Abstract
Background:
The objective of this study was to define the volume (mLs) needed for a positive saline load challenge test in anterolateral (AL), anteromedial (AM), posterolateral (PL), or posteromedial (PM) ankle arthrotomy wounds using normal saline (NS) and methylene blue (MB). Another objective was to evaluate the use of fluoroscopy and iodinated contrast in the diagnosis of ankle arthrotomies.
Methods:
Four cadaveric ankle specimens underwent standardized arthrotomy creation in either the AL, AM, PL, or PM portion of each specimen. An 18-gauge needle was used to inject fluid into each ankle, and the volumes needed for positive fluid challenges were recorded. All 4 ankles were tested 10 times (n = 40) with NS and 10 times using MB (n = 40). A fifth cadaveric ankle was injected with radiopaque contrast solution, and an arthrotomy was simulated and imaged with fluoroscopy.Statistical analyses compared the volumes of NS and MB needed for a positive test. In addition, the 25th, 50th, 75th, 90th, and 95th percentiles of volumes needed for a positive test was calculated.
Results:
The volume of fluid necessary to detect 25%, 50%, 75%, 90%, and 95% of ankle arthrotomies from any site was 2.0 mL, 4.5 mL, 9.0 mL, 10 mL, and 10 mL, respectively. Anterior arthrotomies required less fluid (2.1 mL ± 0.5) than posterior arthrotomies (9.0 mL ± 1.2) for a positive test (P < .0001). There was no difference between the amount of NS (5.5 mL ± 3.6) vs MB (5.6 mL ± 3.7) needed for a positive challenge test (P = .739).
Conclusion:
Ninety-five percent of ankle arthrotomies could be diagnosed with 10 mL of injected fluid; there was no difference between the volume of NS vs MB needed. Fluoroscopy assisted with needle placement and can be combined with radiopaque contrast solution to diagnose ankle arthrotomies.
Clinical Relevance:
The findings of this study may improve sensitivity and efficiency in the diagnosis of traumatic ankle arthrotomies, for which there is currently a paucity of literature.
Introduction
Traumatic arthrotomies represent orthopedic emergencies that must be quickly diagnosed and properly managed in order to avoid devastating complications such as septic arthritis. 3,10 One of the most important aspects of treatment is the prompt and accurate confirmation of capsular disruption. Although the gold standard for diagnosing traumatic arthrotomy is intraoperative inspection, operative exploration is costly, timely, and not without risk to the patient. 3
Currently, there is an abundance of literature regarding the diagnostic accuracy of the saline load challenge test (SLT) and computed tomography (CT) with regard to arthrotomies of larger joints such as the knee, 6 -9 but there is very little clinical research and no published cadaveric studies examining the role of the SLT with regard to diagnosing ankle arthrotomies. Unlike the knee, there are also no studies that examine the role of CT scans in the diagnoses of traumatic ankle arthrotomies, which limits the diagnostic tools available to physicians who are presented with potential ankle arthrotomies. 7 Furthermore, the current literature on traumatic ankle arthrotomy diagnosis using SLT has been generated using an arthroscopy model, which is inherently limited because these studies only evaluate one location for the site of the simulated traumatic arthrotomy—either the anteromedial or anterolateral arthroscopic portal sites. 1,2 The authors of this study sought to evaluate the diagnosis of ankle arthrotomies with the SLT using cadaveric models that more appropriately represent the heterogeneity in traumatic wound distribution around the ankle joint with simulated anterolateral (AL), anteromedial (AM), posterolateral (PL), and posteromedial (PM) ankle arthrotomy wounds. Additionally, we wanted to evaluate the addition of methylene blue as an adjunct to the SLT to determine whether or not this would increase the diagnostic accuracy of the test and also require a smaller volume of injected fluid for diagnosis. The addition of methylene blue to the SLT has previously been studied using a knee arthrotomy model, but until this study, had not yet been evaluated in the context of an arthrotomy of the ankle. 8 Lastly, the authors sought to evaluate whether or not the addition of fluoroscopy and iodinated contrast to the injected saline load would serve as a helpful adjuncts in the diagnosis of arthrotomies, a method not previously described in the diagnosis of ankle arthrotomies in the emergency room setting.
