Abstract
Aims and Background
Snakebite envenomation remains a significant public health issue in India, with a continuous need for comprehensive data on its epidemiology, clinical manifestations, and treatment outcomes. This study aims to analyze the demographic, clinical, and epidemiological profiles of snakebite victims and evaluate their clinical outcomes.
Materials and Methods
This retrospective observational study was conducted over 1 year (January–December 2024) at a 2500-bed tertiary care hospital in Mangaluru. Using a chart review method, data were collected from medical records of patients admitted with snakebite history. The study analyzed demographic details, clinical signs and symptoms, treatment protocols, and laboratory findings.
Results
A total of 183 snakebite cases were documented. There was a clear link between the type of treatment provided and patient outcomes, including discharge status, complications, and mortality. Key factors influencing outcomes included co-existing health conditions, delay in hospital presentation, severity of local and systemic envenomation, and the species of snake involved. Patients with delayed access to care often presented with significant laboratory abnormalities, reflecting severe envenomation.
Conclusion
The study underscores the ongoing threat of snakebite in India and the critical need for prompt medical care. Delays in treatment were associated with worse clinical and laboratory outcomes. These findings highlight the importance of rapid response systems, early intervention, and adherence to treatment protocols, and they offer valuable guidance for improving public health strategies and clinical management of snakebite cases.
Introduction
Snakebite envenomation poses a significant global health burden and was officially recognized as a neglected tropical disease by the World Health Organization (WHO) in 2017. 1 India bears a disproportionate share of this crisis, with an estimated 2 million snakebites annually, resulting in 50,000-60,000 deaths each year. 2 Beyond mortality, snakebite survivors often endure long-term morbidity, including limb amputations, musculoskeletal deformities, chronic kidney injury, neurological deficits, and post-traumatic stress disorder. 3
Recognizing the urgency of this issue, the WHO has set an ambitious target to reduce snakebite mortality to 50% by 2030. 4 In response to this, India, which is identified as a priority nation, launched the National Action Plan for Prevention and Control of Snakebite Envenoming (NAP-SE), aligning with the WHO’s global road map. 5 To achieve this goal, we require robust data, including a comprehensive understanding of snakebite epidemiology, clinical manifestations, and treatment outcomes.
Climate change along with the rapid expansion of human habitats is driving significant shifts in temperature, rainfall, and land use, leading to more frequent interactions between humans and snake populations. Consequently, rising temperatures, habitat fragmentation, and urban encroachment are propelling snakes into new territories, thereby escalating the incidence of snakebites and posing a critical public health challenge. 6 The burden of snakebite diversity is high in India due its vast and varying landscape and vegetation.
India is home to numerous snake species, but four venomous species, known as the “Big Four”—the Indian cobra, the common krait, Russell’s viper, and the saw-scaled viper—are responsible for most medically significant bites. Non-venomous species such as the Indian rat snake, checkered keelback, common wolf snake, and green vine snake are also commonly encountered. There is lack of awareness and misconceptions about snakes among the community, which results in harmless snakes being killed out of fear, while venomous species are mishandled, increasing the risk of envenomation.
Despite the significant burden of snakebites, gaps remain in public awareness, first-aid practices, access to antivenom, and overall patient management. Effective snakebite management depends not only on early clinical recognition, which includes local signs (pain, swelling, ecchymosis, blistering, paresthesia) and systemic symptoms (neurotoxicity, coagulopathy, renal and cardiac effects), but also on rapid diagnosis, appropriate antivenom administration, and supportive care. Laboratory investigations, such as the 20-minute whole blood clotting test (20WBCT), coagulation profiles, and organ function tests, play a crucial role in confirming envenomation. 7
To bridge these gaps, snakebite profile studies are critical. They provide valuable epidemiological data on who is affected, which snakebites are the most prevalent, and how different envenomations present clinically. Such studies help evaluate treatment practices, first-aid practices, effectiveness of public health policies, patient outcomes, and planning preventive strategies through education and habitat management.
Given these critical gaps, we undertook this 1-year retrospective study with the aim: to analyze the demographic, clinical, and epidemiological profiles of snakebite victims and evaluate their clinical outcomes.
