Abstract
Objectives:
This study aimed to identify strategies for implementing and integrating the Canadian Caries Risk Assessment (CRA) tool for preschoolers into the primary care of First Nations and Métis children in Manitoba, Canada, based on the perspectives of nondental primary care providers (NDPCPs).
Methods:
An exploratory qualitative design was employed to gather insights from NDPCPs who provide care to Indigenous children aged <6 y. Fifty participants were purposefully recruited from 10 urban, rural, and remote communities across Manitoba. Data were collected through 8 focus groups and 12 in-depth key informant interviews conducted between April 2023 and September 2024. Interviews were transcribed verbatim and analyzed thematically via an inductive approach informed by a social constructivist framework.
Results:
Four interrelated themes were identified by participants as central to CRA implementation and integration. Strengthening primary care systems involved training in fluoride varnish application, management endorsement, electronic medical record integration, standardized documentation, and incentives such as fee-for-service models. Building trust and culturally safe connections with Indigenous communities included establishing respectful relationships, embedding CRA into trusted programs, and addressing access barriers such as transportation and oral health supplies. Educating and engaging families focused on developing accessible educational materials and using trusted communication channels such as Facebook and local radio to improve oral health literacy. Advocating for policy changes involved calls for billing codes, sugar reduction policies, and CRA integration into existing well-child programs.
Conclusion:
NDPCPs in Manitoba are supportive of integrating the CRA tool into Indigenous pediatric primary care. Their recommendations offer a practical road map for CRA implementation, emphasizing systemic support, culturally responsive care, education, and policy alignment. These findings contribute to broader efforts to reduce oral health disparities and improve early childhood caries prevention in underserved populations.
Knowledge Transfer Statement:
Nondental primary care providers recommend integrating Caries Risk Assessment tools into Indigenous children’s care through enhanced training, culturally safe engagement, and supportive policy development to address persistent oral health inequities.
Keywords
Introduction
First Nations, Métis, and Inuit Canadians experience notable oral health disparities, particularly among children (Kyoon-Achan, Schroth, DeMare, Sturym, Edwards, et al. 2021a; Hussain 2022). Evidence indicates that Indigenous populations face poorer oral health outcomes as compared with other Canadian counterparts (Hussain 2022). These disparities stem from a complex interplay of factors: limited oral health literacy, low income, inadequate health infrastructure, a shortage of oral health providers, cultural disconnection, and intergenerational trauma (Poirier, Soares, et al. 2023).
Early childhood caries (ECC), defined as caries in the primary dentition of children <6 y of age, is one of the most common chronic conditions seen in children, affecting >600 million children worldwide (Pitts et al. 2019). In Canada, ECC is disproportionately prevalent among children living in equity-denied conditions, including those from low-income families, newcomers/immigrants, and rural and remote regions, as well as First Nations, Métis, and Inuit populations (Schroth et al. 2013). Despite the implementation of various public health initiatives, caries prevalence remains high among Indigenous children (Holve et al. 2021). Addressing these inequities requires upstream community-driven approaches that expand beyond traditional dental settings and foster interdisciplinary strategies (Schroth et al. 2021; Poirier, Soares, et al. 2023).
A promising response has been the development of a Canadian Caries Risk Assessment (CRA) tool for preschoolers, designed to support early identification of caries risk and guide preventive care (Schroth et al. 2021). This tool, developed through a systematic review and stakeholder consultation process, is intended for use by dental and nondental primary care providers (NDPCPs). It is designed to facilitate early risk identification, oral health education, fluoride varnish application, and referrals to establish a “dental home” (http://www.cda-adc.ca/en/oral_health/cfyt/dental_care_children/risk_assessment.asp).
NDPCPs, including nurses, physicians, and allied health professionals, often serve as the initial point of contact for families and are uniquely positioned to promote oral health, particularly in regions where access to dental care is limited or unavailable. To enhance the delivery of preventive oral health services to young children, the US Preventive Services Task Force recommends that medical providers apply fluoride varnish to the teeth of children during well-child visits through age 5 y (Davidson et al. 2021). The Canadian CRA tool supports this recommendation by prompting providers to apply fluoride varnish to preschool-aged children following oral health screening. However, there is limited evidence on how to effectively implement the CRA tool in primary care settings, and even less is known about the perspectives of NDPCPs, who play a vital role in its integration and success. Understanding their experiences, perceived roles, and recommendations is crucial for developing realistic and community-informed implementation strategies that are responsive to the needs of Indigenous communities (Schroth et al. 2023).
Given that successful implementation of the CRA tool in primary care requires an understanding of frontline provider perspectives, this study employed a qualitative approach to explore the experiences, insights, and recommendations of NDPCPs. Qualitative methods are well suited for examining complex social and contextual factors that influence clinical practice, especially in culturally and geographically diverse settings (Creswell and Poth 2017; Renjith et al. 2021).
Building on prior research that identified key barriers to CRA implementation in Indigenous primary care (Olatosi et al. 2025), the present study shifts the focus toward provider-recommended strategies for effectively implementing and integrating the Canadian CRA tool into the primary care of First Nations and Métis preschoolers in Manitoba. This study addressed the following research questions:
Research Question 1: What strategies do NDPCPs recommend for effectively implementing and integrating the Canadian CRA tool into First Nations and Métis children’s primary care services in Manitoba?
Research Question 2: How can these recommendations inform approaches to improve ECC prevention in underserved Indigenous communities?