Materials and Methods
The study was performed at one site by the lead author and an assistant. Four different cadaveric mid-leg through toes specimens (2 right ankles, 2 left ankles) were used from 4 unique donors. The average age of the donors was 55.8 years old (range 37 – 66), 3 of the donors were male, 3 were white, and 1 was African American. The lead author created an arthrotomy using a no. 11 scalpel in either the AL, AM, PL, or PM portion of the individual cadaveric ankles. The arthrotomies were created with a “stab” incision, and the entire blade was introduced into the specimen. The examiners used anatomic landmarks to ensure entry into the joint space from the AL, AM, PL, and PM aspects of the joint. This was confirmed with fluoroscopy and with extravasation of injected fluid. Care was taken not to enlarge the arthrotomy site with sawing or dragging of the scalpel blade. Each ankle specimen underwent arthrotomy creation in only 1 of the 4 aforementioned quadrants. No formal distraction setup was used in order to simulate an emergency room scenario. The specimens were each tested in a neutral position with the foot planted on the examination table. A standard anteromedial arthrocentesis portal was made using an 18-gauge needle on a 10-mL syringe; an anterolateral arthrocentesis portal was used for the ankle with the AM arthrotomy wound. The syringe was used to slowly inject normal saline (NS) into each ankle in 1-mL increments. After each milliliter was injected, the authors observed for 5 seconds and documented when the challenge was “positive”—defined as when the injected saline started to extravasate from the arthrotomy wound. No mechanical manipulation of the ankle or wound was performed. Needle position within the tibiotalar joint was confirmed using fluoroscopy for all of the ankles. After trialing all 4 ankles 10 times each (n = 40) with NS, the same procedure was performed 10 more times using a methylene blue–normal saline 1:1 solution (MB) for each ankle (n = 40). Our protocol mandated that after each ankle was trialed, the specimens were drained of injected fluid with the needle/syringe and subsequently left on a back table to drain additional fluid in a dependent position.
Lastly, we used a fifth cadaveric ankle without an arthrotomy (right ankle, donor was a 37-year-old African American man) and injected close to 5 ml of Omnipaque 340 (iodinated contrast) into the tibiotalar joint to illustrate the radiographic appearance of an intact ankle joint using fluoroscopy. We then created an anterolateral ankle arthrotomy using a no. 11 scalpel to demonstrate the radiographic appearance of an ankle arthrotomy challenged with the radiopaque contrast solution.
Statistical Analyses
We compared the volume of NS (n = 40), volume of MB (n = 40), and the volume of any injected fluid (MB+NS, n = 80) necessary for a positive test using the independent samples t test or Mann-Whitney U test where appropriate. The 25th, 50th, 75th, 90th, and 95th percentiles of volumes needed for a positive challenge test for any injected fluid (n = 80), NS (n = 40), or MB (n = 40), were calculated.
Results
The mean fluid volume of all injected fluid samples necessary for a positive joint challenge was 5.5 mL (SD = 3.6 mL). The volume of fluid necessary to detect 25%, 50%, 75%, 90%, and 95% of ankle arthrotomies from any site was 2.0 mL, 4.5 mL, 9.0 mL, 10 mL, and 10 mL, respectively.
The volume of fluid necessary to detect 25%, 50%, 75%, 90%, and 95% of ankle arthrotomies stratified by NS vs MB is shown in Figure 1. There was no difference between the amounts of NS (5.5 mL ± 3.6) vs MB (5.6 mL ± 3.7) needed for a positive challenge test (P = .739).
