Abstract
Diagnosis of mid-cheek mass has always been a diagnostic dilemma for clinicians. The incidence of the accessory parotid gland (APG) has been well documented in the literature. However, a diverse spectrum of pathologies can arise from this accessory parotid tissue. Basal cell adenoma is a rare benign tumor that predominantly affects the parotid gland. Its occurrence in the accessory parotid gland has been documented in 9 cases till date. Surgical approaches for the management of such APG lesions have been in debate. This report documents a case of Basal Cell Adenoma arising in accessory parotid tissue in a 55-year-old woman who was treated by transoral excision. This paper also reviews previously documented cases of all APG lesions and attempts to elucidate the rationale for selecting an appropriate surgical approach.
Introduction
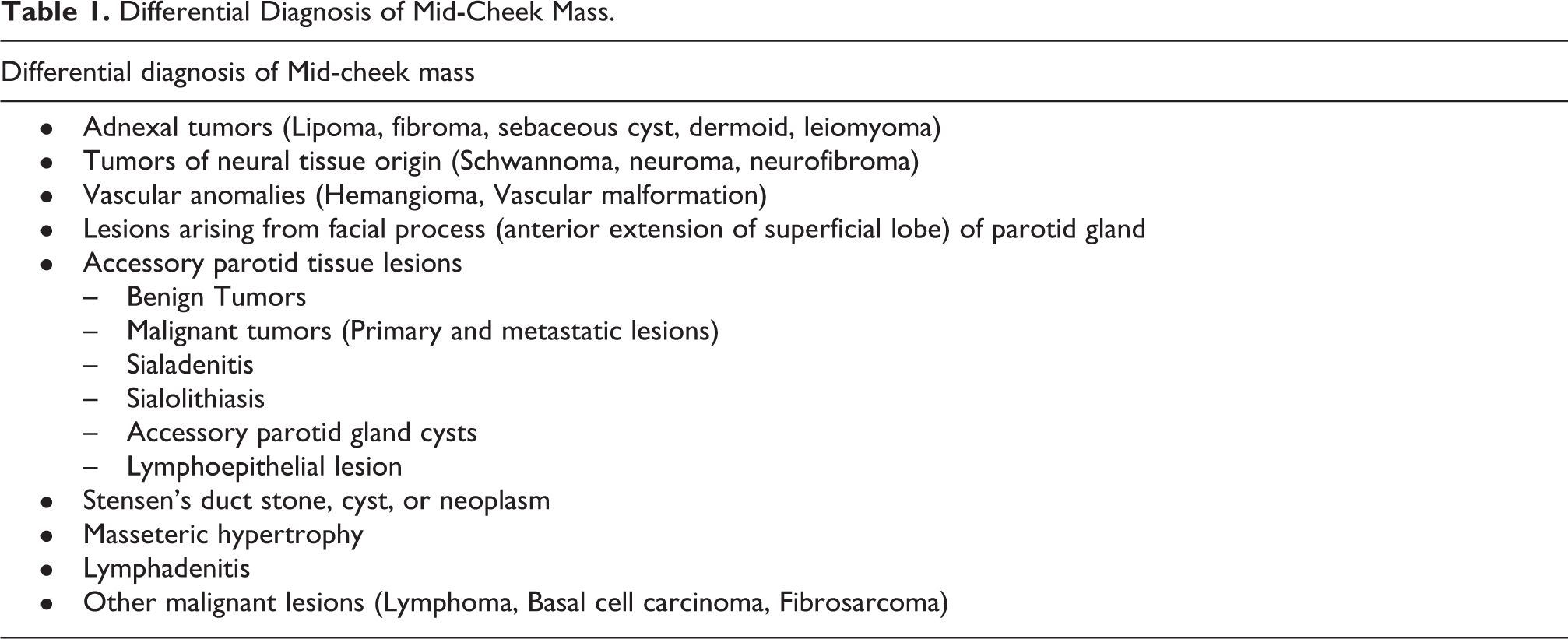
Diagnosis of mid-cheek mass is always challenging because of the anatomic complexities of this region. Pathology can arise out of the epidermis, dermis, nerves, vessels, accessory salivary gland tissue, Stensen’s duct, muscle, fat layer, or minor salivary glands. 1 Table 1 enlists differential diagnoses for such mid-cheek masses. 1 Smaller size lesions are even more misleading and may lead to incorrect diagnosis and subsequently inadequate treatment.
