Abstract
Background:
While proximal first metatarsal osteotomy combined with distal soft tissue realignment is accepted as standard treatment of moderate to severe hallux valgus with metatarsus primus varus, none of the described proximal metatarsal osteotomies address the hyper-obliquity of the first metatarsocuneiform joint. An opening-wedge osteotomy of the medial cuneiform can potentially correct the 1-2 intermetatarsal angle (IMA) in addition to normalizing the hyper-obliquity of the first tarsometatarsal (TMT) joint. The purpose of this study was to retrospectively review the early radiographic and clinical results of the use of a medial cuneiform opening-wedge osteotomy fixed with a low-profile wedge plate combined with distal soft tissue realignment for the treatment of hallux valgus.
Methods:
Fourteen feet (13 patients; 2 male and 11 female, average age 56 years, range 22-75) with hallux valgus underwent an opening-wedge osteotomy of the medial cuneiform fixed with a low-profile nonlocking wedge plate combined with distal soft tissue realignment. The mean preoperative hallux valgus angle (HVA) was 32 degrees and the IMA was 16 degrees. HVA, 1-2 IMA, proximal first metatarsal inclination (PFMI), and presence of osteoarthritis of the first TMT joint were assessed on preoperative and final postoperative radiographs. Final postoperative radiographs were also evaluated for radiographic union and hardware failure at an average of 7 months (range, 3-19 months) postoperatively.
Results:
A mean intraoperative correction of 19 degrees and 7 degrees was achieved for the HVA and IMA, respectively. The mean HVA was 22 degrees and the mean IMA was 11 degrees at the time of final follow-up. At final follow-up, a recurrence of the deformity was observed in 12/14 feet. There were 2 nonunions—one plate failure and one screw failure. No first TMT joint instability or arthritis was observed. All patients were ambulatory without assistive device in either fashionable or comfortable shoe wear.
Conclusion:
Medial cuneiform opening-wedge osteotomy resulted in unreliable correction of HVA and IMA at short-term follow-up with a high rate of early recurrence of hallux valgus deformity and a complication rate similar to that of the Lapidus procedure. This procedure cannot be recommended for addressing hallux valgus in the setting of increased obliquity of the first TMT joint.
Level of Evidence:
Level IV, case series.
Keywords
Introduction
Despite the numerous articles published on treatment of hallux valgus, very few have sought to explain the role of the obliquity of the first tarsometatarsal (TMT) joint in the development of hallux valgus. Hyper-obliquity of the first TMT could be associated with progressive metatarsus varus or instability of the first TMT joint. Hypermobility of the first ray at the first TMT joint has been previously associated with progressive hallux valgus. 6,7,15,16 The issue of first ray obliquity has been considered controversial because measurement of first TMT inclination is dependent on radiographic technique and requires the x-ray beam to be angled perpendicular to the first TMT joint. In fact, some authors have called into question whether the apparent orientation of the first TMT joint is real or rather a radiographic artifact as a result of x-ray beam orientation. 3
The term metatarsus primus varus was first used in 1924 to describe an oblique or varus position of the first metatarsal and was thought to be the primary factor leading to the development of hallux valgus. 28 Varus of the first metatarsal causes the axis of motion of the first TMT joint to be oblique rather than perpendicular to the long axis of the foot. The first operation described to address first TMT obliquity directly involved a laterally based closing wedge osteotomy of the medial cuneiform combined with distal soft tissue realignment. The author of that first description emphasized that attempts to correct metatarsus primus varus with a distal based osteotomy could lead to failure or recurrence if the first TMT joint obliquity was not addressed. 9
This was corroborated by an anatomic study that found the first TMT joint to be oriented obliquely both medially and distally in feet with hallux valgus compared to normal controls. 10 A more recent radiographic study also confirmed, using a 2-dimensional coordinate system, that the articular surface of the first TMT joint is inclined medially in patients with hallux valgus compared to normal controls. 26 Both proximal and distal osteotomies have been successful in the treatment of metatarsus primus varus, but failure to address the obliquity of the first TMT joint may lead to instability of the first TMT joint with subsequent recurrence (Figure 1). 2,17,21,23 -25 An opening-wedge osteotomy of the medial cuneiform may correct the first TMT joint obliquity and thus serve to stabilize the joint (Figure 2).

