Abstract
Press fit fixation is becoming more popular in RSA to preserve, in theory, bone capital. Several studies report that bone resorption can be very high around humeral stems depending on their size, shape and mode of fixation. The aim of the current study is to mid-term follow-up clinical and radiological result of a press fit ovoid regular stem RSA in non acute trauma cases.
Materials and Methods
We performed a retrospective monocentric study of patients continuously implanted with the Humeris® stem RSA for degenerative change of the shoulder. Nineteen shoulders, in eighteen patients (74.6 y.o (from 69 to 81)), were available at minimum five years follow-up.
Results
The mean final adjusted Constant score was 111.9 (65 to 130), and the mean ASES score was 49.82 (10 to 60). Humeral resorption was observed in 21% of cases. We found a statistically significant (p = .014) lower adjusted Constant score in patients presenting with resorption on post-operative X-rays compared to those without resorption (115.6 vs. 98.25). Half cases of patients presenting a resorption underwent L’Episcopo procedure during surgery. Humeral resorption occurs the first year after surgery and do not increase even 8 years after surgery. Analysis demonstrated no correlation between the value of filling ratios and bone resorption.
Conclusion
The current study confirms a low rate of stress shielding around the studied stem, with rare bony resorption and no osteopenia around the humeral stem. This study highlights the importance of choosing the appropriate proximal shape and length of the humeral stem for press fit fixation in RSA.
Introduction
Reverse Shoulder Arthroplasty (RSA) is commonly used to restore function and range of motion in the case of degenerative shoulder arthropathy or even in traumatology. 1 The good clinical outcomes reported in studies has dramatically increase the number of implantations and thus, potentially, the future rate of revisions. Historically, the humeral stem was cemented and this fixation technique is still very popular.2,3 Long term results demonstrate that humeral stem revision rates are very low with cemented stems in TSA.4–6 Boileau reported that in RSA, humeral stem revision is much more frequent than at the glenoid (21% vs. 13%) and is the third cause of revision after dislocation (38%) and infection (22%). 7 Press fit fixation of the humeral stem is currently widely proposed to avoid cement complications (thromboembolism, fracture, and a higher rate of acromial fractures), and to promote bone preservation, decrease operative time and facilitate revision.4–6 With revisions, the impact of cemented humeral fixation on bone preservation has led to the development of press-fit RSA humeral stems that are theoretically bone preserving. Several studies report a high rate of bone resorption after press fit fixation. 8 Furthermore, Denard et al. reported that press-fit humeral implants have varying designs that can lead to changes in stress distribution in the proximal humerus. This makes it important to follow our patients when a new design of humeral stem using press fit fixation is launched. The response of humeral bone to the stem differs from one study to another, and one explanation could be the effect of stress shielding related to the stem design of some implants. 7 Barth et al reported in a finite element study the importance of the global design of the stem on bone remodeling. 9 The aim of the current study was to analyze the clinical and radiological result of a monocentric study of patients who had an RSA implanted with a proximal ovoid HA coated Humeris® stem (Fx Solutions® Viriat, France) for non-traumatic indication with a minimum 5 years follow-up.
Materials and Methods
After IRB approval, we reviewed a consecutive cohort of patients implanted with a Humeris® RSA (Fx Solutions) (Figure 1) for degenerative changes of the shoulder (massive rotator cuff, or osteoarthritis in elderly patients) during the first three years of its availability on the European market (2014-2015-2016). The current stem is not indicated for treatment of acute trauma.

Humeris ® is a press fit, ovoid, stem that can be used for anatomic and reverse shoulder arthroplasty. An asymmetric 135/145 polyethylene / metal backed humeral cup allows to have a 145° cervico-diaphysal angle even with an anatomic cut of the humeral head.
All patients had a minimum 5 years follow up. During this period, thirty-seven patients were eligible for analysis. Seven (7) patients died before five years follow-up from a cause not related to the RSA, 12 were unable to return to clinic because they had moved to a retirement home or were unable to come to clinic because of the covid 19 pandemic. Eighteen (18) patients, 19 shoulders were available for the current study.
