Abstract
Objectives
This study aims to reform and optimize laboratory diagnostics education by developing an innovative teaching model based on M-STEM (Medical Science, Technology, Engineering, and Mathematics).
Methods
Students majoring in clinical medicine at South China University of Technology were included in this study and were randomly assigned to either a traditional group or an M-STEM learning group. The M-STEM instructional design emphasized interdisciplinary integration, role-based learning, and hands-on inquiry. Both quantitative data and qualitative feedback were collected to evaluate learning outcomes and teaching effectiveness.
Results
For laboratory lectures, the proportion of students who were very satisfied was significantly higher in the M-STEM group compared to the traditional group (79.3% vs 51.6%, P = .025). All participants in the M-STEM group expressed approval of the learning design, while those in the traditional learning group did not reach a full consensus. Both groups demonstrated a relatively low willingness to engage in course design (61.0%). A survey on students’ participation in curriculum design revealed that when confronting complex clinical problems, students were most inclined to seek assistance from professionals in the roles of doctors and laboratory technicians. When queried about which interdisciplinary integration is likely to offer greater support, students from both groups predominantly selected social psychology. Nevertheless, there existed a notable difference: the proportion of students in the traditional group who opted for economics was significantly higher than that in the M-STEM group (32.3% vs 10.3%, P = .04). In contrast, M-STEM students tend to focus more on integrating key disciplines and are reluctant to involve an excessive number of disciplines.
Conclusion
The M-STEM pedagogy can stimulate students’ interest and promote multidisciplinary integration, enabling learners to gain a deeper understanding of the disease and develop effective solutions.
Introduction
Johan Friedrich Herbart, the father of Western educational science, introduced the theories of psychology and philosophical ethics into education, creating a new paradigm that integrates education with other disciplines. A study analyzing the professional backgrounds of Nobel laureates from 1901 to 2018 revealed that only 31.0% of Nobel Prize winners in Physiology or Medicine held undergraduate degrees in medicine-related fields, while the percentages for Physics and Chemistry laureates with relevant undergraduate degrees were 55.4% and 59%, respectively. Notably, 49.5% (100 out of 202) of Nobel laureates in Physiology or Medicine had interdisciplinary professional backgrounds. 1 These findings highlight a trend: since 1901, interdisciplinary research achievements in natural sciences have increased annually, reaching 66.7% from 2001 to 2008. 2 Thus, interdisciplinary studies are becoming mainstream in medical education. Currently, the most typical and popular educational approach for interdisciplinary education is STEM (Science, Technology, Engineering, and Mathematics) education, which integrates knowledge and skills from Science, Technology, Engineering, and Mathematics to help students understand and apply interdisciplinary knowledge, cultivate comprehensive abilities, and solve practical problems, thereby laying a solid foundation for future career development.
A meta-analysis of 225 studies utilizing STEM active learning methods found that active learning can reduce course failure rates by about one-third. 3 Roberts and Harden also systematically summarized the application of STEM teaching in European medical education, noting significant impacts over the past 15 years, particularly in the United Kingdom and the Netherlands. STEM education methods have been endorsed by the Best Evidence Medical Education (BEME; www.bemecollaboration.org) and the International Recognition of Excellence in Education (ASPIRE; www.aspire-to-excellence.org) institutions. 4
Laboratory diagnostics is a crucial part of medical education, responsible for training students in diagnostic and analytical skills in the laboratory. This field encompasses various disciplines, including pathology, microbiology, immunology, and molecular biology. However, in everyday teaching at medical schools, some course content has not been updated promptly, struggling to keep pace with advances in medical technology. Traditional teaching methods like lecture-based learning (LBL) often fail to meet the demands for comprehensive talent in modern medicine.
The integration of clinical practice, patient engagement, and medical technology represents a significant trend in modern medical education. This integration not only improves teaching quality and effectiveness but also plays a pivotal role in cultivating well-rounded medical talents. This study applies the STEM education concept to create an educational reform practice for laboratory diagnostics courses—medical STEM (M-STEM). The application of the M-STEM concept in this field aims to enhance students’ comprehensive qualities and elevate the teaching quality of medical schools, thereby enabling students to better confront future challenges.

Design of M-STEM in the School-Based Curriculum for Laboratory Diagnostics.

Comprehensive Quality Control System for the Full Process Design of the Laboratory Diagnostics Curriculum.