Progressive instability of the hallux at the MTC (metatarsocuneiform joint) is seen with resultant OA (osteoarthritis) at 1-year follow-up for a patient treated with an opening-wedge osteotomy of the proximal metatarsal.
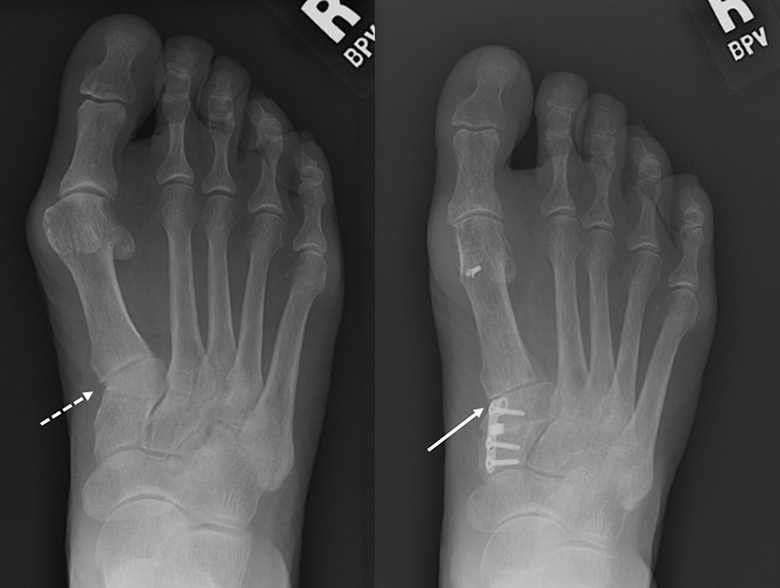
Correction of metatarsocuneiform obliquity (dashed arrow) demonstrated following opening-wedge osteotomy of the cuneiform (solid arrow).
The purpose of this study was to describe our experience with treatment of hallux valgus with associated metatarsus primus varus and first TMT joint obliquity utilizing a medial cuneiform opening-wedge osteotomy fixed with a low-profile wedge plate combined with distal soft tissue realignment. We hypothesized that medial cuneiform opening-wedge osteotomy combined with distal soft tissue realignment would be a safe and effective treatment for moderate to severe hallux valgus with metatarsus primus varus, providing correction of first TMT joint obliquity and conferring stability to the first TMT joint.
Materials and Methods
Approval for this study was obtained through an institutional review board. We retrospectively reviewed the radiographic and clinical records of 14 consecutive patients (16 feet), 2 male and 12 female, who had symptomatic hallux valgus, associated metatarsus primus varus, and medial first TMT obliquity who underwent medial cuneiform opening-wedge osteotomy (CPT 28304) fixed with a low-profile wedge plate combined with distal soft tissue realignment between January 2008 and December 2009. Surgical indications for cuneiform osteotomy included symptomatic hallux valgus with an incongruent hallux metatarsophalangeal (MTP) joint and associated metatarsus primus varus with medial hyper-obliquity of the first TMT joint. All patients demonstrated failure of prior conservative treatment including shoe wear modification and splinting. No patients had a prior bunion procedure.
Two feet were excluded from the analysis, the first due to the addition of a metatarsophalangeal fusion at the time of the index procedure and the second patient since only the initial intraoperative radiographs were available. This second patient had an early loss of fixation after a fall requiring revision to a Lapidus. Thus, data from the remaining 13 patients (14 feet) who underwent pre- and postoperative radiographic and clinical evaluation are presented in this study. These included 5 left and 9 right feet, all with incongruent MTP joints and moderate to severe hallux valgus preoperatively (Table 1). The average patient age was 56 years old (range 22-75). Seven of 13 (54%) patients underwent additional procedures at the time of hallux valgus correction (Table 1).
