Abstract
Background
Metabolic syndrome (MetS) includes risk factors such as obesity, dyslipidemia, hypertension, and insulin resistance. Psychiatric patients are at higher risk due to medication effects and lifestyle factors. Despite its serious consequences, MetS is often underdiagnosed in this group. This study was conducted to study the prevalence of MetS in psychiatric patients attending the tertiary care center in southern India.
Materials and Methods
This analytical cross-sectional study includes 179 patients with a previously diagnosed psychiatric condition. Institutional ethical clearance was obtained. Informed consent was obtained from the participants or family members. Baseline demographic details, clinical data, including physical measurements, and laboratory data were collected. Data collected was analyzed with Statistical Package for Social Sciences (SPSS) version 24.
Results
In the present study, 59% of the study participants had MetS. The proportion of MetS among them increased with age (P < .001) and duration of psychiatric illness (P = .001). Patients with lower educational qualifications had higher chances of MetS (P < .018). Co-morbidities such as type 2 diabetes mellitus (DM) and hypertension were noted to be significantly associated with MetS (P < .001). There was a statistically significant association between alcohol consumption (P = .044) though there was no statistically significant association with smoking (P = .51). There was no statistically significant difference between the major psychiatric diagnosis such as bipolar affective disorder, depression, psychoses and the development of MetS (P = .86). Majority of the patients were non-compliant to their medications and none of the specific categories of drugs used had any significant statistical association with the MetS.
Conclusion
We observed a higher burden of MetS among psychiatric patients and identified factors that directly or indirectly would have contributed to its development. Addressing these factors is essential to prevent long-term complications associated with MetS.
Introduction
A broad spectrum of mental health issues affecting mood, thought processes, and behavior is collectively referred to as psychiatric disorders. According to the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders 1 “a clinically significant behavioral or psychological syndrome or pattern that occurs in an individual and is associated with present distress (e.g., a painful symptom) or disability (i.e., impairment in one or more important areas of functioning) or with a significantly increased risk of suffering from death, pain, disability, or a significant loss of freedom is defined as a psychiatric disorder.”
Individuals diagnosed with psychiatric disorders are more likely than the general population to experience an early all-cause death. 2 Physical co-morbidities, especially cardiovascular illnesses, account for nearly 60% of the excess mortality in mental patients. 3 Central obesity, high blood pressure, poor high-density lipoprotein (HDL) levels, increased triglycerides, and hyperglycemia are the hallmarks of metabolic syndrome (MetS). 4 It functions as a preclinical marker for the diagnosis of diabetes and cardiovascular disease (CVD).
MetS includes important cardiovascular risk factors that are frequently associated with insulin resistance, including central obesity, dysglycemia, high blood pressure, and high cholesterol. 5 The risk of peripheral vascular disorders, myocardial infarction, cerebrovascular accidents, atherosclerosis, and type 2 diabetes mellitus (DM) is increased by this condition.
Numerous variables, including psychological strain, inactivity, unhealthy eating habits, heavy smoking, and insufficient healthcare, have been linked to an increased risk of MetS in patients receiving psychiatric treatment. 6 Notably, a major factor in the rising incidence of MetS is the use of psychiatric medications. 7
Determining the MetS risk factors and directing its treatment can be facilitated by thoroughly reviewing the patient’s lifestyle, food preferences, and family medical history.
A person is diagnosed with MetS when they exhibit three or more metabolic abnormalities. These abnormalities include a waist circumference that is greater than 90 cm in men and 80 cm in women, serum triglyceride levels that are 150 mg/dL or higher, reduced HDL cholesterol that is below 40 mg/dL in men or below 50 mg/dL in women, increased fasting glucose levels that are 100 mg/dL or higher, and blood pressure readings that are either systolic ≥130 mm Hg or diastolic ≥85 mm Hg. 8
People with major depressive disorder, BD, and schizophrenia had comparatively higher odds of developing MetS, suggesting that MetS is a prevalent comorbidity observed in a variety of psychiatric patient populations.
Therefore, the likelihood that MetS and psychiatric diseases co-occur is likely due in large part to generic, non-specific disease mechanisms. MetS causes distress and functional impairment in people affected, and it shortens life spans. 9 Few studies conducted in India show that there are increased CVDs in psychiatric patients. There is a paucity of knowledge regarding the correlation between anti-psychotics with MetS features.
