Abstract
Dislocation of the mandibular condyle into the middle cranial fossa is a rare event with only 59 cases having been reported in the English literature. The common etiology is road traffic accident. Epidemiology wise this injury is found commonly in children and young adults. This has been attributed to the undeveloped condyle being small and rounded. In this report we present a case of central dislocation of the mandibular condyle into the middle cranial fossa in a 20 year old female patient sustained in a road traffic accident. Computed tomography helped in early diagnosis and treatment of the patient. We also stress upon the need for long term follow up of the patient to prevent secondary complications of ankylosis.
Introduction
Facial trauma with dislocated fractures of the mandible condyle is a common presentation accounting for 25-40% of mandibular fractures. 1,2 Although, traumatic dislocation of the mandibular condyle is uncommon, direct dislocation of a mandibular condyle into the middle cranial fossa is an even rarer event with only as much as around 59 cases reported in the English literature. 3 The first cases were reported in 1960 by Heindseick and Dingman and Grabb in 1963. 4 The paucity of this injury was attributed to the fact that it was associated with high velocity road traffic accidents.
The most common etiology reported was road traffic accidents (53%) closely followed by falls and bicycle related injuries. 1,3 The dislocation was found to be more common in children and young adults (75%) and occurred more in women (69%) than in men. 1,3 Underdeveloped condyles being smaller and rounded can cause fracture of the thin glenoid fossa rather than the neck of the condyle which usually happens in mandibular trauma. 5 –10
The clinical findings included restricted jaw movements, altered occlusion with deviation of the jaw to the ipsilateral side. Almost all of the reported cases involved dislocation of only 1 joint except 1 case report of bilateral intracranial dislocation. 9 Trauma to the brain and its lining were very rare.
Identification of the dislocation is difficult with conventional radiographs and hence computed tomographic scans are essential to confirm the diagnosis of dislocation of the condyle into the middle cranial fossa. 1 –3,6,10 –12
The treatment goals include reduction of the condyle into its anatomical position within the glenoid fossa, restoring the barrier between the middle cranial fossa and the glenoid fossa, restoration of pre-injury occlusion, achieving good mouth opening and prevention of secondary neurological complications.
Several treatment modalities have been proposed for treatment of this type of injury, ranging from closed reduction with intermaxillary fixation to craniotomy, reduction and glenoid fossa reconstruction with autogenous and alloplastic materials. Condylotomies and condylectomies have also been performed in some cases when there was the risk for neurological injury during reduction. When diagnosed and treated early, surgery becomes simple without the need for extensive procedures, however if there is a delay, in diagnosis, treatment may necessitate additional procedures. 7,11,13 –16 The risk of ankylosis is present even when open reduction has been done and hence long term follow up of the patients is recommended. 14,16,17
In this article we discuss a case of central dislocation of the condyle in a young female patient sustained from a fall from a bike and the 10 year follow up of the patient. No similar long term follow up has yet been reported in English language literature.
Case Report
A 20 year old woman presented with trismus and inability to move her jaw following a fall from a 2 wheeler on 28 December 2010. She had transient loss of consciousness following the trauma. On arrival she was conscious, oriented with a Glasgow Coma Scale of 15/15. She complained of severe pain in her jaws with restricted jaw movements.
Patient was in distress. On examination she had a 2 cm laceration on the chin with an anterior open bite (Figure 1). Intraoral examination revealed an altered occlusion with anterior open bite and lateral deviation of the jaw to the left (Figure 2).
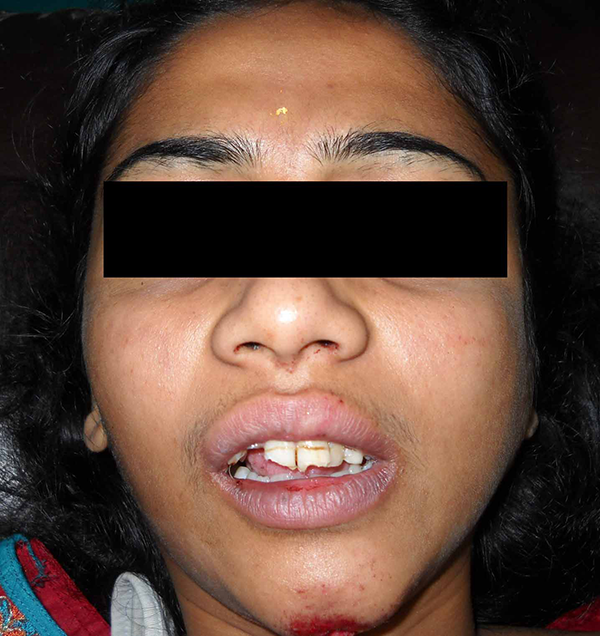
Patient at presentation with pain in the lower jaw and severely restricted jaw movements.