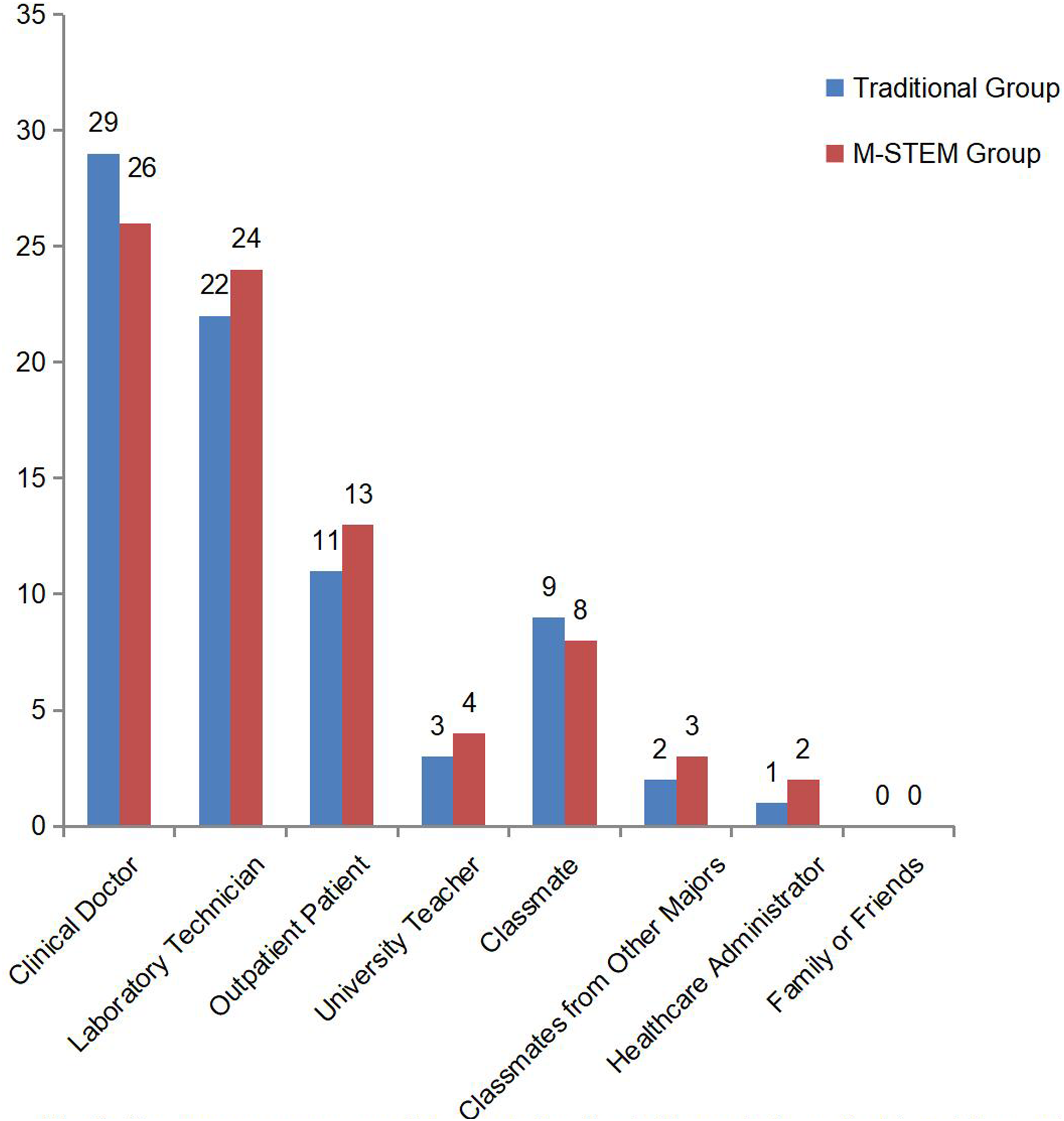
Role selection in integrated teaching teams.
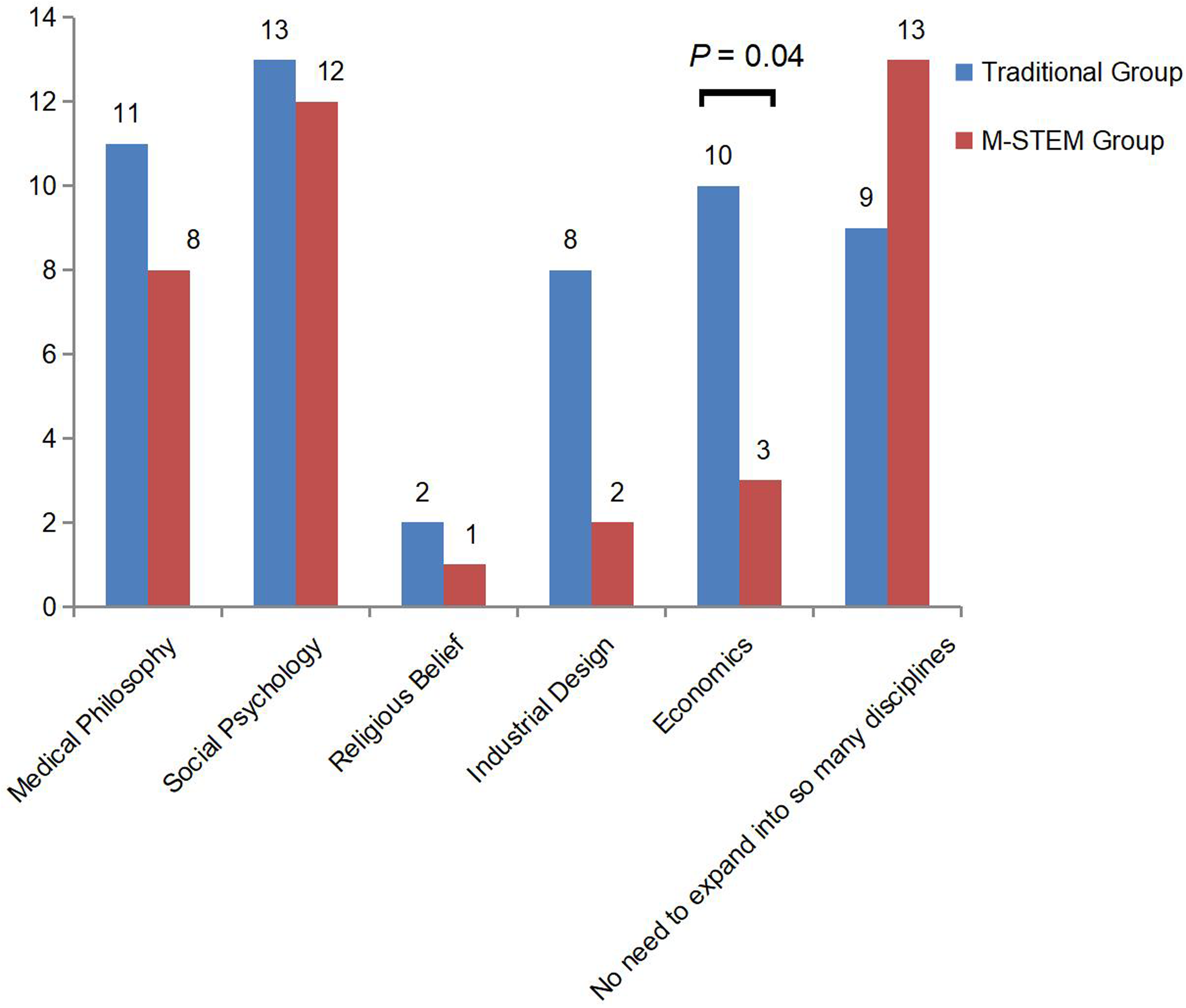
In Your Opinion, Besides Clinical Integration, What Other Discipline Should Be Involved in Molecular Diagnostic Science?
Methods
Research Subjects
This is a randomized interventional study with a duration of 3 months, which utilized the laboratory diagnostics course for clinical medicine majors at the Medical School of South China University of Technology as a platform to implement M-STEM educational programs. The compulsory course was conducted at Guangdong Provincial People's Hospital in 2023, and all 64 students were included in this study. The following criteria were established. Participants must meet all of the criteria.
Inclusion criteria:
Identity and course alignment: Being a formally registered undergraduate student and having enrolled in core M-STEM-related courses in the current semester. This ensures that participants have basic needs and eligibility to participate in the study intervention. Grouping and intervention accessibility: Being assigned to the M-STEM group learning cohort through random grouping and explicitly expressing willingness to abide by the basic rules of group learning. Participants must have no explicit refusal or resistance to participate in the intervention. Data provision capability: Possessing basic ability to complete questionnaires, and committing to cooperate in the collection of relevant data throughout the entire study cycle. Participants must have no explicit time conflicts that may affect their participation (eg, long-term leave, fixed-schedule off-campus tasks, etc).
Exclusion criteria:
