Abstract
Objective
Radiology is important in modern medicine; therefore, adequate inclusion of radiology education in undergraduate medical schools is vital. This study aimed to (1) evaluate Palestinian medical students’ and interns’ perceptions of the adequacy of radiology training (curriculum content, mentorship, and integration into clinical practice) and (2) assess their self-reported confidence in applying core radiological skills (eg, image interpretation and selecting imaging modalities).
Methods
A survey-based cross-sectional study was conducted with 431 medical students and interns from 5 Palestinian medical faculties. An online questionnaire was created, reviewed for content validity, and shared with the recruited participants. Medical students and interns rated their perception of radiology training adequacy and self-reported confidence in applying radiological skills using a 15-item perception score and an 11-item confidence scale. Descriptive statistics, chi-square tests, independent t-tests, and Pearson correlation analyses were performed.
Results
The mean perception score was 10.19 ± 2.92 (68% of total), with 50.6% meeting the predefined threshold for adequate perceived training (≥11/15). Although 96.8% believed physicians should possess basic radiological skills, only 43.2% considered their training sufficient. Confidence was low, with 93.5% scoring below the predefined benchmark (>35/44). Clinical students demonstrated higher confidence than interns (P = .014). Perception and confidence were weakly but significantly correlated (r = 0.309, P < .001).
Conclusion
Palestinian medical students and interns acknowledge radiology's importance but believe they were inadequately trained in radiology and displayed low confidence levels in applying radiological skills. Improving radiology curricula, enhancing mentorship, and the inclusion of simulation-based learning are recommended to increase students’ confidence in applying radiological skills.
Introduction
Radiology plays a crucial role in modern medicine, contributing to the diagnosis and management of a wide range of medical conditions. 1 As imaging techniques and applications continue to evolve rapidly, radiological skills have become increasingly relevant for medical practitioners across various specialties and an integral part of daily clinical practice. 2 Despite this importance, radiology education is not uniformly incorporated into undergraduate medical curricula, and substantial variability exists in the structure, content, and duration of training.3,4 In some curricula, students receive limited exposure to radiological principles, which may result in reduced confidence when applying these skills in clinical settings. Evidence from multiple countries shows that a significant proportion of students perceive the integration of radiology training in their curricula as inadequate.5–7 while earlier exposure has been correlated with higher reported self-knowledge and greater positive perceptions of radiology as a medical speciality.2,5
The development of clinical competency follows the hierarchical structure of Miller's Pyramid, progressing from knows and knows how toward shows how and does. In Palestine, radiology teaching primarily occupies the cognitive levels of this model, with limited opportunities for students to apply knowledge through supervised interpretation or clinical decision-making. According to Bandura's self-efficacy theory, confidence develops through hands-on experience and feedback; however, these elements might not be adequately included in existing training formats. Together, these frameworks highlight the importance of assessing students’ perceived preparedness and confidence in radiological skills, as insufficient hands-on exposure may limit progression to higher competency levels.
While a unified and structured radiology curriculum is lacking in the medical schools in Palestine, radiology training is addressed in the Palestinian medical education curricula as a 2- to 3-week clinical rotation during the clinical phase of the undergraduate medical education program. Despite the central role of radiology in modern clinical practice, there is a lack of comprehensive data on the adequacy of radiology education and its alignment with the competencies required for effective clinical practice and postgraduate training. This gap limits informed curriculum development across different stages of medical education. Accordingly, this study aims to evaluate the perspectives of medical students and interns on the current state of radiology training in Palestinian medical schools and to explore their self-reported confidence in applying basic radiological skills.
Methodology
Setting and Study Design
The study was a cross-sectional, survey-based study design, conducted to (1) assess clinical phase medical students’ and interns’ perceptions of radiology training adequacy (curriculum content, mentorship, and clinical integration) and (2) evaluate their self-reported confidence in applying core radiological skills (eg, image interpretation, selecting appropriate imaging modalities). The targeted population consists of clinical-phase medical students and interns who have taken a clinical rotation in radiology at the Palestinian medical faculties, including An-Najah National University, Al-Quds University, Arab American University of Palestine, Palestinian Polytechnic University, and Hebron University. Including medical schools in the Gaza Strip was not possible at the time of the study. The Palestinian Medical Degree program spans 6 years of academic study followed by a 1-year postgraduate internship. The curriculum consists of 3 preclinical years focused on basic medical sciences and 3 clinical years dedicated to hospital-based clerkships and specialty rotations. The preclinical and clinical phases are administered by accredited Palestinian medical faculties, whereas the internship year constitutes a supervised clinical practice overseen by the Palestinian Medical Council in collaboration with the Ministry of Health.