Surgical Procedure
Surgery was performed in the beach-chair position with general anesthesia and a scalene block. Deltopectoral approach was performed, and the subscapularis muscle was not repaired in any of the cases since the glenosphere was lateralized. All patients had the same glenoid resurfacing with a glenosphere of 36 mm (n = 15) or 40 mm (n = 4) in size, impacted and screwed to a 24 mm diameter baseplate. This hydroxyapatite (HA) coated baseplate was secured to the glenoid by a central peg coated with hydroxyapatite (HA) and one to four compression screws or locking screws. The Humeris® implant (sizes 8 (n = 2), 10 (n = 6), 12 (n = 8), 14 (n = 3)) was used in all cases using an asymmetric 135°/145° humeral cup (ultra-high molecular polyethylene UHMWPE and metal back) in + 3 (n = 16) and + 6 (n = 3)) sizes (Figure 1). The implant was put in place respecting the native retroversion of the humerus. This was possible because the Humeris® Shoulder is a system of shoulder components that can be used in either an anatomic or a reverse configuration. It is manufactured from Ti-6Al-4V alloy conforming to ISO 5832-3 and is available in diameters of 8–16 mm and a length of 100 mm. The distal end of the humeral stem is trapezoidal with a polished surface. The proximal portion of the humeral stem is ovoid with a plasma sprayed commercially pure Titanium (CP Ti) and hydroxyapatite (HA) coating. Two patients who had a dropping sign and negative active external rotation pre-operatively had a latissimus dorsi tendon transfer described by Boileau as l’Episcopo procedure. 10
Clinical evaluation was based on the Constant and ASES score. Radiological assessment was completed immediately post-operatively and at intermediate and maximum follow-up post-operative with anteroposterior (AP) and lateral shoulder X-Rays reviewed by 2 independent reviewers (S.C and G.N). On immediate post-operative X-Rays, the main radiological parameter evaluated was the filling ratio (FR), as determined with the method described by Schnetzke. 11 On AP views, the humeral shaft axis (HSA) was identified and two perpendicular lines to the HSA were drawn. The proximal line intersected the prosthesis on the medial edge of the humeral baseplate (Figure 2).

Measurements of the filling ratio on AP (proximal and distal) and lateral (distal) X-Rays. The blue line materializes the shaft axis (SA) of the humerus. At the level of the humeral baseplate and at the level of the junction between the second and the distal third of the stem, two lines are drawn perpendicular to the SA. The green lines illustrate the measurements of the stem width, and the red lines illustrate the measurements of the endocortical width. The filling ratio is calculated by dividing at each level the stem width by the endocortical width.
The distal line intersected the prosthesis at the junction between the second and the distal third of the humeral stem. At the two intersection points, the width of the prosthesis was measured and normalized to the endocortical bone width to obtain a metaphyseal (FRm) and a diaphyseal (AP-FRd) filling ratio. The measurement process was repeated on lateral views to assess the diaphyseal (L-FRd) filling ratio. Finally on immediate post-operative X-Rays, the contact between the prosthesis and the humeral cortex on AP or lateral views was recorded. On the latest X-Rays, the measurement was performed to evaluate the modification of the FR over the post-operative follow-up. Glenoid notching was evaluated and rated according to the Sirveaux classification.12,13 Migration, stress shielding or cortical bone resorption around the stem were identified and located according to Inoue's description. 14 Increase of the FR throughout the post-operative follow-up was determined to be resorption of the medial central cortical bone, decrease of the FR as loosening around the stem.
Statistical Analysis
Continuous quantitative variables were described by mean and standard deviation (SD). Dichotomous variables were described by their number of events and their percentage. Fisher's exact test and Wilcoxon rank sum test were used for categorical and continuous variables. The threshold of significance retained was 5% for a power of 80% and a risk of the first species at 5%. All tests were 2-sided. The R software (version 3.5.0) was used to perform the statistical analyzes.
Results
Eighteen (18) patients, 19 shoulders, were include in the present study. Mean age at surgery was 74.6 years of age (range 69 to 81), with 14 women and 4 men. No trauma cases were included as specified in the inclusion criteria.
Clinical Results
The minimum follow-up was 72 months, with mean follow-up of 76 (range 72 to 93) months. At longest follow-up, the mean global post-operative raw Constant Score was 74.82 (range 41 to 90); the adjusted Constant score was 111.9 (range 65 to 130), and the mean ASES score was 49.82 (range 10 to 60). We found a statistically significant (p = .014) lower adjusted Constant score in patients presenting with resorption on post-operative X-rays compared to those without resorption, mean 115.6 (range 107.6 to 130.8) versus mean 98.25 (range 72.65 to 108.4) respectively. (Table 1)
Correlation Between the Constant Score and the Radiological status: Resorption is Statistically Correlated to Lower Constant Score.