Withdrawal from intervention after grouping: After being randomly assigned to the M-STEM group learning cohort, voluntarily withdrawing from group learning due to personal reasons (eg, subjective unwillingness to continue participation, unresolved time conflicts) or objective factors (eg, transfer to another university, suspension of studies); or having an accumulated absence from group learning sessions exceeding 3 times, resulting in failure to fully receive the intervention. Invalid questionnaire data: Showing obvious inconsistencies in post-course questionnaires (eg, selecting the same rating for questions with opposite meanings), missing key information, or having regularized response patterns (eg, selecting the same option for all questions). Such data will be confirmed by the research team as unusable for analysis.
The reporting of this study conforms to the CRe-DEPTH statement (The Criteria for Reporting on Development and Evaluation of Professional Training interventions in Healthcare) 5 (see Supplemental Material 1).
Students were randomly divided into 2 groups: a traditional teaching group and an M-STEM teaching group, and an experimental comparison was conducted between the 2 groups. The new M-STEM model is implemented by the experimental diagnosis teaching base within the diagnostics course, which integrates clinical cases and laboratory practices. The director of the base serves as the general supervisor, designing the curriculum framework and overseeing its implementation across all teaching modules. To ensure objectivity, the secretary designed and conducted curriculum effectiveness surveys using a standardized questionnaire. Each group comprised 3 teachers. In the M-STEM group, one teacher oversaw quality management according to the curriculum standards, one coordinated theoretical and experimental teaching materials, and one facilitated case-based learning sessions. However, the traditional team focused solely on lecture design and exam development as specified in the curriculum framework, with each teacher responsible for a separate module.
