ankle fracture implant selection, their understanding of the cost of different implants after monthly updates, and how various factors influenced their ankle implant choice.
Results
The implant costs of 110 ankle fractures’ surgical fixations were reviewed and included in this study. Sixty cases occurred before the cost education, 30 cases occurred during the cost education, and 20 cases occurred after cost education. The before and after cost education groups were similar in age, gender distribution, fracture pattern, BMI, diabetes, smoking status, osteoporosis status, and ASA classification (Table 1). More severe fracture pattern (trimalleolar > bimalleolar > unimalleolar) was found to be associated with higher implant cost, whereas other factors such as age, gender, diabetes, smoking status, osteoporosis, ASA status, surgeon, or the month of surgery were found to not be statistically associated with cost (Table 2).
Patient Demographics. a

Abbreviations: ASA, American Society of Anesthesiologists; BMI, body mass index.
Unless otherwise noted, values are n (%).
Linear Mixed Model Association. a
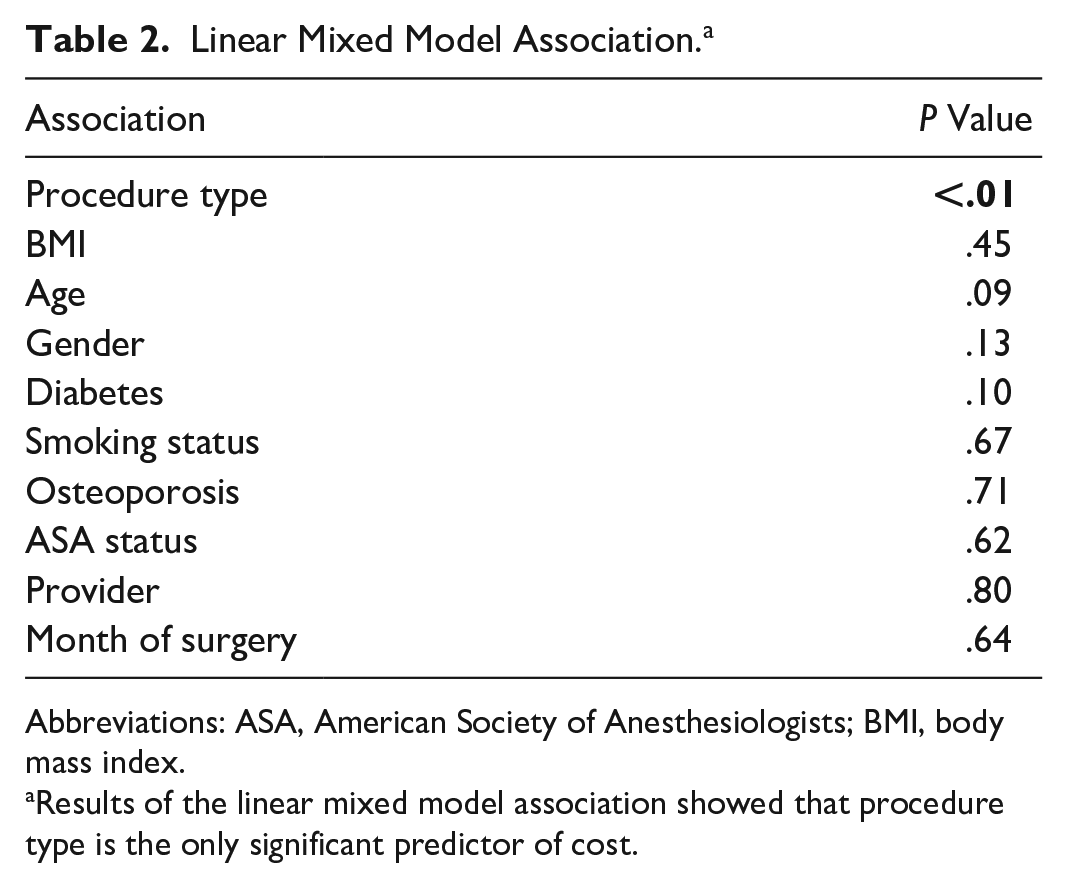
Abbreviations: ASA, American Society of Anesthesiologists; BMI, body mass index.
Results of the linear mixed model association showed that procedure type is the only significant predictor of cost.
The average total implant cost before cost education was provided was $746.20, whereas the average total implant cost after education was $724.70 (P = .48). The average implant cost was similar between the pre- and posteducation with regard to fracture pattern (Table 3). We did not find a statistically significant difference between total implant cost before and after education for all fracture patterns. We also analyzed those cases strictly before and after the education period, and all fracture patterns were not statistically different (P < .05).
Linear Mixed Model Analysis of the Average Difference in Cost Associated With Fracture Pattern Type Before and After Education. a

No statistical significance was found to be associated with education and fracture pattern type with regard to cost.
At the end of the education period, surgeons self-reported what they believed the impacts of cost reports were on their implant choice. Most surgeons (6 of 7) reported that cost reports did impact their implant decision to some level (Figure 1). In particular, 2 surgeons strongly agreed that the monthly cost updates changed their ankle fracture implant selection, whereas 4 somewhat agreed and 1 strongly disagreed. Three surgeons strongly agreed they had a better understanding of what the costs of different implants were after the monthly updates, whereas 3 somewhat agreed and 1 somewhat disagreed. When asked to rank how certain factors would impact their practice toward being more cost conscious, 6 of 7 surgeons ranked fracture characteristics as the most important factor, whereas 3 of 7 surgeons ranked cost as the third most important factor. The 2 surgeons who strongly agreed that the monthly cost education changed their practice demonstrated a decrease in cost for both unimalleolar and bimalleolar fractures after education and 1 of the 2 had a decrease across all fracture patterns (Figure 2). No other surgeons showed a significant difference in implant costs, despite most reporting that this new cost knowledge had affected their decision making.