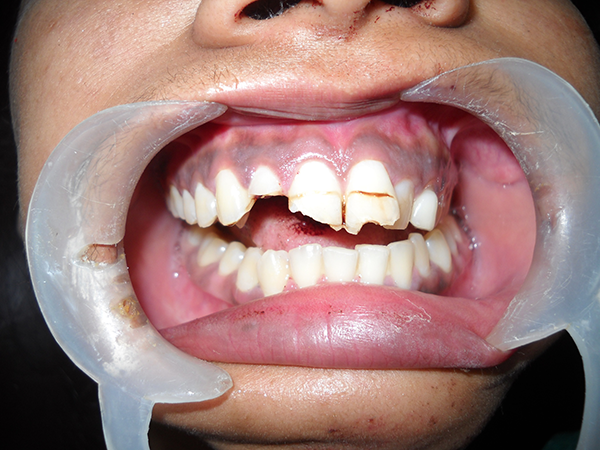
Occlusal derangement seen with open bite and laterognathism to the ipsilateral side.
A CT scan was done which showed a traumatic dislocation of an intact left condyle into the middle cranial fossa, anteromedial displacement of the thin glenoid fossa bone with surrounding pneumocephalus (Figure 3(A) and (B)). A neurosurgical opinion was obtained prior to management by closed reduction. If unsuccessful, the second line of treatment planned was craniotomy, reduction of the condyle and reconstruction of the glenoid fossa.
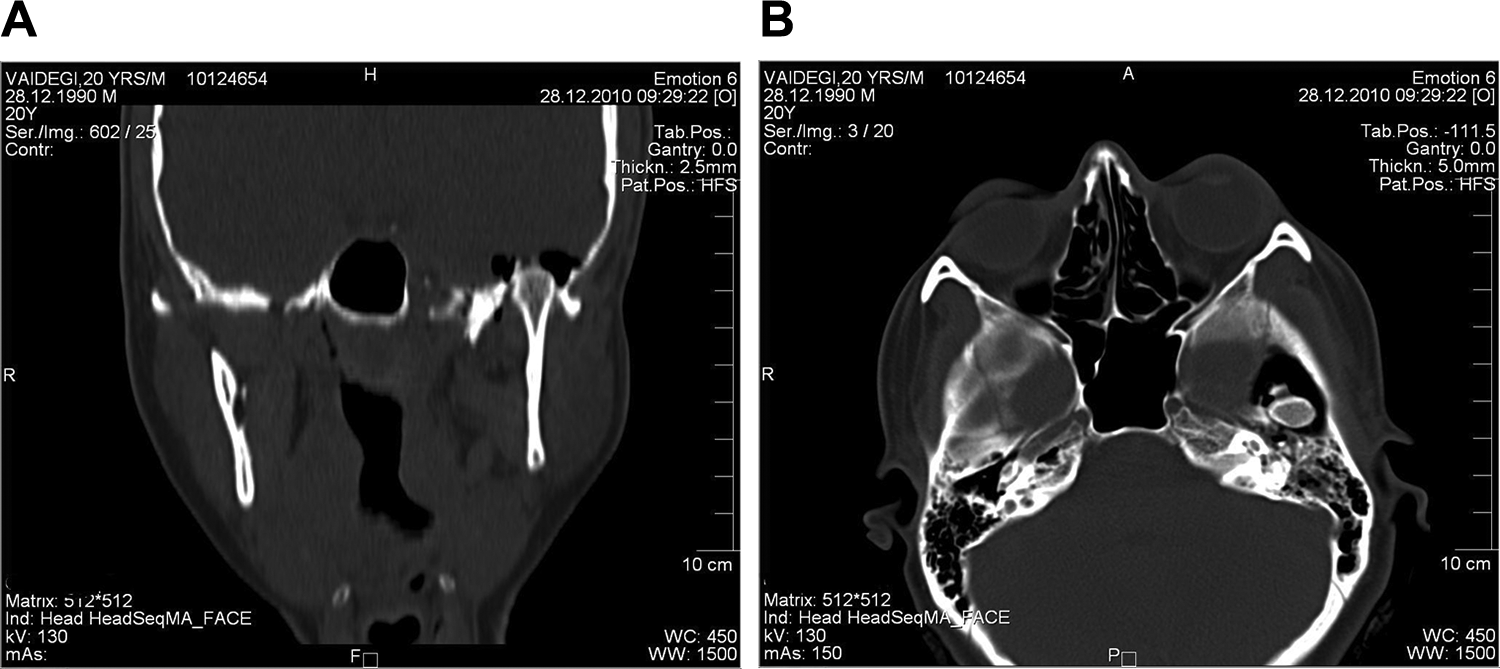
(A) Shows central dislocation of the left mandibular condyle into the middle cranial fossa with surrounding pneumocephalus. (B) Anteromedial dislocation of the fractured segment of the glenoid fossa is also seen.