Research Methods
Design of M-STEM in the School-Based Curriculum for Laboratory Diagnostics
The M-STEM curriculum's 3-dimensional integration is divided into 8 steps:
Problem Orientation: Centered on the patient's chief complaint, guiding students to engage in comprehensive discussions and practices centered on various clinical elements. Role Assignment: Undergraduate students are randomly assigned to 1 of 3 roles (doctor, patient, technician) and form learning teams based on these roles. Theoretical Learning: Each group immerses in the professional knowledge and cutting edge so that they can master skills required for their assigned roles in clinical practice. Interdisciplinary Integration: Organize each group into multidisciplinary team (MDT) roundtable meetings to facilitate comprehensive discussions and the integration of knowledge from different perspectives. Solution Development: Establish diagnostic and treatment goals, with the technician group managing all aspects of the diagnostic process, followed by the doctor group formulating treatment plans, monitoring clinical efficacy, and assessing prognosis. Case Review: Conduct a review session after completing the laboratory diagnostics case study to analyze and reflect on the learning process and outcomes. Role Rotation: Rotate students among different roles based on their performance, allowing them to provide feedback on their previous roles and gain insights from other perspectives. Teacher Summary: Summarize the cases and integrate them into the high-quality course library for the laboratory diagnostics curriculum.
This course design (see Figure 1) has yielded successful results in our teaching on the topic of clinical practice of molecular diagnostics, with students providing positive feedback and demonstrating significant effectiveness in the classroom.
Full Process Design of the Laboratory Diagnostics Curriculum
The curriculum design for laboratory diagnostics requires comprehensive quality control throughout the entire process (see Figure 2). We have divided the curriculum into 5 stages: (1) confirmation of lecture topics, (2) discussion of lecture formats, arrangement of teaching duties, (3) formal implementation of lectures, and (4) post-lecture review. At each stage, we assign lecture responsibilities, prepare teaching materials, and establish key teaching indicators. Each stage allows for further examination of the lecture topics to verify their suitability for the long-term development of laboratory diagnostics. Finally, we evaluate teaching quality using these key indicators aimed at creating innovative, interactive, and high-quality courses.
The quantitative evaluation of courses encompasses several key areas: course design, teacher performance, content innovation, and student performance. All evaluations are based on a 1 to 10 point scale (1 being the lowest and 10 being the highest). The policy of real-time scoring at various stages enables immediate adjustments to the course content. Courses receiving consistently low overall scores will either be canceled or placed into a pending improvement evaluation system.
Construction of the Teaching Model: Application of Clinical Practical Teaching Based on the M-STEM Method
This study used laboratory diagnostics in the clinical molecular division of the laboratory department as a teaching template. Students (a total of 64) were randomly divided into 2 groups with an approximate 1:1 gender ratio: the traditional teaching group (32 students) and the M-STEM integrated teaching group (32 students). The traditional teaching group employed the “six-step method,” which includes teaching the following steps: (1) outlining the course, (2) creating lecture presentations, (3) preparing experimental materials, (4) lecturing in person, student examinations, and (5) grading by the instructor. 6 In contrast, the M-STEM group followed the previously described course design and teaching process. Each group was guided by a different instructor.
Other Methods
Interviews
Semi-structured interviews were conducted with students, teachers, and clinical staff to gather in-depth qualitative data on their experiences and perceptions of the M-STEM integrated teaching model. The interviews focused on multiple aspects such as the clarity of teaching objectives, the effectiveness of the integration between clinical and laboratory learning, the development of problem-solving skills, and the overall satisfaction with the teaching methods.
Teaching Observations
Systematic classroom observations were performed to assess the implementation fidelity of the M-STEM teaching model. Observers recorded the frequency and quality of interdisciplinary interactions, the level of student engagement, and the application of theoretical knowledge in practical scenarios. Specific metrics included the number of student questions, participation in discussions, and the ability to connect laboratory results with clinical cases.
Performance Assessments
Quantitative data were collected through performance assessments, including exams, practical tests, and project evaluations. These assessments were designed to measure students’ knowledge acquisition, practical skills, and ability to apply interdisciplinary approaches to problem-solving. A comparative analysis between the traditional teaching group and the M-STEM group was conducted to evaluate differences in learning outcomes.
Exam Scores
Both groups took the same exams covering theoretical knowledge and practical skills. Scores were compared to determine the effectiveness of the M-STEM approach in improving academic performance.
Practical Tests
Students’ proficiency in laboratory techniques and diagnostic procedures was assessed through hands-on practical tests. These tests evaluated their ability to perform clinical laboratory operations accurately and efficiently.
Project Evaluations
Group projects were assessed based on criteria such as the integration of clinical and laboratory knowledge, creativity in problem-solving, teamwork, and presentation skills. These evaluations provided insights into students’ abilities to work collaboratively and apply their learning in real-world contexts.
