Abstract
Background
Uterine rupture in an unscarred uterus is a rare but life-threatening obstetric emergency associated with high maternal morbidity and mortality.
Case Report
Mid-20s multiparous woman (P3L3) developed uterine rupture and concomitant bladder injury following an instrumental full-term vaginal delivery. The patient presented with hypovolemic shock, with severe anemia, frank hematuria, and ultrasonographic evidence of a broad ligament hematoma. Emergency laparotomy revealed extensive uterine rupture extending from the cornua to the cervix, a 3 cm posterior bladder wall tear, and massive hemoperitoneum. Peripartum hysterectomy, bladder repair, and left internal iliac artery ligation were performed. Despite aggressive resuscitation, she developed disseminated intravascular coagulation, acute kidney injury, and refractory hypotension, culminating in cardiac arrest and death 48 hours after admission.
Conclusion
This case highlights the critical importance of early recognition, timely surgical intervention, and multidisciplinary management to prevent maternal mortality in high-risk deliveries.
Keywords
Introduction
Uterine rupture and bladder injury remain catastrophic yet preventable causes of maternal mortality, particularly in low-resource settings. 1 Though rare after vaginal delivery, their occurrence reflects inadequate intrapartum monitoring, obstructed labor, and misuse of instrumental techniques such as vacuum or forceps assistance.2-4 Studies reveal that most such maternal deaths are preventable with timely diagnosis and intervention 5 and underscore the heightened risk when macrosomia, prolonged labor, or poor obstetric practices coexist.4, 6 Heightened clinical vigilance during labor and postpartum periods is essential to reduce morbidity from this devastating dual complication.
Case Report
A multiparous woman in her mid-20s (P3L3) was referred to our tertiary care center on the first postpartum day in a critical condition. She had delivered vaginally at term with instrumental assistance at an outside hospital and subsequently developed severe postpartum hemorrhage, breathlessness, and hematuria. A cervical tear was repaired at the primary facility, but her hemodynamic status worsened, prompting referral. Her first two pregnancies had been uncomplicated spontaneous vaginal deliveries, and she had no medical comorbidities. During the third labor, she experienced prolonged labor with reported excessive fundal pressure and an instrumental delivery, most likely forceps assisted, resulting in the birth of a healthy 3 kg neonate.
On arrival, the patient was severely pale, tachycardic at 160 beats per minute, hypotensive at 80/40 mmHg, and in respiratory distress, with oxygen saturation of 80% on room air, which improved to 90% on high-flow oxygen. Abdominal examination revealed distension with guarding and rigidity, raising the suspicion of intra-abdominal hemorrhage. Minimal vaginal bleeding was seen on per-speculum examination, with a cervical stitch at the 3 o’clock position, and frank hematuria was draining through the urinary catheter. Laboratory investigations revealed profound anemia (hemoglobin 5.3 g/dL), thrombocytopenia (49,000/mm³), and leukocytosis (14,730/mm³). Coagulation parameters were deranged with APTT 62.1 seconds and ₹1.5, suggesting disseminated intravascular coagulation (DIC). Bedside ultrasound showed a 330 mL broad ligament hematoma and raised the suspicion of uterine rupture and bladder injury.
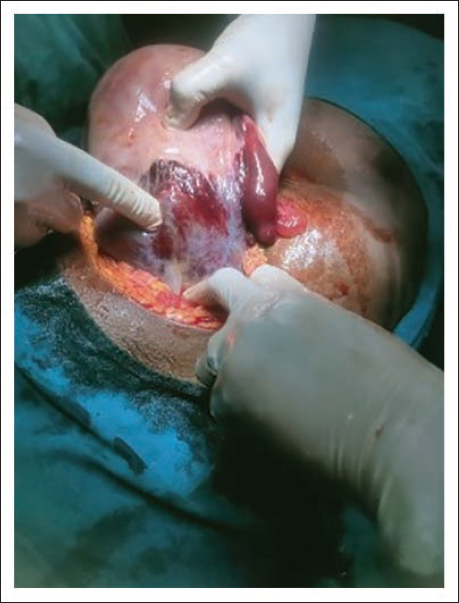
Given the rapidly deteriorating condition, emergency exploratory laparotomy was undertaken. Intraoperatively, a massive hemoperitoneum was identified, with a left lateral uterine wall rupture extending from below the cornua to the cervix. A 3 cm posterior bladder wall tear explained the gross hematuria. Peripartum hysterectomy was performed due to extensive uterine destruction and uncontrolled bleeding (Figures 1–4).