Complications and Revision
One patient had a traumatic dislocation of the RSA two years after initial surgery. During the revision, the +3 mm humeral cup was replaced with a thicker polyethylene +9 mm. At 3 years follow-up post revision the patient had no new episodes of dislocation with an adjusted Constant score of 117 and ASES score of 60. One patient had a post-operative dislocation of the glenosphere from the baseplate 4 weeks after initial surgery. Immediate revision surgery was performed. Seventy-six (76) months after revision, the patient had no further complications and an Adjusted Constant score of 110 and ASES score of 60.
Radiological Evaluation
On immediate post-operative AP views, the mean FR at the metaphysis (FRm) was 0.77 (range 0.65 to 0.93), 0.79 (range 0.62 to 0.0.93) at the distal part (FRd) was and 0.86 (range 0.65 to 1) on the distal part of the profile (Table 2).
Comparison of Filling Ratio pre-Operative to minimum 5 Years Post-Operative.

We identified a cortical contact between the stem and the humerus in 15 cases (79%). At maximum follow-up, humeral resorption was seen in 21% of cases (4 patients). In 2 of those cases this image of resorption was also seen at intermediate follow-up, 1 years after surgery, and was located at the place of suturing for the two cases of latissimus tendon transfer during l’Episcopo procedure. (Figure 3). This image does not change over the 7 years post-operative follow-up of the RSA. Other patient didn't show any resorption at 8 years post op. (Figure 4)
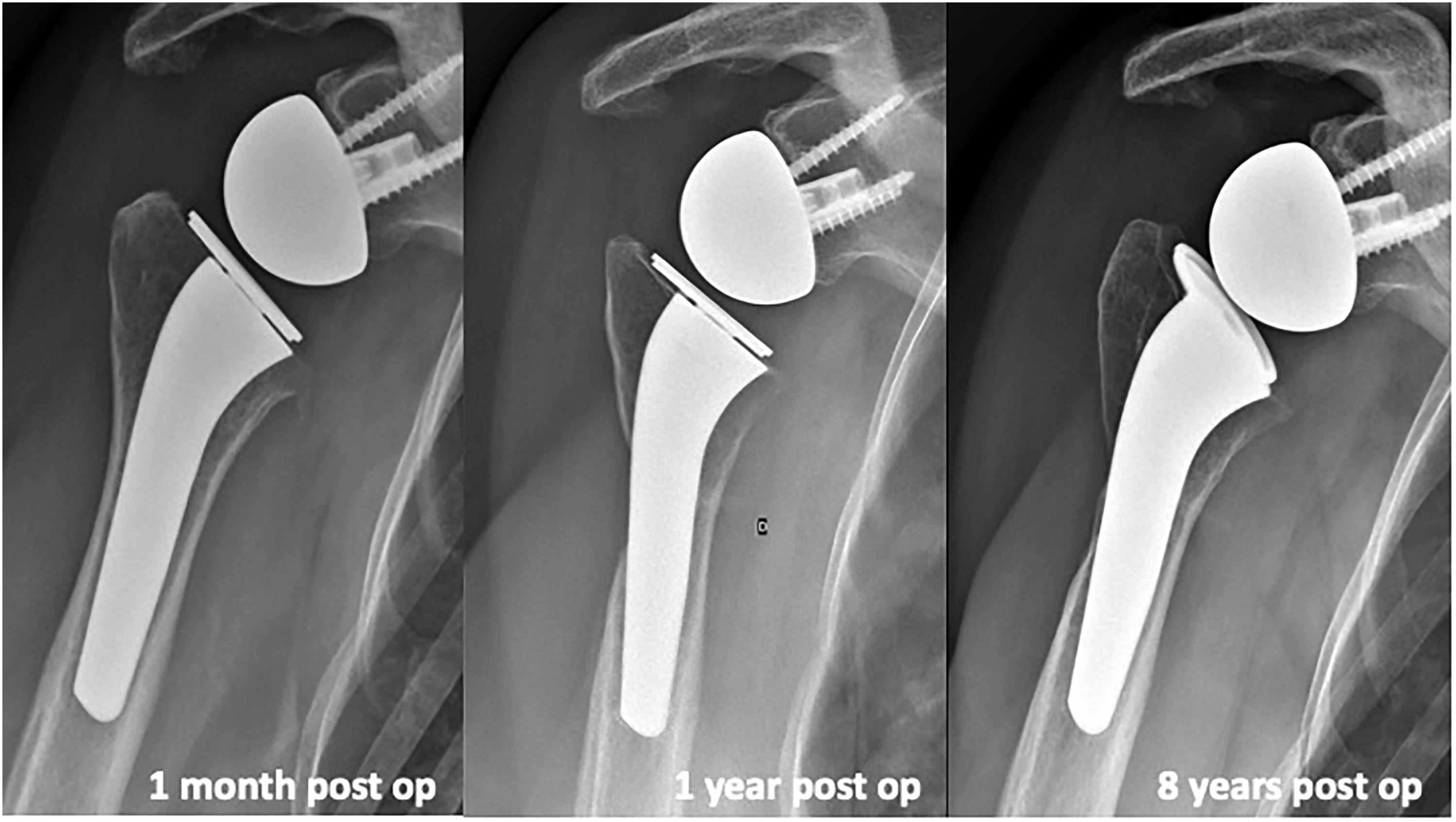
Xray AP view at 1 month, 1 year and 8 years after RSA. Resorption appears at 1 year, at the location of the latissimus dorsi tendon transfer. No progression of the resorption occurs over time.

Xray AP view at 1 month, 1 year and 8 years after RSA. No resorption appears over time. Distal filling ratio changes but no impact is seen on proximal aspect of the humerus.
One resorption was located in Zone 1, 2 in zone 2 (LD tendon transfer), 1 in zone 7. The FR changed with time but without significant difference compared to initial data, (Tables 3 and 4). Analysis demonstrated no correlation between the value of any FR and bone resorption. No patient presented with osteopenia. In summary we identifyed 4 cases of cortical resorption in wich 2 cases had Lat Dorsi transfer. There was no correlation witt the distal or proximal FR nor contact with corticals.
