Abstract
Background
Interoception, the sensing of internal physiological states, is fundamental to homeostasis but remains underrepresented within core physiology teaching and clinical reasoning.
Objectives
To highlight interoception as an integrated physiological system and synthesize its neural, humoral and cortical mechanisms across organ systems.
Methods
This conceptual communication reviews established experimental and clinical literature on visceral afferent pathways, gut–brain hormones, cortical integration and organ-specific internal sensing to propose an integrative physiological framework.
Results
Interoception arises from coordinated signalling through vagal and spinal afferents, circulating hormones and central processing within the insula and anterior cingulate cortex. Cardiovascular, gastrointestinal, urinary, nociceptive and immune systems generate continuous internal feedback that supports autonomic regulation, behavioural adaptation and subjective awareness. Disruptions in interoceptive processing are implicated in anxiety disorders, chronic pain, fatigue and functional syndromes.
Conclusion
Recognizing interoception as a formal physiological domain may enhance integrative teaching and improve clinical interpretation of symptoms lacking structural correlates, thereby bridging objective regulation with subjective experience.
Introduction
Physiology has traditionally focused on organ systems that maintain the internal environment, yet the mechanisms by which internal bodily states are sensed and integrated remain insufficiently emphasized. Interoception refers to the sensing of internal physiological conditions, including hunger, thirst, heartbeat, dyspnoea, pain and visceral discomfort. Unlike exteroception, which monitors the external environment, interoception informs the brain about internal states essential for regulation and adaptation. Despite its foundational role in homeostasis, interoception has largely been conceptualized within neuroscience and psychiatry rather than physiology.1, 2
Recent work has illuminated how interoception arises from a complex integration of afferent neural pathways, including vagal and spinal inputs, hormonal signals such as ghrelin and leptin, and central processing within the insular cortex and anterior cingulate.3, 4 This internal sensing system not only supports vital reflexes like satiety or blood pressure control but also plays a central role in emotional awareness, fatigue and chronic disease.5, 6
Core Mechanisms of Interoception
Interoception arises from coordinated signalling across peripheral sensors, humoral messengers and central neural circuits. Visceral afferents, particularly via the vagus nerve and spinal pathways, detect changes in organ states and relay information to the nucleus tractus solitarius. These signals are subsequently integrated within higher cortical regions, including the posterior and anterior insula and anterior cingulate cortex, contributing to conscious awareness, affective modulation and behavioural regulation.2, 3
In parallel, humoral signals, such as ghrelin, leptin, insulin, cortisol and inflammatory cytokines, modulate internal sensing by acting on peripheral receptors and central targets. Together, neural and humoral pathways enable continuous monitoring of physiological states, linking internal regulation with subjective experience.6, 7
Organ-specific Interoception
In the cardiovascular system, the interoceptive awareness of cardiac activity, often termed cardioception, contributes to emotional regulation and autonomic balance. Signals originating from baroreceptors and cardiac mechanoreceptors are relayed to cortical regions such as the insula and anterior cingulate, where they influence arousal and stress responsiveness. Heightened or distorted cardiac interoception has been associated with anxiety sensitivity and altered emotional processing. 8
The gastrointestinal tract represents a major hub of interoceptive signalling. Mechanoreceptors, chemosensors and enteroendocrine cells detect luminal distension, nutrient composition and chemical stimuli, generating afferent signals conveyed primarily via vagal pathways. Gut-derived hormones such as ghrelin and leptin further modulate central appetite and satiety circuits, linking visceral sensing with energy balance and reward processing. These integrated neural and hormonal signals enable the dynamic regulation of feeding behaviour and metabolic homeostasis.6, 9
Interoception within the urinary system underlies the perception of bladder fullness and urgency. Stretch-sensitive afferents from the bladder wall transmit information to cortical regions involved in sensorimotor integration and salience detection, including the insula. Functional imaging studies demonstrate that bladder-related visceral signals engage neural networks overlapping with emotional and body-awareness circuits, highlighting the integration of continence control with conscious interoceptive processing. 10