Hence, this cross-sectional study was undertaken to study the proportion and risk factors for MetS in people with psychiatric disorders in the South Indian population.
Materials and Methods
Study Design
This study is a hospital-based, analytical cross-sectional study aimed at estimating the proportion of MetS and its associated risk factors among psychiatric patients and correlating it with the usage of psychiatric drugs. This study was conducted in the outpatient (OP) department and inpatient (IP) ward of the Department of General Medicine and the Department of Psychiatry at St. John’s Medical College and Hospital, Bengaluru, Karnataka. The patients come from different parts of Karnataka, Andhra Pradesh, Telangana, and Tamil Nadu (adjacent states), from both rural and urban areas.
Study Participants
The study included all psychiatric patients who visited the OP department and those admitted as IPs at St. John’s Medical College from September 2022 to March 2024. Consecutive sampling was used for the selection of patients. Participants were selected based on predefined inclusion and exclusion criteria to ensure the reliability and validity of the study findings.
Sample Size
The sample size estimation was done using OpenEpi software version 2.3.1, based on the study conducted by Hussain et al. 10 which reported a 34.7% prevalence of MetS among psychiatric patients. Using this prevalence rate, the required minimum sample size was calculated to be 178 patients. This calculation was based on achieving an absolute precision of seven percent with a 95% confidence interval.
Ethical Considerations
The study protocol was reviewed and approved by the Institutional Ethical Committee of St. John’s Medical College and Hospital. Ethical clearance was obtained to ensure compliance with ethical standards in research. Written informed consent was obtained from all participants after explaining the study’s purpose, procedures, risks, and benefits. Participation was voluntary, and confidentiality of participant information was strictly maintained.
Inclusion Criteria
Patients aged 18 years and above.
Patients with a prior diagnosis of psychiatric conditions or those currently receiving treatment for psychiatric conditions.
Patients who provided written informed consent to participate in the study.
Exclusion Criteria
Patients under the age of 18.
Patients who did not provide written informed consent.
Patients admitted to the intensive care unit.
Patients with liver or renal-related disorders.
Pregnant patients.
Method of Data Collection
Data collection involved several steps to ensure comprehensive and accurate information gathering. Informed consent was obtained from all subjects.
Socio-Demographic Data
Collected through interviews and patient records, including age, gender, education level, occupation, and marital status.
Clinical Data
Gathered through clinical interviews with patients and their attendants, focusing on psychiatric diagnoses confirmed by qualified psychiatrists. Diagnoses recorded in OP and IP charts were considered.
Physical Measurements
Height, weight, blood pressure, and waist circumference were measured using standard techniques and calibrated instruments.
MetS Diagnosis
Assessed using the modified NCEP ATP III criteria for the Asian population, 8 which includes specific thresholds for waist circumference, triglycerides, HDL cholesterol, blood pressure, and fasting glucose levels.
Criteria for Metabolic Syndrome Diagnosis
MetS was diagnosed using the modified NCEP ATP III criteria tailored for the Asian population. 8
Waist circumference: >90 cm for males and >80 cm for females.
Triglycerides: ≥150 mg/dl.
HDL cholesterol: <40 mg/dl for males and <50 mg/dl for females.
Blood pressure: ≥130/85 mmHg.
Fasting glucose: ≥100 mg/dl.
Statistical Analysis
The collected data were analyzed using statistical software SPSS version 19. Descriptive statistics summarized the socio-demographic and clinical characteristics of the participants. The proportion of MetS was calculated along with 95% confidence intervals. The association between MetS and variables such as psychiatric diagnosis, psychotropic medication use, and socio-demographic factors was studied using the chi-square test. Statistical significance was at P < .05 considered significant.