Since mouth opening was restricted, fiberoptic nasal intubation was done and closed reduction attempted under general anesthesia. Manual reduction was achieved by applying pressure in the posterior aspect of the mandible. Reduction was confirmed by return of occlusion (with elimination of open bite), ease of jaw movements and palpability of the condylar heads in the preauricular area while manipulating the mandible. Mouth opening was attempted again with a Doyen’s mouth gag, the mandible was freely mobile and settling into proper occlusion confirming appropriate reduction. In the absence of any other neurological issues such as CSF leak or intracranial displacement of the bony fragments of the glenoid fossa, no craniotomy or reconstruction was planned for the fossa. Intermaxillary fixation screws were then placed.
The intermaxillary fixation (IMF) was done on the first postoperative day and retained for a period of 2 weeks. On releasing the IMF occlusion was maintained (Figure 4). She was then started on mouth opening exercises. Mouth opening improved gradually with exercises. She obtained full range of movements with a limited mouth opening of 30 mm, 2 months after her injury (Figure 5).
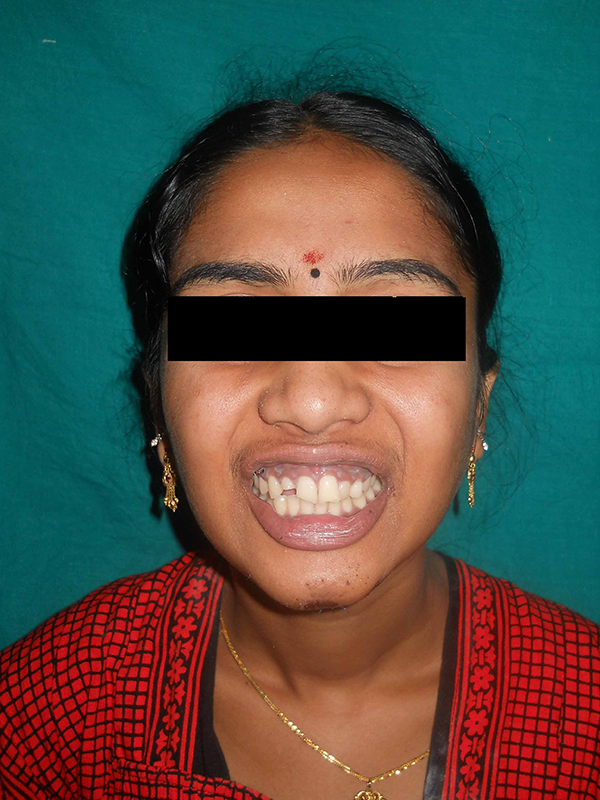
Occlusion of the patient at 2 months post reduction of the dislocation.
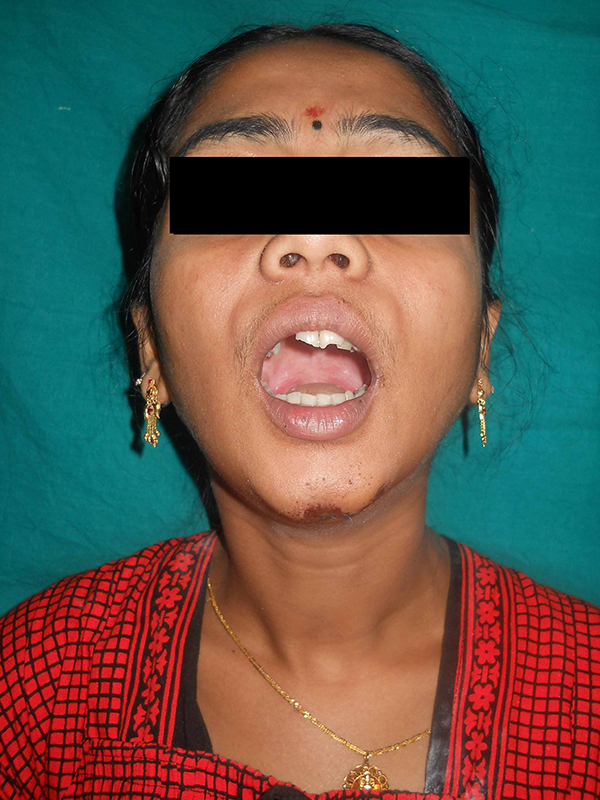
Mouth opening of 30 mm at 2 months after reduction of the dislocated condyle.
2 years later a CT scan done showed remodeling of the left condyle and ossification of the glenoid fossa (Figure 6(A) and (B)). The remodeled condyle appeared elongated in the vertical direction with the level of the condyle slightly higher than that of the right side. Mouth opening which was restricted returned to 25 mm with therapy. There was a deviation of the jaw to the left on opening. An orthopantomogram done at 7 years shows thickened condyle with flattening of the anterior slope of the left condyle (Figure 7).