Methods
After receiving approval from the Institutional Ethics Committee, we conducted a retrospective observational study using the chart review methodology. We extracted data from medical records of snakebite patients admitted to a 2500-bed tertiary care hospital between January and December 2024. The facility includes an 80-bed intensive care unit with dialysis capabilities and a blood bank.
Snakebite is a notifiable disease, and all patient information was accessible through the hospitals Electronic Medical Records system. Our study included all patients who presented to the Emergency Department with snakebite history and were managed according to the hospitals standardized protocol.
This protocol involved collecting detailed information about the incident, including the time and location of the bite, snake identification (either by patient description or by comparison with reference images), and documentation of any treatments received before hospital arrival. Each patient underwent a comprehensive clinical assessment, including the measurement of vital signs (heart rate, blood pressure, temperature, oxygen saturation, and respiratory rate) and documentation of preexisting medical conditions.
The envenomation evaluation included an assessment of both local and systemic manifestations. Local signs examined were swelling, edema, pain, bleeding, ulceration, blistering, bruising, and compartment syndrome (identified by pain, paresthesia, pallor, pulselessness, and paralysis). Systemic manifestations were categorized as hemotoxic (malaise, abdominal pain, weakness, drowsiness, hypotension, syncope, shock, cardiac arrhythmias, myocardial damage, and bleeding manifestations); neurological (diplopia, dysarthria, dysphagia, dysphonia, dyspnea, ptosis, and paralysis); and rhabdomyolysis (muscle stiffness, tenderness, pain on passive stretching, trismus, and dark brown urine).
Diagnostic testing included the 20-minute whole blood clotting test (20WBCT), performed by collecting 2 mL of venous blood, transferring it to a glass test tube, and observing for clot formation after 20 minutes. The absence of clotting indicated coagulopathy. For suspected neurotoxic envenomation, we conducted the single-breath-count test (normal: >30 counts), breath-holding time assessment (normal: 40–45 seconds), inter-incisor distance measurement (normal: ≥3 fingers), and the duration of sustained upward gaze. 8
For suspected hemotoxic envenomation, we performed serial 20WBCT tests every 30 minutes for the first 3 hours, along with comprehensive laboratory investigations: complete blood count, platelet count, coagulation profile, renal function tests, and serum electrolytes. All patients received electrocardiograms, with chest X-rays performed as indicated. Patients without envenomation signs were observed for 6-24 hours, suspected humped nose pit viper cases were observed for 48 hours. Patients declining admission received baseline blood workup and instructions to return immediately if signs or symptoms of envenomation developed.
Patients presenting with envenomation received anti-snake venom (ASV) therapy—10 vials diluted in 500 mL normal saline administered over 1 hour—following premedication with Injection Pheniramine Maleate 22.75 mg (Avil 1 ampoule) and 100 mg hydrocortisone—to prevent hypersensitivity reactions. Patients were closely monitored for infusion-related reactions, including cutaneous rashes, facial swelling, chills, tremors, cough, dizziness, throat tightness, vomiting, tachypnea, hypoxia, sweating, and bronchospasm. If reactions occurred, the infusion was temporarily suspended while symptomatic treatment, including intramuscular injection Adrenaline (0.5 mg), was administered. The infusion resumed cautiously after 10-15 minutes or symptom resolution.
Patients requiring intensive monitoring or mechanical ventilation were transferred to the ICU. All patient details were documented according to the performa in Table 1. Patients who left against medical advice were instructed to monitor for envenomation signs and return promptly if symptoms developed.
Data Collection Performa.

Statistical Analysis
The demographic, clinical, and epidemiological profiles of snakebite victims are summarized using descriptive statistics. For categorical variables such as gender, site of bite, occupation, activity during bite, tourniquet use, local treatment, 20-minute WBCT result, snake identification, ASV administration, reaction to ASV, and final outcome, frequencies and percentages are calculated and presented. For continuous variables such as heart rate and BP measurement, the mean and standard deviation are assessed.
