Abstract
Objectives:
The aim of this study was to analyze private dental fees in Australia in relation to weekly earnings as a measure of relative affordability, looking at changes from 2014 to 2022 and geographic differences within Australia.
Methods:
Using publicly available data from the Australian Dental Association, fees for select dental procedures were calculated based on national averages and compared with weekly full-time earnings across 2014 to 2022. The proportion of full-time weekly earnings (at various percentile levels) required to pay for procedures was analyzed.
Results:
Mean private practice fees for the 6 dental procedures increased 5.3% to 16.8% between 2014 and 2022. Median weekly full-time earnings increased 24.2% from $1,208 to $1,500. There were smaller increases in income for those below the 25th percentile and larger increases above the 75th percentile. The proportion of median weekly full-time income required to pay for various procedures declined from 2014 to 2022, with a dental checkup costing 22% of median income in 2014 and 18.7% in 2022. Variations were apparent across and within states. For those in the lower income groups, dental treatment consumed a much larger proportion of their weekly earnings than those on higher incomes.
Conclusion:
Private dental fees have not increased greater than average weekly earnings over the past decade. Focusing on price misses only the additional context of the competing costs of other necessities, particularly when they are increasing at a rate higher than inflation and income. Improving our understanding of relative affordability is important in informing policies designed to address the broader inequalities evident in access to dental care.
Knowledge Transfer Statement:
This study found that although private dental fees have not increased greater than average weekly earnings over the past decade, income inequality and geographic fee variability are likely to affect dental visiting patterns. This is important for those advocating measures to improve access to care through a better understanding of dental care affordability.
Introduction
Only about half of all Australian adults have visited a dental professional annually throughout the past decade, and cost is a major barrier to accessing care, particularly for those facing socioeconomic disadvantage (Crocombe et al. 2022; Australian Bureau of Statistics 2024d). Dental visiting patterns have a persistently strong social gradient, with people living in areas of least socioeconomic disadvantage or in major cities more likely to have visited a dental professional in the previous 12 mo than their advantaged counterparts have (Brennan et al. 2020).
More than half of Australian adults report having a little or a lot of difficulty paying a $200 dental bill, and 44% report avoiding or delaying dental treatment because of cost (Crocombe et al. 2022). About 1 in 4 adults reported difficulties paying for a basic preventive dental visit, and this is higher for people in lower income groups. This problem is not unique to Australia (Ramraj et al. 2013; Vujicic et al. 2016). Affordability issues in Canada appear to no longer be just in the domain of the lowest income groups, with middle-income earners now affected due to their lack of, or decreased access to, comprehensive dental insurance.
Australians spent $241.3 billion on health, including $11.1 billion on dental services, in 2021 to 2022, in an economy with a gross domestic product of $2.33 trillion (Health Expenditure 2021-22; Australian Bureau of Statistics 2024a). More than 85% of dental care is provided privately, with most as out-of-pocket costs ($6.67 billion), followed by health insurance funds ($2.16 billion), federal government ($1.3 billion), and state/territory governments ($0.96 billion) (Hopcraft 2024). One-third of federal government funding subsidizes private health insurance, further entrenching access advantage for higher-income groups, with income thresholds of $144,000 for individuals and $288,000 for families with 1 child (and higher with more children). In 2021 to 2022, 2.8 million people with incomes less than $55,000 (the median) received $1.96 billion in private health insurance rebates, whereas 4.44 million people with incomes greater than $55,000 received $2.73 billion in rebates (Australian Tax Office 2023). There is a strong social gradient in insurance coverage, with only 30.2% of people earning less than $30,000 having private health insurance that included dental coverage, compared with 82.7% for those earning more than $140,000 (Australian Institute of Health and Welfare 2024). There is also geographic inequality, with 54.7% of those living in capital cities having private health insurance compared with 44.7% of those living in regional and rural areas (Australian Bureau of Statistics 2024d). Insurance is associated with lower out-of-pocket costs (Teusner et al. 2013), and poorer people and those without dental insurance are less likely to have a dental visit in the previous 12 mo or 5 y (Brennan et al. 2020).
The proportion of dentate adults who avoided or delayed dental care due to cost has been increasing, from 31% in 2004 to 2006 to 39% in 2017 to 218 (Crocombe et al. 2022). The inability to afford dental care exacerbates inequalities in oral health outcomes. A greater burden of dental caries exists among those affected by affordability, especially in low-income adults (Vujicic et al. 2016; Sahab and Sabbah 2022).
Affordability is complex, and definitions can have both qualitative and quantitative dimensions. The qualitative aspect focuses on whether a person or household can obtain basic necessities (such as health), whereas the quantitative aspect identifies proxies, for example, the proportion of financial resources that particular health spending consumes (Persad 2023). Qualitatively, a patient can have treatment recommended by a dental professional but may not have the financial resources to undertake that treatment. They may not, however, perceive dental treatment as a high priority due to competing priorities such as housing, food, or energy, particularly when these costs are escalating. Understanding this dynamic interaction between costs and people’s economic circumstances is important. Studies of affordability in dentistry tend to focus on the self-reported qualitative dimension, for example, delaying a dental visit due to cost or difficulty in paying a $200 dental bill, neglecting the actual cost of attending the dentist (Crocombe et al. 2022). Recently, Gage et al. (2024) quantitatively defined unaffordable dental care as a rise in dental service fees over time relative to personal income. Persad (2023) argued that measures such as percentage of income act as a proxy but do not fully constitute affordability because they lack the qualitative dimension, particularly concerning whether other needs are placed in jeopardy. There is, however, merit in these measures because the subjective decisions patients make about affordability rest on judgments about spending priorities that are based on available income. Persad (2023) noted that health spending is considered affordable if it meaningfully improves health without worsening access to basic needs or depriving someone of a reasonable range of opportunities. The greater proportion of income that dental expenditure requires affects the ability to service those basic needs and a reasonable range of opportunities.