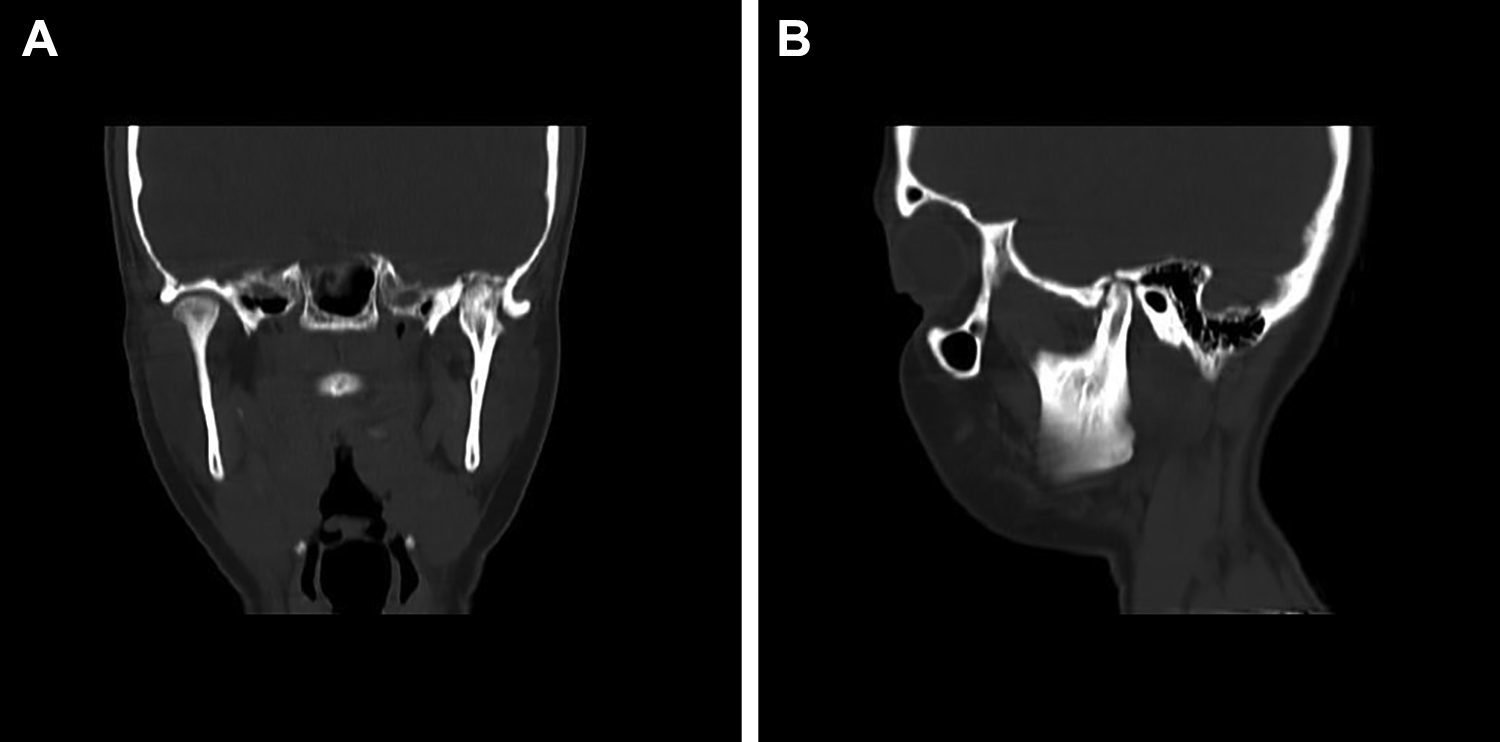
(A) CT scan sections taken 2 years later show a remodeled vertically elongated condyle with closure of the glenoid fossa defect. (B) Sagittal view of the remodeled condyle and glenoid fossa
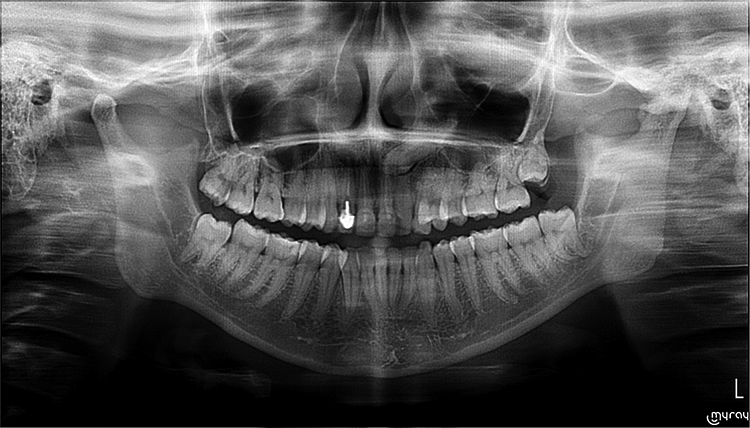
Orthopantomogram taken at 7 year review show further remodeling of the condyle with flattening of the anterior slope.