Results
The demographic and epidemiological profiles of the included patients are shown in Table 2, the clinical assessment and interventions done are shown in Table 3, the relationship between outcome variables and observed variables is shown in Table 4, and the associations between outcome variables are depicted in Table 5.
Frequency and Percentage of 183 Patients Depicting the Demographic and Epidemiological Characteristics.
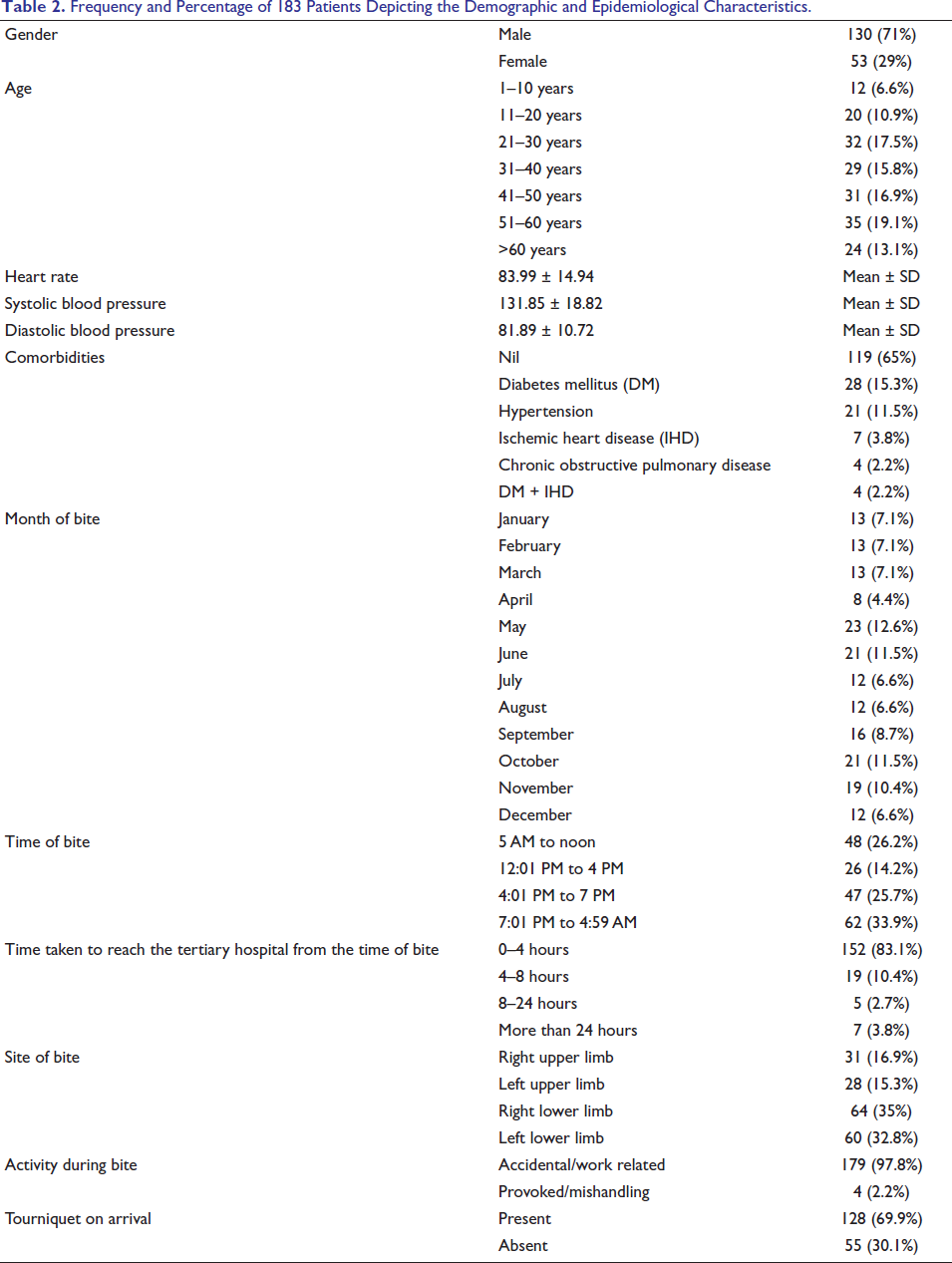
Frequency and Percentage of 183 Patients Depicting the Clinical Assessment and Interventions Done.