Patient Characteristics.

HVA, hallux valgus angle; IMA, intermetatarsal angle; Intraop, intraoperation; MTPJ, metatarsal phalangeal joint; NR, not recorded; PFMI, proximal first metatarsal inclination angle.
Radiographic evaluation included assessment of hallux valgus angle (HVA), 1-2 intermetatarsal angle (IMA), proximal first metatarsal inclination angle (PFMI), and radiographic union (Figure 3). These measurements were made on digital weightbearing anteroposterior radiographs preoperatively, at the first postoperative visit and at the time of most recent follow-up. Final radiographic and clinical analysis occurred at an average of 7 months (range, 3-19 months) postoperatively. Measurements were made by 2 orthopedic foot and ankle fellows blinded to each other’s measurements. Each evaluator’s measurements were then averaged with those of the other evaluator . Both hallux valgus angle and 1-2 intermetatarsal angle have shown high intraobserver and interobserver reliability across multiple studies. 5,19 PFMI was selected as a measure of first TMT joint obliquity. 26 PFMI was measured as the angle between a line perpendicular to the axis of the second metatarsal and a line parallel to the proximal articular surface of the first metatarsal, which is easier to visualize than the articular surface of the medial cuneiform (Figure 3C). Clinical evaluation consisted of an assessment of clinical alignment, weight-bearing status, return to shoe wear, and complications. Radiographs were reviewed to evaluate healing of the osteotomy.

(A) HVA (hallux valgus angle); (B) IMA (intermetatarsal angle); (C) PFMI (proximal first metatarsal inclination angle).
Statistical analysis consisted of calculating means and ranges for preoperative, postoperative, and final HVA, IMA, and PFMI. Comparison was made between preoperative and immediate postoperative radiographic values to determine whether satisfactory intraoperative correction of the hallux valgus deformity was obtained. Additionally, comparison was made between immediate postoperative and final follow-up radiographs to determine if the intraoperative correction was maintained during the postoperative period. A Student paired t test was performed to determine if there were statistically significant differences between the means of pre- and postoperative measurements and between the means of postoperative and final measurements (Table 2).
Results.
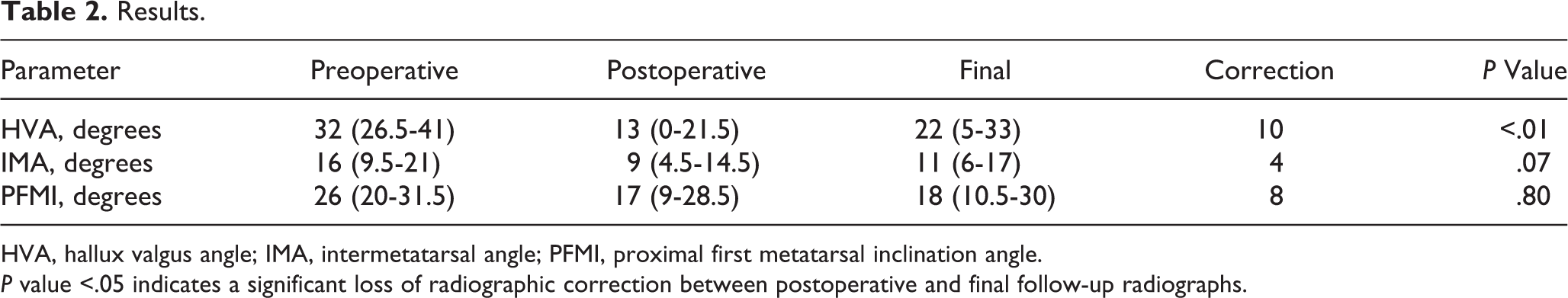
HVA, hallux valgus angle; IMA, intermetatarsal angle; PFMI, proximal first metatarsal inclination angle.
