Abstract
Introduction
The leading cause of death in developing nations is poisoning, which is a significant health care issue. In India, where the majority of people are connected to agriculture and industrial farming, acute pesticide poisoning is extremely common. Early diagnosis and treatment are the most important modes for preventing mortality. However, the only way to address this issue is through prevention.
Objectives
To describe clinical and epidemiological characteristics observed in individuals with organophosphorus (OP) poisoning at a tertiary health care center.
Materials and Methods
A cross-sectional study was carried out during the study period (October-November 2022) in a tertiary health care facility. Institutional Ethics Committee (IEC) clearance was obtained. Clinico-epidemiological features of patients presenting to tertiary care centers were evaluated using a pre-validated questionnaire. A descriptive study was conducted, and the data depict the clinical and epidemiological features of the study sample.
Results
A total of 39 subjects presented to the emergency room with clinical signs of OP poisoning during the study period. The preliminary data showed that 77% of the patients were young and had easy access to poison at home, and it was mostly suicidal (84.61%) in intention. They were admitted to a tertiary care facility and treated accordingly.
Conclusion
Clinical and epidemiological characteristics depend on the type, quantity of poison consumed, and type of exposure. So, the treating health care professionals should have appropriate knowledge toward the treatment of op poisoning as, time matters the most in saving lives.
Keywords
Introduction
Poisoning is an important health care problem in developing countries and leads to the highest mortality rate. According to the WHO, 0.3 million people die due to various poisoning agents annually. 1 Out of 500,000 suicidal deaths, 200,000 are due to organophosphorus (OP) poisoning, which is the leading cause of death according to the National Poison Information Center, India. 2 Acute pesticide poisoning is very common in India as, majority of people are related to agricultural and industrial farming, having easy accessibility to agents. 3 Early diagnosis and treatment are the most important modes for preventing mortality. Variability in clinical profile depends on the nature, type, and amount of poison, time gap between exposure and treatment. 4 In case of unknown history, diagnosis is made by observing the clinical characteristics that indicate the extent of the poisoning. 5 These clinical characteristics aid in determining the severity and prognosis. Therefore, it is critical for emergency physicians and public health professionals to understand the clinical characteristics of poisoning. 6 Hence, this study was taken up to describe clinical and epidemiological characteristics of patients who present to tertiary healthcare centers with OP poisoning.
Materials and Methods
It was a cross-sectional study conducted in a tertiary health center, during October-November 2022. Institutional Ethics Committee (IEC) clearance was obtained. During the study period, all patients who presented to the hospital’s emergency room with a history and clinical evidence of OP poisoning were considered eligible to participate in the research. According to recent studies and references cited, 2 it was evident that most of the patients (>90%) presented with clinical characteristics such as nausea and vomiting. So, by considering a prevalence P value of 30 and 15% of allowable error, a sample size of 37 was derived. Accordingly, during the study period, 39 patients who presented to the tertiary care facility were included as the study sample. Eligible patients or their legally appointed health care provider gave their informed consent (if the patient was unconscious). After immediate treatment at the emergency room, which included initial assessment, resuscitation when necessary to maintain airway, breathing, circulation, and completion of medicolegal formalities, a thorough assessment was then performed to identify the common clinical and epidemiological features of OP poisoning patients presenting to tertiary care facilities using a pre-validated questionnaire.
Statistical Analysis
The obtained data were imported into Microsoft Excel, and version 26 of the Statistical Package for Social Sciences was used for analysis. Data was subjected to descriptive analysis.
Results
During the study period, 39 patients in total arrived at the emergency department with clinical characteristics confirming OP poisoning. Table 1 displays the patients’ demographic information. Most of them belonged to the age group of 21-30 (56.41%), where the majority of them were male 53.8% working mostly as agricultural laborers 35.89% followed by farmers 25.64%, coolie 15.38%, homemakers15.38% and a few were students (7.69%). Details of poison intake were explained in Table 2. As most (84.61%) of them ingested poison with suicidal intention, it was accessed from their homes for 89.74%. Regarding the type of poison ingested, chlorpyriphos 28.20% was the most often one, followed by malathion 20.51% and parathion 17.94%, monochrotofos 10.25% and carbamate 5.12%. The quantity of poison consumed was 15-50 ml. The signs and symptoms with which the patient presented were illustrated in Table 3. In this study, nausea, vomiting, and salivation were mostly reported by 66.66% of patients, followed by nausea, vomiting, and giddiness among 25.64%, while miosis (33.33%) was the only sign observed in them. Two patients, or 5.12% of the total, passed away while they were in the hospital after being admitted. Among them, respiratory failure was the leading cause of death.
Basic Demographic Information on OP Poisoning Patients (n = 39).
