Abstract
OBJECTIVES
Near-peer advising (NPA) is an effective intervention to address gaps in medical education by pairing advisees with advisors of similar social, educational, and professional levels.
METHODS
We implemented an NPA program within a core obstetrics and gynecology (OBGYN) clerkship. The near-peer advisor's role was to lead orientation sessions, send clerkship resources, provide mid- and end-clerkship in-person check-ins, and serve as a feedback liaison between students and clerkship leadership. A postclerkship survey explored how the NPA program impacted clerkship students’ learning and experience including setting up for clinical success, implementing feedback, developing an organizational system, providing study resources, navigating interpersonal relationships, and understanding clerkship logistics. Descriptive statistics were reported and qualitative themes were identified using content analysis.
RESULTS
At the three clerkship sites there were 179 students who completed the OBGYN clerkship between February 2022 and March 2023. Of those, 36 (20.1%) completed the postsurvey and 22 (61.1%) of clerkship students reported the NPA program had a positive impact on their clerkship experience. The program helped students perform successfully in clinical settings (n = 18, 54.5%), implement feedback (n = 9, 27.3%), develop an organizational system for studying (n = 13, 39.4%), access study resources (n = 19, 57.6%), navigate interpersonal relationships (n = 7, 21.2%) and understand clerkship logistics (n = 14, 42.4%). Qualitative themes included clearer orientation, improved studying preparedness, and providing safety-net resources.
CONCLUSION
The majority of clerkship students found NPAs a useful resource to assist them in effectively participating in the OBGYN clerkship, developing an organizational system of learning, and navigating team dynamics. NPA interventions are a feasible, effective, and accessible method to improve student experience in the core OBGYN clerkship.
Keywords
Introduction
Medical students have expressed concerns about the obstetrics and gynecology (OBGYN) clerkship, including missed learning opportunities, lack of meaningful roles, student mistreatment, and communication breakdown.1,2 Near-peer advising (NPA) has been introduced as an intervention to address gaps in medical education in various contexts, including geriatric oncology, 3 a shadowing program, 4 a one-time workshop, 5 tutoring coursework and board exams, 6 adjusting to the first year of medical school, 7 and for URM students interested in surgery, 8 to name a few, peer advising has been found to be an effective supplement to faculty education. 9 While peer advising has been studied previously, it has not been explored within an OBGYN clerkship program.
Several strengths of the NPA pedagogy can be leveraged to address student- and faculty-identified needs in the current state of OBGYN medical education. First, NPAs role model skills and behaviors, provide guidance on medical etiquette, and share knowledge. 8 Second, this structure can help elucidate the hidden curriculum that perpetuates barriers in medical education and professional development by creating a safe learning environment. 9 Lastly, this structure allows for advising to align with “cognitive congruence,” a shared knowledge base, and “social congruence,” a shared social role.10,11 Given their cognitive congruence with clerkship students, peer advisors likely understand the shortcomings of clerkship students’ fund of knowledge and can propose solutions at an appropriate level.10,12 Given their social congruence with clerkship students, NPAs may be empathetic to the professional and social contexts of transitioning to clinical education and able to communicate informally with clerkship students. 10
Research within cognitive psychology has demonstrated that excessive cognitive load and learning demand can increase the risk of student burnout while reducing meaningful learning.13,14 We sought to reduce clerkship students’ cognitive load and thereby improve their experience on the core OBGYN clerkship by identifying and responding to their needs in a longitudinal, student-centered fashion. With this framework in mind, we developed an NPA intervention to provide four structured components and one unstructured component across every iteration of the OBGYN clerkship within each clinical site as well as a postclerkship survey to evaluate the program.
The effectiveness of an NPA educational intervention has yet to be explored within the OBGYN clerkship. Through this report, we will review the implementation of an NPA program, OBGYN PAL (Peer-Advisor Leader), within the context of Harvard Medical School (HMS)'s OBGYN clerkship and share an exploratory assessment of its impact on students learning and experience during the rotation.