Methods
Study Design
This exploratory qualitative study utilized semistructured interviews to examine the perspectives of NDPCPs in Manitoba on strategies for implementing and integrating the Canadian CRA tool into primary care for Indigenous children. The study was guided by a social constructivist research paradigm, which emphasizes the co-construction of knowledge through interactions between researchers and participants, recognizing that multiple realities are shaped by cultural, social, and historical contexts (Charmaz 2015). This paradigm was chosen to guide the research as it aligns with the study’s focus on understanding diverse provider experiences and the contextual factors influencing the implementation of oral health interventions in Indigenous communities. This paradigm was purposefully chosen as it aligns with the aim of the study to explore the nuanced experiences of health care providers working with marginalized populations. It supports an approach that values lived experience, acknowledges power dynamics, and is sensitive to the broader sociopolitical contexts influencing health care delivery. These features are particularly relevant when working with Indigenous communities, whose historical and ongoing experiences with colonization shape health outcomes and health care engagement.
Purposeful sampling was employed to achieve critical representation. To ensure that the participants’ responses were accurately interpreted, the researchers applied a constant comparative method of analysis, facilitating the generation of authentic conceptual descriptions.
Ethics
Ethics approval for the study was obtained from the University of Manitoba Health Research Ethics Board (HS25866; H2023:050), which is linked to the University of Manitoba study funded by the Canadian Institutes of Health Research (HS24621 [H2021:043]; HS20926).
Research Team and Reflexivity
Considering that the study adopted a qualitative approach, there was a need to highlight the researchers’ identity, subjectivity, marginality, and perspectives brought into the research as part of reflexivity and transparency in the research process (Poirier, Haag, et al. 2023). The authorship team is led by R.J.S., a dental public health specialist and researcher who has worked with First Nations and Métis communities in Manitoba for many years. The first author (O.O.O.), a non-Indigenous female researcher and pediatric dentist, conducted the interviews with experience working with underserved communities. The team also consist of 3 Indigenous researchers; all other authors are experienced researchers in child oral health, public health, and Indigenous health.
Participants and Recruitment
Fifty nondental primary care personnel who provide care to First Nations and Métis children aged <6 y were purposefully selected from 10 health and community centers serving Indigenous communities in Manitoba: Winnipeg (urban), Pine Falls, Swan River, St. Laurent, Pine Creek, Camperville, Thompson, St. Theresa Point, Berens River, and Selkirk (urban). NDPCPs (nurses, physicians, dietitians, and social workers) were invited to participate in the study by identifying a contact person (clinic administrator/manager) in each center, who helped to disseminate the study details. In addition, recruitment fliers that contained QR codes to information about the study were posted in selected health centers after getting the necessary approvals. Participants were also recruited from the University of Manitoba’s Ongomiizwin Health Services and the Department of Pediatrics and Child Health member listing. Prospective participants received information about the objectives of the study; informed consent forms were sent via email ahead of the interviews, which were signed on the day of the interview.
Data Collection
A semistructured interview guide (Appendix 1) was developed by the study team, based on literature searches and team experiences from previous investigations. Consistent with a social constructivist approach, which emphasizes the co-construction of meaning through dialogue, the guide was designed to encourage open-ended responses and allow participants to shape the direction of the conversation (Plano Clark and Ivankova 2016; Tashakkori et al. 2020). The interview guide was iteratively refined to include additional questions and probes based on emerging themes. The final version was reviewed by the interdisciplinary study team, including researchers with expertise in early childhood oral health, health promotion, community development, and Indigenous health.
Data were generated from 8 focus groups and 12 in-depth key informant interviews held between April 2023 and September 2024. Each focus group consisted of 5 to 8 NDPCPs who had experience providing care to Indigenous children. Informed consent and demographic information were obtained at the beginning of each session. Focus groups lasted between 45 and 75 min and were conducted at community health centers. Sessions were audio recorded by O.O.O., while 2 other researchers (M.M. and D.D.) took field notes, including observations of nonverbal responses and facial expressions to help contextualize participants’ emotional responses (Patton 2014). Key informant interviews lasted between 15 and 30 min. In keeping with qualitative traditions, the interview guide was modified throughout the data collection process to explore new ideas and themes as they emerged (Guest et al. 2020). Data collection continued until thematic saturation was reached. Data were transcribed verbatim and analyzed via inductive thematic analysis with NVivo software. The study’s validity was ensured by member checking, data sharing with experts, field notes, and memos.
Data Analysis
Data analysis occurred concurrently with data collection and was informed by an inductive thematic analysis (Braun and Clarke 2006) guided by a social constructivist paradigm. This paradigm influenced the analytic process by centering participants’ perspectives, embracing subjectivity, and interpreting meaning within the broader sociocultural context. Transcripts were read and reread line by line per an open coding strategy, in which segments of text were labeled with descriptive words or short phrases that captured key ideas. A constant comparative method was employed to iteratively compare codes across transcripts, allowing for deeper understanding and refinement of concepts as data collection progressed (Creswell and Poth 2017). Inductive and deductive strategies were used: inductive coding allowed new ideas to emerge from the data, whereas deductive codes based on existing literature and the interview guide were applied where appropriate.
Themes were developed through the clustering of related codes into subthemes and overarching themes. Two researchers (O.O.O. and M.M.) independently coded the data and met regularly to discuss interpretations and refine the coding framework, enhancing analytic rigor and reliability. Strategies were employed to enhance trustworthiness, such as member checking by sharing summary of emerging themes with participants for feedback, peer debriefing with experts, and detailed analytic memos (Birt et al. 2016).