Affordability is both transactional and circumstantial, because the consumer must weigh the value of the service against the cost required to obtain them and because it can change based on the price of the service, the price of competing costs, perceptions of value, and the resources available, among other things (Beal and Foli 2021). Understanding the relative changes in both incomes and private dental treatment fee at the population level are important as increased dental treatment costs relative to income place an additional burden on households. If the cost of dental treatment increases more than incomes do, then there is relatively less money available once other basic needs and opportunities are accounted for.
Inequality in Australia has been increasing, with income before housing growing 66% for the highest income decile and only 31% for the lowest income decile between 1993 and 2018 (Wiesel, Ralston, et al. 2023). Including the cost of housing, inequality grew even faster, with income after housing growing only 20% in the lowest decile compared with 62% in the highest decile.
With most dental care provided in the private sector with limited government financial support, cost-of-living pressures and out-of-pocket dental fees will influence dental attendance patterns.
The aim of this study was to investigate the relative affordability of private dental care in Australia using a quantitative approach by measuring the proportion of weekly income required to pay for dental treatment, looking at changes over time and geographic differences within Australia.
Methods
This is an ecological study. Mean dental fee survey data for general dental practitioners published by the Australian Dental Association were obtained for the period of 2014 to 2022 (with no data published in 2021), with breakdowns by states and by capital city and rest of state (Australian Dental Association 2022b). Capital cities are the largest population centers in each state, ranging from 44% (Hobart) to 98% (Canberra) of the total state population.
Income data were drawn from the Australian Bureau of Statistics Characteristics of Employment survey, which reports employee earnings (Australian Bureau of Statistics 2024b; Australian Bureau of Statistics 2024d). The survey reports data from approximately 50,000 individuals aged 15+ y weighted to population benchmarks to estimate weekly earnings. The average weekly earnings (AWE) used for this analysis are the full-time earnings in the main job, reported as median figures and in percentiles. Inflation was measured using the Consumer Price Index from September 2014 to September 2022 (Australian Bureau of Statistics 2024c). Dental fees and incomes are not adjusted for inflation.
Six dental treatment procedures were created based on common procedures to reflect a range of different treatment scenarios, using the item codes in the Australian Dental Association Schedule of Dental Services and Glossary (Australian Dental Association 2022a). The treatment procedures [item code] were as follows:
Checkup: comprehensive dental examination [011], 2 bitewing radiographs [022 × 2], and removal of calculus (scale and clean) [114]
Extraction: removal of a tooth or part(s) thereof [311]
Amalgam: 3-surface amalgam restoration on posterior tooth [513]
Composite: 3-surface resin composite restoration on posterior tooth [533]
Molar root canal: endodontic treatment for 3 canal molar tooth consisting of complete chemo-mechanical preparation of root canal (1 canal) [415], complete chemo-mechanical preparation of root canal (additional canal) [416 × 2], root canal obturation (1 canal) [417], and root canal obturation (additional canal) [418 × 2]
Crown: full crown veneered (indirect) [615]
These fees represent the fee charged to the patient in a private practice setting. Some patients may have a portion of this fee subsidized by private health insurance. Outcomes were analyzed in several ways. First, the change in mean fee for treatment items from 2014 to 2022 at the national and state/territory level. Next, the change in weekly full-time earnings expressed in percentiles (10th, 25th, 50th, 75th, and 90th) from 2014 to 2022 at the national and state/territory level. Relative affordability was calculated as the proportion of full-time weekly earnings (at each percentile level) required to pay for the various treatment items. Trends from 2014 to 2022 are reported as well as state/territory differences in 2022. Finally, dental treatment costs as a proportion of median full-time weekly earnings were compared by capital city and rest of state across jurisdictions. These summary statistics were plotted over time to describe variations. All figures are reported in Australia dollars.
Results
Mean private practice fees for the 6 procedures increased from 5.3% and 16.8% between 2014 and 2022 (Table). A checkup had the lowest increase, whereas the large amalgam restoration had the largest increase.
Mean Dental Fees and Weekly Full-Time Earnings by Percentile, 2014 and 2022.