Differential Diagnosis of Mid-Cheek Mass.

Salivary gland tissue adjacent to the parotid duct (Stensen’s duct), but separate from the body of the parotid, is defined as accessory parotid gland (APG) tissue. 2 It is located along an imaginary line that extends from the tragus to a point midway between the ala of the nose and the vermilion border of the lip. Ahn et al in their computed tomographic assessment reported a 10% incidence of APG. 3 Frommer reported that accessory parotid tissue is present in 21% of the individuals. 4 Other studies have reported even higher incidence. 5
Historically, all benign tumors of salivary glands not showing pleomorphic characteristics were grouped under “Monomorphic Adenoma.” This terminology was dropped by World Health Organization (WHO) classification in 1991. Unfortunately, the terms monomorphic adenoma and basal cell adenoma have often been used interchangeably in the literature, which is inappropriate. The term Basal Cell Adenoma was first used by Kleinsasser and Klein in 1967. BCA is far more common in the parotid gland. It predominantly affects females above 50 years of age. Four subtypes of BCA have been identified viz. solid, trabecular, tubular, and membranous. Among these, membranous variants have multifocal micro-adenomas and a high rate of malignant transformation.
This case report presents a rare case of basal cell adenoma arising from accessory parotid tissue which was excised by intraoral approach.
Case Report
A 55-year-old female patient reported to us with a lump in the right mid-cheek region which has been present for more than 3 months. The increase in the size of the swelling was barely discernible. The patient complained of occasional dull pain in the same region. On examination, a 1 cm × 1 cm firm swelling was palpable at the anterior border of the masseter (Figure 1). The swelling was free from underlying tissues and overlying skin. A provisional diagnosis of lipoma was made. Ultrasonography (USG) and Magnetic Resonance Imaging (MRI) were advised. USG suggested the presence of a solid lesion. MRI studies showed a 1.3 cm × 1.1 cm well-defined enhancing lesion in right accessory parotid tissue, in T1 weighted fat suppressed post-contrast sequence in axial and coronal sections (Figure 2). A well-defined hypointense capsule of the lesion was noted. The lesion was separate from the main parotid gland tissue. Fine Needle Aspiration Cytology (FNAC) was suggestive of benign lesion of salivary gland origin and ruled out malignancy and vascular lesion. Considering the small size of the lesion and its benign nature we considered transoral excision of the lesion.
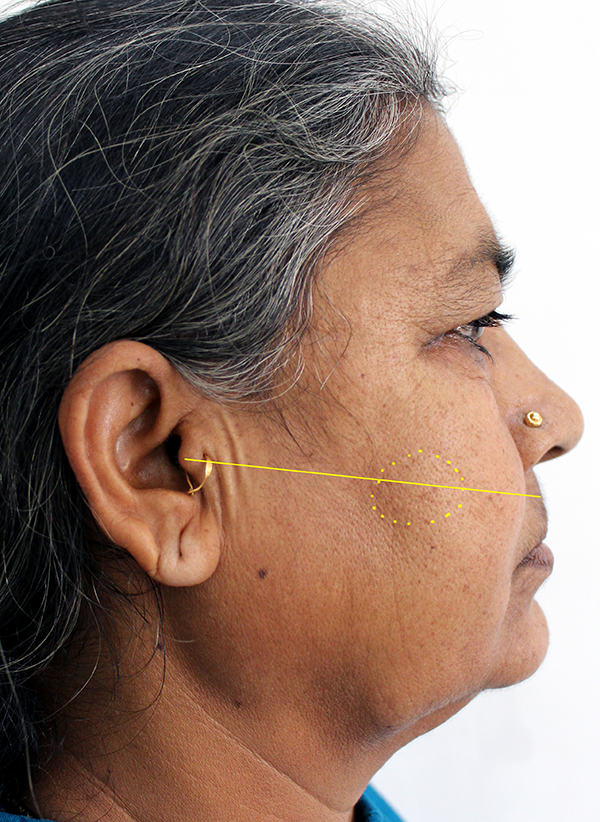
Profile picture of the patient showing the location of the swelling. Note that it is located along the line joining tragus and mid-point between the ala of nose and vermilion border of the upper lip.