Results
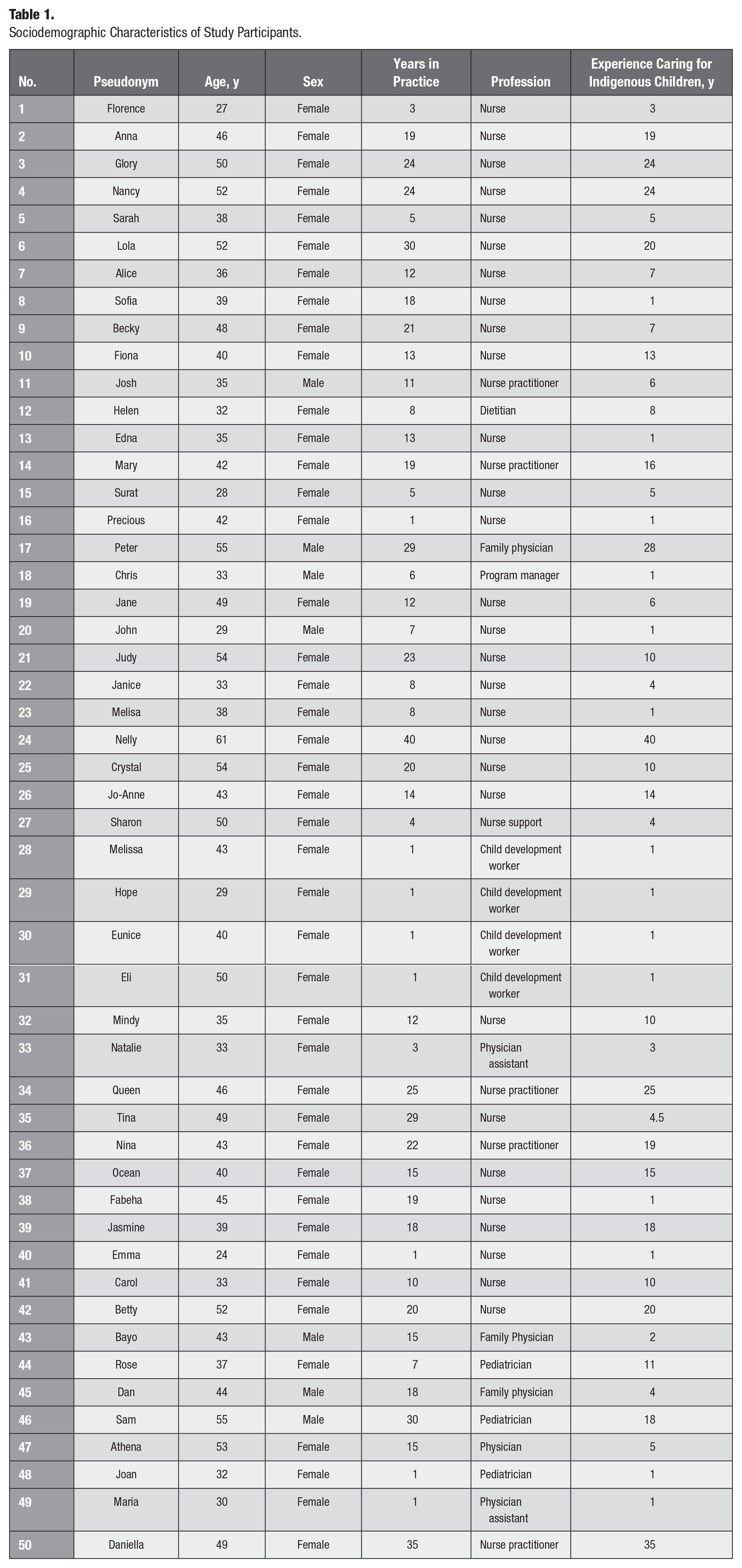
Fifty NDPCPs participated in 8 focus groups and 12 in-depth key informant interviews. The participants consisted of physicians, public health nurses, nurse practitioners, physician assistants, a dietitian, and child development workers (Table 1). The median age of the participants was 41 y, and the median years of practice was 13. In response to the research questions—1) what strategies NDPCPs recommend for implementing the CRA tool in Indigenous primary care and 2) how these can inform broader ECC prevention efforts—we identified 4 interrelated themes. These themes reflect system-level, community-driven, educational, and policy-oriented strategies that NDPCPs consider essential to implementing the CRA tool in a way that is feasible, culturally appropriate, and sustainable. They are presented in order of the number of participants contributing to each theme. Quotes from interviews represent points raised by participants, with pseudonyms and professional designations.
Sociodemographic Characteristics of Study Participants.
Strengthening Primary Care Systems to Support CRA Integration
This theme captures participants’ practical recommendations for embedding CRA into the daily workflows of nondental primary care. NDPCPs emphasized 6 key areas of system-level support: provider training (especially fluoride varnish), management endorsement, streamlined documentation and referral pathways, integration into electronic medical records (EMRs), provision of fluoride and related supplies, and incentives for uptake. These system-focused strategies were seen as foundational for enabling consistent and sustainable CRA use within primary care practices (Table 2).
Key Themes and Subthemes for CRA Implementation.