Participants Recruitment and Data Collection
From October to December 2024, participants were recruited using a convenience snowball sampling approach distributed via student platforms, yielding 431 responses from medical faculties in the West Bank. Sample size was calculated using Raosoft® based on a population size of 3,000, a 95% confidence level, a 5% margin of error, and a 50% response distribution, resulting in a minimum required sample of 341. The obtained sample exceeded this requirement, hence providing adequate statistical power for analysis. Clinical-phase students who had not completed a radiology rotation were excluded.
Data Collection Tool
Data were collected through an anonymized English-language questionnaire designed specifically for this study and delivered electronically using Google Forms. Items were developed based on the 5C's of the Radiology Education Framework.8–12 The final instrument comprised 32 items covering demographic characteristics, perception of radiology training adequacy, and confidence in applying radiological skills. Content validity was confirmed by 2 board-certified radiologists who evaluated item clarity, relevance, and coverage of core learning domains. A pilot test with 42 students demonstrated acceptable internal reliability (Cronbach's alpha = 0.75). Minor modifications were made for clarity, and pilot responses (n = 42) were excluded from the final analysis.
Variables
Sociodemographic variables included age, sex, level of study (clinical phase student or intern), and type of residence (city, village, or refugee camp). Two primary outcome variables were assessed in this study. First, perceived adequacy of radiology training was evaluated using 15 dichotomous items, which were developed based on expert consensus and a review of key competencies outlined in radiology training guidelines. “Yes” responses were scored as 1 and “No” as 0, giving a total possible score range of 0-15. A score of ≥11 (≥70%) was considered indicative of satisfactory perception of radiology training adequacy. The 70% threshold was selected because it aligns with standards in medical education literature, where scores above this level are typically considered indicative of adequate mastery or exposure. This approach reflects Bloom-type cut-offs commonly used in medical education to classify acceptable levels of exposure and learning. Second, self-reported confidence in radiological skills was measured using 11 items presented on a 5-point Likert scale scored from 0 (not at all confident) to 4 (extremely confident), producing total scores between 0 and 44. The 11 items assessed various domains of radiological skills, including image interpretation, equipment handling, and patient positioning. A score of >35 (>80%) was defined as adequate confidence, based on established benchmarks in clinical education literature that commonly use 80% as an indicator of practical skill readiness 18-20, 21, 22, 23-26.
Statistical Analysis
Data analysis was conducted using SPSS version 26.0. Descriptive statistics (frequencies, percentages, means, and standard deviations) summarized sociodemographic variables, perception scores, and confidence scores. Inferential analyses included chi-square tests to assess associations between categorical variables (eg, sex, residence type) and perception/confidence categories, independent sample t-tests to compare mean scores between predefined groups (clinical phase students vs interns; males vs females), and Pearson correlation to evaluate the relationship between perception and confidence scores. A 5% significance level (α=0.05) was applied for all statistical tests.
Ethical Consideration
This study was approved by the Institutional Review Board (IRB) of An-Najah National University (Ref: Med.Oct.2024/29). Written informed consent was obtained electronically from all participants prior to study participation. The consent form was presented on the first page of the Google Form, where participants were required to confirm that they had read and understood the study information and agreed to participate voluntarily before proceeding to the questionnaire. No personal identifiers were collected, and all responses were anonymous. Participants were informed that their participation was voluntary and that they could withdraw at any time without consequences.
Results
Characteristics of the Students
Of the total 431 participants, 82.4% were undergraduate medical students in the clinical phase, and 17.6% were interns who had recently graduated from Palestinian medical schools. The mean age of the participants was 22.87 (±1.10). The majority of participants were females (63.1%), reflecting the actual sex distribution in Palestinian medical schools. A total of 53.8% of the participants were from urban areas, 41.5% from rural areas, and 4.6% from refugee camps. Table 1 summarizes the characteristics of the participants.
Characteristics of the Students who Participated in the Study.