Hematoma from Lower Uterine Segment Extending to the Left Broad Ligament.
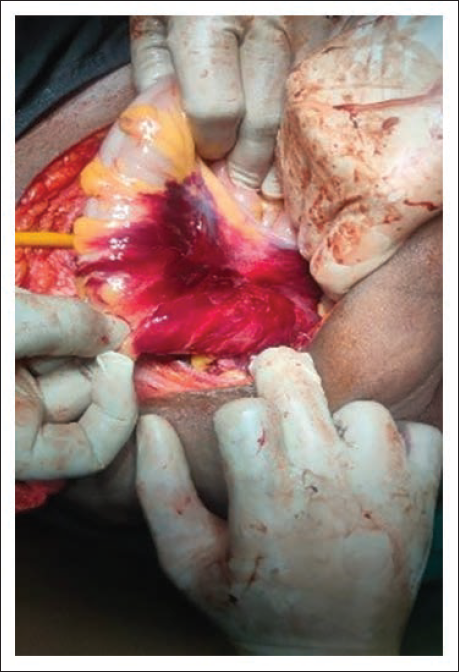
Multiple Mesenteric Contusions.
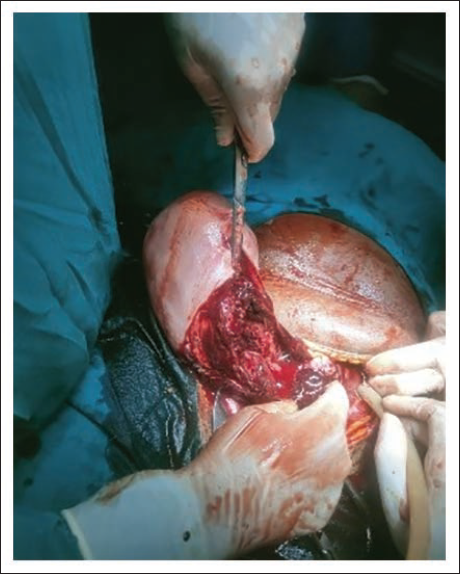
Left-side Lateral Uterine Wall Rupture from Below the Cornua up to the Cervix.
Lateral Uterine Wall Rupture.
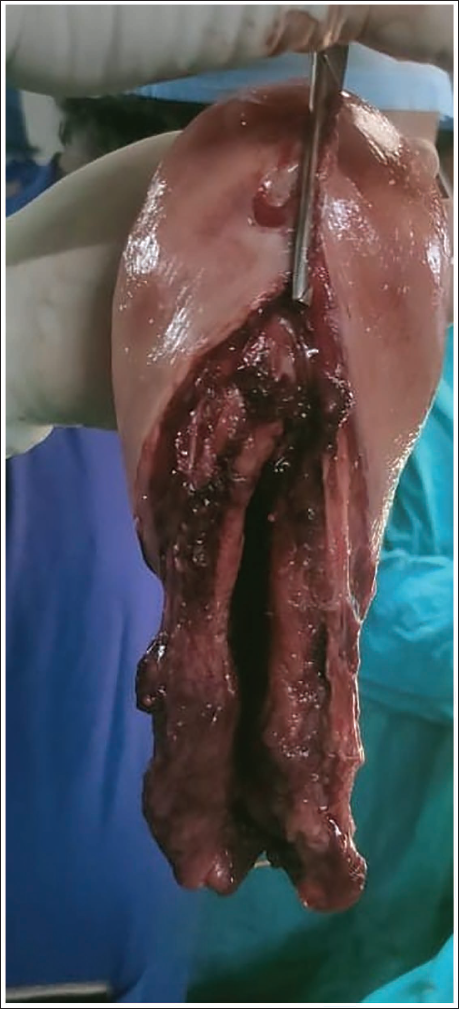
The bladder injury was repaired, a suprapubic catheter was placed, and left internal iliac artery ligation was performed to aid hemostasis. Despite aggressive transfusion of packed red cells, platelets, fresh frozen plasma, and inotropic support, the patient remained unstable postoperatively.