Table Showing the Evolution of the Filling Ration and Resorption Through Time at minimum 5 Years Follow up.

Box Plot Showing the Change in the Filling Ratio Over Time pre-Operative to minimum 5 Years Follow-up.

Index of resorption can be defined by analysis for final filling ratio / initial filling ration. For value 1 = no change occurs between pre-operative to final post-operative. Value over 1 = increase of FR = bony increase resorption, Value < 1 = decrease over time = bony resorption. The current graph shows very low index of resorption.
Only 4 patients presented with resorption of the proximal humerus, but only 1 had partial resorption of the tuberosity. Glenoid notching was observed in 2 cases (6%). According to Sirveaux's classification, 12 glenoid lesions were observed in zone 1.
Discussion
The current study reports good clinical outcomes of RSA with a humeral press fit fixation stem comparable to those reported in the literature.1,2 Clinical results are comparable to those reported in the literature for non trauma cases.1,2 On one hand, we found good clinical outcomes based on Constant score but lower results for ASES score. This could be related to the aged population, with low functional demand. On the other hand we identified a correlation between resorption and worst clinical outcomes. But patient who had resorption also had in half case a latissimus dorsi tendon transfert during surgery for a worth clinical presentation before surgery. This study demonstrates that stress shielding is less frequent with the current design as the global resorption rate is lower than other studies exploring this topic. There are several factors that impact stress shielding. In modern RSA, Denard et al highlight the importance of the stem design in in relation to stress shielding. 8 One element of the design is the length of the stem. The current stem is 100 mm long for all sizes and diameters. It is considered by the authors to be at the junction between short and standard stems. This could be one reason for the specific radiological finding in this study. Resorption of the tuberosities is more common with longer stems, 6 and osteopenia around the stem is more frequently reported in short stems. 8 A stem length of 100 mm could be a good compromise between long and short stems to minimize the risk of resorption.