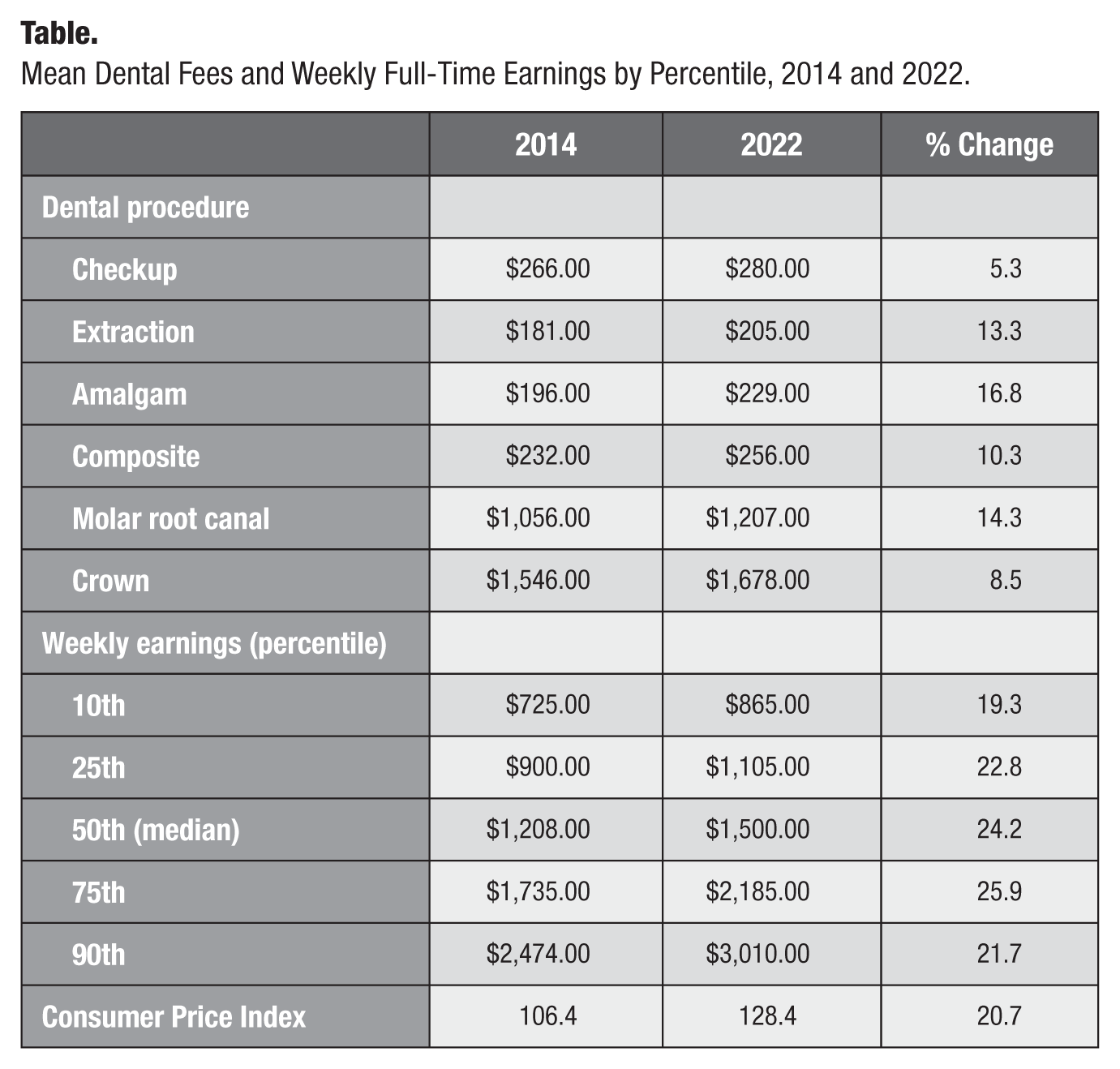
Median weekly full-time earnings increased 24.2% from $1,208 to $1,500 between 2014 and 2022 (Table). There was a smaller increase for those in the 10th (19.3%) and 25th percentile (22.8%) compared with those in the 75th percentile (25.9%). In 2022, the 90th percentile earnings were just more than twice the median, and the 75th percentile was 1.5 times the median, whereas the 25th percentile was 0.74 times the median and the 10th percentile was 0.58 times the median (Appendix Table S1).
Incomes increased at a rate greater than inflation for all groups except for those in the 10th percentile, whereas dental fees increased at a rate much lower than inflation.
The proportion of median weekly full-time income required to pay for the various treatment procedures declined between 2014 and 2022 (Fig. 1). In 2014, a dental checkup cost $266, representing 22% of the median weekly full-time income. By 2022, the percentage of weekly earnings required to pay for a dental checkup declined to 18.7%. There were also similar but smaller declines in the relative proportion of weekly earnings required to pay for the other procedures.