She developed acute kidney injury, with serum creatinine rising to 5.4 mg/dL and severe metabolic acidosis. Coagulopathy persisted with ongoing DIC, and multi-organ dysfunction ensued. On the second postoperative day, she experienced bradycardia followed by circulatory collapse. Five cycles of cardiopulmonary resuscitation were unsuccessful, and she was declared dead 48 hours after admission due to cardiac arrest secondary to hemorrhagic shock, DIC, and multi-organ failure.
Discussion
The present case of a multiparous woman with combined uterine and bladder rupture following an instrumental vaginal delivery aligns with the complications reported in earlier literature, highlighting significant and preventable maternal risks. In the case by Yaliwal et al., 6 a similar pattern emerged where a vacuum-assisted delivery in a grand multipara resulted in cervical, uterine, and bladder injuries necessitating hysterectomy and bladder repair. The current case, however, demonstrates even more critical deterioration, including DIC and eventual multi-organ failure, leading to maternal death, a progression not observed in Yaliwal’s 6 successfully managed patient.
Baheti 4 reported an isolated intraperitoneal bladder rupture following an outlet forceps delivery in a primigravida with macrosomia, underscoring that bladder injuries can occur even without uterine rupture when unrecognized bladder overdistension or trauma exists. The present case extends this observation to the more catastrophic scenario of concurrent uterine and bladder rupture in a multiparous woman, possibly exacerbated by excessive fundal pressure, similar to risk factors described in Abubakar and Idris Takai’s report from a low-resource setting. 7
Namagembe et al. 5 identified obstructed labor and delayed laparotomy as leading contributors to preventable deaths from uterine rupture in Uganda. Their analysis emphasized the importance of early recognition and rapid intervention. This mirrors the index case, where delayed diagnosis and management culminated in fatal multi-organ dysfunction. While Namagembe et al. 5 reported high maternal survival when timely surgery was performed, in the present case, despite prompt laparotomy upon referral, the extent of systemic decompensation was irreversible.
Finally, Stabile et al. 8 reviewed spontaneous bladder ruptures post a vaginal delivery, emphasizing that early signs such as hematuria and rising creatinine should prompt rapid urological evaluation. In the current case, hematuria was present but occurred alongside massive hemorrhage and DIC, compounding the diagnostic and therapeutic complexity.
Collectively, these comparisons stress the critical role of antenatal risk assessment, skilled intrapartum care, and immediate access to surgical intervention in averting such rare but lethal outcomes.
Conclusion
Combined uterine and bladder rupture following vaginal delivery is a rare but life-threatening complication. Early recognition, skilled obstetric care, and timely surgical intervention are vital to reduce maternal morbidity and mortality. Strengthening intrapartum monitoring and emergency response protocols is essential to prevent such catastrophic outcomes, especially in high-risk deliveries.
Authors’ Contribution
Rajasri Yaliwal: Conceived the case report and identified its clinical relevance; designed the structure and clinical focus of the report; defined the key learning points and intellectual focus; supervised the literature review; managed patient care and supervised all interventions; supervised the collection of clinical and operative data; drafted key sections of the manuscript; critically revised and edited the manuscript; reviewed and approved the final version; guarantor of the manuscript.
Shreedevi Kori: Assisted in conceptualizing the report; assisted in report design and flow; assisted in refining the intellectual content; performed literature search and identified key references; assisted in clinical management; assisted in clinical data acquisition; prepared the first draft and case description; assisted in editing and formatting; reviewed and approved the final version.
Ekta Chabra: Contributed to clinical insights; reviewed clinical design; reviewed and edited content; assisted in literature compilation; contributed to case follow-up and clinical correlation; organized perioperative data; assisted in manuscript drafting; provided editorial suggestions; reviewed the final draft.
Annapurna Hadalageri: Assisted in initial case evaluation; contributed clinical inputs; assisted in content compilation; collected additional references; participated in bedside clinical care; collected and documented bedside data; contributed to clinical details; assisted in minor corrections; reviewed the final draft.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from the Institutional Ethics Committee (IEC number: BLDE (DU)/IEC/1209//2025-26).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed consent was taken from the participant.