P value <.05 indicates a significant loss of radiographic correction between postoperative and final follow-up radiographs.
There was no commercial support or other external funding provided for this study.
Surgical Technique
A medial midsagittal incision was made from the midproximal phalanx to the naviculocuneiform joint. An inverted-L capsulotomy was made at the MTP joint, with care taken to avoid injury to the dorsomedial cutaneous nerve. The medial eminence was resected in line with the long axis of the first metatarsal. A second, 2-cm longitudinal incision was made dorsally in the 1-2 interspace at the level of the hallux MTP joint. The adductor tendon was sharply released from its insertion on the base of the proximal phalanx and the lateral aspect of the fibular sesamoid. The transverse metatarsal ligament was identified and divided followed by capsulotomies of the metatarsosesamoid joint and lateral MTP joint to restore appropriate sesamoid station and MTP joint congruency.
Attention was then turned to the medial cuneiform, where a dorsoplantar periosteal incision was made medially at the level of the second TMT joint. Two small Hohmann retractors were placed plantar and dorsal. Care was taken to avoid releasing the first TMT joint capsule, which could destabilize the joint and lead to failure of the correction. An osteotomy was made parallel to the TMT joint through approximately three-fourths of the width of the bone (Figure 4A). Care was taken to avoid completing the cut through the lateral cortex to prevent overlengthening of the first ray. The osteotomy was then carefully wedged open using a distractor. Once the correct IMA alignment had been obtained and the sesamoids had been reduced, a measuring guide was used to measure the osteotomy gap. A nonlocking osteotomy plate (Arthrex Low Profile Opening Wedge, Naples, FL) is then inserted into the osteotomy and fixated with 2.4-mm bicortical screws in all 4 holes. The osteotomy site was then filled with bone graft or bone graft substitute. A suture anchor was then placed centrally in the metatarsal head and the sutures were placed through the plantar medial capsule and tied in a mattress fashion securing the sesamoids into a reduced position and anchoring the joint capsule to the metatarsal head. A pants-over-vest capsulorrhaphy was then completed, with the hallux MTP joint held in a reduced position. A final fluoroscopic examination was performed confirming reduction of the hallux metatarsophalangeal joint, sesamoid position, and osteotomy fixation (Figure 4B). A sterile dressing and short-leg bivalved fiberglass cast were applied postoperatively.

(A) The dashed line represents the planned osteotomy that is made parallel to the metatarsocuneiform joint and extends across three-fourths of the width of the cuneiform. (B) A postfixation image is recommended to verify the reduction of the metatarsophalangeal joint and the sesamoids.
Patients were seen at 2 weeks postoperatively for suture removal and recasting for an additional 2-4 weeks. At 6 weeks, patients were transitioned to a postoperative shoe and allowed to begin progressive weightbearing for 1 month, using a silicone toe spacer during the day and a bunion splint at night. At 10-12 weeks postoperatively, patients were allowed to return to wide toe box shoes with continued use of a toe spacer and night splint for an additional 3 months.
Results
Preoperative hallux valgus severity was classified as moderate in 12/14 feet and severe in 2/14 feet. 7 No patients demonstrated hypermobility of the first ray on preoperative physical exam although objective measurements of hypermobility were not performed.
The mean preoperative HVA was 32 degrees (range 26.5-41 degrees) and the final mean value was 22 degrees (range 5-33 degrees). This 10-degree change in the HVA was statistically significant (P ≤ .01). The IMA corrected from a preoperative mean of 16 degrees (range 9.5-21 degrees) to a postoperative value of 11 degrees (range 6-17 degrees). The change in the IMA was not statistically significant (P = .07). The change in the PFMI from a mean of 26 degrees (range 20-31.5 degrees) to a mean of 18 degrees (range 10.5-30 degrees) was also not statistically significant (P = .80). The correction recorded in the IMA and PFMI at the first postoperative radiograph did not differ from final follow-up, but the mean HVA of 13 degrees recorded postoperatively did not persist through final follow-up (Tables 1 and 2).