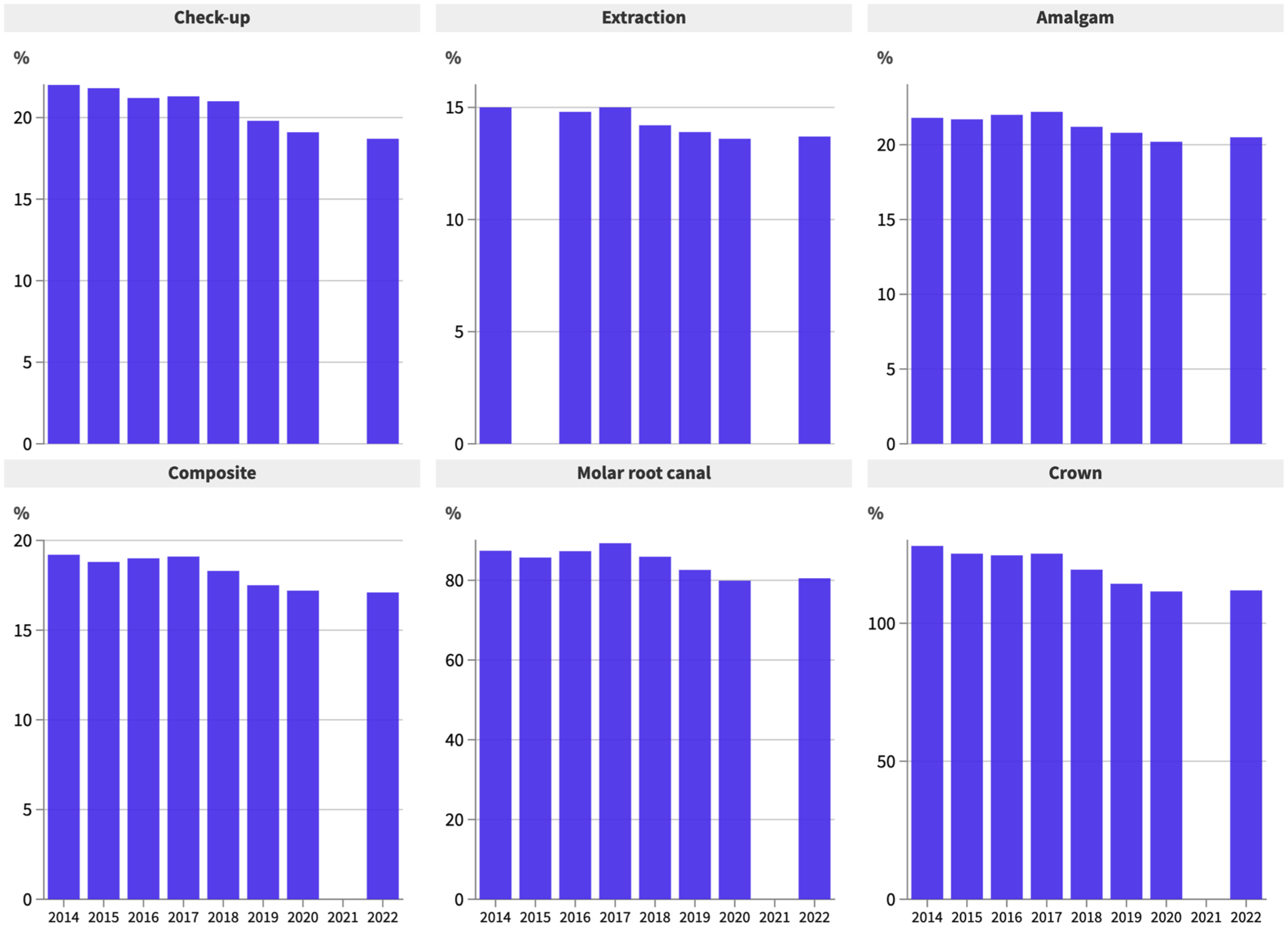
Dental procedure costs as a proportion of median weekly full-time earnings, 2014 to 2022.
Figure 2 shows the costs for a range of dental procedures as a proportion of weekly earnings across earning percentiles between 2014 and 2022. Although a dental checkup cost 18.7% of the median weekly income in 2022, it represented nearly one-third of the weekly income for low-income earners but less than 10% of the weekly income for the highest income earners. This pattern is consistent across the range of procedures. For people in the lowest income decile, a large amalgam filling on average cost 26.5% of weekly earnings, endodontic treatment 1.4 times their weekly earnings, and a crown nearly twice their weekly earnings, whereas for the highest income earners, a large amalgam restoration cost only 7.6% of their weekly earnings and a crown just 55.7% of their weekly earnings. Despite these inequalities, the slope of the change in relative affordability was greater in the lower-income deciles than in the higher-income deciles (Appendix Table S2).