Patient continued to be asymptomatic till a few months back she developed clicking and pain in the right TMJ with restricted mouth opening. At a 10 year follow up patient presented with anterior disc displacement without reduction in the contralateral TMJ which was confirmed with an MRI scan (Figures 8(A) and 9(A)). The left condyle showed remodeling with thick sclerotic bone seen in the lateral and posterior aspect of the condyle in the CT scan (Figure 10(A) and (B)). The disk was not visible in the left condyle (Figures 8(B) and 9(B)). She was treated symptomatically and her mouth opening improved to her earlier status of 25 mm.
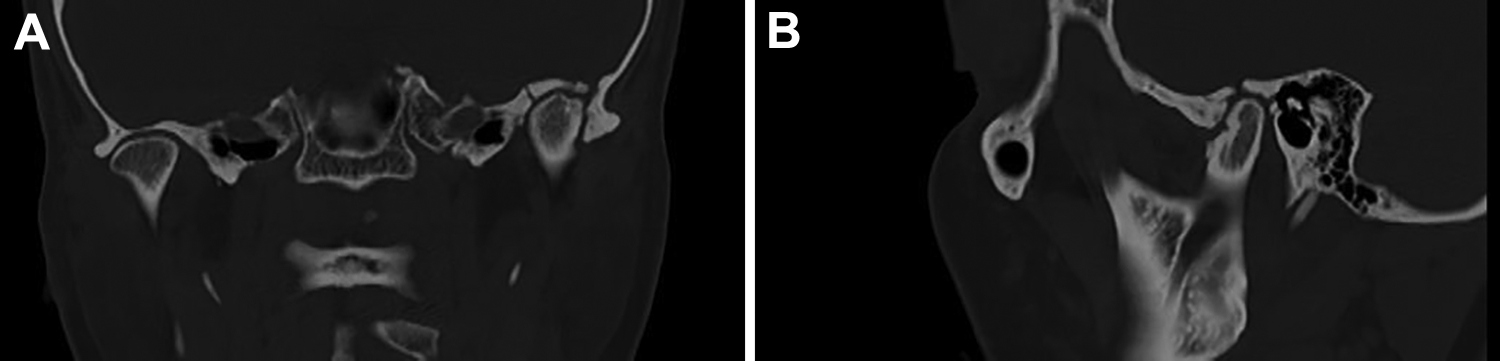
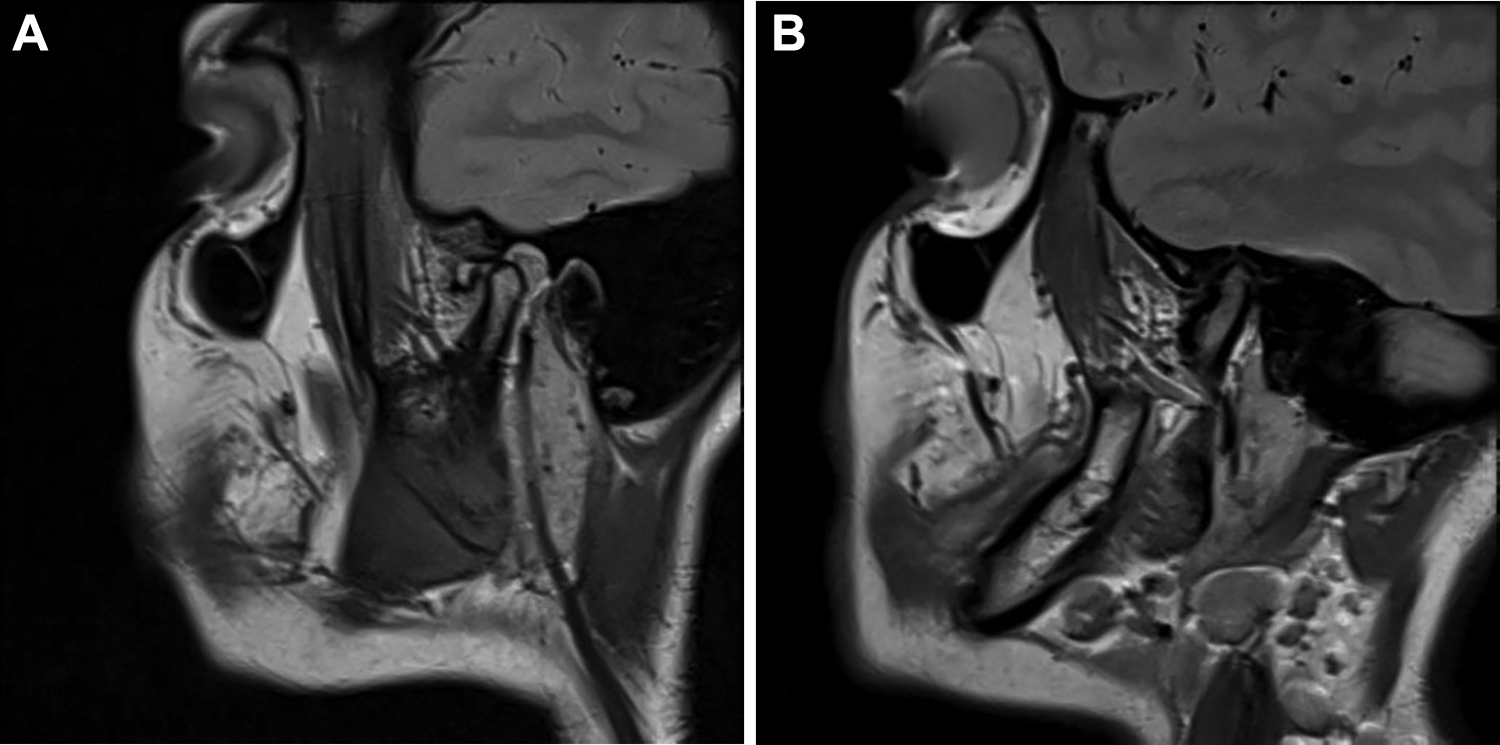
(A) MRI scan—closed mouth of the right condyle—disc positioned anteriorly. (B) MRI scan—closed mouth of the left condyle—shows reduced joint space, disc seen anteriorly as a rudimentary structure with irregularity of the superior surface of the condyle.
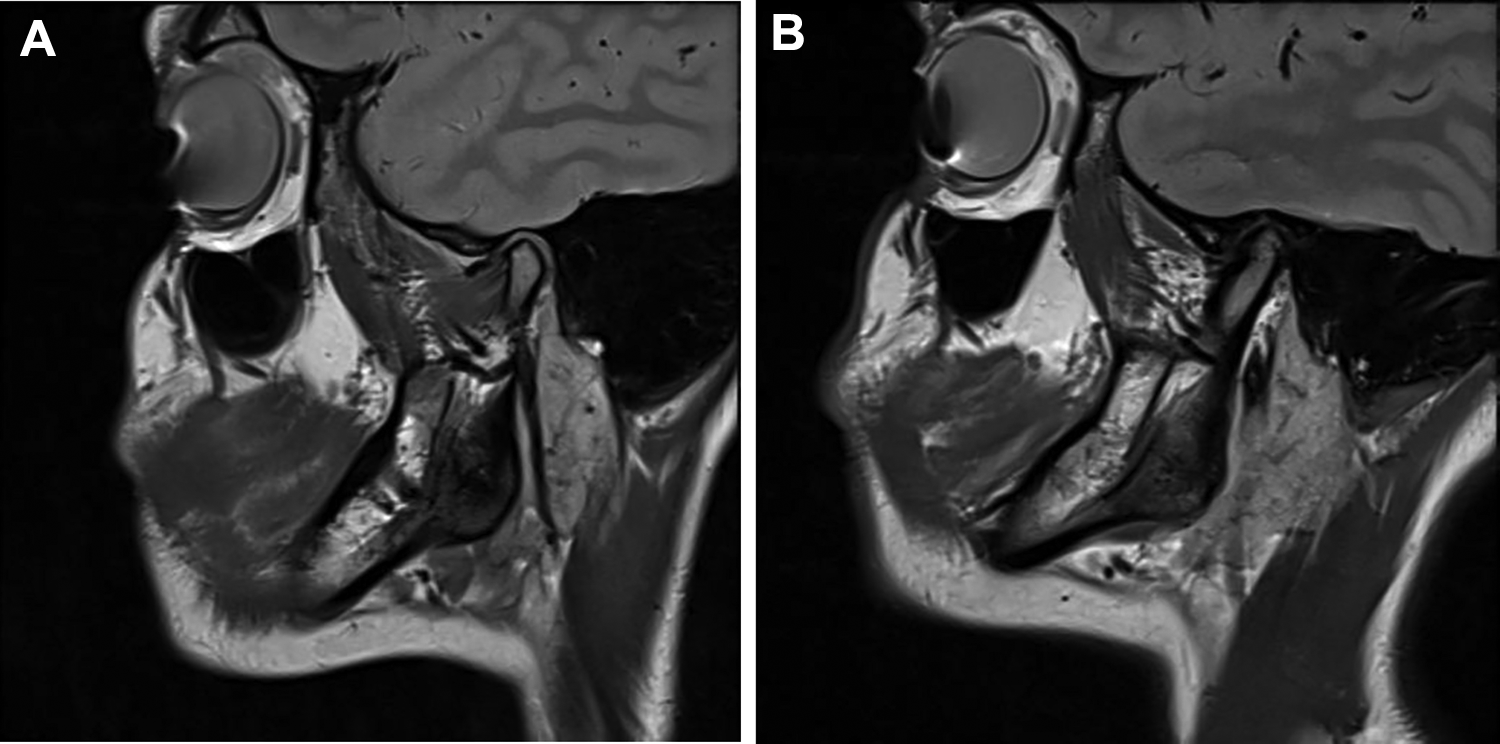
(A) MRI scan—open mouth of the right condyle—disc positioned anteriorly and not reduced on opening the mouth. (B) MRI scan—closed mouth of the left condyle—shows reduced joint space, disc seen anteriorly as a rudimentary structure with irregularity of the superior surface of the condyle.