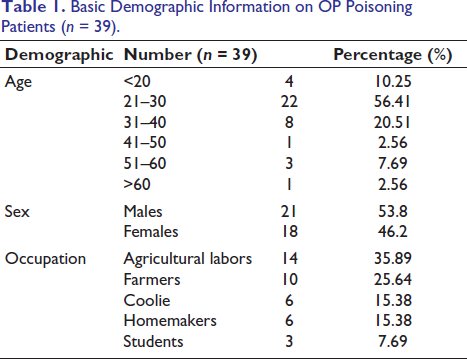
Details of Poison Intake.
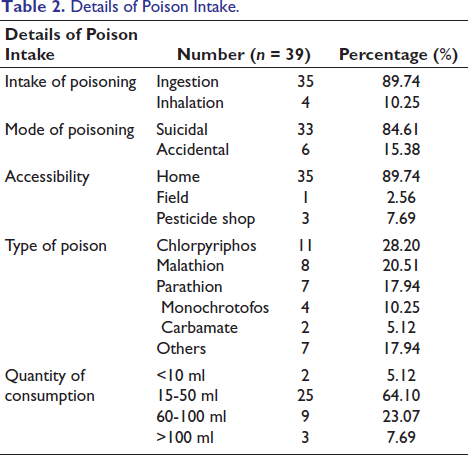
Clinical Features of Patients Suffering from OP Poisoning at Presentation.
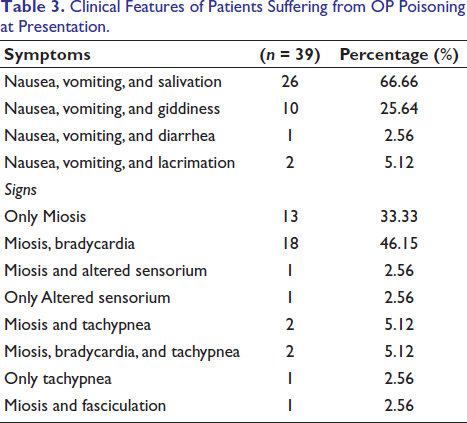
Discussion
In this study, the mean age of the study participants was 30.30 years (mean ± SD: 30.30 ± 10.64). Males and females were almost equally distributed. The majority of the study subjects were agricultural laborers 35.89%, who had more access to poisonous compounds at home 89.74%. Poisoning with suicidal intention was more common, 84.61% than accidental. This is similar to other studies conducted by Banerjee6, 7 and Rehiman. 8 Similarly, in a study by Jamil, similar findings were elicited where these agents were easily accessible and were frequently used as suicidal agents, especially by the uneducated. 9 In terms of poison type, the most often consumed was chlorpyriphos (28.20%), which was followed by malathion, parathion, monochrotofos, and carbamate. According to a study done in Nepal, dichlorfos, baygon spray, malathion, and methyl parathion were the most often used, with a 64.62% prevalence. Research carried out in Chennai also revealed that methyl parathion was the most prevalent toxin. 10 This discrepancy is mostly explained by the fact that many kinds are widely available. Similar to the study by Bajracharya, it was seen that the clinical presentation of the patient mainly depends on the type of poison, quantity consumed, exposure, and types of receptors stimulated at various sites of the body, and based on this, a diagnosis is made. 11 Miosis was the most frequent sign in the current study. Nausea, vomiting, and salivation were the most prevalent symptoms. The death toll in this study was 5.78% which was compared to the study done in Türkiye, 9.1% and in a study conducted by Jamil, where the death rate was high among OP poisoning patients, 67.6%. 12
Conclusion
The current research revealed that OP poisoning with suicidal intention was most commonly observed, mainly affecting the young. Nausea, vomiting, and salivation were the most common symptoms reported by the patients, while miosis was the only common sign interpreted. Most clinical and epidemiological characteristics depend on the type, quantity of poison consumed, and type of exposure. So, the emergency care department and all the health care professionals should have appropriate knowledge of the treatment of op poisoning, as time matters the most in saving lives.
Footnotes
Acknowledgements
Our sincere thanks to the Principal, Dr K. Chitti Narasamma, MS, for permitting us to conduct this study, HOD, Dr. P. Sudha Kumari, MD, and the faculty of the Department of Community Medicine, Kurnool Medical College, Kurnool, for their support and encouragement. We are grateful to the study participants for their cooperation.
Authors’ Contribution
First author, Dr Harika Annavaram, contributed to data collection, analysis, and interpretation of results, and preparation of the original manuscript draft.
Corresponding author, Dr S. Cynthia Subhaprada, contributed to the concept of the study, methodology, validation of the study tool, data collection, analysis, and interpretation of results, and final approval of the manuscript.
A statement that the manuscript has been read and approved by all the authors, that the requirements for authorship as stated earlier in this document have been met, and that each author believes that the manuscript represents honest work.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Institutional Ethics Committee clearance obtained (IEC No. 168/2022, dated October 26, 2022).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from all the participants in the study.
