Abstract
Oral health is integral to general health and supports individuals in participating in society and achieving their potential. Yet, oral diseases are among the most common noncommunicable diseases (NCDs) in the World Health Organization (WHO) African region. The WHO African Regional Oral Health Strategy and the WHO Global Strategy on Oral Health were endorsed in 2016 and 2022, respectively, to address the current alarming situation by integrating oral diseases as part of NCDs toward universal health coverage (UHC). Both strategies highlighted the importance of research, especially the necessity to create and continuously update context- and needs-specific research; however, there is a paucity of information regarding research supporting evidence-informed oral health policies in the region. In this context, the University of Pennsylvania, African universities led by the University of Nairobi, and the WHO Regional Office for Africa initiated an “Evidence to Policy” project. This project consists of 3 phases: (1) preparation: stakeholder analysis; (2) co-creation: online needs assessment survey with oral health academia in the region and 2 scoping literature reviews to identify oral health research and barriers and facilitators for the development, dissemination, implementation, monitoring, and evaluation of oral health policies; and (3) validation: sharing findings from phase 2 through the stakeholder meetings. This executive summary presents the results of phase 3, the stakeholder in-person meeting held in November 2023 in Nairobi, Kenya. About 70 participants, including oral health educators and representatives from the Ministry of Health and WHO in the region, discussed and identified actionable recommendations based on findings from phase 2. Then, participants assessed their alignment with the WHO Global Strategy. At the end of the meeting, participants pledged to maintain the relationships between academia and policy makers and will work collectively toward UHC for oral health for all in the region based on the “Nairobi Declaration.”
Knowledge Transfer Statement:
This executive summary can be used by all key stakeholders involved in creating, disseminating, implementing, monitoring, and evaluating oral health policies in the African region to leverage research and accelerate the implementation of the WHO Global and African Regional Strategies on Oral Health.
Background
Oral health enables individuals to perform essential functions and affects self-confidence, well-being, and ability to socialize and work without pain, discomfort, and embarrassment from early life to old age. However, oral diseases are highly prevalent; 480 million people in the World Health Organization (WHO) African region were estimated to suffer from oral disease in 2019, with social, economic, and health system effects (WHO 2023). Yet, most oral diseases are preventable by controlling for shared risk factors with major noncommunicable diseases (NCDs) (WHO 2023).
To address this situation, the WHO African Regional Oral Health Strategy 2016–2025 and the WHO Global Strategy on Oral Health were endorsed by member states in 2016 and 2022 (WHO 2024), respectively, to address oral diseases as part of NCD prevention and control toward universal health coverage (UHC) for oral health for all by 2030. Both regional and global strategies highlighted the importance of oral health research, especially the necessity to create and continuously update context- and needs-specific research; however, there is a paucity of information regarding research supporting the creation, dissemination, implementation, and monitoring and evaluation (M&E) of evidence-informed oral health policies (OHPs) that have been implemented or what is available in the region.
Given these circumstances, the Center for Integrative Global Oral Health at the University of Pennsylvania, the WHO Regional Office for Africa (AFRO), and the University of Nairobi, in collaboration with policy makers and academia in the region, initiated a project titled “Evidence to Policy: Accelerating the Creation, Dissemination, Implementation, and M&E of Oral Health Policies in the WHO African Region.” This project consisted of 3 phases: (1) preparation: stakeholder analysis; (2) co-creation: online needs assessment survey with oral health academia and 2 scoping literature reviews to identify oral health research and barriers and facilitators for the development, dissemination, implementation, and M&E of OHPs; and (3) validation: sharing findings from phase 2 through the stakeholder meetings, including an online validation meeting held in October 2023 to obtain key insights of oral health focal points in the Ministry of Health (MoH) and WHO country offices in the region.
As part of phase 3, a regional stakeholder in-person meeting was organized in Nairobi, Kenya, on November 15 and 16, 2023, with more than 70 participants, including oral health academicians and administrators (i.e., from institutions that completed the needs assessment survey in phase 2), selected chief dental officers, and representatives from MoHs and WHO in the region (Appendix Table 1), to share the results of phase 2 and develop actionable recommendations to accelerate the creation, dissemination, implementation, and M&E of OHPs in the WHO African region. The following executive summary highlights the results of this regional meeting.
Introduction
At the beginning of the meeting, participants were welcomed by the country representative of the WHO Kenya and the director general of health, MoH Kenya. Both expressed their concern about the high oral disease burden and barriers for research, including limited funding, weak linkages between academia/research institutions and policymakers, inadequate and unequal human resources, and capacity for research for health (R4H), and thus called for a wider collaboration between relevant stakeholders to develop and implement evidence-based, integrated, and comprehensive OHPs.