Materials and Methods
HMS’s clerkship year, The Principal Clinical Experience, occurs in the second year, with most students completing their clinical clerkships at one of three affiliated academic medical centers. Each clerkship rotation at each site has between 6 and 8 students. The OBGYN clerkship is 6 weeks and includes labor and delivery, general gynecological surgery, gynecologic oncology, and ambulatory experiences. All HMS second-year students who completed their OBGYN clerkships at one of the three clinical sites between February 2022 and March 2023 were eligible to participate (n = 179).
NPA recruitment: Senior medical students who were interested in OBGYN medical education assisted in developing the NPA program. These three students also served as the first NPAs at each site. At the completion of the first year of PAL, a job description and recruitment email were circulated to all postclerkship students. The current NPA conducted interviews for interested applicants and nominated a senior medical student who had successfully completed the OBGYN clerkship at the same institution for consideration of the position by the faculty at each site. Prior to onboarding a new NPA, the clerkship director and prior NPA met with each oncoming NPA to review the job description, goals of the NPA program, and provided training on how to handle common student concerns.
Program structure: First, NPAs led a standardized 15-min talk during the clerkship orientation session on the first day of the OBGYN clerkship for clerkship students across all three sites. This session presented study strategies, logistical details, and available resources that might be helpful during the OBGYN clerkship. Second, NPAs sent out three themed, standardized emails to all students throughout the clerkship. The first email focused on orienting students to the clerkship and included helpful information for each of the major OBGYN services: Labor and delivery, general gynecological surgery, gynecologic oncology, and ambulatory experiences. The second email reminded clerkship students of upcoming deadlines, resources for upcoming assignments, and study strategies. The final email provided reminders for final assignments and tips for the shelf exam. Third, NPAs checked in for clerkship student feedback at mid-clerkship and end-of-clerkship sessions. Lastly, NPAs met with clerkship site directors at the end of each clerkship to discuss clerkship student feedback for educational quality improvement.
NPAs were available throughout the clerkship, and clerkship students were encouraged to reach out via phone or email with any questions or concerns. All queries remained anonymous unless clerkship students explicitly requested otherwise. NPAs de-identified and logged all queries into a cross-site NPA log that noted date, nature of concerns, specific concerns, and potential solutions proposed through shared decision-making. NPAs followed up with clerkship students within one week of having received the query, asked them if they deemed the solution to be successful or unsuccessful, and updated the log accordingly.
Survey development: A review of student responses on previous end-of-clerkship evaluations revealed student unmet needs and areas of improvement for the clerkship for which NPA could be helpful and thus informed our creation and implementation of the 15-item postsurvey. The postsurvey asked questions regarding the NPA's impact on clerkship experience (2 questions), logistics and organization (3 questions), clinical success (1 question), learning environment (3 questions), communication (2 questions), and wellness (2 questions). All survey responses were a 3-point Likert scale, either agree/neutral/disagree or positive impact/neutral/negative impact. There were also open-ended questions for students to elaborate on the Likert scale responses. At the completion of the clerkship, survey links were sent by the clerkship coordinator to students via email to complete. Survey completion was voluntary, identifying information was optional, and survey responses were not read by student evaluators. Each survey was designed to take under 5 minutes.
Survey data were de-identified and analyzed by an OBGYN department statistician using Stata 16.0. Descriptive statistics, including frequencies, medians, and interquartile range were calculated. We used a Chi-squared test to compare responses between students in the first versus second half of their PCE year. Content analysis was performed for the qualitative data. Two investigators (ZK, TR) independently reviewed free-text responses and then identified recurring themes. Reviewers then convened to discuss their findings. Each returned to the data and repeated this process. Once data saturation was reached, reviewers finalized and defined each theme.
The intervention was approved by the HMS Program in Medical Education's Educational Scholarship Review and deemed exempt from Institutional Review Board review. Authors followed the CARDA: Guiding document analyses in health professions education research. 15 The CARDA checklist was completed and is included as a supplementary file.
Results
At the three clerkship sites there were 179 students who completed the OBGYN clerkship between February 2022 and March 2023; 36 (20.1%) completed the postcurriculum survey.