Perception of the Students on the Adequacy of Radiology Training in Undergraduate Medical Education
The mean students’ perception score of radiology training adequacy was 10.19 ± 2.92 (95% CI: 9.92-10.47), corresponding to 68% of the total score of 15. A predefined threshold of ≥70% (≥11/15) was used to classify a positive perception, based on Bloom's cut-off and adjusted for the variability of the responses to the score items, with 50.6% of participants meeting this criterion. The mean perception score of radiology training adequacy did not differ between males and females (mean score [SD], 10.17 [± 2.99] vs 10.21[± 2.89], mean difference −0.04 (95% CI: −0.61 to 0.54); P-value .870). Interns scored slightly lower in perception than clinical-phase students (9.63 ± 3.00 vs 10.32 ± 2.90), and although the mean difference (−0.69; 95% CI: −1.41 to 0.04; P = .062) did not reach statistical significance, the CI suggests a subtle tendency toward lower perception among interns. Overall, 50% of participants demonstrated adequate perception (≥11/15). Adequacy rates were 42.1% in interns compared with 52.4% in students; while this difference was not statistically significant (difference = 10.3%, 95% CI: −2.1% to 22.2%; P = .103), the lower perception scores among interns may indicate a need for continued targeted educational interventions or support during the internship phase (Table 2).
Comparison of the Participants’ Perception Status With Sex and Level of Students.
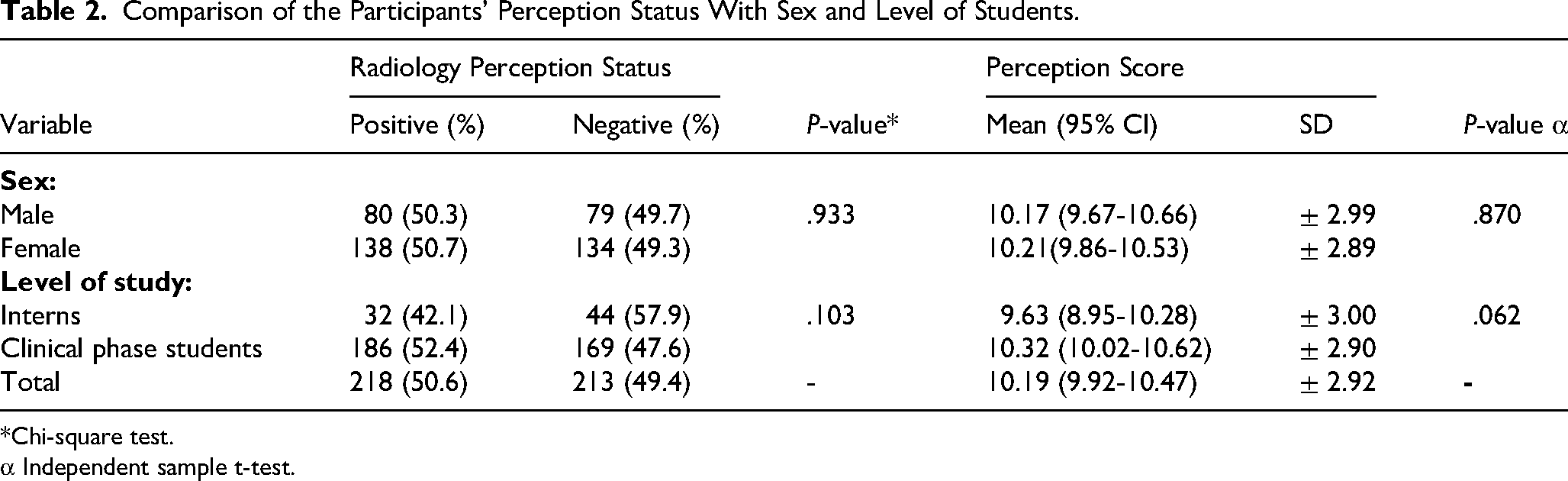
*Chi-square test.
α Independent sample t-test.
Awareness of radiology's importance was high (98.6%), and 96.8% believed all physicians should possess basic radiological skills. However, only 43.2% considered the amount of radiology training they received to be adequate. Most participants (63.6%) felt that radiology was sufficiently integrated into clinical rotations, while 62.2% believed mentorship within radiology teaching was adequate(Figure 1). Notably, interns were more likely than students to report sufficient mentorship (66.8% vs 40.8%). More interns also indicated interest in pursuing radiology as a specialty (71.1% vs 49.6%) (Figure 2). Supplemental Table 1 summarizes the participants’ responses to the questionnaire items.
