Abstract
Managing the uncertainty of clinical practice represents a significant source of stress for clinicians, including medical students transitioning into the clinical workplace. Self-compassion, a strategy to better cope with stress and burnout, may represent a skill that can be leveraged to better prepare learners for the uncertainty inherent in clinical practice. A negative correlation between intolerance of uncertainty and self-compassion has been demonstrated in undergraduate students and in the general population. An examination of this relationship in medical students may help inform future curricular development for addressing burnout in undergraduate medical education. We electronically administered the Intolerance of Uncertainty Short Scale and the Self-Compassion Short Form to 273 third-year medical students from a single institution and analyzed data via regression. A significant negative correlation was found between intolerance of uncertainty and self-compassion (p < 0.0001). Students with higher levels of self-compassion showed lower levels of intolerance of uncertainty. This is consistent with findings in other populations. Our findings offer a starting point for designing training experiences that strengthen student self-compassion to enhance their ability to reconcile the uncertainty they will encounter in clinical practice.
Introduction
To enter the practice of medicine is to enter a world replete with uncertainty. Intolerance of uncertainty, defined as one’s tendency to consider the occurrence of negative events as unacceptable, independent of the probability of that occurrence. 1 For example, a person with higher intolerance of uncertainty is more likely to interpret ambiguous information as threatening, increasing their level of stress. A clinician with a high intolerance of uncertainty may be predisposed to order significant diagnostic testing despite evidence-based practice recommendations. Intolerance of uncertainty may be measured using validated instruments, such as the Intolerance of Uncertainty Scale (IUS). 1 For clinicians, higher scores on the IUS have been linked with failure to comply with evidence-based guidelines and increased test ordering, 2 withholding information from patients and families, 3 and higher likelihood of burnout.4,5 Given these findings, some schools have integrated tolerance of uncertainty measures into their selection criteria. 6
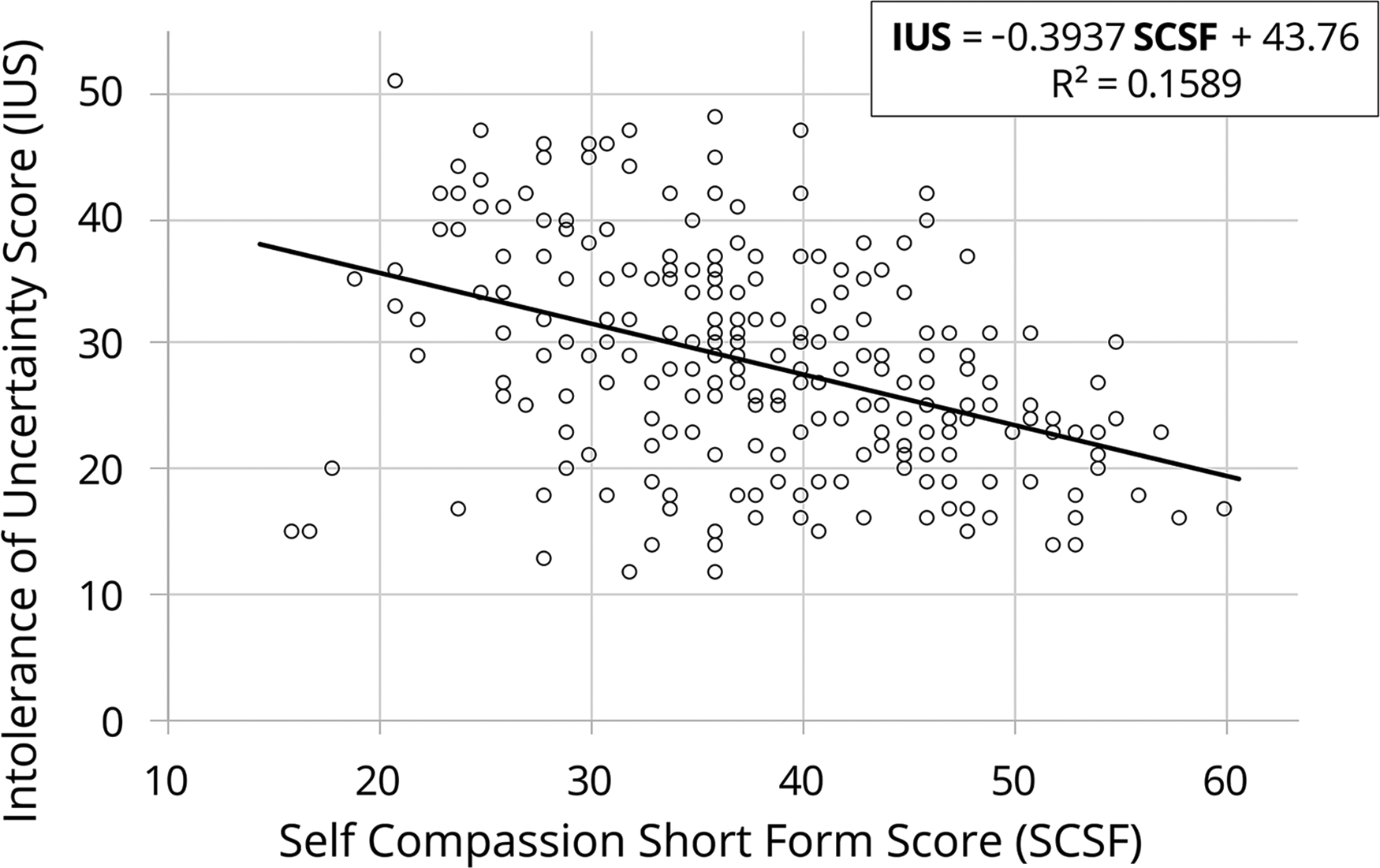
Correlation of intolerance of uncertainty score and self-compassion short form score in third-year medical students.