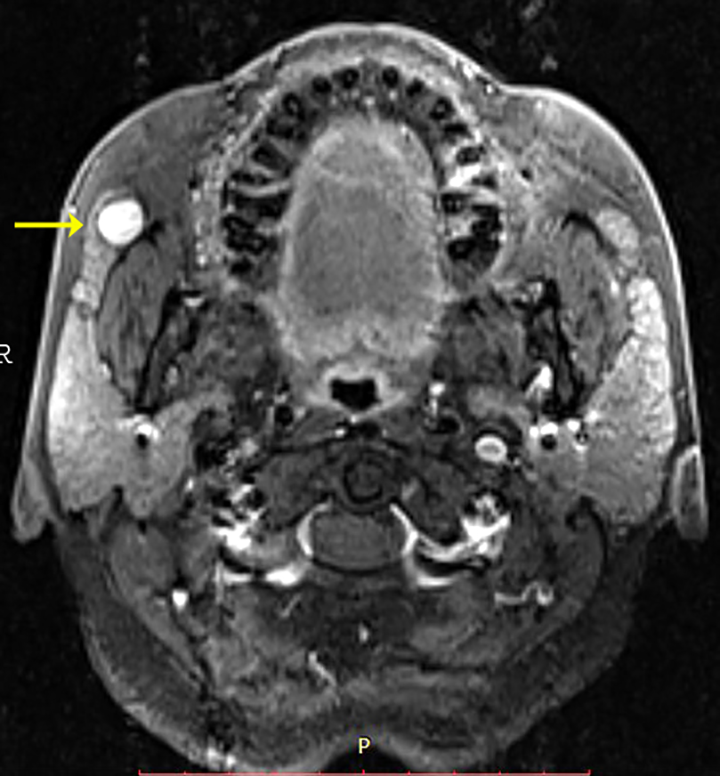
Axial, contrast-enhanced T1 weighted MRI image showing hypointense capsule around a homogenously enhancing lesion in the right accessory parotid gland located superficial to the masseter muscle. A distinction can be made between the main parotid gland and the accessory parotid tissue.
Informed consent was obtained, and surgery was planned under general anesthesia. The parotid duct was cannulated using an infant feeding tube and it was left in place till the completion of surgery. A small 2.5 cm incision was placed cephalad to Stensen’s duct opening (Figure 3). We minimized the use of cautery to prevent inadvertent injury to adjoining vital structures. Blunt dissection was carried out through the buccal fat pad. Bimanual palpation was done to orient dissection. With adequate illumination and retraction, mass was localized and excised (Figure 4). There was no significant bleeding encountered during or after surgery. The infant feeding tube was removed, and the patency of the duct was reassessed. A small Penrose drain was placed, and closure was done with resorbable sutures. Excised tissue was forwarded for histopathological examination. The postoperative course was uneventful with no evidence of facial nerve injury. There were no signs of parotid duct injury. The patient was discharged the next day and asked to follow up on regular basis. A 2-week postoperative MRI showed complete elimination of the lesion (Figure 5). There is no evidence of any recurrence in the last 24 months.