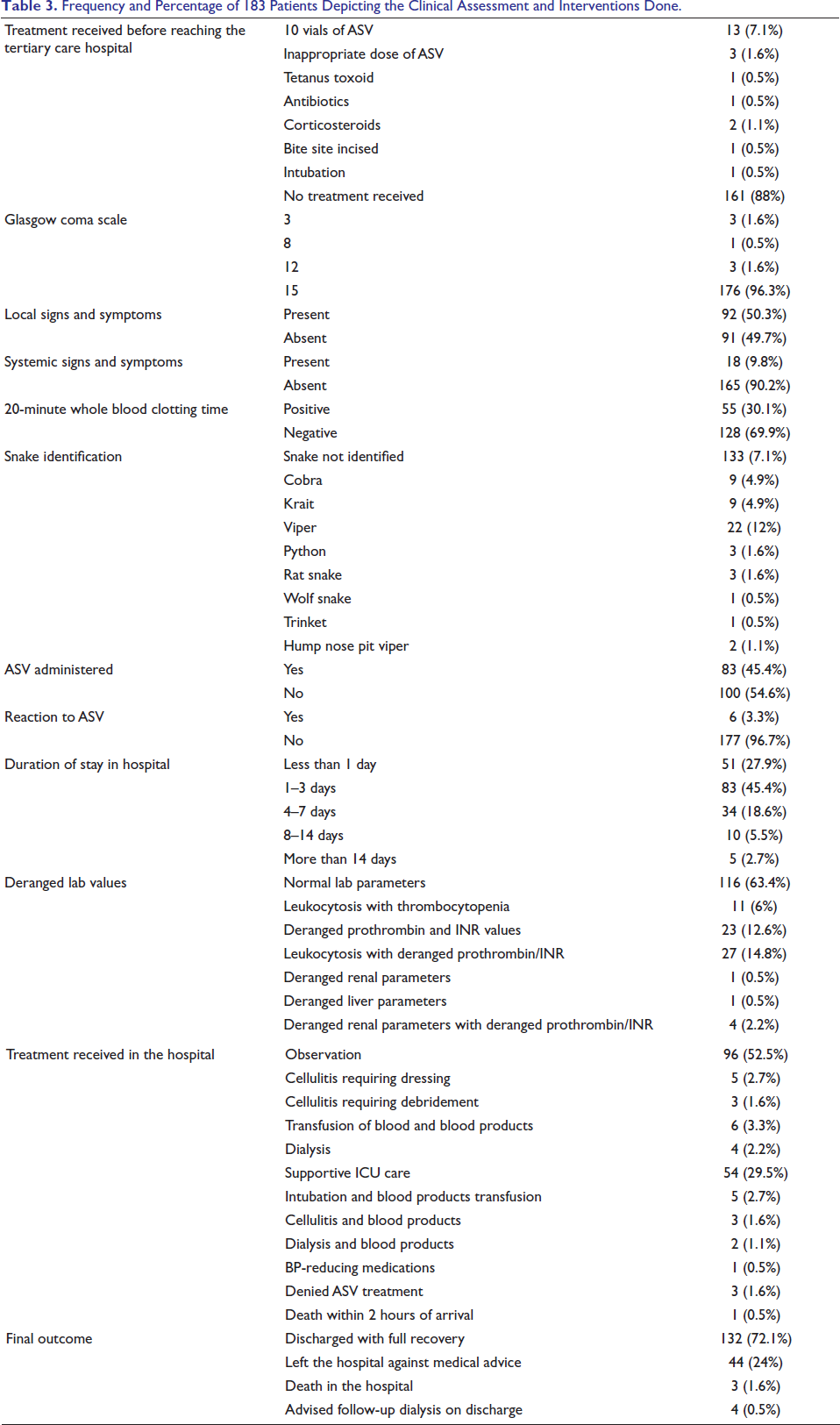
Relationship Between Outcome Variables: Duration of Stay in the Hospital, Deranged Lab Values, Treatment Received, and Final Outcome with Other Measured Variables.