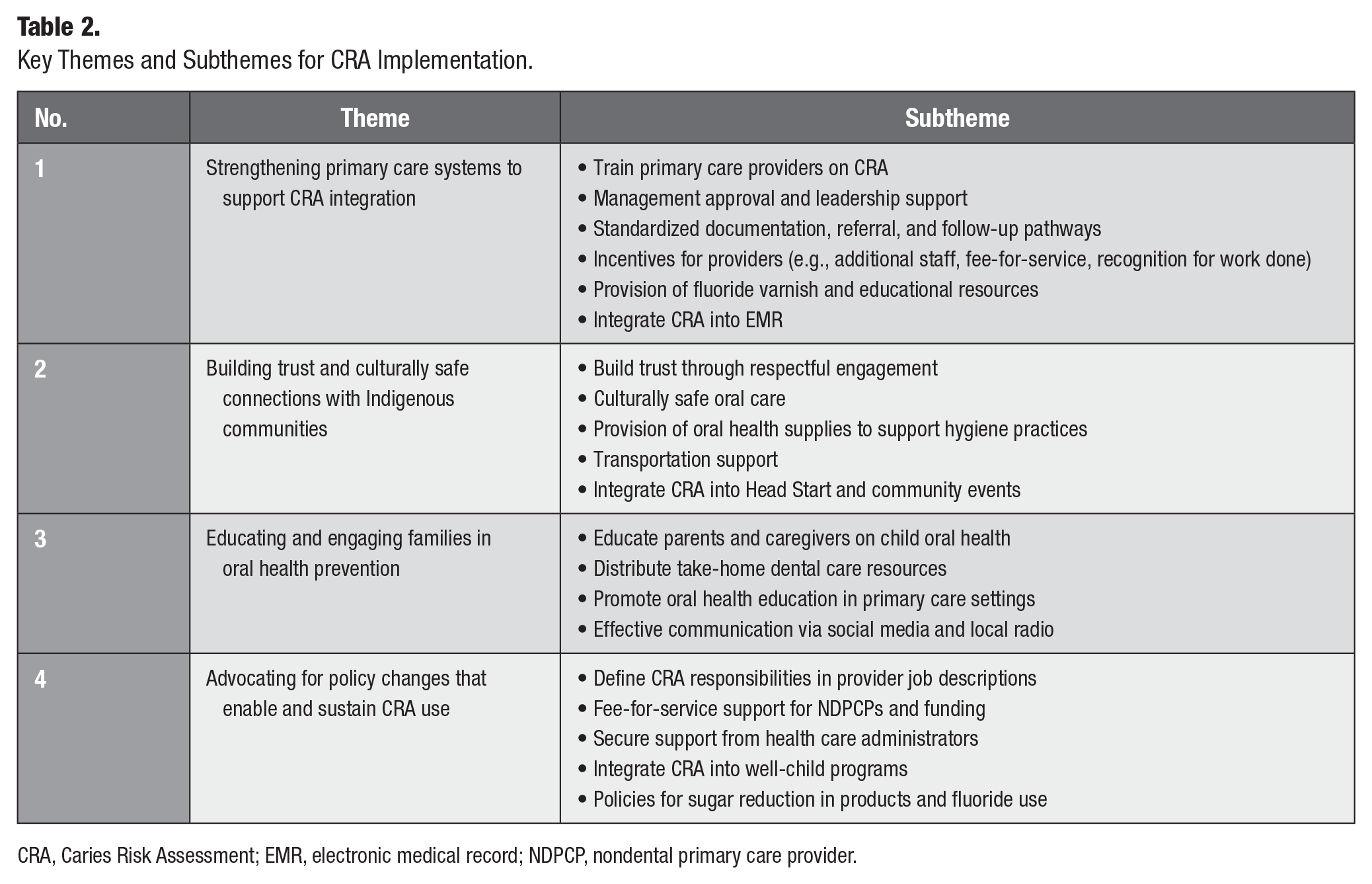
CRA, Caries Risk Assessment; EMR, electronic medical record; NDPCP, nondental primary care provider.
Nearly all participants described the CRA tool as user-friendly but highlighted the need for hands-on training, particularly in fluoride varnish application, as a prerequisite for implementation. Additional training needs included anticipatory guidance and managing young children during oral health procedures: And regarding the fluoride about applying it, I would definitely say we would want some training and maybe tips on how to get a kid to keep their mouth open long enough for me to put fluoride. (Tina, nurse)
Participants emphasized that formal support from health care managers, with designated CRA champions in each clinic, would help staff feel confident and authorized to use the tool: I think having support from the program to use it because I don’t want to get in trouble and have people saying I’m working outside of my scope. . . . I would want the support of the program to go ahead. . . . Nurses are a big part of getting these families dental care. (Alice, nurse) I’m sure our case manager probably would. She would be the one that would have the final say and final answer. Right. (Eli, child development worker) Having a lead person in the office that sort of leads it and is kind of a resource . . . so this would be your responsibility for the contact for whoever is leading it from outside of the office. (Becky, nurse)
Participants also recommended integrating CRA into EMR systems to make documentation more efficient and user-friendly. Standardized fields, auto-calculations, and dropdown options were viewed as helpful for routine use: Just making sure that it’s there and that you can check the boxes. And then it would tally it for you would be really nice. (Edna, nurse)
In addition to EMR integration, referral systems and access to lists of local dentists accepting publicly funded patients were seen as necessary to connect families to care: Knowing which centers are going to be available for patients, particularly of low socioeconomic class, where they can go and get affordable treatment . . . that sort of information will be useful. (Bayo, physician)
Incentives such as fee-for-service models, staff recognition, and additional support for new responsibilities were also recommended. Some participants expressed concern that the added workload would require funding or formal adjustment of duties: The only factors I see to that is the funding. . . . Is our program going to fund us to have that extra time to go out? Be there for the registrations and check the kid’s teeth at the same time? (Nancy, nurse)
The availability of fluoride varnish was a concern for those already using the CRA tool: I don’t think we have any more fluoride. So it’s probably not the greatest idea to use the risk assessment and not be able to apply the fluoride. . . . It’s a little bit problematic. (Josh, nurse practitioner)
Building Trust and Culturally Safe Connections with Indigenous Communities
Participants emphasized that successful implementation of the CRA tool requires trust building, cultural humility, and an understanding of the lived experiences of Indigenous families. Cultural humility is a lifelong process of self-reflection and self-critique that acknowledges power imbalances and emphasizes respectful partnerships with communities by recognizing and valuing their cultural identities, histories, and knowledge systems (Tervalon and Murray-García 1998). Many providers noted that historical trauma, socioeconomic barriers, and negative experiences with health care have created distrust in new systems and tools. As such, CRA implementation must be rooted in relationship-centered care and cultural safety.