There were of 4 osseous and hardware-related complications, including 2 nonunions—one broken plate and one broken screw. Neither patient with a nonunion elected to undergo revision. There was a high rate of partial recurrence of deformity, with 12/14 feet showing partial recurrence of hallux valgus angle and 1 patient with a nonunion who demonstrated a worse HVA at final follow-up compared to preoperatively. There were 7 intraoperative fractures of the lateral cortex of the medial cuneiform, 2 of which were treated with supplemental K-wire fixation at the time of surgery. None of the patients with lateral cortical fracture developed nonunion, and there was not an observed higher recurrence rate in these feet. There were no infections and no wound complications. Two patients complained of painful hardware, though neither had elected to undergo hardware removal. There was no first TMT joint instability or progressive arthrosis observed during postoperative follow-up. At final follow-up, all patients had returned to wearing either fashionable or comfortable shoes and none required assistive devices for ambulation.
Discussion
The medial cuneiform osteotomy provided intraoperative radiographic correction of hallux valgus deformity with associated increased first TMT obliquity; however, this correction was not maintained in most of the patients at short-term follow-up. The high rate of recurrence has been seen in other studies evaluating the proximal oblique metatarsal osteotomy. One recent study reported a 64.7% recurrence of the HVA associated with an increased preoperative distal metatarsal articular angle (DMAA). It is possible that a frontal plane correction of the IMA in a patient with an increased DMAA will result in worsening of that angle unless a distal metatarsal osteotomy is also performed. In addition, rotational correction of the first metatarsal is not possible with an opening-wedge technique. 13 Malrotation of the first metatarsal with increased pronation has been associated with hallux valgus deformity, and failure to correct that malrotation through the use of a wedge osteotomy may be associated with recurrence. 15
We had 3 cases of nonunion with hardware failure. 12,25 The observed high rate of hardware failure may have been related to the use of a low-profile standard nonlocking plate with 2.4-mm cortical screws for fixation of the osteotomy. In comparison, several recent studies have highlighted using a wedge-plate fixation for fixation of a proximal metatarsal opening-wedge osteotomy. 21,23,25 The reported benefits of wedge plate fixation over use of allograft or autograft wedges include less risk of graft collapse, accelerated rehabilitation, and time to weightbearing. The use of nonlocked plates is another potential factor associated with our high nonunion rate. However, the use of locking wedge plates is controversial as some studies have found that they may prevent nonunion and hardware failure, while other studies have demonstrated an increased rate. 11,12
A fusion of the first TMT is an alternative means of addressing first TMT obliquity or instability. First tarsometatarsal joint arthrodesis (modified Lapidus procedure), is another well-established treatment for symptomatic hallux valgus with associated metatarsus primus varus and increased first TMT medial obliquity. 6,8,15,16 Fusion of the first TMT joint could theoretically increase stresses at adjacent joints leading to degenerative arthritis and pain. 9,18 A first TMT arthrodesis also shortens the first ray which may have the associated increased risk of transfer metatarsalgia due to shortening, although stabilizing the TMT joint and placing the metatarsal in a more plantar position may mitigate that risk. 4 An opening-wedge osteotomy of the medial cuneiform may mitigate the potential risks of shortening, although comparative studies with longer follow-up would be required to evaluate that. Another concern with the Lapidus procedure is the potential risk of nonunion, which has been reported in up to 10% of patients in previous studies. 4,20 Given the 2 nonunions observed in our cohort, an opening-wedge osteotomy does not appear to have a decreased risk of nonunion when compared to the Lapidus procedure.