WHO Strategies on Research and Oral Health
A research focal point from AFRO introduced the regional strategy on R4H and mentioned that research is a key tool for dealing with the complexity of health challenges and an important ingredient in the realization of the UHC agenda. He explained the result of the latest situational analysis of R4H in the region, demonstrating that despite the increase in research, there was a paucity of research on policy and its implementation. This can be attributed to unsustainable financing, which is usually donor driven, coupled with a lack of translation and poor implementation. Therefore, the necessity to “strengthen health research systems capacity, including domestic resource mobilization for R4H,” “set research priorities, including oral health, to meet health needs,” and “conduct locally-led research” was emphasized.
Subsequently, a technical officer for oral health in AFRO underscored the suboptimal investment in oral health in the region in which half of the countries did not have OHPs and more than 70% of the countries spent less than US $1 per person per year on treatment costs for oral health care in 2019 (WHO 2023). She introduced WHO’s recently developed oral health strategies to address this situation and highlighted that research is part of the strategic objectives of the Global Strategy on Oral Health and global targets as part of the Global Oral Health Action Plan. She emphasized global target 6: “By 2030, 50% of countries have a national oral health research agenda focused on public health and population-based interventions.” She further reiterated the proposed actions to translate the research strategy at the country level, namely, prioritizing oral health research of public health interest, including evaluating essential oral health care and integration into primary health care; identifying and addressing barriers to access to oral health care; addressing oral health inequalities; promoting emerging research areas such as digital technologies and environmentally sound practices, including mercury-free dental materials; conducting economic analyses; supporting population-based epidemiological studies; and then translating oral health research findings into practice (WHO 2024).
Plenary Session: Results from the Scoping Reviews and Needs Assessment Survey Informing the Meeting
This session aimed to inform key stakeholders about the results of 2 scoping literature reviews and the online needs assessment survey on OHP and research capacity.
Scoping review 1: Barriers to and facilitators for the creation, dissemination, implementation, and M&E of OHPs in the region
This review aimed at examining barriers to and facilitators for creating, disseminating, implementing, and M&E of OHPs in the region between 2002 and 2022. The findings suggested that most countries lack a country-specific body of evidence to assist policy makers in anticipating barriers to and facilitators for OHPs. Financial constraints, a limited and poorly organized workforce, deprioritization of oral health, absence of health information systems, inadequate integration of oral health services within the NCD agenda and the health system, and limited oral health literacy are commonly encountered challenges.
Aspects identified as facilitators include a renewed commitment to establishing national OHP, diversification of the oral health workforce, and an increased understanding of the influence of social determinants of health among oral health care providers. Advancing OHPs must consider different barriers and facilitators suitable for diverse subnational, national, and regional conditions and circumstances (Verdugo-Paiva et al. 2024).
Scoping review 2: Scope and output of oral health research from 2011 to 2022 in the WHO African region
This review compiled information on oral health research in the Sub-Saharan region, which can be used as a starting point for establishing a regional research agenda.
In the past decade, the number of published research articles on oral health in the WHO African region has remained largely unchanged, averaging 114 oral health–related articles annually. Of the 1,379 oral health–related research articles published between 2011 and 2022, 1,053 (76.4%) were cross-sectional studies. There was a general lack of evidence synthesis studies (systematic reviews and policy briefs) necessary to inform national and regional policies as well as the development of clinical guidelines and other context-specific interventions.
The top 5 research areas constituting more than three-quarters of all research publications (76.4%) were dental public health (21.5%), general dentistry (20.2%), pediatric dentistry (12.0%), oral and maxillofacial surgery (11.4%), and oral and maxillofacial pathology (11.3%). This review revealed that 82% of the research being undertaken in the region largely focused on the problems and causes, and only 18% focused on implementation and evaluation research.
Participants in research studies from Nigeria accounted for 46.2% of all the research output in the 2011 to 2022 period in the WHO African region, followed by South Africa (9.2%). These 2 countries also accounted for the highest numbers of collaboration networks within researchers and institutions within the WHO African region. Research infrastructure was generally poor or lacking altogether, and more trained personnel to carry out high-quality, context-specific research is needed (Labarca et al. 2024).
Online needs assessment survey: OHP and research capacity—Perspectives from dental academic institutions in Africa
The objectives of the survey, which targeted deans or their designees at dental schools, were to determine how dental schools contribute to OHPs in the region, the barriers and facilitators they face when engaging with other local stakeholders, and their capacity to respond to population and public health needs.