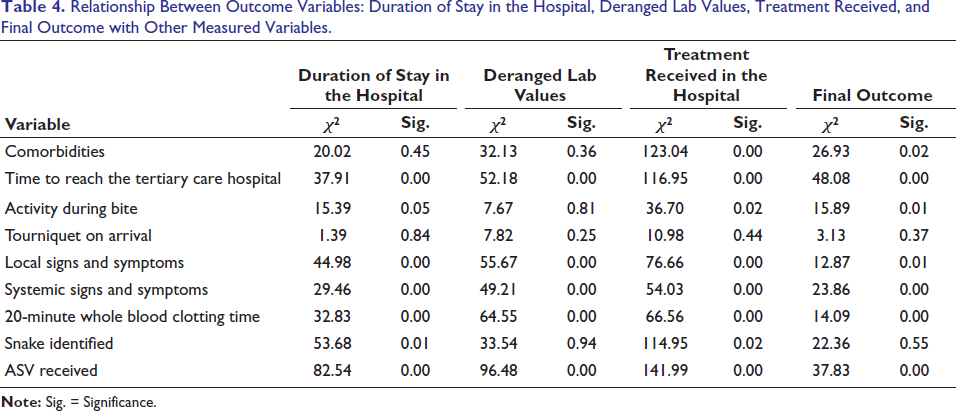
Association Between Outcome Variables.
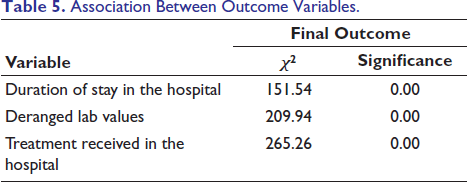
Discussion
The present study provides insights into the demographic and clinical characteristics of snakebite victims presenting to a tertiary care center. Understanding the specific epidemiological patterns and clinical characteristics of snakebites within particular regions is crucial for developing and implementing targeted public health interventions. This report aims to analyze the findings of a profile study conducted in Mangaluru.
Demographic and Epidemiological Profiles
We noticed that there was predominance of males being bitten by snakes, which is consistent with previous literature, which states that the outdoor activity of males contributes to the increased occurrence of bites among them.9, 10 We noticed that people aged 51-60 years and 21-30 years experienced more snakebites, and there are regional variations in the age group among snakebite victims. Meghan noticed more elderly being bitten by snakes in the United States, while Bhavesh noticed more incidents of snakebites in younger populations.10, 11 We noticed normal mean baseline vitals of heart rate and blood pressure on arrival. A higher frequency of bites was noted in the months of May, June, and October in our region. Snakes are ectothermic and more active in warmer temperatures, which are typical in May and June, before and during the monsoon. Studies show a positive correlation between higher ambient temperatures and snakebite incidence, especially in spring and summer months. 12 During the monsoon, heavy rains cause flooding and waterlogging of snake habitats, forcing snakes to move and increasing their encounters with humans. Also, the breeding habits of frogs and the rodent population, common prey for snakes, increase during the monsoon and post-monsoon periods. This abundance attracts snakes closer to human dwellings and agricultural fields, where they hunt, leading to more human–snake encounters. 13 November–January are relatively cooler, and snakes enter a state of brumation, that is, decreased activity to conserve energy, and therefore, the bite incidents are also low.