Only one other series reviewing the results of medial cuneiform opening-wedge osteotomy for treatment of hallux valgus in adults can be found in the orthopedic literature. A recently published retrospective case series detailed results of medial cuneiform opening wedge osteotomies using an allograft wedge combined with distal soft tissue realignment. 14 The series included 63 patients (101 feet) with an average age of 42 years with varying severity of hallux valgus deformities (4% mild, 54% moderate, and 42% severe). All patients underwent medial cuneiform osteotomy regardless of preoperative radiographic measurements or degree of first TMT joint obliquity. At a mean follow-up of 7.7 years (range, 1.5-14.8 years), all patients underwent radiographic evaluation, clinical exam, and AOFAS hallux metatarsophalangeal-interphalangeal scoring. Radiographs revealed improved mean HVA from 29 degrees preoperatively to 16 degrees postoperatively, and improved mean IMA from 14 degrees preoperatively to 10 degrees postoperatively in the moderate deformity group. The group of severely deformed feet had similar results. Average AOFAS Hallux MTP-IP score improved from 35 preoperatively to 86 postoperatively. The radiographic results of their study correlate well with the results of our current study; however, the studies varied in several ways. From a patient selection standpoint, their study did not include selection criteria in terms of preoperative intermetatarsal angle or medial obliquity of the first TMT joint. From a technical standpoint, allograft wedges were utilized rather than a wedge plate and there was no medial eminence resection performed in their study. The authors reported a 100% union rate with the use of allograft wedges. Additionally, in 15 feet, they performed a shortening osteotomy of the hallux proximal phalanx. Akin osteotomies of the hallux proximal phalanx were performed in 2 of our patients in order to correct hallux valgus interphalangeus. The authors did not list or record fracture of the cuneiform as a complication, although it is clearly demonstrated in 2 of the figures presented. In our study we had a high rate of intraoperative fracture of the lateral cortex of the cuneiform (7/14). With the low number of patients in our series, we were not able to correlate the fractures with the size of the wedge or to the experience of the senior author with the procedure. Of some concern in that study is the finding of osteoarthritis at the first TMT joint in 8/101 cases (7.9%) and in 15/101 cases (14.8%) at the MTP level at the time of most recent follow-up. 14 None of these patients reportedly had signs of osteoarthritis on preoperative radiographs. None of the patients in our current series demonstrated adjacent joint osteoarthritis at short-term follow-up.
This study has a number of limitations, including its retrospective design, small sample size, and short follow-up. Moreover we only evaluated radiographic and not functional outcomes. Because radiographic measurements were utilized in the study, it should be noted that both intraobserver and interobserver reliability rates are decreased when evaluating postoperative radiographs after hallux valgus surgery. 1,22 In addition, the PFMI on both pre- and postoperative radiographs can be altered if the x-ray beam is not angled perpendicular to the first TMT joint. It is also possible that the first TMT obliquity observed radiographically is not related to the actual cuneiform shape but rather is a radiographic phenomenon related to a combination of frontal, sagittal, or transverse plane motion of the first ray and TMT joint.
While our final radiographic outcomes were mostly poor, some authors have observed that functional outcomes do not always correlate with radiographic outcomes after hallux valgus surgery. 27 Thus, a larger longitudinal cohort study measuring functional and radiographic outcomes is needed to clarify the relationship between hallux valgus and first TMT joint obliquity.
Conclusion
Medial cuneiform opening-wedge osteotomy resulted in unreliable correction of HVA and IMA at short-term follow-up with a high rate of early recurrence of hallux valgus deformity and a complication rate similar to or greater than that of the Lapidus procedure. This procedure cannot be recommended for addressing hallux valgus in the setting of increased obliquity of the first tarsalmetatarsal joint.
Supplemental Material
Supplemental Material, FAI813318-ICMJE - Medial Cuneiform Opening-Wedge Osteotomy for the Treatment of Hallux Valgus
Supplemental Material, FAI813318-ICMJE for Medial Cuneiform Opening-Wedge Osteotomy for the Treatment of Hallux Valgus by Jason S. Ahuero, John S. Kirchner, and Paul M. Ryan in Foot & Ankle Orthopaedics
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. ICMJE forms for all authors are available online.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