This theme included 5 subthemes: building trust through respectful engagement, providing culturally safe and nonjudgmental care, distributing oral health supplies to support daily hygiene, embedding CRA into existing trusted programs (e.g., Head Start), and addressing transportation as a key barrier to follow-up dental care.
Participants described how effective oral health conversations required a deep understanding of families’ realities and values. They noted that questions about feeding or hygiene habits from the CRA tool could be perceived as judgmental, especially when compounded by challenges such as food insecurity or unstable housing: And in those circumstances, there can be a different level of trust and relationship. For those types of conversations as well, right? Like that relationship and power differential can be a challenging piece as well that contributes to this. (Tina, nurse) I think the preamble for using this tool would be very important, right? Because there are a lot of things that can be perceived as judgment of their parenting. . . . It gets a little bit touchy with food as well, right? Different families have different values. (Fiona, nurse)
Providers highlighted the need for culturally safe interactions, especially when working with families affected by trauma, addiction, or systemic racism: Experienced, well-trained providers working with that demographic. . . . Their approach is such that people don’t tend to feel judged, or they try to comfort people and provide care in a way that makes them comfortable to get care. (Alice, nurse)
Practical support measures, such as giving families toothbrushes and child care items, were seen as simple but effective strategies to build rapport and reinforce oral hygiene messages: If it was something that we were looking to be able to offer and have stock here and say “Hey! Here is a new toothbrush, here is some child care,” I think that would be exceptionally helpful because then people are more likely to be able to actually implement. (Tina, nurse)
Participants flagged transportation as a major structural barrier to oral health follow-up, suggesting that CRA efforts should be supported by tangible logistics solutions: And to provide them with transportation to go home after. So let’s say, “Okay, you know what? They made it there, let’s give them bus tokens to get home.” Let’s think things that we can do to sit next to them and say “Hey! You know what? I got this done, this doesn’t suck and they help me get there and they help me get home.” (Nina, nurse practitioner)
Together, these strategies reflect a relational community-informed approach to CRA implementation that goes beyond technical delivery to address trust, comfort, and social realities in Indigenous communities.
Educating and Engaging Families in Oral Health Prevention
NDPCPs highlighted that empowering families through accessible and culturally relevant education is central to the success of CRA implementation. This theme includes 4 key strategies: educating parents and caregivers about child oral health, providing take-home dental resources, promoting oral health messages through trusted community channels, and using communication methods that are engaging and appropriate to varying literacy levels.
Many participants observed that caregivers lacked awareness of the importance of primary teeth, preventive dental care, and appropriate nutrition for young children. Misconceptions such as viewing juice in bottles or certain sugary drinks as healthy were seen as widespread. Participants emphasized that low engagement was often due to limited knowledge rather than willful neglect.
But you know, education for the parents will be very key and important to help with oral hygiene care. So brushing your teeth twice a day and obviously watching what the kids eat and ensuring that they look after their dentition just to prevent complications later on. But yes, it can be prevented if its primary care is taken seriously. (Bayo, family physician)
To reinforce learning beyond clinical encounters, participants recommended distributing simple, visually engaging educational materials. These resources, such as pamphlets or visual guides, could support at-home oral health practices and serve as helpful reminders for caregivers.
So when we’re doing our education, it’s helpful to have like a really nice pamphlet that we can leave with them because, you know, everyone learns different ways . . . and then they might not take it all in when they were there at the visit. So having something to refer to later on is nice too. (Sophia, nurse)
Participants emphasized the importance of community-based communication strategies. Several highlighted that Indigenous communities are already using platforms such as Facebook and local radio to spread health-related information. These channels were seen as effective tools for normalizing CRA and educating families on the role of nondental providers in oral health promotion.
They often in Garden Hill use Facebook in order to get some of the patients and say that, okay, the dentist did show up for this visit and a mass Facebook thing goes out and then lots of people that have been told that they should see the dentist come in for that visit. (Sam, pediatrician)
Together, these strategies reflect participants’ recognition that oral health education must be ongoing, tailored, and accessible and delivered in ways that resonate with families’ realities and communication preferences. By building understanding and confidence among caregivers, NDPCPs saw education and engagement as powerful levers for improving ECC prevention.
Advocating for Policy Changes That Enable and Sustain CRA Use
NDPCPs noted that supportive policies are necessary to institutionalize CRA as part of routine child health care. This theme highlights 4 key areas of advocacy: establishing fee-for-service models for NDPCPs, formally incorporating CRA into existing well-child programs, engaging health care administrators to support implementation at the system level, and introducing upstream strategies to reduce sugar consumption.