Raiss et al. reported that a filling ratio superior to 0.7 is detrimental for stress shielding, but we did not confirm this hypothesis. 15 This is probably related also to the design of the stem. Boileau reports results of long stems and stems around 100 mm and suggests that these shorter stems had less proximal resorption due to the shorter distal fixation. 7 In our study, we didn't observed correlation between the filling ratio and resorption of the bone. One explanation should be the trapezoid distal shape of the studied stem, the proximal ovoid shape, or even the limited number of cases in our study.
The proximal ovoid design of the stem can also induce a better distribution of forces as proposed by Bath et al. 9 Authors suggest in a finite element study that, for shorter stems, the angular design increased the physiologic bone stresses at the proximal section by 39–42%, while the oval and semi-angular designs reduced them by 5–9% and 8–13%, respectively. Our study confirms the low incidence of stress shielding by the specific design of the stem.
Contrary to previous studies we found a correlating factor with the bony resorption around the stem. It is possible to discuss this causality link because there were 2 cases of resorption in zone 2 in the 2 patients who sustained L’Episcopo procedure during surgery in this study. Those patients had more extensive surgeries than others, for worse initial clinical conditions. Unfortunately, we were unable to collect the pre-operative Constant score to evaluate the progression of the score in these patients.
The current study tends to suggest that stress shielding does not progress with time as evidenced in our 4 cases where resorption was seen at 1 year follow-up and did not increase over time to last follow-up (Figures 3 and 4).
Several publications emphasize the crucial role of the design of the stem when choosing press fit fixation. At 2 years follow-up, Denard et al reported the results of a rectangular stem. The humeral component was designed for press-fit fixation with a medial-lateral taper and proximal calcium phosphate coating. 16 The proximal shape of the stem was rectangular at the level of the tuberosity and the calcar. Calcar osteolysis was reported in 43% of press-fit and 58% of cemented stems. Proximal lateral stress shielding was more common in the press-fit group (68%) than in the cemented group (25%) with significant difference. Adaptive changes were considered low in 97% of press-fit stems, and there were no cases of tuberosity resorption at this follow up. Authors didn't report any case of loosening of the humeral component. Inoue et al reported at a mean 34 month follow-up, a bone resorption in 85.7% of uncemented TSA. 14 Authors reported also full-thickness cortical bone resorption occurred in 18.4% of cases. They noted that bone resorption was frequently observed at the greater tuberosity, lateral diaphysis, and calcar region (zones 1, 2, and 7). It is interesting to note that Inoue et al analyzed several types of stems from several companies for anatomic and reverse arthroplasties, none with an ovoid proximal shape and most of them were long stems. Mazalayrat et al reported the results of long stem design at longer follow-up. 6 Authors reported 60% of tuberosity resorption in press fit design versus 30% for cemented stem. They concluded that the tuberosity resorption rate was two times higher in the cementless stem group (59%) than in the cemented stem group (30%) (p < .001). In the same paper, authors reported that scapular notching was often found in shoulders that had tuberosity resorption. In the cementless stem group, stage 3 scapular notching was more likely to occur in the presence of tuberosity resorption and in the cementless stem group, osteopenia was more common in shoulders with tuberosity resorption. In this study, at a mean 72-month follow-up, we found a lower bony impact with the current stem design.
Bias and Limits
As a retrospective study, some patients refused to participate or did not return at minimum 5 years follow-up. The current study does not include trauma cases, which are a common cause of RSA. We chose to exclude trauma cases because the non-healing rate of tuberosities is high. The focus of this study was on humeral stem design for arthroplasties for degenerative shoulders. It is highly possible that trauma cases would have confounded the results by reporting a higher rate of resorption of the tuberosities that cannot be directly related to humeral stem design. The number of patients in this study is limited, but a benefit is that it is a monocentric study with consecutive patient selection and consistent surgical technique.
Conclusion
The current study confirms the good clinical results reported by RSA in management of degenerative changes of the shoulder. It reports a low rate of stress shielding around the stem, with rare bony resorption and no osteopenia around the humeral stem. This radiological data confirms several studies that suggest that the ovoid shape of the proximal part of the stem around 100 mm long allows a good distribution of the forces around the stem. This study highlights the importance of choosing the appropriate proximal shape and length of the humeral stem for non-cemented fixation in RSA and that any new design of stem needs to be radiologically evaluated. In our study radiologic changes occurred in the year following the implantation and do not seem to progress over time.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Geoffroy Nourissat and Howard Harris are consultant for FX Shoulder solution
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.