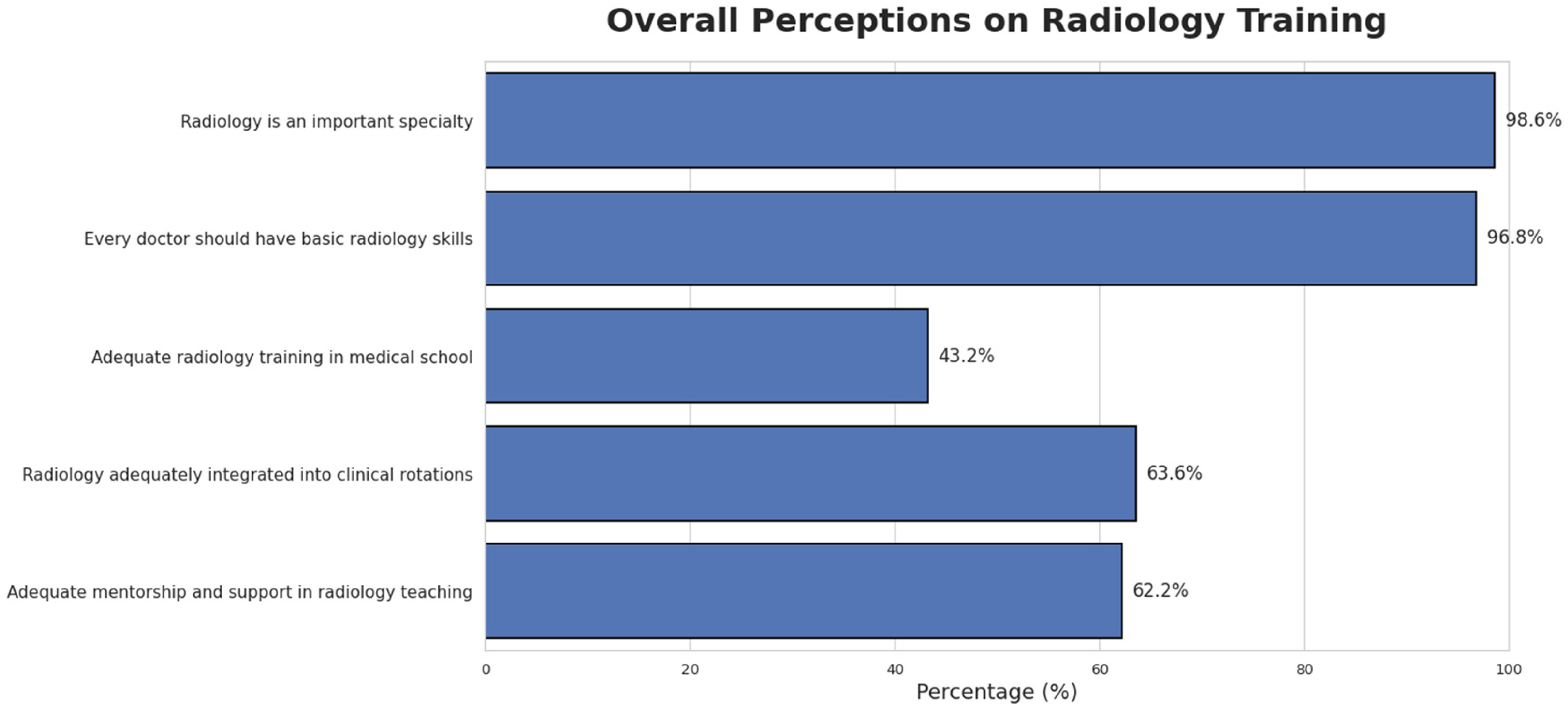
Participants’ overall perception of radiology training in Palestine. The results highlight a gap between the perceived importance of radiological skills and the adequacy of radiology training.

Comparison of clinical students’ and interns’ perception of radiology training.
Confidence of the Students in Applying Radiological Skills
The mean confidence score was 23.85 ± 6.92 (95% CI: 23.19-24.50), corresponding to 54.2% of the total scale. Using >35 as the threshold for adequate confidence, only 6.5% of participants met this level, indicating a low confidence in basic radiological skills. Males had a slightly higher mean confidence score than females (24.30 ± 6.58 vs 23.58 ± 7.11; mean difference = + 0.72, 95% CI: −0.63 to 2.08), although this difference was not statistically significant (P = .296).