Overall, 25 (69.4%) clerkship students reported communicating with the OBGYN PAL at least once over the course of the clerkship. Twenty-two (61.1%) clerkship students felt the OBGYN PAL improved their clerkship experience and 11 (30.6%) felt that the OBGYN PAL had a neutral impact on their clerkship experience. Additionally, 21 (63.6%) students agreed that the OBGYN PAL supported their learning, 16 (44%) agreed that they felt more comfortable sharing concerns/questions with the OBGYN PAL than through other mechanisms, and 13 (39.4%) found that the OBGYN PAL helped them develop an organizational system for studying.
To account for differences in clinical experience, we compared responses from students who completed the OBGYN clerkship during the first half of their clerkship year to the second half. Students who completed the clerkship during the first half of the academic year were more likely to report that the OBGYN PAL helped to improve their organizational system during the clerkship (50.0% vs 18.2% p = 0.033). No other significant differences were found between students’ responses based on timing of clerkship.
The most positive impacts were reported for the following OBGYN PAL roles: providing resources for studying (n = 19, 57.6%), setting up for success in the wards (n = 18, 54.5%) and navigating clerkship logistics (n = 14, 42.4%). Other responses included implementing feedback for the clerkship in real-time (n = 9, 27.3%) and navigating difficult interpersonal situations (n = 7, 21.2%). Of note, 9 (27.3%) learners stated that the OBGYN PAL improved wellness and/or reduced stress levels while 5 (15.2%) found the OBGYN PAL improved their sense of confidence.
We identified three themes from responses to the open-ended question “How did the PAL help you prepare for/support your learning on the clerkship?”. These were orientation (setting expectations for the clerkship), studying (providing resources and exam preparation), and safety-net resource (being available as needed). We identified three themes from the question “In what ways did you feel more comfortable sharing concerns/questions with the OBGYN PALS than through other mechanisms?”. These were relatability (closer in age and more recently completed the same training), safety (voicing concerns to a person not in an evaluator role), and accessibility (more approachable and comfortable). Lastly, we identified themes to the question, “How could we improve the OBGYN PAL position moving forward?” Students reported touch points (providing more one-on-one meeting opportunities), review (providing review sessions for shelf exams), and overview (more structured information on the entire rotation during orientation) (Table 1).
Thematic analysis of survey responses.

Note. OBGYN, obstetrics and gynecology; PAL, Peer-Advisor Leader.
Discussion
The NPA program met its objectives. PALs were able to positively impact each of the learning needs for which clerkship students requested support. Several clerkship students stated they felt supported merely in knowing they had a readily available resource should concerns arise, reflecting the adaptability of the NPA to address varying levels of student need. Many reported that the PAL was useful in adapting to the culture of OBYGN. This understanding of the hidden curriculum may be more difficult for clerkship students to obtain from traditional resources (educational materials, residents, faculty) than from a fellow student. Finally, the NPA may have particular value in the first half of the clerkship year. Students in the first half of their clerkship year were less likely to report an organizational system for studying than those in the second half, which suggests that developing one occurs in an experiential, trial-and-error fashion that could lead to increased cognitive load in an already-demanding clerkship. The NPA's ability to successfully intervene and co-develop these organizational systems with clerkship students justifies the critical role an NPA can have in supporting clerkship students’ transition to the clinical learning environment. It may be important for NPAs to pay special attention to students in their first clerkship.