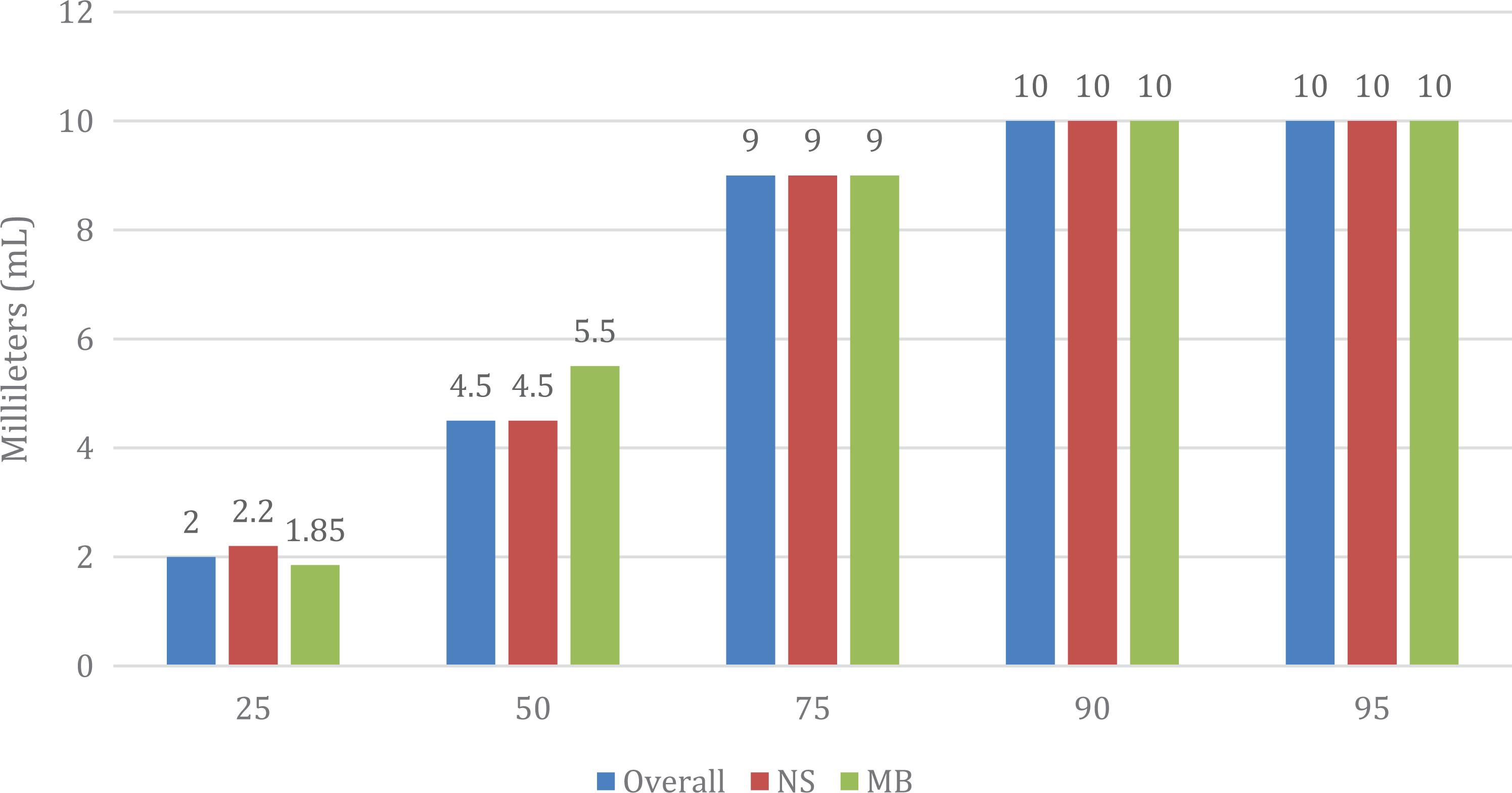
Percent detection of ankle arthrotomy in fluid load test using normal saline or methylene blue. The researchers found that 10 mL of either fluid was sufficient to diagnose 95% of ankle arthrotomies.
The volume of fluid necessary to detect 25%, 50%, 75%, 90%, and 95% of ankle arthrotomies stratified by portal site is shown in Figure 2. Anterior (AM, AL) arthrotomies required less fluid (2.1 mL ± 0.5) than posterior (PM, PL) arthrotomies (9.0 mL ± 1.2) for a positive test (P < .0001).
Fluoroscopy assisted with needle placement into the tibiotalar joint. It can be used to diagnose arthrotomies with the use of radiopaque contrast.

Percentage detection of ankle arthrotomy by portal position using either type of fluid (NS or MB). The examiners found that both the anteromedial and anterolateral portals required less fluid to be injected for a positive test than either the posteromedial or posterolateral portals. Examiners found no difference between NS or MB in detecting ankle arthrotomies. NS, normal saline; MB, methylene blue.
Discussion
Traumatic arthrotomies are common injuries that require urgent operative intervention, and although there have been multiple studies examining the SLT in larger joints, there is a paucity of literature with regard to traumatic arthrotomies of the ankle. Two previous studies attempted to determine the minimum volume of saline required to achieve a high sensitivity for detection of ankle arthrotomies in living patients undergoing ankle arthroscopy. However, to our knowledge, the present study is the first cadaveric study examining the role of the nonarthroscopic SLT with regard to diagnosing ankle arthrotomies.