Results
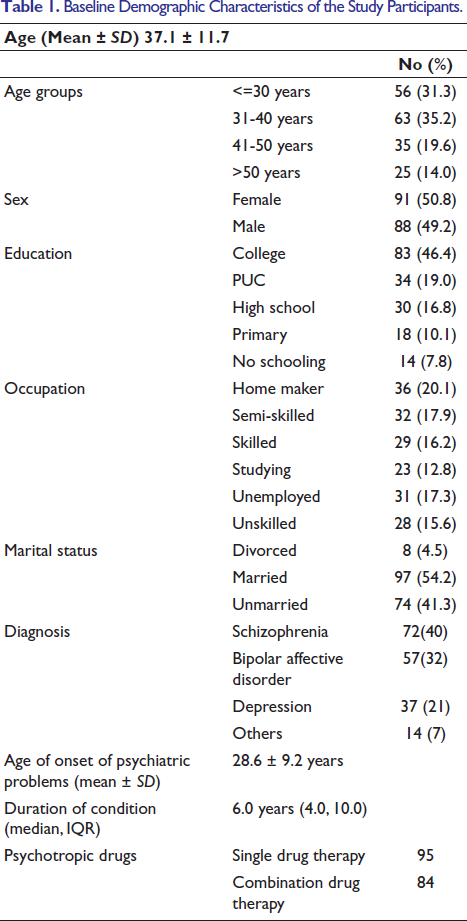
There were 179 participants in the study, and their average age was 37.1 years with a standard deviation of 11.7 years. The gender distribution showed a slight predominance of females, with 50.8% of the participants being female and 49.2% being male. A significant portion of the participants had attained higher education, with 46.4% having completed college. Among the participants, 20.1% were homemakers, reflecting a significant portion of individuals managing household responsibilities. Among the participants, a majority were married, accounting for 54.2% of the sample, as shown in Table 1.
Baseline Demographic Characteristics of the Study Participants.
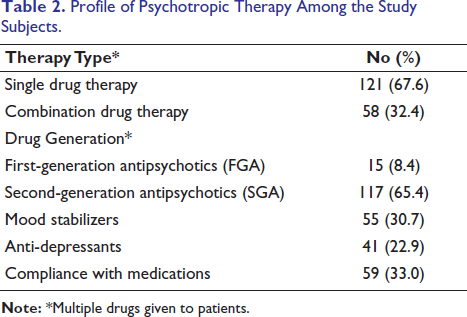
A majority of the participants were undergoing single drug therapy, with 95 individuals, accounting for 53.1% of the total sample. Combination drug therapy was utilized by 84 participants, representing 46.9% of the total sample. About 65.4% were on second-generation antipsychotics (SGAs). These medications are preferred for their efficacy and lower risk of certain side effects compared to first-generation antipsychotics (FGAs), which were used by 8.4% of the participants. Mood stabilizers were used by 30.7% of the participants. Anti-depressants were used by 22.9% of the participants. Compliance with medications was recorded for 59 participants, making up 33.0% of the total sample. As shown in Table 2.
Profile of Psychotropic Therapy Among the Study Subjects.
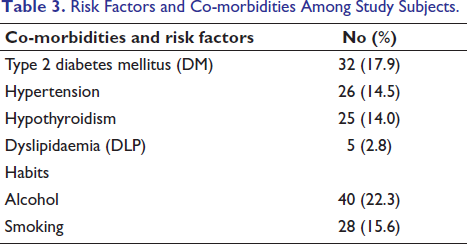
DM was the most prevalent co-morbid condition, affecting 17.9% of the participants. In terms of habits, ethanol consumption was reported by 22.3% of the participants. Smoking was reported by 15.6% of the participants. As shown in Table 3.
Risk Factors and Co-morbidities Among Study Subjects.
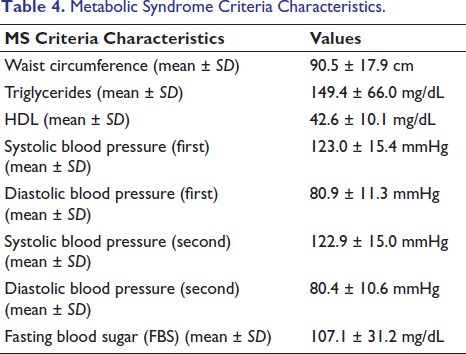
The “good cholesterol,” or HDL, had a mean of 42.6 mg/dL and a standard deviation of 10.1 mg/dL. Reduced HDL levels are a diagnostic criterion for MetS. Blood pressure’s systolic value was tested twice. The average values for the two measurements were 122.9 mmHg with a standard deviation of 15.0 mmHg and 123.0 mmHg with a standard deviation of 15.4 mmHg. Furthermore, the diastolic blood pressure was measured twice. The mean values of the two measurements were 80.4 mmHg with a standard deviation of 10.6 mmHg and 80.9 mmHg with a standard deviation of 11.3 mmHg in the first measurement.
The average fasting blood sugar (FBS) was 107.1 mg/dL, with a 31.2 mg/dL standard deviation. High FBS levels are a sign of diabetes or impaired glucose tolerance, two conditions that are part of the MetS. As shown in Table 4.