Prior literature has suggested that the intersection of ineffective study methods, inadequate organizational frameworks, steep learning curves for clinical acclimation, unclear expectations, unavailable mentors, and communication breakdowns can cumulatively compromise student wellness.16–18 Upon review of our clerkship students’ needs and experiences, we formed a conceptual framework that demonstrates a mechanism by which clerkship students’ concerns can negatively impact their experience (Figure 1). Our review of previous student clerkship evaluations identified concerns about patient care, intricate clerkship logistics, limited fund of knowledge and surgical skills, difficulty balancing clinical duties, studying, and wellness, lack of organizational system, lack of resource to provide support, adjusting to team dynamics, and navigating the hidden curriculum. When unmet, these needs can limit learners’ ability to engage with the clinical material and learning environments. The resulting increased cognitive load can present barriers to clerkship students preserving wellness and optimizing learning.13,14
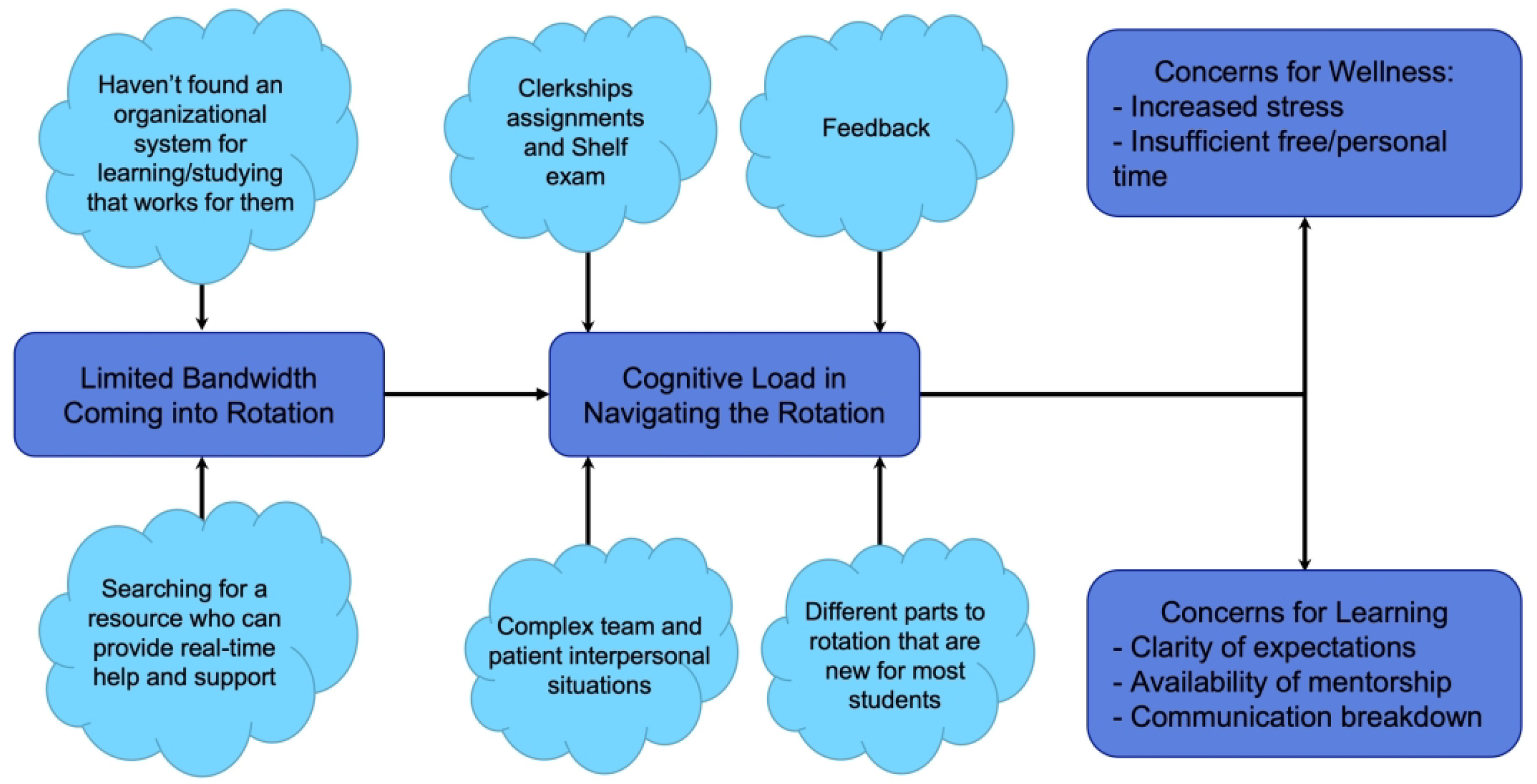
Conceptual framework demonstrating impact of student concerns on wellness and learning.