In the previous study by Bariteau et al, 21 patients underwent ankle arthroscopy via an AL arthrotomy site. 1 The authors reported that 30 mL of saline was required to achieve 99% sensitivity. Another study by Bohl et al examined 42 patients undergoing ankle arthroscopy via an AM arthrotomy site and reported that 50 mL, 55 mL and 60 mL must be injected to achieve 90%, 95%, and 99% sensitivity, respectively. 2 The present study of 4 cadaveric ankles examined AM, AL, PM, and PL arthrotomies and demonstrated that 10 mL of saline was required to diagnose 95% of ankle arthrotomies regardless of arthrotomy location. The underlying pathology of the patients who underwent an ankle arthroscopy in the previous studies may explain the drastic differences in volume between the previous arthroscopic models and the present cadaveric model. More specifically, in those patients undergoing arthroscopy, scarring or hypertrophy of the capsule could have altered the distensibility of the joint, leading to differences in the volumes needed for a positive test. 2 Furthermore, the arthroscopic studies may have been performed with the presence of traction, which distends the ankle joint. Finally, arthroscopic portal sites are kept small to create a 1-way valve effect that prevents outflow of fluid during the case; this along with other factors could potentially result in more volume necessary for extravasation. These factors could account for the differences between the results of the current study in contrast to prior investigations.
The present study also found that anterior arthrotomies required significantly less fluid than posterior arthrotomies. The difference may be the result of soft tissue characteristics (synovial outpouching, plicae, capsule/ligamentous elasticity, capsule volume in the setting or arthritic conditions, etc) or related to the bony anatomy. The authors postulate that there may be a difference in hydrodynamics if fluid is introduced anteriorly into the tibiotalar joint and exits anteriorly vs posteriorly given that the width of the talar dome is larger anteriorly than posteriorly. 4 Perhaps there is a larger potential space posteriorly, which requires filling prior to extravasation. Also, as cadaveric specimens are often contracted posteriorly, it is possible that the rigidity of the tissues required more fluid injection in order for extravasation to occur.
With regard to MB, the present study found that its addition to NS did not decrease the volume needed for a positive test when compared to NS alone. These results are consistent with the study performed by Metzger et al, which found no difference in SLT sensitivities with or without MB in traumatic knee arthrotomies. 8 Furthermore, MB may be cytotoxic to chondrocytes as demonstrated by Getgood et al, who observed reduced viability of chondrocytes cultured in vitro on collagen membranes marked with MB marking pens. 5 The addition of MB to solution has traditionally been left to surgeon preference in the diagnosis of arthrotomies; however, because it is a potential cytotoxin and does not improve the diagnostic ability of the SLT in traumatic ankle arthrotomies, the authors recommend against its use.
The use of fluoroscopy to confirm and guide needle placement within the tibiotalar joint was another non-objective data point worth noting (Figures 3 and 4). The authors observed that in the 66-year-old cadaveric specimen, there was a large anterior tibial osteophyte at the level of the plafond that blocked needle insertion when performed without fluoroscopy. The osteophyte was more easily bypassed once fluoroscopy was used. In summation, the authors believe that the routine use of fluoroscopy will lead to less diagnostic error and morbidity such as iatrogenic cartilaginous injury and repeated needle sticks.

Fluoroscopic mortise view of a cadaveric left ankle specimen with an 18-gauge needle placed in the anteromedial arthrocentesis site within the tibiotalar joint.

Fluoroscopic lateral view of a cadaveric left ankle specimen with an 18-gauge needle placed in the anteromedial arthrocentesis site within the tibiotalar joint. Note how the needle is well centered within the joint.
Lastly, we evaluated the impact of iodinated contrast in the diagnosis of traumatic ankle arthrotomies. To facilitate this, a fifth cadaveric ankle specimen without a prior arthrotomy site was used. The solution of iodinated contrast and NS (5 mL of NS, 5 mL of Omnipaque 340) was injected via the standard AM arthrocentesis site and subsequently imaged (Figure 5). Thereafter, a traumatic AL arthrotomy was created and the ankle was again imaged with fluoroscopy; the extravasation of contrast solution was easily identified by the examiners (Figure 6). This additional method represents yet another useful adjunct in the diagnosis of traumatic ankle arthrotomies, particularly in the emergency room setting when the diagnosis remains uncertain. The benefit of using this method is that the needle position within the tibiotalar joint can be confirmed, and capsular disruption is more readily identifiable via arthrography. The examiners did not record the volume of contrast solution injected into the ankle with this method, but instead relied on the radiographic appearance of contrast extravasation to confirm the presence of an arthrotomy.

