Abstract
Background:
Austere fracture immobilization equipment and techniques are often overlooked, with few studies critically evaluating the process. The purpose of this study was to evaluate current austere splinting techniques and equipment used for lower extremity fractures while field testing a new 1-step spray-on foam splint.
Methods:
This is a prospective analysis of austere splinting techniques. A cadaveric model with a distal third tibia-fibula fracture was used for testing. The specimens were placed in an austere environment and participants immobilized the injury with standard equipment (structural aluminum malleable [SAM] splint, 6-in. ACE wrap) while being critically evaluated. The specimens were also immobilized with a 1-step in-situ foam splint.
Results:
Twenty-one military Special Operations medical personnel participated. Each participant was observed and scored by a single orthopedic foot and ankle surgeon using a Likert scale based on 10 splinting criteria. Standard splinting resulted in an average score of 32.2 (range, 5-50), with significant deficiencies in fracture traction (1/5), fracture motion (2.9/5), protection of neurovascular structures (3/5), and soft tissue manipulation (3/5). The average time to completion was 203 seconds, with 1 splint failure. The spray-on foam splinting technique yielded a significantly higher score of 48.5 while completing the task significantly faster (68 seconds), with no failures.
Conclusion:
Special Operations medical personnel demonstrated success in immobilizing a complex fracture with standard techniques in a cadaveric model. However, testing demonstrated the inherent inability of the SAM splint to provide longitudinal traction while simultaneously allowing excessive fracture motion and potential injury to the soft tissues. In comparison, our spray-on foam proof of concept technique eliminated motion by allowing an in situ application with adequate rigidity.
Clinical Relevance:
This experiment included a likert scale to critically evaluate splinting techniques and equipment. It reliably tested standard splinting equipment and a 1-step in-situ foam splint for distal third tibia-fibula fractures.
Introduction
Splinting and immobilization of fractures and musculoskeletal injuries is a relatively simple technique with few improvements throughout time. It is well known that reducing a fracture and restoring anatomic position improves pain, reduces blood loss, and preserves soft tissue structures. 2,7,8,12 The entire extremity and associated injuries must be considered while selecting splinting materials and techniques. The splint must be strong enough to realign the limb and hold it in place while also preserving the associated soft tissues. Applying the splint must also be easily understood as immobilization is typically performed by personnel with variable medical training, unaware of the clinical consequences when in a pre-hospital and austere environment.
Currently, musculoskeletal extremity injuries have been on the rise, approaching 50% of all combat-related injuries secondary to body-armor and mine-resistant vehicles improving battlefield survivability. 1 As the number of extremity injuries increases, very little recent progress has been made in the advancement of initial austere treatment. In World War I, the implementation of the Thomas leg splint reduced mortality in military femur fractures from 80% to 10%. 3 Following his experiences in the Vietnam War, Dr Sam Scheinberg developed the structural aluminum malleable (SAM) splint, a lightweight multipurpose immobilization device. The simplicity and versatility of the SAM splint has led to it becoming the standard for military providers worldwide. The SAM splint, although widely used, has very little published evidence documenting its success, failures, and best methods of application. The United States Special Operations Community (USSOCOM) and countless other organizations have published technique guides and recommendations based on anecdotal principles and soldier ingenuity. 13 The same anecdotal principles have guided splinting indications and application techniques as relevant scientific evidence is lacking. As technologies improve, our techniques and instructions should be critically evaluated and sequentially validated to ensure optimal care is being rendered. Recently the US Army Medical Research and Material Command has patented a novel 1-step spray-on foam splint (Fast Cast) that has shown great promise but lacks validation and requires further proof-of-concept testing. 5
The purpose of the current study was to prospectively evaluate the application technique and capabilities of the SAM splint to immobilize a distal third tibia-fibula fracture in a cadaveric model, as performed by experienced Special Operations providers in an austere environment. We also wanted to establish the utility of a new proof-of-concept 1-step spray-on foam splint.