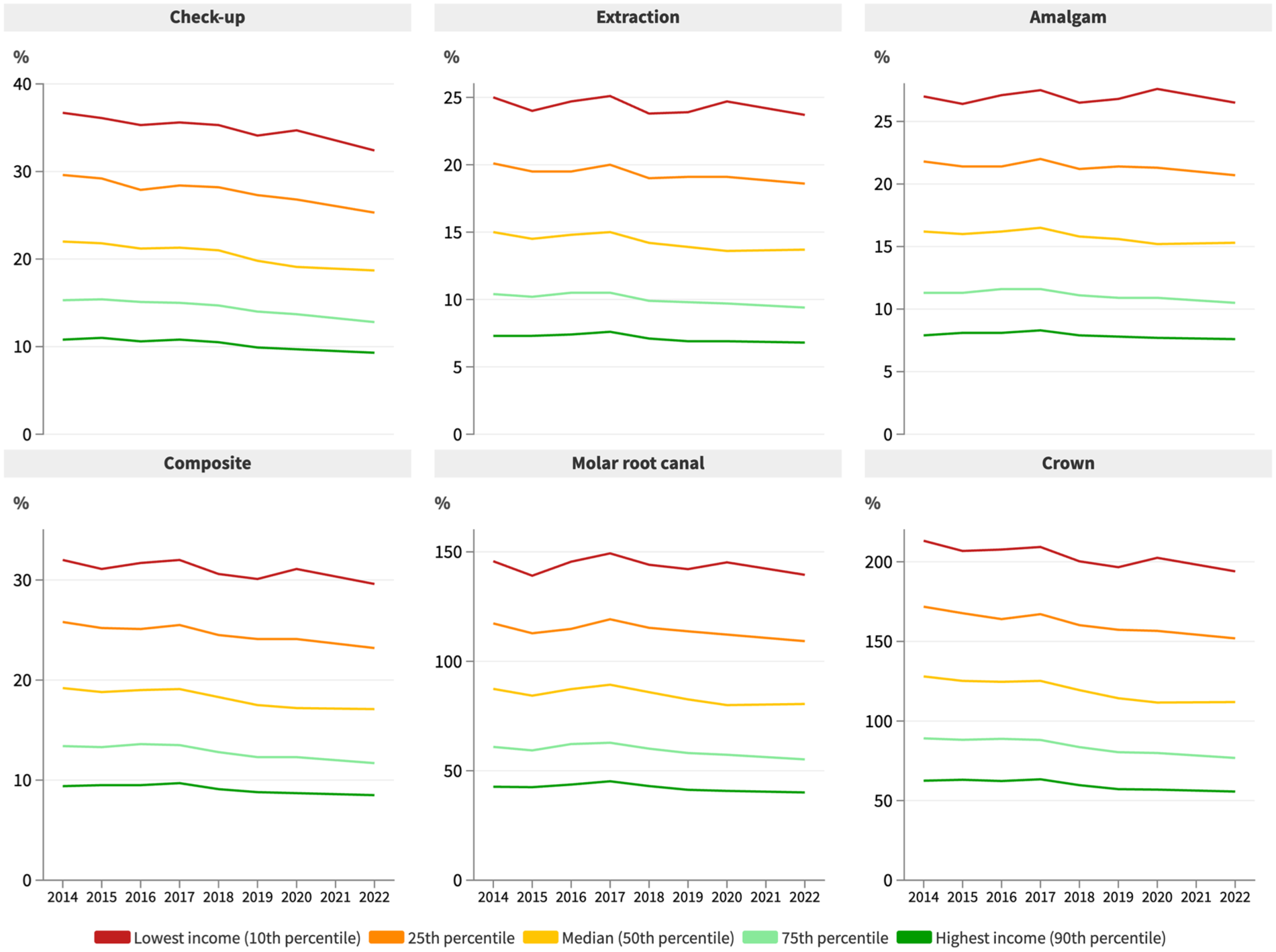
Dental procedure costs as a proportion of weekly full-time earnings by income percentile, 2014 to 2022.
There is wide variation in weekly earnings across Australia and dental fees across states/territories (Appendix Table S3 and Table S4). Figure 3 shows the variation in dental treatment as a proportion of weekly earnings by state and earning percentiles. Affordability varied by state, which was both a function of variation in average dental fees and in weekly earnings across states. For example, dental fees in Tasmania were 8.8% higher than the Australian average for an examination and 12.9% higher for an amalgam restoration, whereas the median weekly income in Tasmania was 10% lower than the Australian average. Dental treatment was generally least affordable across all earnings groups and treatment procedures in Tasmania and most affordable in Western Australia.
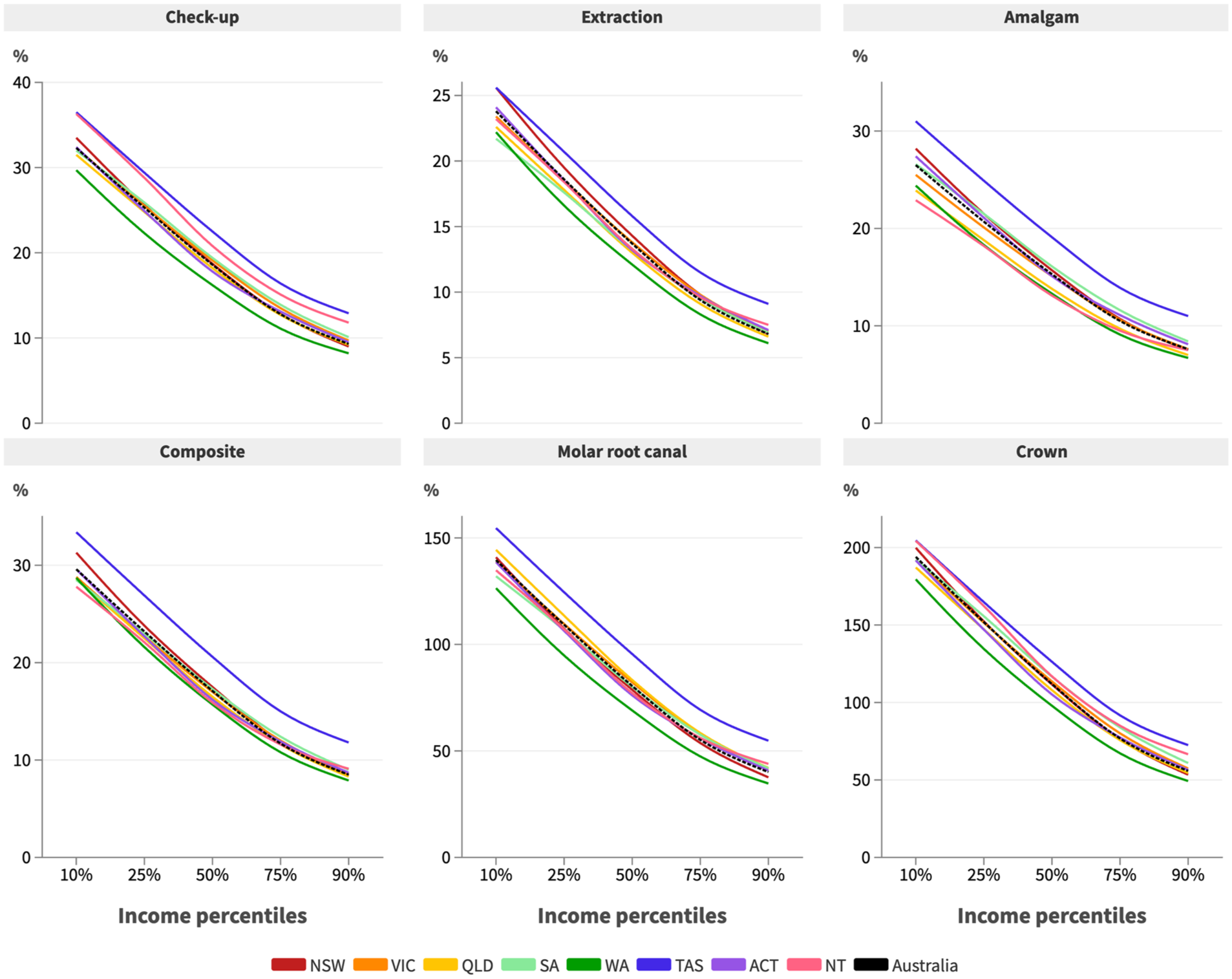
Dental treatment costs as a proportion of weekly full-time income by income percentile and state, 2022.