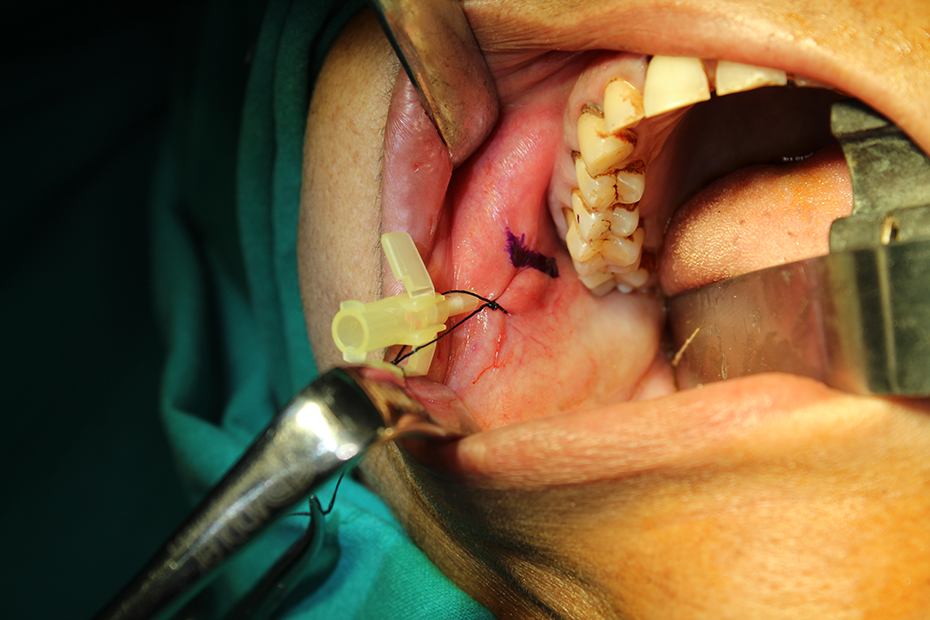
Marking of incision cephalad to Stensen’s duct opening. Intravenous (IV) cannula sleeve used for identification of Stensen’s duct opening.
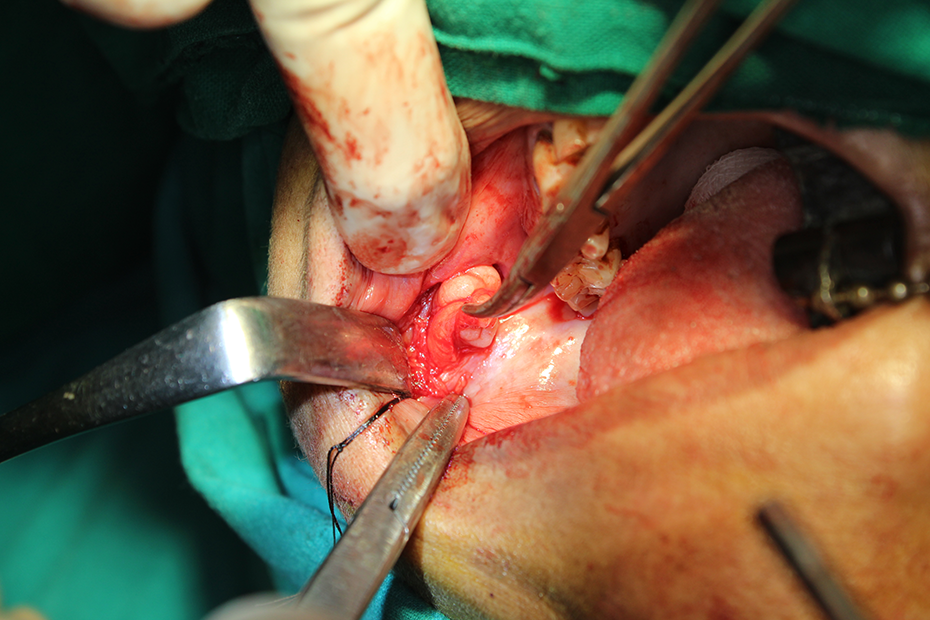
Excision of the mass in toto.
