Abstract
Traumatic injury and pathological palatal defects can present a challenge in both acute care and clinical settings. Due to the vascularity of the maxillary region, thin mucosa, and difficulty of isolated stabilization, effective management and treatment planning are paramount to long-term patient outcomes. Palatal and dentoalveolar splinting has been widely used to manage palatal defects both intraoperatively and postsurgically with acrylic or polyvinyl chloride vacuum form materials as the basis for splint fabrication. We propose a method for palatal stabilization and hemorrhage control through the use of thermoplastic splinting material.
Traumatic injury and pathological palatal defects can present a challenge in both acute care and clinical settings. 1 Due to the vascularity of the maxillary region, thin mucosa, and difficulty of isolated stabilization, effective management and treatment planning are paramount to long-term patient outcomes. 2 In addition, managing postsurgical palatal defects presents a challenge due to constant tongue movement and leverage against the palate during swallowing, mastication, and phonation (Figure 1).
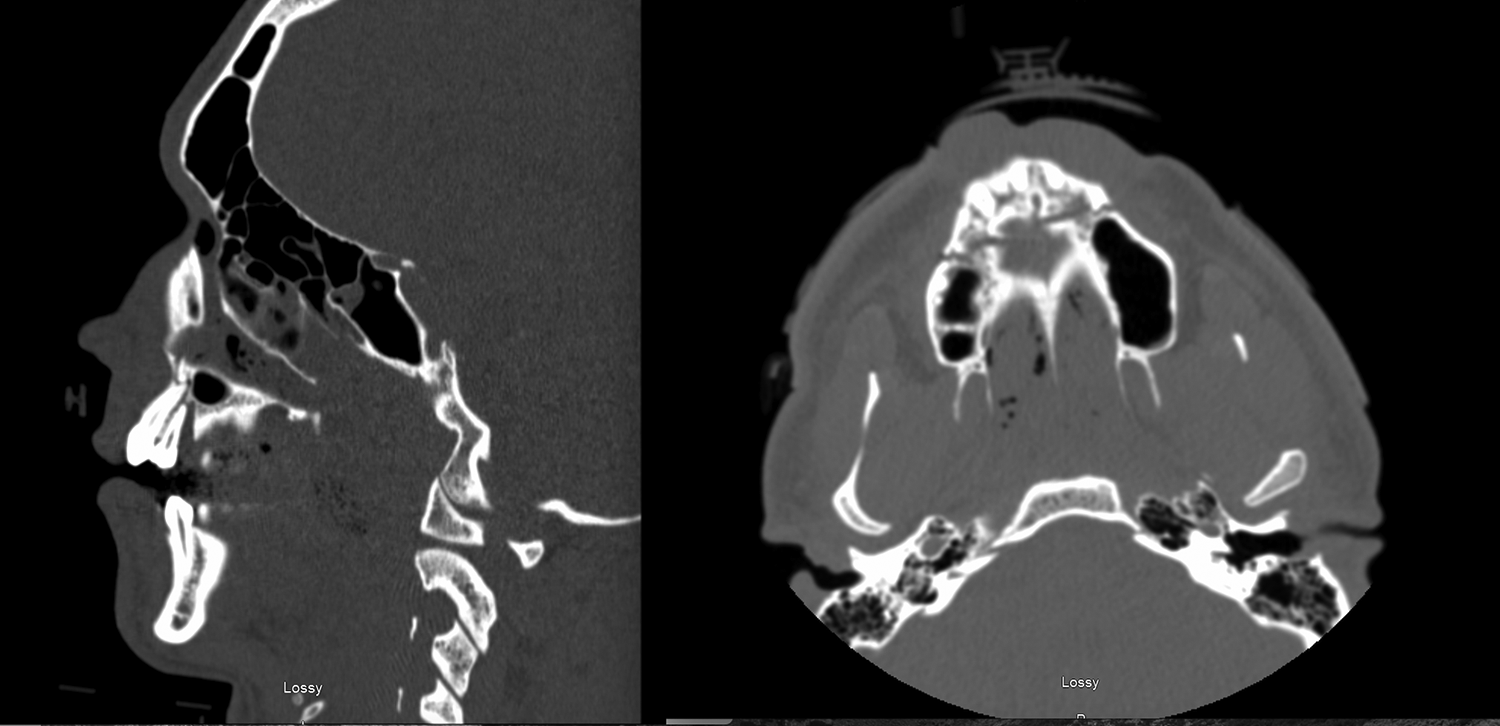
CT imaging demonstrates a transverse palatal fracture sustained after blunt head trauma. CT indicates sagittal and axial sections of the anterior palate.