There were differences between capital cities and the rest of the state, highlighting another aspect of regional and rural inequality (Fig. 4). This was a function of both generally lower incomes and higher dental fees in regional and rural areas, although this played out differently across states (Appendix Tables S5 and S6). For example, the median full-time weekly earnings for Hobart (Tasmania) was $1,389 and for the rest of the state $1,338, but the cost of an extraction in Hobart was $203.63 and for the rest of the state $228.39, so the gap in the proportion of weekly earnings of 14.7% (capital city) to 17.1% (rest of state) in Tasmania was driven mostly by the higher cost of treatment in regional and rural areas. In contrast, median weekly earnings in Sydney (New South Wales) were $1,583 and for the rest of the state $1,400, whereas the cost of an extraction was $221.43 in Sydney and $200.96 for the rest of the state, so the gap in the proportion of weekly earnings required was driven by a greater inequality in weekly earnings.
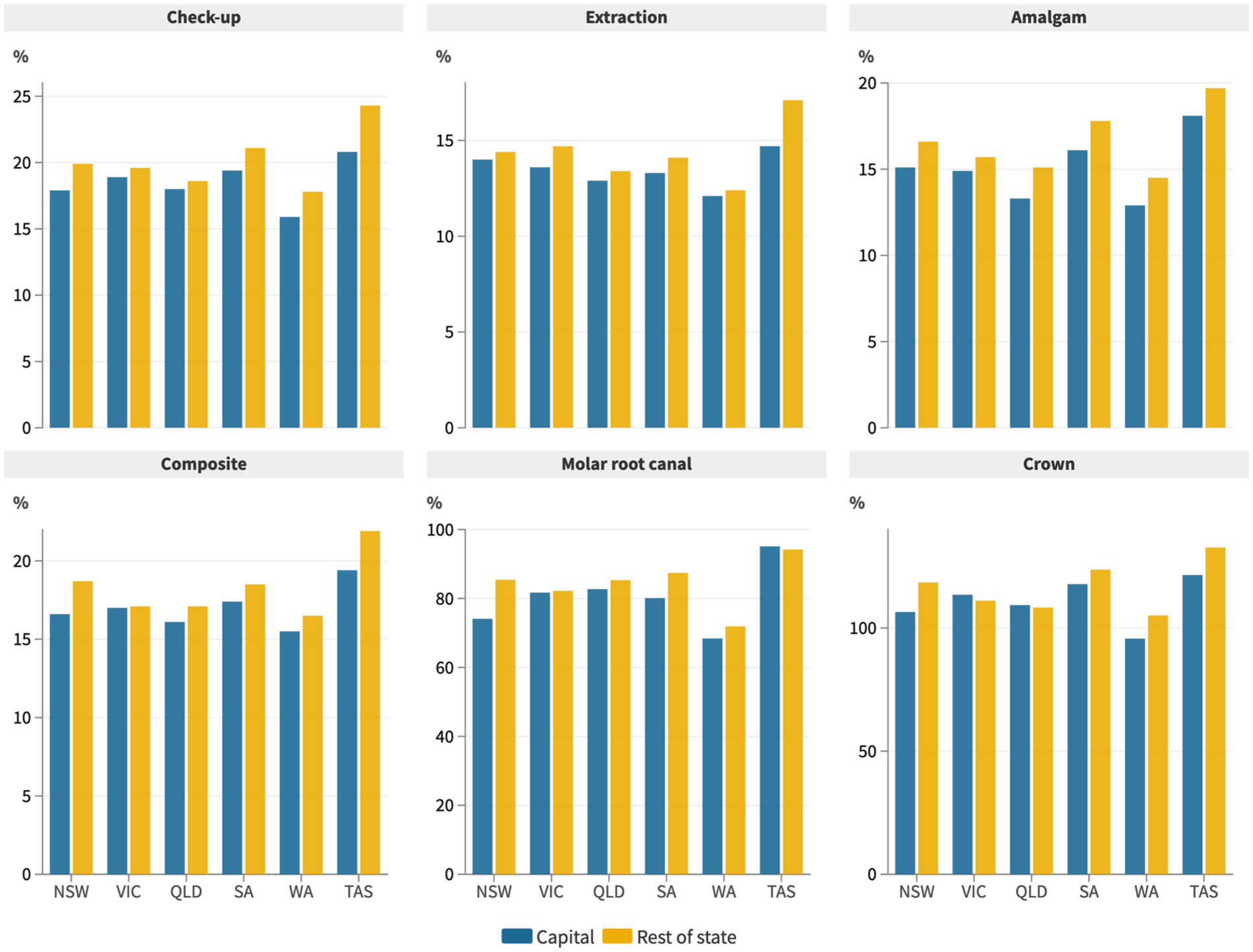
Dental treatment costs as a proportion of median full-time weekly earnings by capital city and rest of state, 2022.