Materials and Methods
This study was a prospective cohort of 21 United States Special Operations medical personnel immobilizing a distal third tibia-fibula in an austere environment. The testing was performed on a single training day at a single center under the same austere conditions. All evaluations were performed by the senior author, a fellowship-trained orthopedic foot and ankle surgeon. All medical personnel were certified and credentialed by their respective governing bodies according to training level. Training levels ranged from Special Operations Medics (18D and 68WW1), physician assistants with prior 18D or pararescue (PJ) training, and emergency medicine physicians with varying operational medical backgrounds and 1 orthopedic surgeon with prior medic training. Each provider had completed provider-specific military medicine training for austere environments. All but one provider had deployed to an active combat zone as a medical provider (Table 1).
Subject Demographic Data.a

a All subjects tested were members of the United States Joint Special Operations Command, Joint Medical Augmentation Unit. Medics had completed either 18D or 68WW1 training. Physician assistants have a master’s degree equivalent education and all had prior medic backgrounds. Emergency medicine physicians and the orthopedic surgeon had completed an ACGME-accredited residency and were board certified.
Twenty subjects were evaluated on SAM splint application in an austere environment. One subject was evaluated twice using the Fast Cast spray-on foam splint. The study group of military medical personnel consisted of 21 males and no females. The group was composed of 11 medics, 4 physician assistants, 5 emergency medicine physicians, and 1 orthopedic surgeon. The subjects had, on average, 7.7 years of experience in their respective positions and an astounding average of 25.4 months deployed into various combat zones throughout the world. A summary of the demographic information for the study sample is presented in Table 1.
Testing
The providers were briefed on the injury pattern and the solo task of immobilizing the fracture expeditiously and safely in order to allow for medivac. The subjects knew they were being evaluated and timed, but the individual testing parameters and time implications were not provided. An adult full-body cadaveric model with a distal one-third tibia-fibula fracture was used for all testing. The fracture pattern was created using blunt impaction while preserving the skin and soft tissue envelope. The fracture was initiated approximately 10 cm from the joint line with a similar fracture of the fibula at the same level. This fracture pattern was selected because of its inherent instability, reproducibility, and the well-known catastrophic complications associated with the soft tissues. 9 The model was then placed in an austere urban environment with no external equipment and no extrication needed. During testing, no assistance, coaching, or feedback was provided to the subjects. No restrictions were placed on the splinting technique within the constraints of the environment and provided equipment.
SAM Splint Immobilization
At the onset of testing, each provider was issued 2 standard SAM splints and 2 standard 6-inch ACE wraps. The subjects were required to manipulate and mold the SAM splint according to their preferred method of application. After the subject felt they had completed the task well enough to allow for evacuation, time was stopped. During the application, the senior author observed and scored the subjects on 10 predetermined splinting characteristics using a 5-point Likert-type scale (Figure 1). After completion of the task, the immobilized leg was held suspended by the knee/thigh in a horizontal position for 30 seconds. If the splint maintained its posture and continuity, it was considered a success; if intrinsic stability was lost, it was considered a failure.

Austere splint immobilization, technical evaluation score sheet.
Spray-On Foam Splint
The same cadaveric model and testing environment was used for both splinting methods. The spray-on foam consisted of 2 components, one being a liquid polyol alcohol and a second isocyanate propellant. The 2 chemicals react, creating an open-cell rigid foam that contours to the surface on which it is applied. The foam has a modest (non–injury producing) exothermic reaction that then forms into a solid state in less than 60 seconds. 5 The foam mildly adheres to dry or tacky skin/clothing but has not been found to adhere to moist or bloody soft tissue secondary to the hydrophobic nature of the foam. Because of the limited availability of the foam kits, only 2 models were able to be tested and evaluated (Figure 2). The testing scenario was the same, except the spray mechanism (spray-gun and hose) was pre-assembled before testing. The pre-assembly was allowed to mitigate confounding factors and to create a uniform testing environment, as the SAM splint and ACE wraps were also unpackaged.

Demonstration of the spray-on foam splint. Demonstration only and not involved in the study due to security.
Statistical Analysis
Standard descriptive statistics were calculated for all variables of interest. Mathematical means and standard deviations were calculated for continuous variables when the data were normally distributed. If continuous data were not normally distributed or in ordinal nature, then medians and interquartile ranges were calculated.