Pain represents a prominent interoceptive experience shaped by both peripheral nociception and central interpretation. Rather than reflecting tissue injury alone, pain perception is influenced by emotional context, prior experience and cortical modulation of bodily signals. Chronic pain conditions are increasingly associated with altered interoceptive accuracy, wherein exaggerated or misinterpreted internal signals contribute to symptom persistence and functional impairment.8, 11
The immune system also contributes to interoceptive signalling through the action of inflammatory mediators. Cytokines released during immune activation can influence central neural circuits, giving rise to subjective sensations such as fatigue, malaise and cognitive slowing. These internally generated experiences reflect the integration of immune-derived signals into conscious awareness, reinforcing the role of interoception in coordinating physiological defence responses with behavioural adaptation. 7
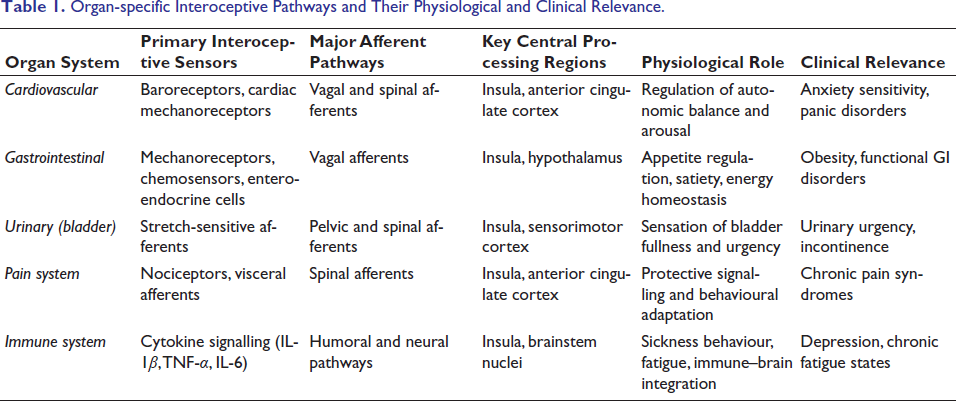
The organ-specific components of interoceptive signalling, including peripheral sensors, afferent pathways, central processing regions and clinical relevance, are summarized in Table 1.
Organ-specific Interoceptive Pathways and Their Physiological and Clinical Relevance.
Clinical and Translational Relevance
Disruptions in interoceptive processing are increasingly linked to clinical conditions involving emotion regulation, pain perception and fatigue. In anxiety and panic disorders, heightened sensitivity to internal signals such as heart rate or respiration may amplify threat perception, whereas depressive states may involve blunted interoceptive awareness.3, 12 Chronic pain represents a paradigmatic interoceptive disorder, in which an altered central interpretation of bodily signals contributes to persistent symptoms despite limited peripheral pathology. 11
These observations suggest that interoceptive function merits consideration alongside conventional physiological measures. Simple assessment tools and emerging digital approaches may help identify maladaptive internal sensing, offering new translational opportunities.
Implications for Physiology
Despite its anatomical and biochemical foundations, interoception remains largely absent from standard physiology curricula. Physiological systems are often taught in isolation, with limited emphasis on how internal states are sensed, integrated and subjectively experienced. Recognizing interoception as a physiological system highlights the importance of brain–body feedback loops in shaping behaviour and homeostasis. 4
Incorporating interoception into physiology education may enhance the understanding of symptoms that lack clear structural correlates, such as unexplained fatigue or dyspnoea. Framing internal sensing as a unifying physiological process encourages integrative teaching across cardiovascular, gastrointestinal, endocrine and neural systems.
From a broader conceptual perspective, interoception can be understood as an active process in which the brain continually interprets and updates information about internal bodily states to maintain physiological stability. This view aligns with the framework of active interoceptive inference, which emphasizes prediction and regulation of internal signals rather than passive sensing. 13
Limitations
This communication is conceptual in nature and does not include original empirical data; however, it synthesizes established physiological and clinical evidence to advance an integrative framework for understanding interoception.
Conclusion
Interoception represents a central but underrecognized component of physiological regulation. Framing interoception as a multilevel system spanning neural, humoral and cortical processes provides a more integrated account of how the body monitors and maintains internal stability. Greater incorporation of interoceptive principles into physiology teaching and clinical reasoning may strengthen links between objective regulation and subjective experience.
Footnotes
Authors’ Contribution
DKG conceptualized the manuscript, performed the literature review, drafted and revised the text. AC contributed to conceptual development, critical revision, and final approval of the manuscript.
Both authors approved the final version of the manuscript and agree to be accountable for all the aspects of the work.
Declaration of Conflict of Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval and Informed Consent
Ethical approval and informed consent are not applicable for this article, as it is a conceptual review and does not involve human participants, animals, or identifiable data.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