Only 5.0% of males and 7.4% of females demonstrated adequate confidence (>35/44), representing a proportional difference of −2.4% (95% CI: −7.2% to 6.8%; P = .354). Clinical-phase students showed significantly higher confidence than interns (mean 24.16 ± 7.10 vs 22.38 ± 5.29; mean difference = 1.78, 95% CI: 0.07-3.49; P = .014). Adequate confidence was reported by 7.6% of clinical students compared to 1.3% of interns (difference = 6.3%, 95% CI: 0.1%-9.8%; P = .043) (Table 3; Figure 3).

Comparison of mean scores of confidence in radiological skills based on sex and level of training.
Participants’ Level of Confidence in Applying Basic Radiological Skills.

*Chi-square test.
α Independent sample t-test.
Bold values indicate statistically significant results (P < 0.05).
Confidence levels varied across radiological tasks. Around 47.7% of participants felt confident interpreting chest radiographs, and 38.5% were confident reviewing abdominal radiographs; however, confidence for recognizing life-threatening conditions on these radiographs was greater at 67%. The reported confidence was lower for musculoskeletal radiographs (33.2%), for identifying major abnormalities on head (26.9%) and thoracoabdominal (25.1%) CT/MRI studies, and for ultrasound interpretation (21.8%). Confidence was also low in selecting appropriate investigations (38.5%) and recognizing contrast media indications/potential side effects (33.9%) (Supplemental Table 2).
Effect of Students’ Perception of Radiology Training Adequacy on Their Confidence in Radiological Skills
Confidence was positively correlated with perception of radiology training adequacy, although the strength of this association was weak (r = 0.309, P < .001), as shown in Table 4 and Figure 4.

Scatter plot showing the relationship between confidence score (0-44) and perception score (0-15). The red dashed line represents the trendline for linear regression. A weak but statistically significant correlation was observed (r = 0.309, P < .001).
Correlation Between Students’ Confidence and Perception Scores.

*Pearson correlation test.
Discussion
Radiological competency is a clinical problem-based competency that requires medical students and practitioners to be able to incorporate the information obtained from their observation of imaging with their understanding of anatomy, pathology, and the patient's clinical information. 13 The importance of acquiring a basic level of radiological skills by medical students is non-questionable. 2 The students’ and interns’ confidence in applying radiological skills, particularly in advanced imaging, has been identified as inadequate, highlighting areas that need to be addressed in the current curriculum. These findings are consistent with studies conducted in Kuwait, 4 Saudi Arabia, 7 Turkey, 6 and Canada, 14 in which students similarly reported inadequacies in radiology education, particularly in practical training, and their impact on their confidence in applying radiological skills effectively.
Generally, the participants recognized the importance of developing radiological skills; however, they perceived that the amount of formal radiology training they received in the undergraduate training was inadequate. One factor is the limited time students spend learning radiology, which often emphasizes theory over practical experience in interpreting images. Without regular opportunities to work directly on real cases, students may become familiar with radiology but find it challenging to apply this knowledge in clinical settings. This general perception was common among the participants, regardless of their sex or level of training. This aligns with previous studies, in which more than half of the students reported insufficient radiology training coverage in the undergraduate curriculum despite its recognized importance.5–7,15,16 The consistency of these findings with data from other countries highlights an ongoing disparity between the recognized importance of radiology and the extent of training provided. This gap has significant consequences for clinical readiness, as newly minted interns are required to request, interpret, and respond to imaging results, especially in acute patient care settings. Accordingly, our findings underscore the necessity of structured curriculum development and enhanced instruction in applied radiology within Palestinian medical schools.
The participants expressed that some essential radiological topics were adequately covered in their formal training curriculum, such as the indications for various imaging modalities and the basics of radiation protection. On the other hand, the need for more practical, hands-on training and the lack of mentorship and support in radiology training were identified as key areas for improvement in the current formal radiology training. These results are in line with findings from a study conducted in Saudi Arabia, where medical students expressed satisfaction with theoretical components but identified a lack of practical opportunities as a key limitation. 7
Moreover, in a previous study conducted in Turkey, students reported limited interaction with radiologists during their clinical rotations, which was identified as a factor contributing to their low confidence in radiological skills. 6 The lack of mentorship and support in radiology training was recognized as a challenge, particularly among the interns. Interns frequently experience limited mentorship because they face greater responsibilities and receive less supervision than during their student clinical rotations. In Palestine, interns primarily serve as assistants within a national training program at government hospitals, which results in a service-based rather than systematically organized training environment. As a result, this may increase their perception of insufficient mentorship compared to the more structured guidance provided as medical students. It is important, however, to interpret these differences cautiously, as the smaller intern sample may have contributed to variability in estimates.