Discussion
Private practice dental fees in Australia have increased broadly in line with AWE over the past decade, but state-level and geographic variations by remoteness was present. Although the overall trend suggests dental treatment is slightly relatively more affordable now than it was in 2014, a dental examination still costs one-third of weekly income for a large section of the population. A small increase in dental fees will have a larger affordability impact on those facing financial hardship.
The findings of this study contrast with a recent investigation into dental affordability in New Zealand, which found that dental fees increased 75% to 236% whereas earnings increased only 46% from 1978 to 2023, although from 2008 to 2023, AWE increased 21%, which was broadly in line with most dental treatment costs (Gage et al. 2024). The authors argued that commercial determinants, including the increasing cost of regulation, compliance, and dental equipment and the changing models of practice ownership from individual dentists to dental corporates may be factors increasing the cost of dental care. In Australia, dental fees increased at a rate substantially below inflation, which could be a function of increasing numbers of dental practitioners and increased competition keeping downward pressure on fees.
Across-State and within-State Differences
Physical or geographic access to dental services is an important determinant of oral health (Ghanbarzadegan et al. 2021). There is geographic inequality in the availability of dental services in terms of both the number of practitioners and the distance to the nearest service, with more than 74.9 practicing dentists per 100,000 population in major cities, compared with 40.7 in outer regional areas and only 20.7 per 100,000 in remote/very remote areas (Department of Health and Aged Care 2024). This study adds an additional overlay to the geographic access issue, demonstrating that the interplay of lower incomes and sometimes higher costs of dental services in regional and rural areas exacerbates inequities in oral health outcomes.
Understanding Affordability
Affordability has a different meaning to patients, providers, governments, and third-party payors. Discussions of affordability usual focus solely on the cost of treatment from the perspective of the patient, for example, the ability to pay a $200 dental bill, aligning with the qualitative definition proposed by Persad (2023). Long-term Australian data show that self-reported measures of unaffordability have generally increased from 1994 to 2021 (Australian Institute of Health and Welfare 2024). These measures reflect individual circumstances and patient preferences but are subjective. By contrast, our findings using percentage of income as a quantitative proxy for affordability suggest that private dental care has become slightly more affordable. This highlights the dynamic nature of oral health care affordability based on prioritization and competing demands on household income. Although prices for oral health care may not have grown dramatically, inflation and the increasing cost of living force people to prioritize urgent household needs, taking available resources for oral health care away. This highlights the importance of the subjective nature of affordability based on individual circumstances (Beal and Foli 2021).
Cost-of-Living Pressures
Lower-income families are 4 times more likely to be in financial stress than high-income families are, and the proportion of low-income families experiencing financial stress has increased between 2015 and 2019 in Australia (Phillips 2022). These households often pay less than higher-income households in absolute terms on living expenses, but it is usually a larger proportion of their overall income (Wiesel, de Bruyn, et al. 2023). This is exacerbated as the cost-of-living increases in relative terms. Since 2020, the cost of many essential items such as food, housing, and energy has increased substantially at a time when incomes (particularly for those below the median) have been relatively stagnant. As essential costs increase, discretionary income decreases, affecting how and where people choose to spend their money. People substitute expenditure on items as essential costs increase, with an increase in the relative price of energy leading to lower food expenditure for people living in low income (Fry et al. 2023). This tradeoff may also extend to health costs, and specifically dental expenditure, which is often seen as discretionary and therefore perceived as being less affordable.
People living in poverty experience higher psychological distress (Bray 2024), and prioritizing health care requires not just the ability to pay but also the emotional and psychological resources to make those decisions.
People with low income may prioritize dental treatment to treat acute disease or pain because of urgency, but they may neglect paying for prevention, which may only offer long-term reward.
Is Cost a Barrier to Accessing Dental Care?
Cost has been consistently cited as a key barrier for accessing dental care over decades in Australia and internationally (Vujicic 2014; Vujicic et al. 2016; Crocombe et al. 2022; Australian Bureau of Statistics 2024e). This underpins global demands for universal health care in dentistry (Watt et al. 2019). The high reliance on out-of-pocket expenditure with limited public funding clearly exacerbates the issue of cost as a barrier (Hopcraft 2024). Our findings highlight that although the cost of dental treatment has not exceeded increases in median wages over the past 9 y, for people with lower than median incomes, the cost of routine dental care affects disposable income significantly. In the context of the current cost-of-living crisis, income inequality is likely to be a factor in dental attendance patterns. For people in the lowest income quartile, routine dental treatment such as an examination, extraction, or restoration costs at least 18.6% to 25.3% of their weekly income, but more complex treatment such as endodontic treatment for a molar tooth with a subsequent crown would cost the equivalent of nearly 3 weeks of pretax income. These are people who would not otherwise be eligible for publicly funded dental care and are therefore the group most likely to delay care or forgo necessary and recommended treatment (Crocombe et al. 2022).