Results
Our subjects were able to demonstrate an overall success rate of 95% with only 1 failure while placing a SAM splint in an austere environment as determined by the 30-second hang test. Further investigation of individual tasks per our predetermined criteria for splint application demonstrated a mean failing score of 32.2 (range 5-50), a score of 35 or greater was required for success. Uniformly the SAM splint failed to maintain fracture traction (reduction), significantly impacting overall scores. Other significant failures were fracture motion (2.9/5), protection of neurovascular structures (3/5), and soft tissue manipulation (3/5). The time to completion was, on average, 203 seconds (range, 102-301). A summary of the results is presented in Table 2. Performing the task completely unassisted in an austere environment as well as the limitations of the SAM splint must be considered when assessing the total score for the splinting cohort.
Mean Scores for the Providers on the Technical Evaluation Score Sheet.
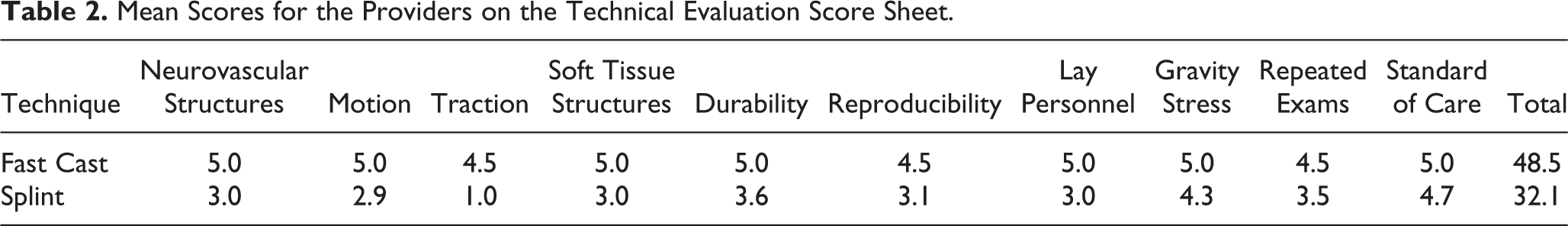
The Fast Cast spray-on foam splint was limited to 2 evaluations on separate cadaveric models as a proof of concept. The Fast Cast demonstrated 2 successful 30-second hang tests with a 100% pass rate. Upon investigation of individual parameters, the spray-on foam demonstrated a mean passing score of 48.5, significantly better than the SAM splint. The spray-on foam also demonstrated significantly shorter time to completion with a mean of 68 seconds compared to 203 seconds reported for the SAM splint. The “reduction-in-situ” application technique avoided picking the extremity up, molding the splinting material and circumferentially wrapping. The unique adherence to the skin, as in Bucks traction, 11 demonstrated sustained traction preventing shortening, thus maintaining the reduction during application and the horizontal test.
Discussion
Our study is the first of its kind to validate the success of US Special Operations medical personnel independently immobilizing a complex extremity fracture with a SAM splint as well as field testing our new 1-step spray-on foam technique. The current results demonstrate the SAM splint’s inherent inability to provide longitudinal traction while allowing for excessive fracture site motion during application. The newly developed spray-on foam proof of concept technique eliminated motion and provided traction by allowing in situ reduction application with adequate rigidity.