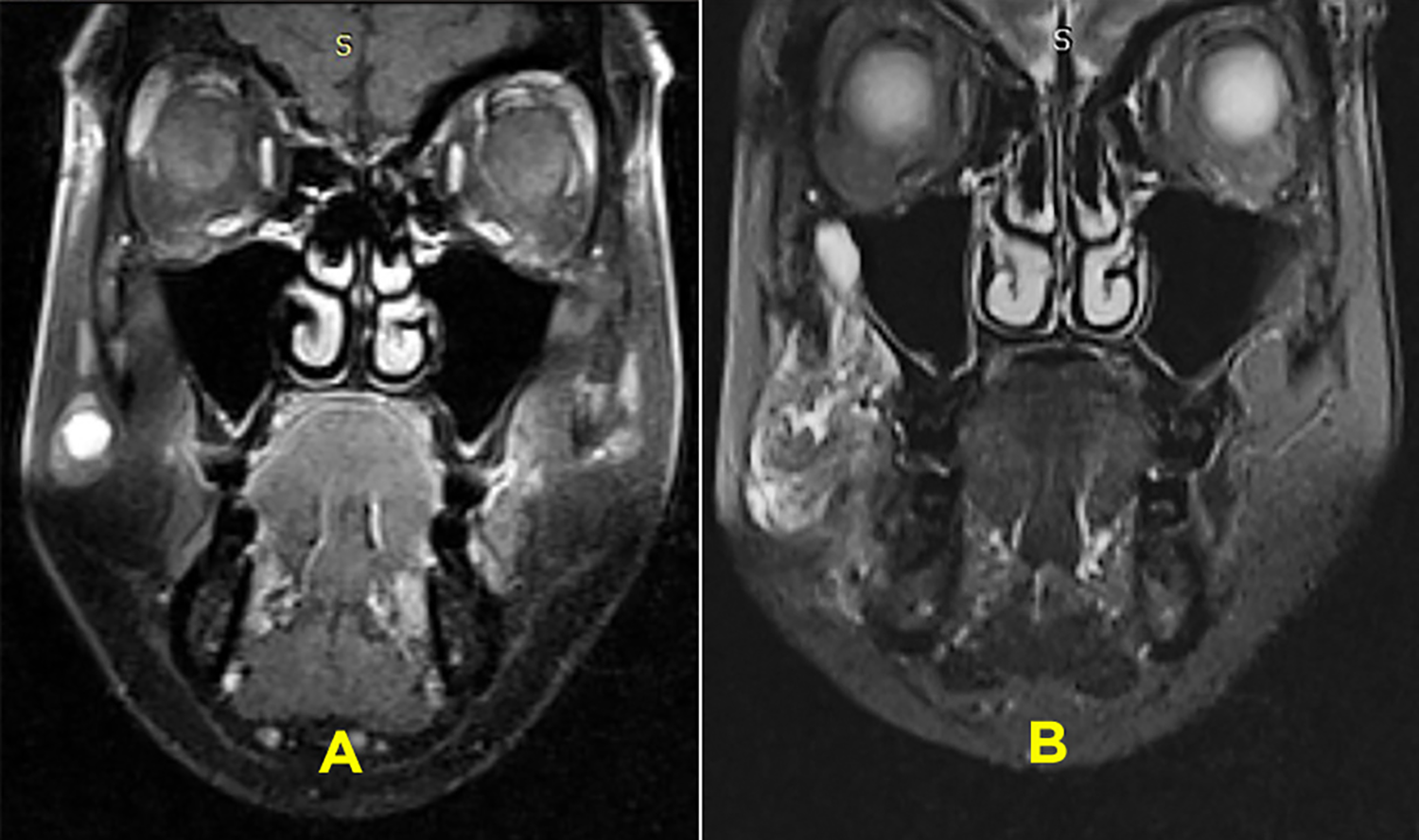
Comparison of preoperative and 2-week postoperative MRI. Figure (A) shows the coronal section of preoperative T1 weighted MRI showing homogeneously enhancing lesion, surrounded by hypointense tissue. Figure (B) shows the coronal section of a 2-week postoperative T2 weighted MRI showing complete elimination of the lesion. Note the postoperative inflammation around the location of the lesion.