Aside from the demonstrated value of this intervention for clerkship students’ experiences, this role offers potential benefits to multiple important stakeholders in medical education. First, OBGYN PALs are afforded a medical education leadership opportunity that helps develop important teaching skills prior to residency. The time invested working with residents and faculty members allows for relationship-building, mentoring, and development of a professional network. 19 Second, NPAs can relieve some of the demand on OBGYN residents’ time by orienting clerkship students to effectively contribute to the clinical team.9,12 Finally, the OBGYN PAL can be beneficial to clerkship leadership by serving as a liaison between clerkship students and faculty members. As a result, senior students not only identify issues in the clerkship but also help provide solutions from the students’ perspective. As they are a confidential resource and uninvolved with clerkship evaluation, the OBGYN PAL serves as an avenue for students to openly express concerns or questions without fear of negative repercussions.
Our study was strengthened by a mixed-methods approach. By considering both quantitative and qualitative data, we were able to quantify the effectiveness of the program as well as gain deeper insight into how and why the program was useful, or not. Also, by utilizing an anonymous survey, we protected students’ capacity to share honest feedback and therefore increased internal validity. However, our study had several limitations. First, our institution and clinical sites provided high support for medical education innovation and allocated resources for the implementation of this program. This may not be representative of all institutions and can limit the generalizability of our results. Second, social desirability bias could have affected students’ responses to the postclerkship surveys. To address this, we ensured that data collection was anonymous and that clerkship students were aware of its de-identified nature prior to submission. Third, only 20.1% of students completed the postclerkship survey, which may have been affected by nonresponse bias. Low postsurvey responses likely reflect course evaluation fatigue and competing time demands as students approached the end of the clerkship and started a subsequent clerkship. Nonresponse to the postclerkship survey would likely bias results away from null, but, given that students comfortably shared feedback with OBGYN PALs for improvement in future clerkships at end-of-clerkship sessions, nonresponse is unlikely to bias away from a negative experience. Power calculations were not performed as all students participating in the clerkship were included.
Conclusion
Overall, cross-site implementation of the OBGYN PAL within the HMS OBGYN clerkship and the promising results of its initial assessment suggest that a similar program should be considered at other undergraduate medical institutions, in other clerkships, and in the clinical education of other health professionals. We recommend that this program be included in clerkship education using a needs-responsive, learner-centered paradigm to improve student success on the wards, studying on the clerkship, and navigation of difficult interpersonal situations.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251328252 - Supplemental material for Implementing a Near-peer Advising Program During the Obstetrics and Gynecology Clerkship Improves Students’ Experience
Supplemental material, sj-docx-1-mde-10.1177_23821205251328252 for Implementing a Near-peer Advising Program During the Obstetrics and Gynecology Clerkship Improves Students’ Experience
Footnotes
FUNDING
The authors received no financial support for the research, authorship, and/or publication of this article.
DECLARATION OF CONFLICTING INTERESTS
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The intervention was approved by the Harvard Medical School Program in Medical Education's Educational Scholarship Review and deemed exempt from Brigham & Women's Hospital Institutional Review Board review. The letter does not reference a waiver number but does read: “Your proposal to pursue scholarship to inform educational quality improvement has been reviewed and approved by the HMS Program in Medical Education's Educational Scholarship Review Committee. Your proposal does not meet the definition of research and therefore does not require formal IRB review. We recommend that you share your PME-approved study with your hospital IRB which will coordinate with the Harvard Longwood Campus IRB as needed.”
Informed Consent
Survey completion by students was voluntary, identifying information was optional, and survey responses were not read by student evaluators. Completion of the survey implied consent.
Authors’ Contributions
ZK, JP, LM, RHR, RS, DB and NR designed and led the project, with equal contributions from all authors on the main conceptual idea and outline. TR, GC, FH, GW, CR, TL, DB contributed equally to the preparation of the initial manuscript. NJ, DB and AP reviewed and edited the manuscript.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