Participants consistently noted that without financial incentives or protected time, providers may be unable to sustain CRA activities in already-overstretched clinical settings. Introducing billing codes and compensation models for activities such as CRA assessments and fluoride varnish application was viewed as critical.
Maybe it’s a fee-for-service billing code, so if a physician is doing this as part of their assessment for a well-child, they can be remunerated for their time, you know, providing service. (Josh, nurse practitioner)
Beyond clinical delivery, participants pointed to the need for broader public health measures that support oral health prevention, such as reducing the sugar content in commonly consumed foods and beverages.
If things can be done to reduce the sugar content before they’re even on the shelves that will go a long way. (Bayo, family physician)
Several participants saw opportunities to embed CRA into already-existing touchpoints with families, particularly during routine well-child visits. These visits were viewed as ideal moments for CRA, given the preventative focus and reduced stress as compared with acute care encounters.
Yeah, so like I said, I really think this is like a well-child thing that you’re coming in there, there’s no stresses or anything like they’re coming in there for that. I think that’s the mindset. (Betty, nurse)
Finally, participants noted that policy-level decisions, such as enabling CRA through management directives, training supports, and institutional buy-in, must come from leadership and be embedded in health system processes.
That would definitely be coming from much higher up for that part. . . . We do the education pieces, but yeah, applying the fluoride varnish, I would want training in that if it was implemented through management. (Fabeha, nurse)
Together, these insights reflect NDPCPs’ understanding that policy support from funding to leadership engagement is necessary to implement the CRA tool and embed oral health into the everyday structure of child health care.
Discussion
This qualitative study explored the perspectives of NDPCPs on the implementation and integration of the Canadian CRA tool into primary care for First Nations and Métis children in Manitoba. The study findings provide actionable strategies that can inform culturally responsive oral health integration in underserved communities. These are organized under 4 thematic areas that reflect provider recommendations: strengthening primary care systems, building trust and culturally safe connections, educating and engaging families, and advocating for policy change.
Strengthening Primary Care Systems to Support CRA Integration
While NDPCPs described the CRA tool as user-friendly, they emphasized that successful implementation requires foundational system-level support. The most pressing need identified was training, particularly in fluoride varnish application, for which many providers lacked experience. Participants also expressed the need for training in anticipatory guidance and behavior management. These findings reflect broader literature emphasizing the importance of comprehensive training, technical and relational, for effective preventive dental care (Atchison and Weintraub 2017; Lienhart et al. 2023).
Institutional support was viewed as essential. Endorsement from clinic managers and the presence of local CRA “champions” were seen as enablers of sustained implementation, especially among providers concerned about operating outside their scope. This aligns with research showing that leadership and organizational buy-in are critical to integrating new clinical practices (Christian et al. 2023).
The need for standardized and straightforward documentation was emphasized. Effective ways to document the CRA visit and the referral pathway to dental providers are essential for ensuring consistent application of the CRA tool and for streamlining its use across different settings (Christian et al. 2023). Participants recommended integrating CRA into EMRs to streamline documentation and support referrals. EMR integration was seen as a way to standardize practice, improve data flow, and enhance interdisciplinary care. Literature supports these benefits, noting that EMRs improve efficiency, reduce errors, and support coordinated care (Uslu and Stausberg 2021). Additionally, access to up-to-date directories of dental providers who accept children with public insurance was considered crucial to ensure continuity of care. Participants noted that assessing a child’s caries risk is pointless if there are no available dentists to provide treatment. The Canadian government recently launched the expansion of public coverage for dental services for children through the interim Canada Dental Benefit (October 2022 to June 30, 2024) and the Canadian Dental Care Plan (CDCP; enrollment began June 27, 2024, for children aged <18 y). The purpose of the interim Canada Dental Benefit was to provide low-income families in Canada with financial assistance in accessing oral health care services for eligible children ≤12 y of age (Government of Canada 2022). With the successful implementation of the CDCP, there is optimism that more children will access needed oral health care. Still, access to dental providers will remain a challenge in many rural and remote communities, underscoring the need to improve prevention. Integrating CRA into primary care may facilitate the uptake of the CDCP, especially in Indigenous communities where there is shortage of dental providers.
Beyond logistical integration, participants highlighted that workplace incentives could promote CRA uptake. These included fee-for-service billing, staffing support, and formal recognition of new responsibilities. In the United States, similar incentive models through Medicaid have improved preventive dental service delivery by medical providers (Herndon et al. 2015; Kim et al. 2020; Goldstein et al. 2022; Kranz et al. 2022). Currently, such mechanisms are lacking in Canada. Policies that support medical providers to provide preventive oral health services for infants and toddlers should be implemented in Canada.
Building Trust and Culturally Safe Connections with Indigenous Communities
NDPCPs emphasized that fostering trust and providing culturally safe care are critical for successfully implementing the CRA tool in Indigenous communities. Participants acknowledged that First Nations and Métis families have experienced long-standing systemic inequities in oral health care, which have led to skepticism and reduced engagement with health services (Kyoon-Achan, Schroth, DeMare, Sturym, Edwards, et al. 2021b). To address this, they recommended relationship-based approaches rooted in respect, consistency, and cultural humility.
Embedding CRA into trusted, community-led programs such as the Families First home visiting program was seen as a promising strategy. These programs are already well integrated into family routines and offer a foundation for delivering preventive oral health guidance in a supportive and familiar environment (Healthy Child Manitoba 2010). Leveraging existing relationships with public health nurses could increase community acceptance of CRA and improve access to dental referrals.