Statistical Analysis
This study is primarily descriptive research, which collects single-choice or multiple-choice answers through questionnaires and calculates the proportion of each option in the 2 groups. For data involving comparisons between the 2 groups, chi-square analysis is performed using SPSS 26.0, and P < .05 is taken as the criterion for statistically significant differences.
Results
Collection of Teaching Effectiveness Evaluation Questionnaires
Course Satisfaction Survey Results
This study used a blind method to survey all students (a total of 64) with an 8-question teaching questionnaire. We received 60 valid questionnaires; 4 were deemed invalid due to contradictory answers to questions 3 and 6. The proportion of students in the M-STEM group who were very satisfied with theoretical lectures was higher than that in the traditional group (58.6% [17/29] vs 41.9% [13/31], P = .196). For laboratory lectures, the number of students who were very satisfied was significantly higher in the M-STEM group compared to the traditional group (79.3% vs 51.6%, P = .025). In the traditional group, one student held the view that this course could not enhance students’ clinical thinking, while 4 students believed it failed to improve clinical skills. In contrast, all participants in the M-STEM group expressed approval. Except for one student, both groups felt that the integration of laboratory diagnostics with clinical cases was an excellent teaching method. However, both groups showed a relatively low willingness to participate in course design, with only 61.3% (19/31) and 62.1% (18/29) expressing interest for the traditional group and the M-STEM group.
Survey on Willingness to Participate in the Integrated Curriculum System
From the survey on the willingness to participate in the integrated curriculum system, we found that in the M-STEM group, all but one student believed that integrated teaching was enlightening for their course understanding. Additionally, 82.8% (24/29) of the students felt it helped them understand clinical laboratory operations, and 41.4% (12/29) of the students believed that they had gained significant improvement in the following 3 aspects
When choosing roles in the integrated teaching teams (see Figure 3), clinical doctors and laboratory technicians were the most selected roles by students in the 2 groups (93.5% vs 89.7%, 71.0% vs 83.0%), followed by outpatients and classmates. Regarding the choice of disciplines for integrated teaching (see Figure 4), both professional groups predominantly selected social psychology (41.9% vs 41.4%). However, the number of students in the traditional group who chose economics was significantly higher than in the M-STEM group (32.3% vs 10.3%, P = .04). Moreover, 44.8% of the M-STEM group felt that it was unnecessary to expand into so many disciplines, compared to only 29.0% in the traditional group (P = .21).
Collection of Teaching Effectiveness Evaluations (Interviews, Teaching Observations, Performance Assessments, Etc)
The collected data from interviews, teaching observations, and performance assessments revealed several key insights:
Student Engagement: The M-STEM group showed higher levels of engagement and participation in both theoretical and practical sessions compared to the traditional group. Interdisciplinary Skills: Students in the M-STEM group demonstrated a better understanding of the integration between clinical and laboratory sciences, as evidenced by their ability to apply interdisciplinary approaches to diagnostic problems. Satisfaction and Motivation: Interviews indicated that students in the M-STEM group were more satisfied with the teaching methods and felt more motivated to learn due to the interactive and integrative nature of the curriculum. Performance Outcomes: Quantitative assessments indicated that the M-STEM group outperformed the traditional group in both theoretical exams and practical tests, suggesting that the integrated teaching model effectively enhances learning outcomes.
Discussion
Major Findings
The study demonstrates that the M-STEM integrated teaching model offers significant advantages over traditional teaching methods in laboratory diagnostics education. It enhances student engagement, satisfaction, and interdisciplinary understanding. By effectively integrating clinical, patient, and medical technology roles, M-STEM provides a comprehensive framework that better prepares students for the complexities of modern medical practice. Moving forward, medical schools should consider adopting and refining M-STEM approaches to improve the quality of medical education and address the evolving needs of healthcare.
Current State of Undergraduate Teaching in Laboratory Diagnostics
The current approach to undergraduate teaching in laboratory diagnostics primarily follows a model of basic theoretical lectures, laboratory teaching, and clinical internships. This traditional teaching mode (LBL) is predominantly teacher-centered, with limited active participation from students. Typically, medical undergraduates learn theoretical knowledge in university settings and then move on to clinical internships at a later stage. This separation between theory and practice often leads to a disconnect, causing students to struggle in applying theoretical knowledge to clinical demands, particularly during frequent departmental or intra-departmental rotations.
Emerging Educational Reforms in Medical Schools
In response to these challenges, medical schools globally are adopting innovative educational reforms. These include project-based learning, problem-based learning, team-based learning (TBL), case-based learning (CBL), and research-based learning (RBL). Each of these methods has unique teaching effects and challenges, suited to different educational goals and needs. While these methods provide an attractive alternative to traditional single-theme lectures, they often lack a comprehensive approach from a curriculum design perspective. Interdisciplinary transplantation of teaching methods significantly addresses this gap.
