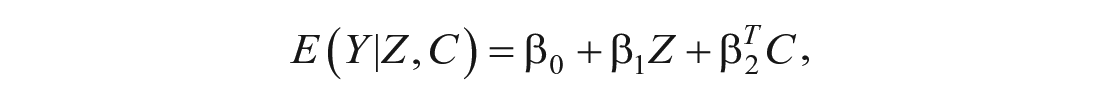Abstract
Head Start is a federal antipoverty program that provides free childcare, preschool, and related services to disadvantaged families. Research on Head Start has focused almost exclusively on impacts among children. Using data from the Head Start Impact Study, a nationally representative field experiment, the authors estimate treatment effects on maternal employment, economic hardship, and depression. The authors find that Head Start admission generates some improvements among Black mothers but not among other subpopulations. In analyses accounting for treatment intensity, noncompliance, and program substitution, the authors find suggestive evidence that Head Start participation may lead to even greater improvements in these outcomes specifically among Black mothers who would otherwise look after their children at home and when they participate in the program full-time. In conclusion, Head Start likely improves outcomes for some groups of low-income mothers, but these effects are heterogeneous, and they may be small, dose-dependent, or otherwise difficult to detect for many women.
Access to affordable childcare is widely thought to promote upward economic mobility for low-income parents, and especially for low-income mothers (Forry and Hofferth 2011; Morrissey 2017; Press, Fagan, and Laughlin 2006). Without access to affordable care, low-income mothers face a difficult dilemma: they can work but then must dedicate much of their earnings to costly childcare services, or they can withdraw from the paid labor force to care for their children but then must forego an important means of transcending poverty. Navigating this dilemma has only become more challenging in recent decades. Broad shifts in the economy, culture, and family have increasingly brought mothers of young children into the paid labor force, while the real costs of childcare have increased substantially (DeSilver 2014; Joughin 2021). At the same time, low-income mothers now have fewer options for supporting their families outside of employment for wages. After the Personal Responsibility and Work Opportunity Reconciliation Act was passed in 1996, mothers in poverty began to face stringent work requirements to qualify for meager cash benefits, whose value has been eroded by inflation over time (Parolin 2021). The intersection of waning and increasingly restrictive public assistance with the high prevalence of working motherhood and escalating childcare costs has made it difficult for low-income women with children to improve their lives.
The difficulty of balancing work with childcare interferes with the ability of low-income mothers to maintain stable employment, avoid economic hardship, and protect their mental health (Edin and Shaefer 2015; Henly and Lyons 2000; Newman 1999). Childcare costs are inversely related to women’s employment overall (Han and Waldfogel 2001), and a large volume of evidence shows how an absence of affordable care disrupts the efforts of low-income mothers to secure a job and, by extension, achieve financial stability (Henly and Lyons 2000; Morrissey 2017; Scott, London, and Hurst 2005). A lack of affordable childcare can also force low-income mothers into overcrowded and/or precarious living arrangements with other adults, which may have potentially negative consequences for both their physical and emotional well-being (Edin and Shaefer 2015). The chronic stress that arises from daily navigating these challenges may increase feelings of depression and anxiety (Evenson and Simon 2005).
The Head Start program holds promise for alleviating at least some of the challenges associated with low-income motherhood. Head Start is a large, federally funded antipoverty program that provides center-based early childhood education, among several other services, to disadvantaged children at no cost to their families. Because this program provides low-income mothers with childcare, preschool, and related services for free, participation may allow them to work for pay with less difficulty, improve their economic position by boosting consumption or savings, and relieve at least some of the stressors linked with balancing employment and care obligations. Few studies, however, have examined the impact of Head Start on maternal rather than child outcomes, and their results are mixed (e.g., Landivar et al. 2022; Sabol and Chase-Landale 2015).
In this study, we investigate whether participation in Head Start improves the well-being of low-income mothers. To this end, we use data from the Head Start Impact Study (HSIS), a nationally representative field experiment in which eligible participants were randomly assigned to a control group or an experimental group that was offered admission to Head Start. Because the HSIS collected follow-up data from both participating children and their caregivers, we use the experiment to explore program impacts on mothers. Specifically, we extend prior research by estimating the effects of Head Start participation on a wide array of maternal outcomes, including measures of employment, economic hardship, and mental health. We also consider whether the effects of Head Start on mothers differ by race or family income, as program impacts are likely heterogeneous and may be more pronounced among those facing greater initial disadvantages. In addition, because a nontrivial number of families assigned to the HSIS control group sought out alternative forms of center-based childcare, most of which were themselves highly subsidized, we attempt to disentangle the consequences of program substitution, which can include unduly negative assessments of program effectiveness if participants receive similar services absent the focal intervention (Heckman et al. 2000; Kline and Walters 2016). Finally, we also consider whether the effects of Head Start participation are more pronounced when mothers send their children for a longer period of time each week.
Using instrumental variable (IV) methods, where experimental assignment is used to instrument for treatment receipt, we find that participation in Head Start generates improvements in employment, economic stability, and mental health among Black mothers, but we uncover little evidence of program effects among other subpopulations. We also find suggestive evidence that inattention to treatment intensity and program substitution may lead to estimates that understate the beneficial impacts of Head Start for mothers. In another set of analyses, we parse the effects of hours spent in Head Start and competing childcare services relative to home care by using an alternative IV approach with interactions between experimental assignment, family covariates, and center characteristics. Results from this analysis suggest that participation in Head Start may lead to even larger improvements in maternal well-being among Black mothers who would otherwise look after their children at home and when they participate in the program full-time.