Palatal splinting has been widely used to manage palatal defects both intraoperatively and postsurgically with acrylic or polyvinyl chloride vacuum form materials as the basis for splint fabrication. 3 Fabrication requires taking alginate impressions and stone-model casting before the splint can be delivered to the patient. It has been observed clinically that splint materials can result in a stagnant environment conducive to food debris and plaque accumulation, impeding wound healing.
Management of palatal defects in pediatric patients imposes additional challenges. Palatal trauma is common in children due to the tendency to place objects in the oral cavity combined with an unsteady gait. Furthermore, an increased gag-reflex sensitivity and the intolerance of applying gauze pressure for extended periods of time limit the options for hemorrhage management. The dollar cost in the community care, morbidity of delayed hemostasis of palatal bleeding in pediatric patients can often increase the risk of aspiration and can result in intubation, thus prolonging their hospital stay in this commonly known traumatic event. 4
Design
We propose a method for palatal stabilization and hemorrhage control using thermoplastic splinting material (Figure 2). This material has been widely used in the context of nasal reconstruction and orthopedic fractures. Thermoplastic splinting material allows for immediate anatomical molding immobilization without the need for presurgical preparations, including impressions and model casting (Figure 3). This offers a novel alternative in the acute care setting of palatal or maxillary hemorrhage, fracture, and postsurgical management. 2 The material provides hemorrhage control and does not require immediate wiring or screw fixation—as the splint material easily engages with inter-arch undercuts or via splint intaglio surface adherence to soft tissues (Figure 4). This provides a short-term, hemorrhage control technique that can be stabilized with wiring or screws if needed in the clinic or operating theater at a later time (Figure 5). Thermoplastic splinting material is lightweight, latex-free, and can be made available in an antimicrobial formulation. In addition, perforations and decreased bulk of the material create a breathable environment to allow observation if any further hemorrhage, air to circulate around the injury, prevent debris accumulation, and allows for adequate drainage. 5

The thermoplastic splinting material is cut into the general shape of the patient’s palate. Once placed in warmed water, the material turns clear and pliable. The material remains pliable for a short time while it can be shaped to the palate.
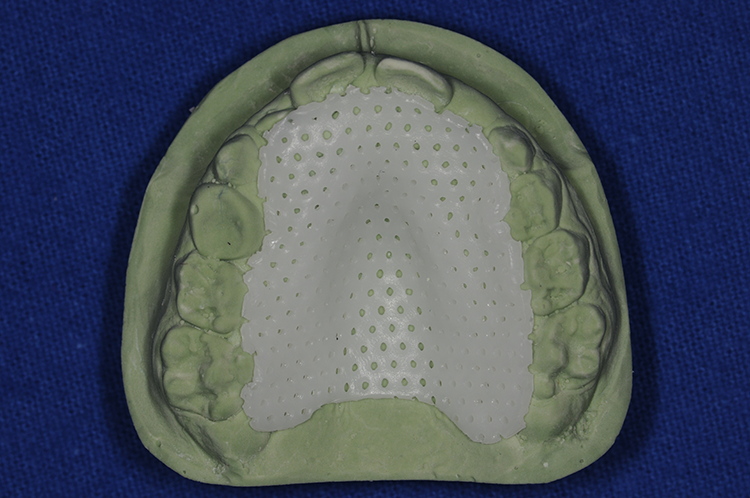
Casts were used for demonstration purposes only, with the formed palatal splint intimately formed to the patient’s palate. The ease of preparation and adaptiveness of the thermoplastic material allows for direct application without the need for impressions and casts.