The participants recognized the need to integrate practical and simulation-based training into their curriculum. They believe more hands-on sessions, such as radiology labs and supervised image interpretation, should be included in their curriculum. They also acknowledged that the use of simulation-based learning resources, including virtual radiology cases and other digital tools, would help improve their radiology training. When combined with traditional didactic lectures, simulation-based learning is more effective than didactic lectures alone, providing a comprehensive learning experience that enhances knowledge retention and application skills 30. Therefore, these responses underscore the need to adopt a more interactive, practice-oriented approach to radiology training.
Generally, students and interns displayed an inadequate level of confidence in applying radiological skills. Surprisingly, clinical phase students scored higher confidence level scores than interns, suggesting a decline in confidence following graduation. This decline may be related to the transition from structured undergraduate teaching to real clinical environments where supervision is reduced and decision-making expectations increase. When the various aspects of confidence were assessed, the majority of students and interns had an inadequate level of confidence in applying radiological skills, especially when interpreting findings on ultrasound, CT scans, and MRIs. Additionally, most students and interns have inadequate confidence in selecting the most appropriate and cost-effective imaging modality and in using contrast media. Previous studies have reported similar findings, in which students have higher confidence in basic radiography but struggle with more complex imaging techniques.5,7 These findings underscore the need for targeted interventions to improve practical skills, particularly in more complex imaging techniques. Again, our findings align with earlier research, indicating that trainees often feel comfortable with plain radiographs but lack confidence with advanced modalities due to limited hands-on exposure. Structured case-based picture archiving and communication system (PACS) practice, simulation reporting sessions, and guided interpretation during clinical rotations are some of the educational activities that may help bridge this gap.
Clinical students and interns value the importance of developing essential radiological competencies; however, they are not sufficiently trained. This mismatch is reflected in their low level of confidence in applying essential radiological skills. The participants’ responses highlighted that their radiology training is limited to the lower levels of Miller's pyramid of clinical competencies development (knowledge and comprehension), emphasizing theoretical understanding rather than practical application. As suggested by the low confidence scores observed among Palestinian medical students and interns, this limited experiential learning may hinder students’ ability to transition from knowledge acquisition to skill performance.
Based on Bandura's theory of self-efficacy, confidence results from self-efficacy, fundamentally developed through mastery experiences and guided practice. For example, structured reporting sessions using PACS or supervised case-reading workshops could provide opportunities for mastery development, reinforcing skill acquisition beyond theoretical instruction. The lack of structured mentorship and limited exposure to hands-on radiology training restrict students’ opportunities to gain experience, leading to diminished self-efficacy and, consequently, lower confidence. One possible solution to address this gap is to ensure a curriculum that embeds longitudinal radiology exposure across clinical rotations, which can help support progression up Miller's pyramid and ultimately improve performance-level competency and confidence. This is further supported by the weak positive correlation observed between perception and confidence (r = 0.309). Therefore, strengthening experiential learning—through hands-on image interpretation, simulation-based teaching, and structured mentorship—may help shift learners from theoretical knowledge to higher-level performance stages in Miller's Pyramid. Such interventions are particularly relevant given the weak yet significant correlation, suggesting that improving perceived training adequacy alone is unlikely to elevate confidence without practical skill-building.
Among the limitations of this study is its observational nature and the absence of comparisons between the effects of different learning methodologies among Palestinian students. Additionally, in this study, including medical students from faculties in the Gaza Strip was not possible due to the destruction of universities and the interruption of the academic year. Moreover, the sampling technique and data collection method used in this study may have introduced a selection bias. All participants completed a mandatory radiology rotation; however, students and interns interested in radiology may be more likely to respond to the questionnaire than those who are not. Therefore, they may have been overrepresented. Furthermore, the subjective, self-report nature of the questionnaire may have introduced reporting and social desirability bias, especially regarding confidence levels. Finally, as perceived confidence may not correlate with objective radiological performance, the findings may not accurately reflect the actual objective diagnostic skills or ability; therefore, future studies should consider incorporating performance-based assessments (OSCE-style image interpretation or practical reporting tasks), which would provide a more robust evaluation of competency.