Factors impacting implant choice ranked by surgeons from most important to least important.

Average cost of the 2 surgeons who indicated on their survey that the monthly cost education changed their practice. Both had decreases in their average cost for unimalleolar and bimalleolar after cost education. One of the 2 showed a decrease in cost for trimalleolar fractures after cost education.
Discussion
Even though participating surgeons identified the lack of cost transparency as the number 1 barrier to reducing implant cost prior to the study, we found that resolving the barrier did not lead to a statistically significant lowering of implant costs overall. Informing orthopaedic surgeons on their implant cost for each ORIF of ankle fractures did not change their behavior in deciding on implants to use. Only 2 of 7 surgeons decreased their implant cost from before to after education in both unimalleolar and bimalleolar cases, with only 1 of the 2 also decreasing their cost in trimalleolar cases. Previous studies using more complicated cost ranking systems have demonstrated effectiveness toward minimizing implant costs in other trauma implants8,13 whereas others found implant cost was not an important factor. 1 Our study is the first to evaluate whether increasing the transparency of ankle fracture implant costs change surgeon behavior.
We explored important factors affecting a surgeon’s ankle fracture implant choice. Through surveys, surgeons identified that fracture characteristics, including fracture pattern, was the most important factor in selecting implants. Analysis of our data showed that fracture pattern did affect implant cost, with trimalleolar fractures being the most expensive. This is consistent with results found by Okelana et al 6 in their study examining factors affecting cost.
Patient factors, such as age, bone density, and medical history, were also deemed important for surgeons to consider when deciding which implants to use during ankle fracture fixation. However, these factors were not found to be associated with cost in our linear mixed model. Our data analysis is consistent with evidence found by Kibble et al, 5 who did not find osteoporosis and age did not affect the cost of implants.
Factors that influence surgeons’ implant choice are numerous and complex, with cost demonstrated not to be a main driver in our study. It is worth noting that the surgeons are health system employed and do not have any direct financial benefit from lowering implant cost. The compensation model at our academic institution is productivity based on the number of RVUs generated. Hence, the cost of implants does not factor directly into their salary. Perhaps an incentivized program providing surgeons or their department with some benefits for choosing lower-cost implants would provide a greater decrease in implant cost than what our study observed.
Our study has limitations. The authors acknowledge the limited data size in this study and certain fracture pattern outliers could skew our results. Not all surgeons saw a uniform number of ankle fractures. This could have affected our overall cost data as each surgeon had a different average implant cost for each fracture type. Our study only included patients from a single health care system, which may impact the exact cost of implants. This might not be applicable to other health care institutions around the world. Despite this, our study included consistent prices for ankle fracture implants over the duration of the study. Prices remained the same and allowed us to accurately measure the change in the mean costs of ankle implants. In addition, the same surgeons participated for the duration of our study, allowing for continuity in ankle fracture treatment.
Costs of health care in the United States continues to rise and practitioners are being held accountable to help mitigate direct patient and health care costs. 9 Kibble et al 5 showed significant variability in ankle implant cost, with no correlation between higher cost implants and better patient outcomes. Orthopaedic surgeons have a unique opportunity to help decrease health care cost by lowering implant costs. The process of choosing implants is a complex pathway that we do not fully understand and, as yet, there is no clear direct benefit of cost savings for surgeons and patients. Our study did not find a significant difference in the mean costs of ORIF of ankle implants before and after increased transparency in cost, despite surgeons reporting this as the number 1 barrier to decreasing implant costs. We did find that a patient’s fracture pattern can influence the cost of the implant construct, but this is beyond a surgeons’ control. With no significant association between patient outcomes and ankle implant costs, 5 further study is warranted to identify what influences surgeon behavior and how strategies can assist orthopaedic surgeons in lower implant costs.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114241247826 – Supplemental material for Does Transparency of Ankle Implant Costs Influence Surgeon Behavior?
Supplemental material, sj-pdf-1-fao-10.1177_24730114241247826 for Does Transparency of Ankle Implant Costs Influence Surgeon Behavior? by Riley Swenson, Thomas Paull, Gaonhia Moua, David Weatherby, Khalid Azzam, Robert Wojahn, Sarah Anderson, Peter A. Cole and Mai Nguyen in Foot & Ankle Orthopaedics
Footnotes
Ethical Approval
Ethical approval for this study was waived by Regions Hospital Institutional Review Board due to the quality improvement nature of the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