Effectiveness of M-STEM in Laboratory Diagnostics Education
Our study revealed that students in the M-STEM group expressed significantly higher satisfaction compared to those in the traditional group, with 96.6% of the students finding this teaching method to be inspirational. The traditional teaching of laboratory diagnostics requires active participation from doctors, patients, and medical technicians. Given the diverse yet interconnected nature of various departments and diseases, many patients often have multiple concurrent illnesses, highlighting the need for interdisciplinary diagnostic approaches.
Student Engagement and Satisfaction with M-STEM
The M-STEM integrated teaching model proved more appealing to students. Survey results indicated a significantly higher satisfaction rate among students in the M-STEM group compared to the traditional group. Clinical doctors and laboratory technicians were identified as the most critical roles in integrated teaching, aligning closely with clinical practice. However, 45.0% of the students in the M-STEM group felt that expanding into too many disciplines was unnecessary, suggesting that integrating 3 or fewer disciplines is optimal. Excessive expansion could overwhelm students, leading to increased workload and potential negative effects.
Development and Future Directions of M-STEM Teaching Methods
Over the past decade, M-STEM teaching methods have undergone significant evolution. Initially focused on the integration of basic interdisciplinary knowledge, these methods now emphasize deep interdisciplinary integration and practical application. Advances in technology and changing student needs have driven the evolution of teaching philosophies, technological applications, curriculum content, the breadth of interdisciplinary integration, and the diversification of teaching modes. These changes enable M-STEM teaching methods to better meet the demands of modern medical education, equipping students with the skills to solve complex medical problems and adapt to the continually evolving medical technology and industry needs.
Today's M-STEM teaching incorporates more complex projects, making sophisticated medical education feasible. Examples include developing intelligent medical devices, precision medicine solutions, and the application of big data analysis in clinical decision-making. Advanced technological tools and digital resources, including virtual reality (VR), augmented reality (AR), artificial intelligence (AI), and big data analytics, have significantly enhanced the interactivity and realism of teaching. Future curricula may extensively use VR for medical simulation training, AI for data analysis and disease prediction, and AR for intricate anatomy teaching.
The M-STEM teaching model has also become more diverse, incorporating project-driven, problem-solving, and practical application-based methods. There is a greater emphasis on practical projects and teamwork to enhance students’ hands-on skills and innovative thinking. Current teaching modes include interdisciplinary team projects, practical medical technology development, and virtual simulation training, all aimed at improving students’ practical application abilities and innovative capacities.
Practical Significance of M-STEM Teaching Methods in Medical Education
The M-STEM teaching method holds substantial practical significance in the field of medical education both domestically and internationally. By integrating interdisciplinary approaches and practical applications, this teaching method significantly enhances students’ comprehensive abilities, innovative thinking, and practical skills. It drives the reform and development of medical education, fostering high-quality talents that meet the demands of future medical advancements. Promoting and deepening the M-STEM teaching method can further improve the quality and effectiveness of medical education, providing a solid foundation for the development of modern medicine.
Enhancing Comprehensive Abilities
The M-STEM teaching method helps students develop systematic medical thinking and the ability to apply interdisciplinary knowledge. This comprehensive training enables students to not only understand medical theories but also apply modern technological tools to solve real-world problems. For example, through the STEM program at Harvard Medical School, students learn genomics, data analysis, and bioengineering, applying these interdisciplinary skills to medical research and clinical practice. 7
Promoting Innovation and Research
The M-STEM teaching method encourages students to engage in innovative thinking and research exploration throughout their studies. Through interdisciplinary projects and practical applications, students can identify and solve new medical problems, advancing medical science. At Stanford University School of Medicine, the STEM curriculum involves students in interdisciplinary research projects, such as developing new medical devices and biomaterials, fostering their research capabilities and innovative thinking. 8
Improving Practical Skills
The M-STEM teaching method emphasizes practice-oriented learning, enhancing students’ clinical skills and technical application abilities through hands-on projects and practical exercises. This practice not only includes the application of medical technology but also involves engineering design and data analysis. Tsinghua University School of Medicine, in collaboration with the School of Engineering, offers a STEM program where students design and develop medical devices, learning and applying interdisciplinary knowledge through practical work, thereby improving their practical skills. 9
Driving Medical Education Reform
The application of the M-STEM teaching method in medical education promotes the reform of traditional teaching models. By introducing modern technology and interdisciplinary projects, it breaks down barriers between disciplines, making teaching content richer and more diverse, thus enhancing students’ interest and engagement. Imperial College London, through its science, technology, engineering, mathematicsand medicine (STEMM) program, has reformed traditional medical education by incorporating courses in programming, AI, and bioengineering, cultivating students’ interdisciplinary thinking and technical application abilities. 10
Cultivating Medical Talents for Future Development
The development of modern medicine requires medical professionals with interdisciplinary knowledge and innovative abilities. The M-STEM teaching method cultivates students’ comprehensive abilities and practical skills, enabling them to adapt to and lead future medical advancements. At the National University of Singapore Medical School, the STEM program equips students with knowledge in bioinformatics, medical data analysis, and intelligent medical technology, preparing high-quality talents for future medical development. 11
Facilitating International Cooperation and Exchange
The global application of the M-STEM teaching method promotes international cooperation and exchange in medical education. Through international projects and collaborative research, students gain advanced medical knowledge and technologies, enhancing their international perspectives and collaborative abilities. The Sino-American “Future Medical Engineers Program” involves cooperation between universities in China and the United States, allowing students to participate in international research projects and exchange activities, thereby improving their international cooperation skills and cross-cultural understanding. 12
In conclusion, the M-STEM teaching method has significant practical implications in the field of medical education, both domestically and internationally. By integrating interdisciplinary approaches and practical applications, it enhances students’ comprehensive abilities, innovative thinking, and practical skills, driving the reform and development of medical education, and cultivating high-quality talent that meets the demands of future medical advancements. Promoting and deepening the M-STEM teaching method can further improve the quality and effectiveness of medical education, providing a solid foundation for the development of modern medicine.