The issue of affordability and cost as barriers is often framed as one of prioritization and of victim blaming, with people who claim difficulties with paying a $200 dental bill using cost as an excuse. For many on low incomes, private dental fees represent a significant proportion of their income. As in many high-income countries, our findings show that in Australia, relative inequality is a more important issue than absolute inequality is (Peres et al. 2019). While measures such as inclusion of welfare recipients in subsidized dental care in a public setting is beneficial, measures targeting those in absolute poverty do not address affordability for those on relatively low incomes but who are not in absolute poverty.
Expanding Public Funding for Dental Services
Dentistry has one of the highest out-of-pocket expenses across health care in Australia, with 80% of all dental care effectively paid by individuals and only 20% subsidized by governments (Hopcraft 2024). There are differing views on the impact of high out-of-pocket fees on the ability for people to access care, the equity implications, and the rights of private health care providers to set their own fees in a free-market economy. There is also a need for ongoing debate about the role of increased government funding to address the issue of affordability (Callander 2023). This study suggests a need for targeted government support to fund dental care for those on lower incomes to reduce inequalities in access to dental care and in the burden of oral disease, which aligns with the push toward universal health coverage for dental services to ensure they are more accessible and responsive to the needs of the population (Watt et al. 2019).
Limitations
There are several important caveats with this analysis. First, the AWE data represent only a subset of total household income and do not account for those working part-time or on income support payments (where affordability would be an even greater issue). Nor does it account for income or earnings from other sources. Nonetheless, 68% of those with jobs are working full-time, so for the purposes of understanding affordability of dental care for a large proportion of Australians, AWE is an acceptable measure (Australian Bureau of Statistics 2024b).
Second, the analysis does not take into account other factors that might affect discretionary spending power. As essential living costs have increased in the past few years, people have less discretionary income available to spend on dental care now than they did 9 y ago, and this will be felt disproportionately by those with lower incomes (Cope and Chestnutt 2023). That is likely to be an important factor contributing to affordability and access to care for people who earn below the median income, with less discretionary income to allocate to dental care. There are no available data to compare cost-of-living changes at a geographic level in a way that matches the fee survey data to determine what impact that might have on affordability beyond the changes to fees and incomes.
Finally, dental fee surveys reflect an average fee across Australia, self-reported by a subset of dentists who were members of the Australian Dental Association, with a wide variation across states and within states across metropolitan and rural areas. In 2014, the fee survey data came from 3,056 of 9,346 (33%) general dental practitioners who were members of the Australian Dental Association, and in 2022, the data came from 3,535 of 9,711 (36%) general dental practitioners. These factors affect the generalizability of these findings. Nonetheless, private dental fees are typically market driven, and large variations are not expected between those who did and did not provide data.
The fees represent the amount charged to patients accessing care in the private dental system. Some patients have a portion of this fee subsidized by private health insurance, reducing their direct out-of-pocket costs to the dentist. This does not, however, account for the cost of private health insurance, which is ultimately paid for by the individual. Nearly 1 in 5 people with private health insurance still reported that they avoided or delayed dental care due to cost (Australian Institute of Health and Welfare 2024).
This study contributes to the affordability debate by adding the overlay of the change in the cost of dental treatment relative to individual income. The gap in current knowledge that self-reported measures of affordability and price changes relative to inflation and income do not adequately address is a consideration of the competing costs of other necessities—particularly if they are growing at a pace greater than both inflation and income. Furthermore, affordability is contextual, which means that people may be able to prioritize treatment that is seen to have an intrinsic value (for example, to repair a broken tooth or relieve pain) but not necessarily for prevention, which is conceptually more difficult to assign value to. There is a risk that a narrow view on affordability may result in “victim blaming,” with patients making “poor” choices about their oral health. Therefore, there is a need for further research that explores how patients understand affordability of dental care in the context of competing financial demands.
Conclusion
Many Australians continue to report cost as a barrier to accessing dental care, and this is worse for the one-third of Australians who live outside of capital cities, where there are fewer dental practitioners. Private dental fees have not increased greater than average weekly earnings over the past decade. Improving our understanding of relative affordability is important in informing policies designed to address the broader disparities evident in access to dental care.
Author Contributions
M.S. Hopcraft, contributed to conception and design, data acquisition, analysis, and interpretation, drafted the manuscript; A. Singh, contributed to conception and design, data analysis and interpretation, drafted the manuscript. All authors gave their final approval and agree to be accountable for all aspects of work.
Supplemental Material
sj-docx-1-jct-10.1177_23800844251384649 – Supplemental material for Relative Affordability of Private Dentistry in Australia over the Past Decade
Supplemental material, sj-docx-1-jct-10.1177_23800844251384649 for Relative Affordability of Private Dentistry in Australia over the Past Decade by M.S. Hopcraft and A. Singh in JDR Clinical & Translational Research
Footnotes
Acknowledgements
The open access publication was facilitated by the arrangement between Sage Publishing and the Council of Australian University Librarians.
A supplemental appendix to this article is available online.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