Metabolic Syndrome Criteria Characteristics.
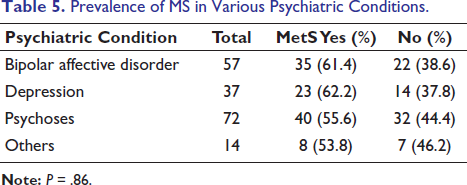
Among patients with bipolar affective disorder, 61.4% (54.4-68.4) with 95% CI were diagnosed with MetS. This indicates a high prevalence of MetS in individuals with bipolar disorder. Patients with depression showed a similar prevalence, with 62.2% (55.2-69) with 95% CI diagnosed with MetS. However, the difference was not statistically significant as shown in Table 5.
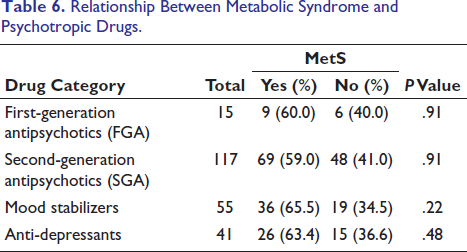
Among the 15 participants using FGAs, 60.0% (nine out of 15) were diagnosed with MetS. Among the 117 participants using SGAs, 59.0% (69 out of 117) were diagnosed with MetS. Among the 55 participants using mood stabilizers, 65.5% (36 out of 55) were diagnosed with MetS, while 34.5% (19 out of 55) were not. Among the 41 participants using antidepressants, 63.4% (26 out of 41) were diagnosed with MetS. Though these were not statistically significant (Table 6).
Prevalence of MS in Various Psychiatric Conditions.
Relationship Between Metabolic Syndrome and Psychotropic Drugs.
Discussion
In the present study, 179 study subjects, who were diagnosed with a psychiatric diagnosis, were included. About 61.4% (54.4-68.4) with 95% CI of the 57 bipolar affective disorder patients had MetS, compared to 38.6% who did not. There is no statistically significant correlation between bipolar affective illness and MetS, according to the P value of .86. This suggests that these patients’ MetS may be influenced by variables other than their mental health.
Our research is consistent with that of D’Mello (2007), who discovered that a considerably larger percentage of patients with bipolar disorder, 56% met the criteria for MetS when hospitalized than when they were in community samples. The idea that bipolar disorder is linked to an increased risk of MetS is supported by the study’s finding that there is a positive correlation between the severity of mood disorders in these patients and the presence of metabolic conditions such as obesity, hypertension, dyslipidemia, and diabetes. 11
Our findings are consistent with the 2023 study conducted by Hemen Najar and associates. 12 In contrast to control subjects, a group of people with bipolar disorder diagnosed in this replication study had noticeably higher levels of cardiometabolic risk variables. The results highlighted the higher prevalence of diseases such as dyslipidemia and hypertension in bipolar disorder patients, which is consistent with the higher rates of MetS found in our own study.
About 62.2% of a group of 37 patients with a diagnosis of depression also had MetS. This demonstrates the comparatively high rate of MetS in depressed people, although it was not made clear how statistically significant this association was.
Our research findings are corroborated by Moradi et al.’s 2021 study, which was a meta-analysis of observational studies. They conducted a comprehensive analysis of 49 articles, including both cross-sectional and cohort studies, and found that the risk of developing MetS was 1.48 times higher in those with depression than in those without the condition. In keeping with our finding that 62.2% of patients with depression also had MetS, this study emphasized the strong correlation between depression and an elevated risk of MetS. 13 Our findings corroborate those of Pan et al. (2012), who investigated the reciprocal relationship between depression and MetS. According to the study’s findings, depression increases not just the risk of MetS but also the chance of getting depression. This confirms even more the high frequency of MetS among depressed people, as our study showed. 14
About 55.6% of the 72 schizophrenia patients who were part of the study had MetS. This result highlights a significant prevalence; however, it is impossible to determine the statistical significance of this correlation because no P value is provided. Our research confirms the results of Heald et al. (2017), 15 who found that, according to the IDF criteria, 67.6% of schizophrenia patients fulfilled the requirements for MetS.