The participants stressed the need for culturally safe dental care within Indigenous communities. They recommended meeting patients where they are, recognizing that many have experienced racism and intergenerational trauma. Challenges such as houselessness and a lack of phones often prevent patients from keeping dental appointments, as they may not receive reminder calls. To address this, some participants proposed implementing flexible walk-in clinics, allowing patients to receive care when they are ready, especially those struggling with addiction.
Creating a safe space for children’s oral health was highlighted. Participants noted that parents might avoid dental visits due to fear of judgment for delayed dental visits or having advanced caries. Dental personnel should be trained in trauma-informed care. The CRA tool, for example, requires guidance on feeding practices and dietary habits, but many communities face food insecurity where healthy options are costly or unavailable. Cultural safety and appropriateness are particularly important for First Nations and Métis peoples in light of the history of the colonial health care system in Canada (Auger et al. 2019). Oral health advice should be delivered in a culturally safe manner to be effective (Kyoon-Achan, Schroth, Sanguins, et al. 2021b).
Participants identified that transportation was a major barrier to accessing dental care, with the challenge of making alternative arrangements to travel outside the community. This is due to the frequent lack of publicly funded or private transportation in remote areas, and when transportation is available, it is often very expensive (Hussain 2022). Commuting to care and not having transportation to get there is a challenge faced by First Nations and Métis parents in northern, remote, rural, and urban communities. Many missed dental appointments are linked to inadequate transportation options (Kyoon-Achan, Schroth, DeMare, Sturym, Edwards, et al. 2021a). In Indigenous communities, the scarcity of local dental providers often necessitates travel to other communities or cities for care. Single parents in particular often depend on other community members for transportation. Referring children to the dentist after a CRA will require additional support for parents, including transportation. Missed appointments result in no-show bills, which further discourages families from seeking necessary dental care for their children. Policies should be geared toward availability of affordable transportation for these communities.
Educating and Engaging Families in Oral Health Prevention
Participants identified caregiver education as a critical component of CRA implementation. Many parents were perceived to lack foundational knowledge about early childhood oral health, including the importance of primary teeth, appropriate feeding practices, and early hygiene routines. NDPCPs frequently encountered misconceptions such as the belief that apple juice is a healthy bottle option or that baby teeth do not require regular care. These findings reflect previous literature documenting gaps in oral health literacy among caregivers in underserved communities (Kyoon-Achan, Schroth, Sanguins, et al. 2021; Poirier et al. 2021b). To address these gaps, providers recommended using plain-language, culturally appropriate educational materials that include visual aids. They emphasized the importance of take-home resources such as leaflets and posters that caregivers could reference after clinic visits. Participants also supported providing oral hygiene supplies (e.g., toothbrushes, toothpaste) alongside education to reinforce behavior change and reduce financial barriers. This corroborates a recent study where Indigenous parents in Manitoba recommended ways in which child oral health can be promoted in their communities (Kyoon-Achan, Schroth, Sanguins, et al. 2021b). Some of these recommendations include using culturally appropriate information in local languages, conducting home visits for hands-on teaching, promoting oral health during community health fairs or in schools and daycares, and placing information sheets with visual teaching aids at community centers (Kyoon-Achan, Schroth, DeMare, Sturym, Edwards, et al. 2021b; Kyoon-Achan, Schroth, Sanguins, et al. 2021c). It is interesting to note that there are existing educational resources for parents through our Healthy Smile Happy Child initiative, but perhaps NDPCPs are not aware. To make CRA integration easier, the Healthy Smile happy Child initiative needs to reach out to NDPCPs to provide their offices with these resources to distribute to families (Kyoon-Achan, Schroth, DeMare, Sturym, Sanguins, et al. 2021c). In addition to traditional materials, participants highlighted the importance of effective information dissemination through trusted community channels. Social media platforms such as Facebook, local radio stations, and posters in community centers were seen as valuable tools for promoting oral health messages and raising awareness about CRA. These channels are already widely used in many Indigenous communities to share health information, preserve cultural identity, and promote engagement across all generations (Intahchomphoo et al. 2021). Several NDPCPs also noted that integrating oral health messaging into routine medical visits could help normalize dental care as part of holistic child health. However, participants believed that caregivers and clinic staff may need further orientation to understand and accept the role of NDPCPs in delivering preventive oral health services. Ensuring that families recognize CRA as a credible and beneficial tool was seen as important to fostering uptake and follow-through.
Advocating for Policy Changes That Enable and Sustain CRA Use
NDPCPs emphasized that meaningful integration of CRA into Indigenous pediatric primary care requires policy-level support. Participants advocated for system-wide changes that would embed CRA into routine child health services, backed by clear funding mechanisms, organizational endorsement, and public health alignment.
A central recommendation was the introduction of fee-for-service billing codes to compensate NDPCPs for conducting CRA, applying fluoride varnish, and delivering oral health education. Without financial incentives or formal recognition, participants feared that CRA would remain a low priority in busy primary care settings. This aligns with evidence from US programs where fee-for-service billing models have been successfully implemented in many states. Involving and reimbursing NDPCPs for delivering preventive oral health services has been linked to increased uptake and delivery of these services in medical settings for children (Okunseri et al. 2009; Kranz et al. 2021; Kranz et al. 2022; American Academy of Pediatrics 2024). Participants also recommended integrating CRA into existing well-child clinics and services, positioning oral health as a routine part of early developmental care. By embedding CRA within familiar child health check-ups, NDPCPs believed that uptake could improve without the need for creating entirely new service streams.