Most incidents occurred between 7 PM and 5 AM (33.9%), and between 5 AM and noon (26.2%). These findings indicate nocturnal and early morning activity of snakes, periods when visibility is compromised and human activities intersect with snake movement patterns, emphasizing the importance of preventive strategies such as the use of protective footwear and bed nets during sleep.10, 14 A majority of patients (83%) reached the tertiary care facility within 4 hours of the bite, suggesting improved awareness or access to medical care. However, a small proportion (6.6%) had delays exceeding 8 hours, underlining the need for continued community education and improved transport infrastructure. 15 The lower limbs were the most common site of bite, which aligns with the existing literature noted by Jarvani and Satyanarayan and highlights the need for protective legwear in at-risk populations.10, 16 A majority of the bites were due to accidental bites, and 4 out of the 183 bite incidents were due to snake mishandling and provoked bites; this emphasizes the safe handling of snakes, which includes knowledge, caution, and the use of proper techniques and tools to minimize risk to both the handler and the snake. The use of tourniquets was noted in 70% of cases, reflecting ongoing reliance on traditional first-aid practices, despite their potential for harm. This finding signals a crucial gap in public knowledge and points to the need for targeted health education interventions promoting evidence-based pre-hospital care.13, 17
Clinical Presentation and Early Management
Pre-hospital care was found to be suboptimal in 3 out of 183 patients, with one case involving a harmful procedure such as incising the bite site. The continued use of such detrimental practices highlights a persistent lack of awareness and education within the community. 18 Identifying snake species remains a considerable challenge, with 72.7% of cases involving unidentified snakes. Among the cases where species were identified, vipers accounted for the highest proportion (12.0%), followed by cobras and kraits, each representing 4.9% of cases. A scoping review on identifying snakes where snakebites are common involves a variety of approaches such as capturing or killing the biting snake for examination, descriptions provided by the victim or bystanders, assessment of clinical symptoms, laboratory testing, and photographic documentation of the snake. The ability of victims, witnesses, and healthcare workers to recognize and identify the snake is highly context-dependent, influenced by the circumstances surrounding the bite, the diversity of local snake species, and their familiarity with these snakes. Taking a photograph of the snake may serve as a practical alternative in some cases. 19 Local signs and symptoms were observed in 50.3% of the cases, while systemic manifestations occurred in only 9.8%, indicating that local envenomation was more common. The occurrence of systemic envenomation among snakebite patients varies significantly—ranging from approximately 14% to over 90%—depending on the snake species involved and the geographical region. This underscores the wide variability in envenomation severity and emphasizes the need for context-specific data. 20
Treatment Modalities and Course in Hospital
Antivenom was administered to 45.4% of patients based on clinical and laboratory evidence of envenomation, with a low adverse reaction rate (3.3%). The majority of patients (73.2%) required a hospital stay of less than 3 days, suggesting predominantly mild to moderate envenomation severity in our population. However, 15 patients (8.2%) required hospitalization exceeding 8 days, indicating severe envenomation or complications. Laboratory abnormalities were present in 36.6% of the cases, with coagulation disturbances being the most common (29.5% had deranged prothrombin/INR values with or without other abnormalities). This reinforces the predominance of hemotoxic envenomation in our patient population, consistent with the regional prevalence of viper bites. Snakebite envenomation leads to significant derangements in hematological, renal, and inflammatory parameters. These laboratory findings are critical for diagnosing complications, guiding treatment, and predicting patient outcomes.3, 10, 13
The spectrum of interventions ranged from simple observations (52.5%) to intensive supportive care. Notably, 54 patients (29.5%) required ICU support, 11 patients (6.0%) needed blood product transfusions, and 6 patients (3.3%) required dialysis for acute kidney injury. Surgical interventions for local complications were relatively uncommon, with only 8 patients (4.4%) requiring wound dressing or debridement for cellulitis. Research indicates that snakebite management typically involves antivenom as the primary specific therapy, supplemented by supportive measures such as analgesics, ventilatory support, fluid resuscitation, hemodialysis, blood transfusions, and antibiotics when needed. 21
The overall mortality rate was 1.6% (three patients), which is comparable to figures reported in similar contexts where antivenom and supportive care are readily available. 22 A majority of patients (72.1%) experienced full recovery, while four individuals (2.2%) were discharged with a need for ongoing dialysis, reflecting continued renal issues. Notably, a relatively high percentage (24.0%) of patients left the hospital against medical advice, highlighting the need to explore potential socioeconomic factors that may hinder the completion of treatment. Overall, timely access to antivenom and appropriate supportive care plays a vital role in minimizing snakebite-related deaths. Mortality rates in such settings typically remain low, often between 1% and 3%. 22