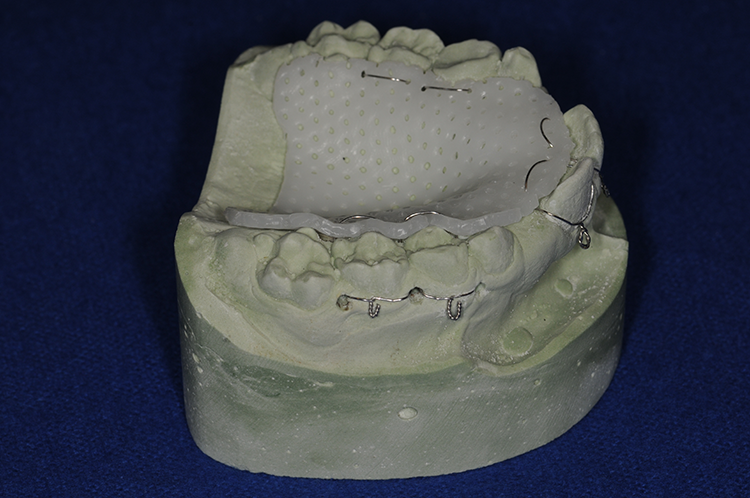
If long-term palatal stabilization is required, the pores of thermoplastic splint allow for circumdental wire stabilization. This is particularly useful in palatal fractures from high-impact trauma. Porous characteristics of the splint also provide adequate drainage of fluids and circulation of air around the wound in the instance of palatal grafts.
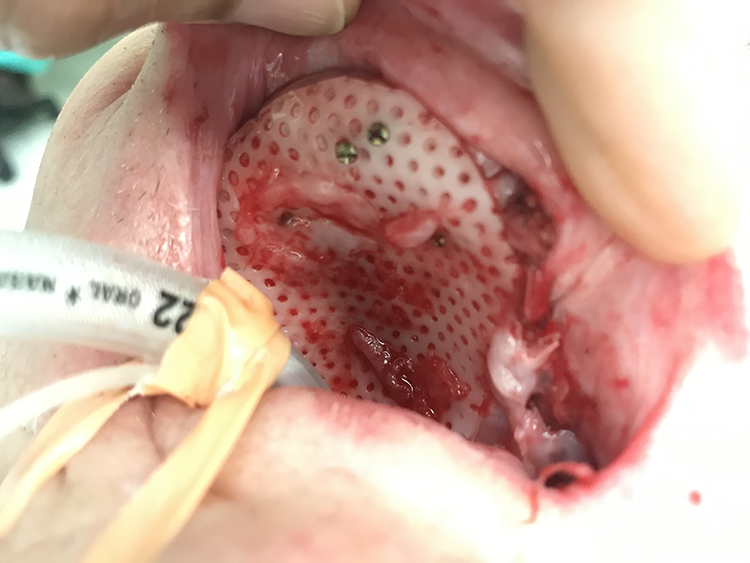
Photograph of a patient with palatal and maxillary stabilization using screws and thermoplastic splint material. Wires or screws can be utilized to achieve reduction and stabilization of maxillary and palatal segments.
Construction
The thermoplastic material is cut into the general shape and size of the patient’s hard palate or alveolus. Placed under heated water for a short duration of time, the material becomes pliable and easily adaptive. The plastic maintains an appropriate thickness with minimal material expansion and maintains pliability and functionality when contacted with oral secretions. This makes the material an ideal option for real-time splint fabrication. Following adaptation of the material to the hard palate and cooling of the material, the splint can be removed and modified as needed. Retention and stability are noted upon splint placement, and subsequent hemostasis is achieved. Additionally, fibrin glue or cellulose-based hemostatic agents can be inserted under or through the perforated splint.
The strength of the material and existing perforations allow the plastic to maintain its durability in combination with wire and/or screw fixation of the splint. This is particularly useful in fractures following high-impact trauma and can be completed under local anesthesia, if indicated. The splint is easily adapted for closed approximation and reduction of multiple maxillary or palatal fragments and can be secured to the maxilla, palate, or alveolar segments with screw or wire utilizing the splint perforations. Perforations provide an additional benefit of adequate fluid drainage and circulation around the wound, enhancing healing of palatal graft techniques. The splint is effective for short-term stabilization and reduction of palatal and maxillary segments. This splint technique can be utilized for adult and pediatric patients and has been used successfully in clinical practice without requiring subsequent long-term splint replacements.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Statement/Confirmation of Patient’s Permission
Patient permission was obtained.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