(A) CT scan—coronal section showing sclerotic changes in the left condyle with a formed glenoid fossa. (B) CT scan—sagittal section of the left condyle showing sclerotic changes in the left condyle with a formed glenoid fossa.
Discussion
Dislocation of the condyle into the middle cranial fossa is a rare event. The latest literature review done by Monteiro reports of a total of 56 cases reported in the English literature. Why is this type of dislocation uncommon? Though various theories have been expounded, one important aspect is that such injuries are associated with high velocity trauma. In patients with injuries due to high velocity trauma either they go unnoticed when associated with other injuries 15,16,18,19 or the severity of the injury leads to mortality 12 which in turn leads to under-reporting of these cases.
Second theory was based on the shape of the condyle. It was felt that for a condyle to penetrate the middle cranial fossa it had to be small and rounded. The shape of fully formed condyle is mostly that of a scroll with well-developed medial and lateral poles. A study done by Yale et al on condylar shapes, classified condyles into 4 types. He found that most common shape is a scroll shaped condyle with a superior convex surface—radius of curvature greater than one half the axial length (46.3%). The least common shape was that of a rounded condyle accounting for only 2.8%. 20 This could also explain as to why such cases are rare. Whitacre was the first to point out about this anatomical variance of the condyle in his case. 5
A condyle with thin neck dissipates the forces directed superiorly thereby reducing the injury to the skull and brain. Children and young adults have a more rounded condyle with thick necks which fail to fracture but rather dislocate. 6 Hence the increased incidence in children and young adults. 69% of the reported cases were females with the right condyle affected more than the left condyle. 3 A study was done by Al-Koshab et al using CBCT to assess the morphology of 200 glenoid fossa and condyles in 100 subjects. According to the study there was no significant difference in terms of thickness of the glenoid fossa between genders, but the condylar volume, width and height in males were larger than in females. 21 This was also confirmed by studies done by Honda et al. The condylar volume, length, and width however were significantly larger on the right side while height and thickness of the roof of the glenoid fossa were significantly larger on the left side. 22
Steinhauser did a cadaveric study that proved that the central part of the glenoid fossa is the weakest part of the skull base. The lateral aspect of the glenoid fossa is thick and buttressed by the root of the zygoma. In a normal scroll shaped condyle, the lateral and medial elevated margins of the glenoid fossa meet the medial and lateral pole of the mandibular condyle on impact. But in case of a rounded condyle, it was assumed that the articular surface came into direct contact with the central part of the glenoid fossa. 6 And according to Da Fonseca a rounded condyle creates a higher pressure onto the glenoid fossa when compared to a scroll shaped condyle causing fracture of the glenoid fossa and dislocation of the condyle. 20 Other reasons speculated for dislocation include lack of posterior occlusion and increased pneumatization of the temporal bone 7,10,23
The common finding was the laceration on the chin indicating fall on the chin. On presentation, the patients have trismus, laterognathism, posterior cross bite and anterior open bite. Very rarely do they present with head injury findings. These clinical signs are very similar to that of condylar fractures or internal derangement of the TMJ, hence are easily missed in the due process of examination and treatment. 10 21 out of 43 cases were not diagnosed on the first examination. 2 Conventional radiographs also fail to pick up these fractures easily and this is evident in the literature with many of the cases being diagnosed after primary treatment. 6,11,14,19 It must also be noted that with the absence of neurological injuries, CT scans were not taken as a primary investigational modality. Hence it is mandatory that a CT scan is done as a routine, so as to not only diagnose a condylar dislocation but also to rule out intra cranial injuries. The 1977 article by Kallal et al gives the first mention of a CT scan performed to diagnosis Intracranial dislocation. 12
Only 6 cases of dural lesions were seen 2 There was no mention of meningitis as a complication in any of these patients. However if there is CSF leak or evidence of meningitis, administration of appropriate antibiotics crossing the blood brain barrier is mandatory. As per CDC recommendation (Atlanta, USA) vaccines are very effective to prevent and control bacterial meningitis, hence appropriate use of such vaccines may be optimal in such instances. 24
Although most of the articles talked about the close proximity of the middle meningeal artery to the glenoid fossa, there was only 1 reported case of bleeding from the middle meningeal artery.