Association Between Outcomes: Duration of Stay in Hospital, Deranged Lab Values, Treatment Received in the Hospital, Final Outcome, and Other Measured Variables
The present study showed a significant association between the time to reach tertiary care hospital, activity during bite, local and systemic signs of envenomation, 20-minute WBCT, the type of snake, and ASV administration and the length of stay in the hospital. Studies have consistently shown that delays in seeking medical care are associated with longer hospital stays and increased morbidity. 23 The severity of envenoming is a significant determinant of hospital stay duration. Patients with severe systemic manifestations, such as respiratory failure, acute renal failure, or hematologic abnormalities, require longer hospitalization. A study in South India reported that patients with severe envenomation had a mean hospital stay of 8.2 days, compared to 4.8 days for those with mild envenoming, similar to our findings. 9
We also documented significant derangement in lab parameters with patients who took prolonged time to reach the hospital, local and systemic signs of envenomation, 20-minute WBCT and ASV administration; these findings are consistent with findings of Satyanarayan et al and Jayaram et al.16, 23 The study noted a significant association between the treatment received in a hospital and the final outcome (discharged/mortality/morbidity), with variables such as existing comorbidities of patients, time taken to reach the hospital, local and systemic signs of envenomation, type of snake and ASV administration. This implies that these parameters are crucial for predicting outcomes; it is also important to consider that individual patient responses can vary significantly based on factors such as overall health, severity of envenomation, and specific snake species involved.23-25 This study also revealed a significant association between outcome variables. The length of stay in the hospital, deranged lab values, and treatment received in the hospital had a significant association with the final outcome in the patients; similar finding were noted by Melit et al, Warrell et al, Saravu et al, and Menon et al.15, 21, 26, 27
Limitations of the Study
The retrospective design prevents establishing clear cause–effect relationships. The study being limited to a single center in Mangaluru restricts generalizability to regions with different snake species and healthcare resources. Missing data, especially from patients who left against medical advice, create a potential selection bias. The lack of detailed socioeconomic analysis misses an opportunity to understand factors affecting patient decisions. The treatment protocol variations could introduce confounding variables that might account for outcome differences. These constraints suggest future studies would benefit from prospective designs, multicenter collaboration, standardized treatment protocols, and more comprehensive socioeconomic data collection to strengthen the evidence base for snakebite management.
Conclusion
This study underscores snakebite envenomation as a persistent public health challenge in India, providing critical insights into demographic patterns and clinical factors that significantly influence patient outcomes. The identification of key prognostic indicators—including time to hospital presentation, local and systemic signs of envenomation, comorbidities, and snake species—establishes an evidence base for optimizing treatment protocols and developing targeted interventions for vulnerable populations
Clinical Significance
This study reinforces the urgent need for rapid medical intervention in snakebite cases, as delayed hospital arrival was strongly associated with worse clinical outcomes and abnormal lab findings. It underscores the importance of early recognition and administration of ASV to mitigate morbidity and mortality. The data also reveal that preexisting comorbidities and specific envenomation signs significantly impact recovery, offering a framework for risk stratification in clinical settings. These findings can guide public health policies to enhance awareness, expedite referrals, and optimize treatment protocols for snakebite victims in India.
Footnotes
Authors’ Contribution
Shailaja Sampangiramaiah: Design, definition and intellectual content, literature search, clinical studies, data acquisition, data analysis, statistical analysis, manuscript preparation, editing and review, guarantor.
Nagesh Karpur Ramegowda: Design, definition and intellectual content, manuscript preparation, editing and review, guarantor.
Joanne Juliet Sequeira: Literature search, clinical studies, data acquisition, data analysis, manuscript preparation, editing and review, guarantor.
Ruban Shaun Dsouza: Literature search, clinical studies, manuscript preparation, editing and review, guarantor.
Declaration of Conflict of Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from the Institutional Ethics Committee (FMIEC/CCM/185/2025).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed consent was taken from the patients before the conduct of the study.