The results demonstrated that the capacity for dental schools in the region to respond to population and public health needs varied. Most schools have graduate programs to train the next generation of researchers. However, these programs have limitations that may hinder the students from achieving the necessary skills and training. Most (75%) respondents were aware of the existence of national OHPs and encountered myriad challenges when engaging with them, including a lack of coordination with other stakeholders, resources, and oral health professionals and the low priority given to oral health. Their strengths as technical experts and researchers were a common theme in the reported facilitators for engaging with OHPs (Urquhart et al. 2024).
Group Discussions and Workshops
After the plenary session, all participants joined together in group discussions and workshops to identify actionable recommendations to address barriers and facilitators associated with OHPs as well as gaps and opportunities in research identified from the results of the scoping literature reviews and the needs assessment survey. These group discussions were organized to answer semi-structured questions that addressed the findings from the scoping reviews and the needs assessment survey. Further, participants determined which key actionable recommendations aligned with the objectives of the Global Strategy on Oral Health. If addressed, these could have far-reaching positive impacts on the creation, dissemination, implementation, and M&E of OHPs.
Plenary Session to Receive Reports from All Group Discussions and Workshops
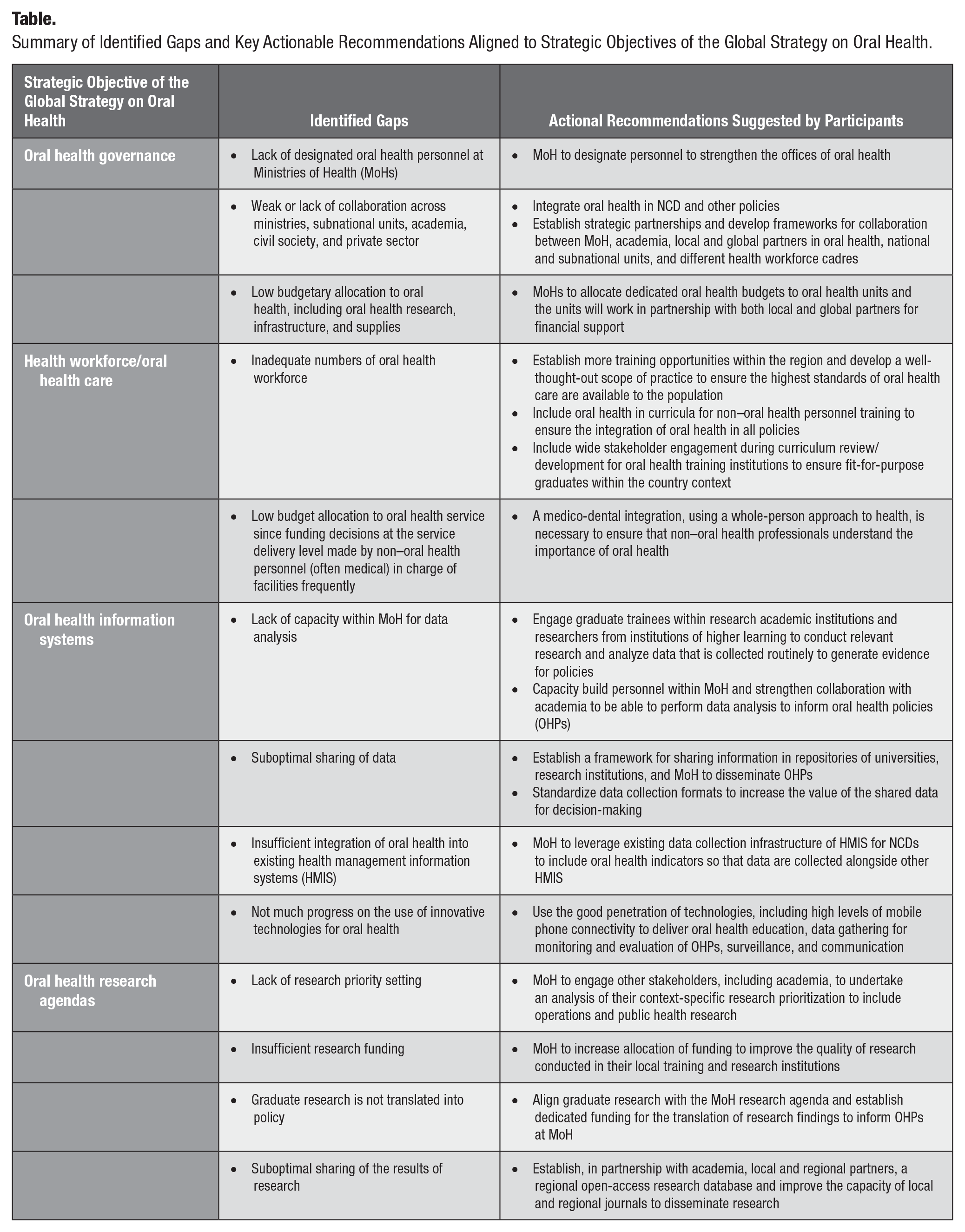
During this plenary session, recommendations and summaries derived from the group discussions and workshops were presented. All participants had the chance to hear from various groups and to edit, amend, and align proposed outcomes. The Table summarizes the results of this session.