This study comprehensively assessed trainees’ perspectives regarding radiology training in Palestinian medical schools and their confidence in radiological skills, offering a multidimensional understanding of the outcomes of this training. Therefore, it addressed a significant gap in the literature. It included a sufficient and representative sample from the 5 primary medical schools in Palestine, enhancing the generalizability of the findings across educational settings. With 431 participants, which exceeded the minimum required sample size, the study had adequate statistical power to detect significant differences among subgroups. We developed a new questionnaire, based on the 5C's Radiology Education Framework and items of previously published questionnaires. The questionnaire was content-validated by radiology experts and pilot-tested, demonstrating acceptable internal consistency, ensuring reliability and validity. Finally, we provided data-based and action-oriented recommendations for curriculum improvement.
Based on the findings of this study, we provide recommendations to enhance radiology training in undergraduate medical schools in Palestine. First, we recommend that medical schools in Palestine conduct a curriculum reform, guided by Miller's Pyramid of clinical competencies development and Bandura's theory of self-efficacy, to integrate more hands-on training alongside traditional didactic teaching. Including more effective teaching methods, such as case discussions and problem-based learning, alongside didactic lectures, may improve the current radiology curriculum and, therefore, students’ and interns’ perceptions and confidence. Moreover, earlier integration of radiology education into curricula and enhancement of students’ hands-on experience are needed to address these gaps. Future research focusing on the objective evaluation of students’ and interns’ radiology knowledge and competency, rather than perceived confidence, would be particularly valuable. Additionally, future research could also compare the effects of various teaching formats (such as simulation, PACS-based reporting, and problem-based learning) and validate these methods with real clinical cases.
Conclusion
Palestinian medical students and interns identified critical gaps in radiology training, specifically in the coverage of essential radiological skills, the quality of mentorship, and the development of practical skills. Moreover, inadequate confidence in applying radiological skills was found among clinical phase students, with even lower confidence among interns. The findings of this study highlight the need for educational interventions to improve radiology training in undergraduate medical education in Palestine. The results underscore the importance of designing a competency-based curriculum for radiology training in the internship for Palestinian postgraduates. Introducing more innovative teaching methods and promoting mentorship and support in radiology education are expected to improve the students’ confidence in applying radiological skills. An assessment of the current radiology curriculum in undergraduate medical school and its efficiency is needed. Further studies can assess medical students’ and interns’ radiology knowledge and compare the efficacy of different teaching approaches.
Supplemental Material
sj-docx-1-mde-10.1177_23821205261441364 - Supplemental material for Confidence in Radiological Skills and Perceived Adequacy of Radiology Training Among Medical Students and Interns in Palestine
Supplemental material, sj-docx-1-mde-10.1177_23821205261441364 for Confidence in Radiological Skills and Perceived Adequacy of Radiology Training Among Medical Students and Interns in Palestine by Motaz Daraghma, Yazan Dumaidi, Ahmad Rjoub, Mohammad Nour, Dalya Abusnaina, Kholoud Jamal Hamarsheh, Lana Anwar Morshed, Mohammad Abuawad, Husameddin El Khudari, Saher S. Sabri, Gulraiz Chaudry, Ahsun Riaz, Osman Ahmed and Junaid Raja in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205261441364 - Supplemental material for Confidence in Radiological Skills and Perceived Adequacy of Radiology Training Among Medical Students and Interns in Palestine
Supplemental material, sj-docx-2-mde-10.1177_23821205261441364 for Confidence in Radiological Skills and Perceived Adequacy of Radiology Training Among Medical Students and Interns in Palestine by Motaz Daraghma, Yazan Dumaidi, Ahmad Rjoub, Mohammad Nour, Dalya Abusnaina, Kholoud Jamal Hamarsheh, Lana Anwar Morshed, Mohammad Abuawad, Husameddin El Khudari, Saher S. Sabri, Gulraiz Chaudry, Ahsun Riaz, Osman Ahmed and Junaid Raja in Journal of Medical Education and Curricular Development
Footnotes
Author Contributions
All authors have reviewed and approved the final version of the manuscript to be submitted.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Statement
The authors declare that they had full access to all of the data in this study and take complete responsibility for the integrity of the data and the accuracy of the data analysis.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