We observed that FGA was being taken by 8.4% of the 179 mental health patients in our investigation. Sixty-one percent of these patients had MetS. Given that there is no statistically significant correlation between FGA use and MetS (P value of .91), it is possible that other factors played a role in these individuals’ development of MetS. About 179 psychiatric patients using SGA were included in our study; 65.4% of patients had SGA, and 59.0% had MetS. The lack of a significant correlation between the use of SGAs and MetS is indicated by the P value of .91, indicating that factors other than SGA use may also have an impact on the development of MetS.
Among the 179 patients with mental disorders in our study, mood stabilizer use accounted for 30.7% and 65.5% of these individuals had MetS. The lack of a statistically significant correlation between the usage of mood stabilizers and MetS is indicated by the P value of .22. About 41 people (22.9%) who were using antidepressants were found to be psychiatric patients according to our investigation. Of these, 15 (36.6%) of those patients did not have MetS, while 26 (63.4%) did. Our study’s P value of .48 suggests that there may be other factors that contribute to the development of MetS in these people because there is no statistically significant association between the usage of antidepressants and the existence of MetS.
Of the 179 mental health patients that were part of the research, 121 (67.6%) are now receiving treatment with just one medication, while 58 (32.4%) are receiving treatment with two or more drugs. This breakdown shows that a considerable proportion of patients need combination therapy to meet their complicated clinical needs, even though single drug therapy is more common. Single drug therapy is preferred because it is easier to manage, has a lower chance of drug interactions, and improves patient compliance, among other reasons.
Conversely, individuals with severe or unresponsive diseases could require combination medication therapy to address several symptoms or attain a more successful course of treatment.
A 2006 study by Correll et al. with 367 individuals receiving SGAs showed that 37.3% of patients had MetS, which was associated with a markedly increased risk of events related to coronary heart disease (CHD). Men (11.5% vs. 5.3%) and women (4.5%) had a greater risk. White racial background, waist circumference, and triglyceride levels were also substantially linked to the 10-year risk of CHD events. The study emphasizes the significance of the “hypertriglyceridemic waist” for identifying high-risk psychiatric patients and validates the high prevalence of MetS in patients receiving SGAs. 16
About 32 individuals (17.9%) in our study had type 2 DM, 26 individuals (14.5%) had hypertension, five individuals (2.8%) had dyslipidemia, and 25 individuals (14.0%) had hypothyroidism. A P value of less than .001 indicated that 28 (87.5%) of the 32 diabetes patients had MetS. Given that the majority of patients with type 2 DM (87.5%) also had MetS, the results show a noteworthy association between type 2 DM and MetS in mental patients. It is statistically significant that this correlation has a P value of less than .001. There was a 100% prevalence rate among the 26 hypertensive patients who were all diagnosed with MetS. In this specific cohort, there is strong evidence of a substantial association between MetS and hypertension, as indicated by the P value of less than .001. With a P value of .057, it was discovered that all five individuals (100%) with dyslipidemia had MetS. The P value of .057 indicates that the link is not statistically significant at the conventional .05 threshold, indicating a probable but not definitive relationship, despite the fact that all patients with dyslipidemia also had MetS. Of the 25 hypothyroid individuals, 12 (48.0%) did not have MetS, and 13 (52.0%) did. In psychiatric patients, the P value of .47 suggests that there is no statistically significant correlation between hypothyroidism and MetS. This study is limited due to a small sample size, a cross-sectional, and hospital-based design.
Our research highlights the importance of closely monitoring and treating metabolic health in mental health patients, especially those with type 2 diabetes and high blood pressure.
Conclusion
The prevalence of MS increased with age. The age of onset of MS was noted to be in the early third decade in patients with psychiatric conditions. The proportion of psychiatric patients with MetS was quite high. This could be due to altered lifestyle practices, eating habits, and psychotropic drugs. High prevalence of MetS among psychiatric patients demands integrated psychiatric-medical care. Further studies are required to ascertain the increased risk for MS among psychiatric patients and drug interactions for the same.
Moving forward, aggressive targeted evaluation and diagnosis, followed by comprehensive lifestyle counseling, are essential to mitigate the impact of MetS on individuals with psychiatric disorders and ultimately improve public health outcomes.
Footnotes
Acknowledgement
The authors sincerely thank the patients for their kind cooperation.
Authors’ Contribution
Declaration of Conflict of Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study protocol was reviewed and approved by the Institutional Ethical Committee of St. John’s Medical College and Hospital. Ethical clearance was obtained to ensure compliance with ethical standards in research.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from all participants after explaining the study’s purpose, procedures, risks, and benefits.