Summary of Identified Gaps and Key Actionable Recommendations Aligned to Strategic Objectives of the Global Strategy on Oral Health.
Outcome of the Meeting and Recommendations
Deliberations from the meeting led to the Nairobi Declaration, a list of 10 key recommendations. Participants who are leaders of academia and oral health within MoHs, as well as global and local partners, committed to ensuring implementation within their countries.
Nairobi Declaration
Strengthening collaboration between academic institutions and MoHs through the establishment of formal partnerships and communication channels
Encouraging active government support and involvement for oral health research and policy activities, including prioritizing oral health research agendas and securing and allocating dedicated and sustainable funding
Building research capacity in oral health, including by developing and implementing training programs and mentorship schemes to enhance skills in oral health research, particularly in implementation science and policy evaluation
Engaging a wide range of stakeholders, such as nongovernmental organizations, patient advocacy groups, professional associations, the private sector, and international health organizations in OHP development and implementation
Integrating oral health in all policies through active efforts to incorporate oral health into all policies and programs across the life course
Utilizing digital technologies and leveraging digital platforms, including social media, institutional websites, and online repositories, to disseminate OHPs and research findings
Prioritizing and focusing research efforts on identifying practical solutions, effective implementation strategies, and robust evaluation methods while ensuring that research priorities align with public needs and challenges in oral health
Establishing and fostering collaboration at national and regional levels to share resources, expertise, and best practices
Developing and disseminating evidence-informed policies, guidelines, and standards for oral health practice, research, and policy implementation
Including oral health, public health, and population-based oral health research in curricula for health professionals
Author Contributions
R. Mutave, A. Carrasco-Labra, Y. Makino, contributed to conception and design, drafted the manuscript; P. Muange, O. Urquhart, A.S. Bhosale, J.C. Okeibunor, contributed to conception, critically revised the manuscript; M. Glick, contributed to conception and design, critically revised the manuscript. All authors gave their final approval and agree to be accountable for all aspects of work.
Supplemental Material
sj-docx-1-jct-10.1177_23800844241291529 – Supplemental material for Executive Summar Executive Summary of a Regional Meeting to Accelerate Oral Health Policies in the WHO African Region y of a Regional Meeting to Accelerate Oral Health Policies in the WHO African Region
Supplemental material, sj-docx-1-jct-10.1177_23800844241291529 for Executive Summar Executive Summary of a Regional Meeting to Accelerate Oral Health Policies in the WHO African Region y of a Regional Meeting to Accelerate Oral Health Policies in the WHO African Region by R. Mutave, P. Muange, A. Carrasco-Labra, O. Urquhart, A.S. Bhosale, Y. Makino, J.C. Okeibunor and M. Glick in JDR Clinical & Translational Research
Footnotes
Acknowledgements
We acknowledge the contribution of participants of the Regional Meeting on Evidence to Policy: Accelerating the Creation, Dissemination, Implementation, and Monitoring and Evaluation of Oral Health Policies in the WHO African Region (![]() ). The Center for Integrative Global Oral Health, School of Dental Medicine, University of Pennsylvania, funded the scoping reviews and needs assessment survey. The regional meeting in Nairobi, Kenya, was funded by the Penn Global Engagement Fund and School of Dental Medicine, University of Pennsylvania, with support from Colgate Palmolive, CareQuest Institute for Oral Health, and Dentsply Sirona. The authors are responsible for the views expressed in this article, and they do not necessarily represent the views, decisions, or policies of the institutions with which they are affiliated.
). The Center for Integrative Global Oral Health, School of Dental Medicine, University of Pennsylvania, funded the scoping reviews and needs assessment survey. The regional meeting in Nairobi, Kenya, was funded by the Penn Global Engagement Fund and School of Dental Medicine, University of Pennsylvania, with support from Colgate Palmolive, CareQuest Institute for Oral Health, and Dentsply Sirona. The authors are responsible for the views expressed in this article, and they do not necessarily represent the views, decisions, or policies of the institutions with which they are affiliated.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
A supplemental appendix to this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