Histopathology showed monotonous proliferation of basaloid cells having round to oval hyperchromatic nuclei and pale eosinophilic cytoplasm. Tumor cells were arranged in tubules, trabeculae, and solid nests with thin fibrous connective tissue stroma. Peripheral palisading was observed within the nests (Figure 6). Pleomorphism, mitosis, invasion, and necrosis were absent. Based on these findings, the final diagnosis of Basal Cell Adenoma was made.
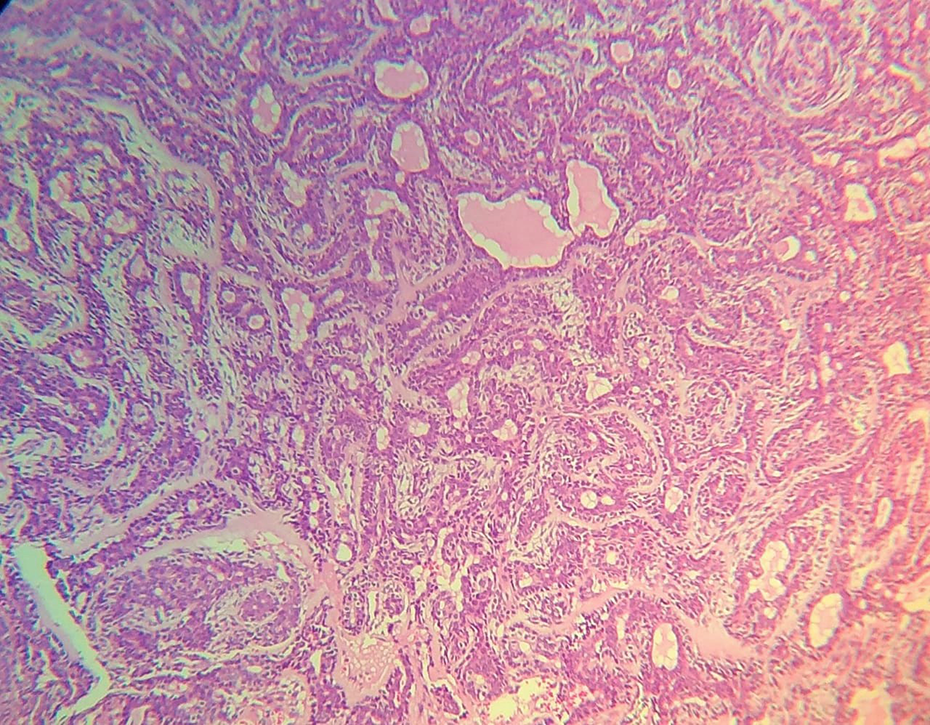
Histological section showing basaloid cells with round to oval nuclei, with eosinophilic cytoplasm arranged in a tubulo-trabecular pattern (H & E stain, 10×).
As per our institute protocol, this being a single case report with a review, it was exempted from Institutional Review Board (IRB) approval.