The application of a properly placed splint is essential in the management of lower extremity fractures. Periosteum and venous bleeding during a fracture can contribute to blood loss that fills a potential space caused by the fracture displacement. A tibia fracture can be associated with as much as 500 to 1000 mL of blood loss within the soft tissue envelope. 4 This amount of blood loss can combine with other associated injuries and potentiate hypovolemic shock. The application of traction across a fracture site reduces the deformity and the potential space in which blood accumulates. Anatomic position and splinting also reduce muscles spasms and contractures, which lead to further displacement and bayonetting of the fracture ends. 7,10,12 Because of its simplicity and effectiveness, traction remains a pillar of fracture management. In the current study, none of our experts was able to establish nor maintain traction across the fracture site (1/5), simultaneously allowing excessive fracture manipulation (2.9/5) while using the SAM splint. In contrast, our spray-on foam splint was able to maintain traction and alignment secondary to its total contact application, prohibiting shortening. The mild adherent of the foam to the skin also serves much like Bucks traction without the need for ropes and pullies. 11
Outside of fracture management, the soft tissues must be considered when evaluating a splinting mechanism. The SAM splint has inherent limitations secondary to its malleability and intended multipurpose use construct. The technician applying the splint must estimate the shape and contour the splint before application vs direct pressure molding after application. Both techniques were used by our experts depending on training preference, but they struggled to maintain control and position of the distal segment with a mean score of 3/5. Our observations also point out that maintaining the reduction and managing the splint while simultaneously circumferentially applying the ACE wrap was of notable concern, scoring 3/5 in protection of neurovascular structures and 3/5 in soft tissue manipulation. The extent of potential injury from excessive soft tissue manipulation is difficult to estimate, but with a high association of compartment syndrome and neurovascular injury, reduction of motion is paramount. 6 The spray foam application technique allowed the technician to reduce the deformity, and hold alignment with one hand while applying the foam in situ. The reduction in situ application technique avoided picking the extremity up, molding the splinting material and circumferentially wrapping, thus scoring 5/5 for protection and manipulation. The reduction in situ foaming technique also inherently prevents foam application along the ground or undersurface, preventing circumferential constriction potentiating injury. As with all austere treatments, the SAM splint and spray-foam are intended only for temporizing the injury and transportation to the next higher level of care. A definitive time of use has not been determined and would be highly variable depending on transport times and additional resources.
The strengths of our study include using a standardized control group applying the SAM splint as the gold standard method. We also used a single fellowship-trained orthopedic foot and ankle surgeon for all evaluations using predefined testing parameters that the subjects were blinded to, mitigating altered testing behavior. Our simulated austere battlefield environment provided high-fidelity testing, whereas using a full body cadaveric model greatly increased the overall face validity. The current study does have limitations, including selection bias. Our subjects were a homogenous group of very experienced providers, which may not apply to basic or lay providers. We were also limited to the reproducibility of 2 cadaveric models that had to be reused for multiple providers. Our cadaveric model had no muscular tone contributing to the deforming forces, potentially making splint application less difficult. Multiple rounds were not used because it was not feasible in an austere environment and we felt that using 1 evaluator would keep a more consistent scoring pattern limiting the variability. The subjects were also aware they were being timed, which may have compromised their attention to protecting the soft tissues and fracture reduction. We understand that time to completion is not a measure indicating success or failure, but because it does impact true battlefield evacuation movements, time was also used to draw a contrast between the 2 methods. The proof of concept spray-on foam was of limited quantity, allowing for only 2 evaluations, which limited statistical power analysis. The foam was also only tested at approximately 70°F, thus limiting evaluation of the foam in more extreme conditions.
Conclusion
Our results demonstrate the success of Special Operations medical personnel to individually immobilize a complex extremity fracture with a SAM splint in an austere environment. The results also highlight the failures in standardized training emphasizing the end product but neglecting the critical steps of immobilization. With the given results, educators can improve training and training models, allowing providers to better appreciate extremity instability and the vulnerability of the soft tissue envelope. Further study is needed to compare which method of molding the SAM splint is mechanically advantageous while providing appropriate immobilization in a timely manner. The 10-point testing criteria may also serve as a training aid but will need further validation in practical applications. In conclusion, the SAM splint was an appropriate immobilization aid. However, further research and development of newer technologies, such as the Fast Cast spray-on foam splint are needed to address traction and fracture reduction within the austere environment.
Supplemental Material
Supplemental Material, FAO916144-ICMJE - Prospective Study of Military Special Operations Medical Personnel and Lower Extremity Fracture Immobilization in an Austere Environment
Supplemental Material, FAO916144-ICMJE for Prospective Study of Military Special Operations Medical Personnel and Lower Extremity Fracture Immobilization in an Austere Environment by LTC Kevin D. Martin, 2LT Trevor J. Mcbride, CPT Alicia Unangst and Jaime Chisholm in Foot & Ankle Orthopaedics
Footnotes
Author Note
Some authors are employees of the US Federal Government and the United States Army. The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or reflecting the views of the Department of Defense or United States government.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: ICMJE forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