Self-compassion represents yet another psychological trait that may influence one’s clinical practice. Similarly, it can be measured using validated instruments, such as the Self-Compassion Scale. 7 In contrast to intolerance of uncertainty, higher self-compassion scores are correlated with decreased stress, burnout, and depression.8,9 Self-compassion may assist with moderating the stress associated with reconciling uncertainty encountered in clinical practice. 10 Importantly, research demonstrates that self-compassion is malleable,10,11 serving as an opportunity for educators to leverage self-compassion as they design training experiences that prepare students for the uncertainties of clinical practice.
Medical students represent a unique community when compared to the United States and Canadian general population. They have a higher prevalence of depression and anxiety relative to their non-medical-student counterparts when matched for age. 12 Medical students also demonstrate higher perceived stress, negative coping, and lower resilience when compared to general populations. 13 For this reason, it is essential to study the relationship between intolerance of uncertainty and self-compassion specifically in medical students.
Our study examined third-year medical students who have completed their core clerkships, who were recently introduced to uncertainty in the clinical environment and have accrued clinical experiences that may impact the way they view uncertainty. We hypothesized that higher levels of self-compassion would be associated with lower levels of intolerance of uncertainty. If highly correlated, potential integration of self-compassion training in undergraduate medical education may be advisable to prepare learners for the uncertainty of clinical practice.
Methods
Subjects included a class of 273 third-year medical students at a private urban medical school in Philadelphia, PA. Per the registrar’s office, this class contains 50.5% students who identified as females and 49.5% identified as males, with age ranges between 23 and 39. At the completion of their core clerkship rotations, students were asked to complete the Intolerance of Uncertainty Scale (IUS) short version 1 and the Self-Compassion Short Form (SCSF) 7 electronically through an online survey weblink that was distributed to students via the Canvas™ Learning Management System (LMS). The study was approved by the institutional review board (IRB) of Thomas Jefferson University for the involvement of human subjects (#20E.805). The survey was linked to pre-work for a mandatory curricular session, and responses were meant to inform discussions during the session. Data was de-identified and mean scores were compared with published mean values via t-test. Cronbach’s alpha was calculated to determine internal consistency. Levene’s test was used to compare variance between the two scales and data was subsequently analyzed via regression. Shapiro’s Wilk test was used to evaluate residuals for normality. Pearson’s correlation was calculated to determine effect size (Figure 1).
Results
Of the 273 third-year medical students, 259 (95%) completed both scales. All participants completed all items. No responses were excluded from our analysis. Scores for IUS and SCSF were treated as continuous variables and analyzed parametrically. 14 Mean scores for IUS in surveyed medical students did not differ from previously reported community sample means (28.73, SD = 8.65 vs. 29.53, SD = 10.96, respectively; p = 0.14). 15 High internal consistency was observed in IUS data (Cronbach’s alpha = 0.90). Mean scores for SCSF in students did not differ from previously reported community means (38.17, SD = 8.76 vs. 37.73, SD = 7.69, respectively; p = 0.43). 16 SCSF data also showed good internal consistency (Cronbach’s Alpha = 0.87).
A simple linear regression was calculated to predict IUS based on SCSF. Levene’s test confirmed equal variances, and Shapiro-Wilk Test confirmed normality of residuals. A significant regression equation was found (F[1256] = 48.372, p < 0.0001) with an R 2 of 0.159. For each point scored on SCSF, IUS fell by 0.394 points. Pearson correlation was calculated at r = 0.399 (moderate effect size).
Discussion
Our results suggest a significant negative correlation between medical students’ self-compassion and intolerance of uncertainty. This carries potential implications for curricular design, as educators consider training interventions that will prepare medical students for uncertainty in clinical practice. Being able to appraise and navigate clinical uncertainty is critical; self-compassion may represent an effective strategy for students to cope with this stressor. It is important to note, however, that our study is limited by only examining a single cohort of medical students at a single institution.
Our work is consistent with previous work that demonstrated a negative correlation between self-compassion and intolerance uncertainty among undergraduate (i.e., college) students, 15 as well as adults sampled from the general population. 16 Our study represents the first to report these findings among medical students, specifically those in the clinical environment. Establishing this relationship among trainees and clinicians, in general, is essential to better inform training in health professions education.3–5
While our study suggests a strong correlation, it does not address the question of causation. Future work should explore this potential causal link to determine if increases in self-compassion drive decreases in uncertainty and/or the stress related to uncertainty. Positive findings can have potentially significant implications on curriculum design. Specifically, there is an opportunity for curriculum developers to intentionally design coursework that aligns with the development of student self-compassion and treat the development of self-compassion as a skill that can be learned and integrated into humanities-based programs across the educational continuum. Interventions aimed at mindfulness, for example, can lead to increased self-compassion in healthcare students, which, in turn, may have effects on their attitudes surrounding uncertainty. 17
Footnotes
Declaration of Interests
The authors declare that they have no financial and/or non-financial competing interests. The authors have no conflicts to declare. This study has no financial relationship with any organization that sponsored the research and authorship.
Ethical Approval
The study was approved by the institutional review board of Thomas Jefferson University.
Informed Consent
Informed consent was obtained.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