Challenges and Solutions of the M-STEM Teaching Method
Interdisciplinary teaching integration can break down professional barriers, allowing individuals with relevant experience both within and outside the profession to participate in teaching activities, thus serving as an important source of educational innovation. The STEM education method is an active learning approach. Professor Tom Duff from the University of the West of Scotland's Paisley Campus found that team-based active learning methods can improve learning performance by 20% compared to conventional teaching methods. 13
Educational transplantation is a popular teaching method today. For example, the differentiated education model from the United Kingdom has been transplanted to compulsory education in China, Peking Opera teaching methods have been transplanted to Cantonese Opera, and clinical linguistics teaching methods have been transplanted to Chinese language teaching. However, according to our existing research, examples of teaching that achieve true interdisciplinary integration (transplanting beyond the educational system) are very rare.
There is a noticeable gap between Chinese medical schools and renowned international medical schools in terms of the application of the M-STEM teaching method. These differences are mainly reflected in teaching concepts, technological applications, course content, teaching methods, faculty quality, and student needs.
Challenges Faced
Limited Implementation of STEAM Courses in China
According to our understanding, STEM courses are rarely implemented in various educational fields in China, particularly in daily teaching activities. However, since 2015, the Ministry of Education has encouraged the exploration of new technological methods in teaching. In its “Guidance on Deepening Education Informatization During the 13th Five-Year Plan” (Draft for Comments), the Ministry stated: Regions with the necessary conditions should actively explore the daily application of new technological methods in teaching processes, effectively use information technology to promote the construction of “mass entrepreneurship spaces,” and explore new educational models such as STEAM (Science, Technology, Engineering, Art, and Mathematics) education and maker education.
14
In 2017, the Ministry of Education issued the “Compulsory Education Primary School Science Curriculum Standards,” which for the first time clearly defined STEAM. The same year, a report titled “China's STEAM Education Development Report,” co-published by Beijing Normal University, Beijing Guoxin Shijiao Consulting and Research Institute, and the Education Management Consulting Center of the Ministry of Education, noted that STEAM was not widely practiced in the daily teaching of Chinese universities but more often appeared as club courses and elective courses (accounting for 72.0%). 15
Unique Characteristics of Higher Education in China
One distinguishing feature of higher education compared to primary and secondary education is its openness and focus on innovation and development, rather than simple knowledge transmission. This is precisely where STEAM's strengths lie. Current interdisciplinary learning in universities is more formal, such as using analogy and association methods. These methods can visually represent natural phenomena that cannot be directly observed, creating tangible representations in students’ knowledge systems and thus reinforcing learning memory. However, such simple transplanted teaching does not integrate the academic system.
Differences in M-STEM Application Between Domestic and International Medical Schools
Independent Academic Language Systems: Each discipline has its unique academic language system. Connecting these disciplines requires educators to construct a rich, multi-node learning network where different nodes can connect and interact, forming a cohesive knowledge system. 16
High Qualifications Required for Instructors: Cross-disciplinary teaching transplantation places high demands on instructors’ personal qualities. Teachers must be familiar with the intrinsic attributes of both disciplines and be able to link them through external forms, highlighting their commonalities.
Audience Limitations: This method is challenging to implement universally. Students unfamiliar with either discipline might face confusion and disorder in their knowledge systems. However, for specific target groups, it can be highly attractive and effective.
Solutions to Challenges
Institutional Level
To enhance the application of the M-STEM teaching method, medical schools in China should:
Promote Interdisciplinary Concepts: Strengthen the promotion of interdisciplinary concepts within the curriculum, optimize course design, and develop and implement more interdisciplinary courses that integrate medicine, technology, engineering, and mathematics. Introducing real-world projects and cutting-edge technology applications will allow students to apply their knowledge in practical settings.
Create Interdisciplinary Collaboration Platforms: Encourage collaboration among experts in medicine, engineering, technology, and other fields for research and teaching activities. Provide systematic multidisciplinary training for faculty, covering the latest technologies, teaching methods, and interdisciplinary integration knowledge. Encourage teachers to participate in academic exchanges and training both domestically and internationally to enhance their interdisciplinary teaching capabilities.