Several participants raised concerns about sugar consumption in early childhood, suggesting that policies aimed at reducing sugar in marketed foods and beverages could complement CRA efforts. While fluoride varnish plays a protective role, reducing dietary sugar remains a cornerstone of ECC prevention (van Loveren 2019). Public health strategies that target prevention and broader determinants of oral health were seen as necessary.
Finally, participants stressed the importance of leadership and advocacy from regional and provincial health authorities. Engaging Manitoba Health, Shared Health, and regional health managers will be critical to developing implementation frameworks, coordinating training, and ensuring that CRA-related services are equitably supported across communities.
While NDPCPs play a critical role in integrating oral health into primary care, participants emphasized the need for greater collaboration with dental professionals. In many rural and Indigenous communities, however, limited availability of dental providers presents a challenge to sustained interdisciplinary care. Strengthening pathways for communication and shared care between NDPCPs and dental professionals may enhance the implementation of CRA and improve continuity of care. Future research should explore models of interdisciplinary collaboration that support oral health integration in primary care, particularly in underresourced settings.
Strengths and Limitations
To our knowledge, this is the first qualitative study to explore NDPCPs’ perspectives on implementing the Canadian CRA tool for preschool-aged children. Although focused on First Nations and Métis communities in Manitoba, which could limit the transferability of the study, the findings have broader relevance. Globally, Indigenous and marginalized populations face similar barriers to accessing preventive oral health care, including systemic inequities, workforce shortages, and concerns about cultural safety. This study contributes to the international discourse on integrating oral health into primary care through interdisciplinary, community-based approaches. By illustrating how a CRA tool can be integrated into nondental primary care workflows, our study provides practical insights that may inform similar efforts in other countries working to address disparities in early childhood oral health.
As with most qualitative research, our findings are shaped by the researcher’s role as the primary instrument of data collection and analysis, which introduces the potential for interpretive bias. We mitigated this risk through triangulation and member checking. While the contextual specificity of the Canadian health care system and CRA tool may limit transferability, the broader principles, such as culturally safe care, provider training, interprofessional collaboration, and policy support, are applicable to other international settings aiming to improve early childhood oral health in underserved populations.
Finally, this study focused solely on health care providers’ views. Future research should engage parents and caregivers as the end users to understand their perspectives on integrating the CRA tool into primary care. This will support the design of culturally appropriate, acceptable, and effective interventions.
Conclusion
NDPCPs in Manitoba, Canada, are supportive of integrating oral health care into the primary care of Indigenous children. Key recommendations include training on how to perform CRA, deliver anticipatory guidance, and apply fluoride varnish, as well as securing funding, addressing staffing shortages, improving access to dental resources, and establishing clear referral pathways for children in need of dental care. NDPCPs’ recommendations can inform the implementation of the Canadian CRA tool and the development of policies aimed at improving access to preventive oral health care services for Indigenous children. Integrating the CRA into primary care, supported by relationship-based, culturally responsive approaches, will help promote uptake of the CDCP, especially in Indigenous communities.
Author Contributions
O.O. Olatosi and R.J. Schroth contributed to conception, design, data analysis interpretation, drafted and critically revised manuscript; D. DeMaré, B.-A. Mittermuller, and M. Manigque contributed to data acquisition, interpretation, and critically revised manuscript; J. Edwards, M. Amin, J. Lavoie, and J. Sanguins contributed to interpretation of results and critically revised manuscript; A. Nicolae, P. Chelikani, and P. Wong critically revised manuscript; J. Lamoureux contributed to data acquisition and critically revised manuscript; M. Bertone and K. Yerex contributed to conception and critically revised manuscript; R. Campbell contributed to data interpretation acquisition and interpretation. All authors gave final approval and agree to be accountable for all aspects of the work.
Supplemental Material
sj-docx-2-jct-10.1177_23800844251372545 – Supplemental material for Recommendations for Integrating Caries Risk Assessment into Primary Care for Indigenous Children
Supplemental material, sj-docx-2-jct-10.1177_23800844251372545 for Recommendations for Integrating Caries Risk Assessment into Primary Care for Indigenous Children by O.O. Olatosi, R.J. Schroth, D. DeMaré, B.-A. Mittermuller, M. Manigque, J. Edwards, M. Amin, A. Nicolae, J. Lavoie, J. Sanguins, P. Chelikani, P. Wong, J. Lamoureux, M. Bertone, K. Yerex and R. Campbell, Working Together for Early Childhood Oral Health Study Team in JDR Clinical & Translational Research
Supplemental Material
sj-pdf-1-jct-10.1177_23800844251372545 – Supplemental material for Recommendations for Integrating Caries Risk Assessment into Primary Care for Indigenous Children
Supplemental material, sj-pdf-1-jct-10.1177_23800844251372545 for Recommendations for Integrating Caries Risk Assessment into Primary Care for Indigenous Children by O.O. Olatosi, R.J. Schroth, D. DeMaré, B.-A. Mittermuller, M. Manigque, J. Edwards, M. Amin, A. Nicolae, J. Lavoie, J. Sanguins, P. Chelikani, P. Wong, J. Lamoureux, M. Bertone, K. Yerex and R. Campbell, Working Together for Early Childhood Oral Health Study Team in JDR Clinical & Translational Research
Footnotes
Acknowledgements
The authors wish to thank all the NDPCPs who participated in this study.
A supplemental appendix to this article is available online.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Canadian Institutes of Health Research (202003PJT‑437507‑PJT‑173377) and Research Manitoba PhD Studentship.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