Fluoroscopic mortise view of a cadaveric right ankle specimen demonstrating iodinated contrast solution within the tibiotalar joint introduced via an anteromedial arthrocentesis site. Note how the contrast solution is well demarcated and maintained within the joint space.
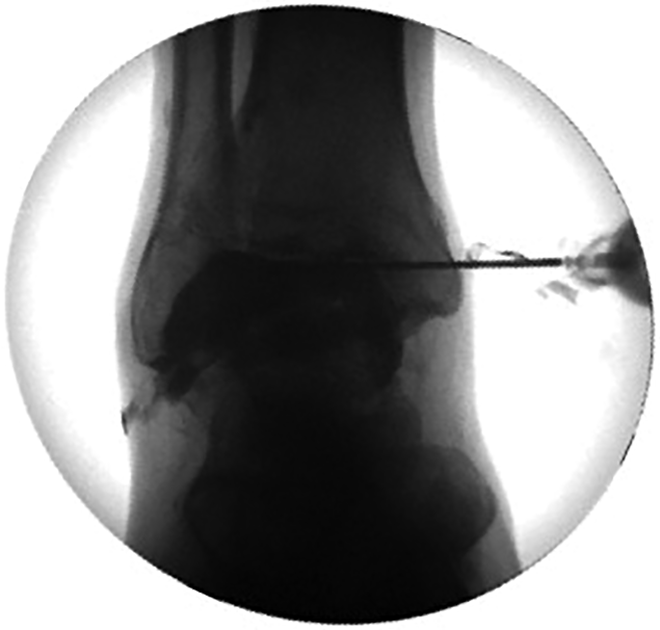
Fluoroscopic mortise view of a cadaveric right ankle specimen demonstrating iodinated contrast solution extravasation from an anterolateral arthrotomy site. Note how the contrast solution is not entirely contained within the tibiotalar joint.
It is important to acknowledge the various limitations to this current study. The present study represents a simulated traumatic ankle arthrotomy and used cadaveric specimens. The volumes required for a positive diagnosis may differ in the setting of trauma and in vivo, considering the contracted nature of cadaveric specimens. Another limitation is that only 4 cadaveric specimens were used and trialed 10 times each; this may have produced unreliable results because it is difficult to remove all of the fluid injected after each trial. We did not note, however, a decrease in fluid necessary for extravasation between subsequent tests. There may also be differences in the morphology of ankle joints, soft tissue elasticity, and capsular contractures (and therefore the volumes required for positive diagnosis of an arthrotomy) among pediatric vs adult vs geriatric specimens, different ethnicities, and different sexes. Ideally, more cadaveric ankles could have been used for the study to provide enhanced power and represent greater range with regard to age, sex, ethnicity, and ankle morphology. It is important to recognize that only a single specimen was used to evaluate the utility of iodinated contrast in the setting of traumatic ankle arthrotomies; more research is needed to gauge its true utility in this particular clinical setting.
In conclusion, 95% of ankle arthrotomies were diagnosed with 10 mL of injected fluid in this cadaveric model. There was no difference between NS vs MB challenge test volumes in the diagnosis of ankle arthrotomies. All anterior ankle arthrotomies required significantly less fluid to be injected into the joint for a positive SLT than all of the posterior ankle arthrotomies, regardless of injected fluid. Fluoroscopy assisted with needle placement and could be used to diagnose arthrotomies with the use of radiopaque contrast.
Supplemental Material
Supplemental Material, FAO905610-ICMJE - Diagnosis of Traumatic Ankle Arthrotomies Using Saline Load Tests, Methylene Blue, and Radiopaque Tracer: A Cadaveric Study
Supplemental Material, FAO905610-ICMJE for Diagnosis of Traumatic Ankle Arthrotomies Using Saline Load Tests, Methylene Blue, and Radiopaque Tracer: A Cadaveric Study by Paul R. Allegra, Rafael A. Sanchez, Samuel Huntley, Loren Latta, Sohil S. Desai, Jonathan Kaplan and Amiethab Aiyer in Foot & Ankle Orthopaedics
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. ICMJE forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