Diversify Teaching Methods: Additionally, teachers should adopt diverse teaching methods, focus more on students’ practical needs and feedback, and enhance the interactivity and practicality of teaching to better engage students and improve learning outcomes.
Clinical Level
Encourage Clinician Involvement: We encourage clinical doctors to participate in teaching, strengthening the connection between clinical practice and research. By sharing their practical experiences and clinical cases, clinicians can help students apply theoretical knowledge to clinical practice more effectively.
Medical Technology Level
Incorporate Advanced Medical Technologies: We should introduce advanced medical technologies and equipment into the teaching process to help students master the latest technological applications and understand their importance in real medical scenarios. The use of the latest medical imaging technologies, intelligent diagnostic systems, and other equipment in teaching will enhance students’ technical skills.
Facilitate Collaboration Between Medical Technologists and Educators: Promoting collaboration between medical technologists and educators will improve students’ understanding and application of medical technologies. Medical technology experts should be invited to participate in course instruction, introducing the latest technologies and application cases.
Patient Level
Enhance Patient Involvement in Teaching: Enhancing patient involvement in the teaching process is crucial. Utilizing real patient cases for teaching will help students better understand the realities of diseases and treatment outcomes. Gathering patient feedback on the medical process and outcomes can serve as an important basis for optimizing teaching content and methods. This will also improve students’ sensitivity to patient needs. For instance, organizing patient lectures or case-sharing sessions will allow students to learn about patient experiences and requirements, enhancing their clinical decision-making skills.
Data Saturation Limitation
This study was our first course exploration; hence, it was piloted among a small student cohort (n = 60) initially. The limitation in the number of students may lead to insufficient effectiveness in the result analysis. Nonetheless, teaching reform work must push forward steadily and could not be achieved overnight. Thereafter, we will make targeted adjustments based on the outcomes and limitations of the courses and then continuously promote the M-STEM teaching approach to more students and other courses.
By addressing these challenges with targeted solutions, the M-STEM teaching method can be implemented more effectively, thereby amplifying its impact on medical education both domestically and internationally. These improvements will help enhance the quality of medical education and the comprehensive abilities of students, better preparing them to face future challenges in the medical field and address the complex issues of modern medicine.
Conclusion
This study, grounded in the M-STEM educational philosophy, innovatively adopted an interdisciplinary teaching method that stimulated students’ interest in learning. The integration of clinical practice, patient care, and medical technology is of paramount importance in medical education. This integration not only enhances students’ comprehensive abilities, practical skills, and innovative thinking but also promotes patient-centered healthcare, improves teaching outcomes, and better equips students to meet the demands of modern medical practice. By leveraging successful experiences and best practices from both domestic and international contexts, we can further advance this integration in medical education. This will lay a solid foundation for cultivating high-quality medical professionals, introduce new directions and impacts in the teaching and research of future medical sciences, and provide a theoretical basis and practical framework for designing future teaching objectives, methods, and curricula.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251384390 - Supplemental material for Optimizing Laboratory Diagnostics Education: Research on the Doctor-Patient-Technician Integrated Teaching Model Based on Medical STEM Concepts
Supplemental material, sj-docx-1-mde-10.1177_23821205251384390 for Optimizing Laboratory Diagnostics Education: Research on the Doctor-Patient-Technician Integrated Teaching Model Based on Medical STEM Concepts by Zhengkang Li, Liwen Ma, Jinxin Lai, Xinqiang Zhang, Chengyuan He, Yuwei Di and Bing Gu in Journal of Medical Education and Curricular Development
Footnotes
Ethical Approval
The study was conducted in compliance with ethical guidelines, and the study proposal was submitted to the Ethics Committee of Guangdong Provincial People's Hospital for review. The committee granted an exemption from review (KY2024-1145-01).
Informed Consent
Informed consent was deemed unnecessary as the study utilized anonymized and irreversibly modified data, aligning with relevant data protection regulations.
Author Contributions
Literature search: Zhengkang Li, Liwen Ma, Jinxin Lai, and Xinqiang Zhang. Writing—original draft: Zhengkang Li and Liwen Ma. Data acquisition and analysis: Chenyuan He. Writing—review and editing: Yuwei Di and Bing Gu. Study design: Bing Gu. All authors approved the final version of the manuscript for publication.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: 2023 University-Industry Collaborative Education Program (230824485007010); 2022 South China University of Technology School-level Teaching and Education Reform Project; 2022 Guangdong Provincial People's Hospital First-Class Undergraduate Course Project; 2022 National Natural Science Foundation of China Incubation Program of GDPH (8220080559) 2024 Guangdong Provincial Undergraduate Teaching Quality and Teaching Reform Project (448, 536) 2024 South China University of Technology Teaching and Research Reform Project Southern Medical University Teaching Quality and Teaching Reform Project (ZL2024083).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