Another important finding from literature reviews point out to the fact that it was an intact condyle that was dislocated into the middle cranial fossa. Rarely was the involved condyle fractured. Only 6 out of 43 cases of intracranial dislocation was associate with a fracture. 2 Some common associated mandibular fractures were symphysis and contralateral condylar fractures. 15
The treatment goals are aimed at reducing the condyle into its functional position, restoring cranial shape thus separating the middle cranial fossa from the temporomandibular joint, restoration of stable occlusion, and preventing secondary neurologic complications. If not treated, the joint gets ankylosed. 17,25,26
It is not possible to reduce this dislocation under the action of muscle relaxants or neuro muscular blocking agents as the obstruction to mouth opening is a mechanical problem. 1 Historically treatment began with exposure of the dislocated condyle and resection of the fragment within the middle cranial fossa 11,16,23,27,28 or a sub condylar osteotomy leaving behind the dislocated head of the condyle thereby creating a barrier between the middle cranial fossa and glenoid cavity. 4,14 In both instances the dislocation was identified late. This was mainly due to the fear of causing intra cranial lesions during manipulation. Subsequently closed or open reduction of the condyle was done by downward pressure either manually or with wire traction in the angle ramus region. 2,5 –8,10,12,13,29 –31 Surgery was always followed up with a minimum of 2 weeks of intermaxillary fixation followed by physical therapy. Physical therapy was essential to prevent ankylosis. According to De Fabianis, in children, functional therapy was aimed at restoring posterior facial height, getting good occlusion and function.
The glenoid fossa when reconstructed was done using various materials ranging from bone grafts to silastic sheets and titanium plates. 2,15,23,30,32 –36 The glenoid fossa reconstruction is important in order to prevent redislocation. Fascia lata to temporalis fascia and muscle was used as interposition material between the new glenoid fossa and articular surface. Placing an interpositional material may help prevent degenerative changes and prevent ankylosis. 37 The use of an interpositional material depended upon the severity of displacement of the fracture and damage to the glenoid fossa. 6 Thus treatment of this injury is patient specific taking into account various factors such as time gap between injury and treatment, growth potential of the patient, degree of glenoid fracture, risk of additional intracranial injuries, restoration of posterior facial height and restoration of function and the risk for ankylosis. 15
Dislocations diagnosed immediately within 2 weeks of trauma was treated by closed reduction and 2 weeks of intermaxillary fixation. In our case we were able to diagnosis and treat the patient on the same day of trauma. When diagnosed beyond 2 weeks, conservative treatment failed because of muscle spasm, shortening and subsequent fibrosis of temporalis and pterygoid muscles, hence the need for open reduction. Closed reduction was recommended as treatment in growing children in order not to disturb the mandibular growth. 1,38 Closed reduction was avoided in fracture dislocations because of the difficulty in reduction. Arthroplasty procedures were done in cases with risk for high threatening intracranial lesions during manipulation.
The articular disk was seen in the cases where open reduction was done. Disk was ruptured and displaced 19,23,30,32,35 Although the articular disk was repositioned it did not help in preventing deviation while opening or remodeling of the condyle. However some have reported incidence of ankylosis (4 cases reported) even after open reduction especially in cases with delayed intervention. This could be due to inadequate condylar mobility due to loss of lateral pterygoid attachment. 1,16 Hence stressing on the need for long term follow up.
The follow up period of the cases varied from 6 months to 5 1/2 years. The common follow up finding was ipsilateral deviation of the jaw while opening. Remodeling of the condyle with flattening of the articular surface was seen in follow up radiographs and CT scans. In our patient we noted similar changes of remodeling in the condyle with flattening of the articular surface with increased sclerotic changes seen in the involved condyle on the posterior and lateral aspect with absence of the disc. Even in the absence of a normal disk and sclerosis of the condylar head, she had adequate jaw movement and function with occasional discomfort. Should the mouth opening reduce considerably with severe pain and degeneration of the TMJ, a total joint replacement may be an option. Long term follow up (10 years later) revealed TMJ dysfunction—anterior disc displacement without reduction on the contralateral side. It is difficult to say with certainty if this is a sequalae to the trauma or a de novo problem.
Conclusion
Intact central (middle cranial fossa) condylar dislocations though rare maybe be associated with short, rounded condylar necks. Early diagnosis of such dislocations can be successfully managed by reduction alone under anesthesia. Prompt diagnosis also helps in obviating the need for extensive surgical procedures. Though the disc may get damaged during the injury, the condyle remodels and helps in maintaining function thus reducing chances of ankylosis. Considering the changes observed in the affected condyle, it is mandatory to review these patients long term. The issue of TMJ dysfunction of the contralateral side over a long term cannot be said with certainty based on a single case. This presentation helps one in appreciating the importance of early diagnosis, prompt management when encountering such a case along with understanding the condylar changes over a 10 year period.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