Discussion
Basal cell adenoma is rarely found in accessory parotid gland tissue (APG). To the best of our knowledge, there have been 9 such cases reported in the literature till date. 6 –12 Only 1 reported case of BCA has been operated by transoral endoscopic approach. 8
There is little controversy over the diagnostic approach for APG pathologies. The clinical examination which reveals a mass in this APG region should be investigated further using CT (computed tomography) and/or MRI and FNAC. Nemecek et al 13 suggested that MRI is the best imaging technique for defining soft tissue pathology associated with APG, although some authors recommend CT over MRI. Chiu et al suggested that the age of the patient and the attenuation on unenhanced and contrast-enhanced CT may help in differentiating basal cell adenoma from pleomorphic adenoma of the parotid gland. 14 We had both contrast-enhanced CT and MRI for this patient. Authors believe that MRI gives a better delineation of such APG pathologies compared to CT. There has been some controversy over the diagnostic accuracy of FNAC. Most studies suggest that the diagnostic accuracy of FNAC is above 90%. Especially it has a good negative predictive value to rule out malignancies which makes it a useful diagnostic test.
The surgical approach to address such pathologies has been a topic of controversy in the literature. Four primary surgical approaches have been discussed in the literature. 1) Preauricular parotidectomy approach and its modifications, 2) direct cheek approach, 3) transoral/peroral buccal mucosa approach and 4) endoscopic approach. Choice of approach depends on the type of lesion, size of the pathology, need for parotidectomy, and skill of the operator. There has been some criticism in the past about the transoral approach for such APG pathologies. Opponents of this approach envisage the possibility of facial nerve injury, Stensen’s duct injury, and the possibility of inadequate excision owing to poor visualization. Authors strongly believe that small, non-malignant lesions, located anterior to masseter muscle are amenable for transoral excision provided it is distinctly separated from the main parotid gland. For that reason, it is imperative to radiologically distinguish between accessory parotid gland tissue and anterior extension of the main parotid gland. The use of high magnification and a good light source is a must. The endoscopic approach appears to be promising and will surely revolutionize the management of head and neck pathologies. Authors presently lack experience in minimally invasive techniques in the management of such lesions.
Authors have reviewed documented English literature extracted from PubMed and Web of Science databases related to APG and mid-cheek lesions from January 1966 till March 2020. Authors have taken the utmost precaution to eliminate duplication of studies from 1 center. Also, some of the old terminologies have been purposely retained to avoid misinterpretation of data and diagnoses have been recorded as described in respective case reports (Table 2). The incidence of malignancy in APG tissue is significantly higher (26–50%) than in the parotid gland. 15,16 Most commonly found benign tumor is Pleomorphic adenoma (85%) whereas mucoepidermoid carcinoma (42.9%) is the most commonly seen malignant tumor in APG. 9 cases of BCA have been reported in the literature comprising 5% of all benign tumors of APG. 6 –12 Out of 9 cases of BCA, 7 cases have been operated by standard parotidectomy approach or one of its modifications. One case described by Xie et al 11 is managed by a preauricular endoscopic approach. Kim et al 8 reported 2 cases of BCA, 1 operated by parotidectomy approach and 1 by transoral endoscopic approach. Schmutzhard et al 17 have suggested the use of facial nerve monitoring for transoral excision of APG lesions. None of the cases have reported recurrence irrespective of the approach used.
Review of Literature of Accessory Parotid Gland Lesions.

The prognosis of most benign pathologies involving APG is good. Very few cases of recurrence have been reported in the literature. In our case report, 2 years of follow-up is not enough to prove the adequacy of treatment. However, considering lesser recurrence rates and the overall “benign” nature of such lesion, a less morbid-transoral approach can be considered as an alternative.
Conclusion
Given the myriad possibilities of pathologies that may arise in this region of the cheek, the clinician must use every possible diagnostic tool to reach a specific diagnosis before planning surgery. Basal cell adenoma although rare, should be considered in the list of differential diagnoses. Small non-malignant APG tumors are amenable to transoral excision. The importance of long-term follow-up should not be underestimated.
Footnotes
Acknowledgements
Sincere thanks to Department of Oral Pathology, Terna Dental College and Department of Radiology, Terna Speciality Hospital and Research Centre for their support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