This study contributes to research on antipoverty policy and low-income motherhood in several ways. First, we provide experimental estimates for the effects of a large, federally funded early childhood program on a range of outcomes among low-income mothers. Second, we examine multiple sources of heterogeneity in these effects across different subpopulations. And third, we outline several problems related to treatment intensity and program substitution, and we take initial steps toward disentangling their impact on our inferences.
The Head Start Program
Head Start provides childcare, preschool, and related services to disadvantaged children and their families. The program adopts a comprehensive approach to early childhood development, offering not only center-based care and education but also home wellness visits, parenting classes, social networking opportunities, and a bridge to additional public services, such as health care, nutrition, and housing assistance, for enrolled children and their parents (Vinovskis 2008). Funded largely by federal grants awarded to local organizations, Head Start is free to participants. Eligibility for the program is limited to children aged three to four years in families that fall at or below the federal poverty threshold, although a small portion of a center’s enrollment may also come from families with higher incomes. The program currently serves around one million children per year and costs the U.S. government over $6 billion annually (U.S. Department of Health and Human Services 2020).
The effects of Head Start participation on children have been extensively studied. Children who attend Head Start are better prepared for kindergarten than similar children who do not attend any preschool program (Phillips et al. 2017). Head Start attendance also improves children’s cognitive test scores, although these effects appear to “fade out” after the program ends and children enter primary school (Puma et al. 2012). Beyond indicators of school readiness and test scores, research on Head Start indicates that the program has positive effects on later life outcomes among participating children, including higher educational attainment, fewer adolescent pregnancies, greater earnings, and improved health (Currie and Thomas 1995; Garces, Thomas, and Currie 2002; Ludwig and Miller 2007).
Although research on the effects of Head Start has focused mainly on children and typically assumes that any improvements for this population are driven by center-based instruction, the program may also affect parents, and especially low-income mothers, in positive ways. Moreover, improvements for parents could, in turn, contribute to or enhance the program’s impacts on their children, given the powerful connection between family environments during early childhood and later life chances. Studying the effects of Head Start on maternal outcomes is therefore essential for building a holistic understanding of existing policy remedies for poverty.
Head Start Participation and Maternal Well-Being
Finding affordable and high-quality childcare is a struggle for low-income mothers, and these difficulties often stymie their efforts to achieve upward economic mobility (Henly and Lyons 2000; Morrissey 2017; Scott et al. 2005). The Head Start program holds the potential to improve the well-being of low-income mothers by reducing the costs of entering the paid labor force and boosting consumption or savings, by relieving stressors associated with working while caring for young children, and by connecting them to a support network composed of other parents and service providers.
In conventional economic models, the cost of childcare acts as a “tax” on wages: for each hour that a single mother works, she must pay someone else to care for her children. Thus, a mother’s take-home pay from employment, and by extension her labor supply, should decrease with the price of childcare. Access to subsidized childcare lowers or eliminates the “childcare tax” on a mother’s wages, which will either increase her labor supply or allow the same level of consumption while working less (Kimmel 1995; Tekin 2007). Decisions to enter the labor force or work additional hours are surely more complex than is implied by abstract models of utility maximizing agents, but this complexity notwithstanding, it is reasonable to expect that working will generally be easier for low-income mothers when they are less burdened by the high costs of childcare because they have access to a Head Start program.
Because of their precarious employment situation, low-income mothers commonly suffer economic hardships. These hardships can include a near total absence of cash income, food insecurity, utility service shutoff, exposure to overcrowded and dilapidated housing, and residential instability (Edin and Shaefer 2015; Newman 1999). Because the costs of housing have escalated in tandem with the costs of childcare in many cities, rent now accounts for more than half of the typical poor family’s budget (McConnell 2012; Newman and Holupka 2014). In this situation, even minor disruptions to steady employment or work hours can expose low-income families to eviction and plunge them deeper into poverty (Desmond and Kimbro 2015; Edin and Lein 1997). If access to Head Start increases maternal employment or retained earnings, it should also help low-income families avoid these forms of economic hardship by allowing greater spending on other essential goods and services.
The experience of material deprivation can lead to mental health problems. Qualitative studies have documented cases where food and housing insecurity have forced low-income mothers into perilous “survival strategies” that are emotionally taxing and can lead to psychological distress (Belle 1990; Edin and Lein 1997; Edin and Shaefer 2015). Without access to affordable childcare, parents struggling to balance work with child-rearing may rely on informal care arrangements, such as leaving children with neighbors or distant relatives. Although these arrangements are often convenient, cost-effective, and enriching, in some situations they can be unstable or even expose children and their mothers to abuse (Edin and Shaefer 2015; Henly and Lyons 2000). Partly because of these challenges, single parents with minor children report very high rates of depression (Evenson and Simon 2005; Henderson, Harmon, and Newman 2016). By providing free childcare and early education, access to Head Start may relieve some of these stressors and improve the mental health of low-income mothers.
Head Start may also help cultivate larger and more supportive social networks for low-income mothers (Small 2009). Because the program provides opportunities for parents to interact with each other and to engage with their children’s center, participation in Head Start may increase social capital and, in turn, improve the well-being of caregivers through these connections. In addition, Head Start provides other social services to families beyond childcare that may bolster the support system available to parents. For example, the program aims to connect participating families with medical, nutrition, and mental health services, and staff may refer parents to other agencies for help with obtaining stable housing, continuing their education, or finding employment. If participation in Head Start enriches the social networks of low-income mothers and connects them with other social services, this may contribute to securing paid employment, attenuating financial hardships, and improving mental health as well.
Few prior studies have empirically evaluated the effects of Head Start on maternal well-being, despite a strong theoretical rationale for anticipating significant improvements. Specifically, no prior studies, to our knowledge, have examined the effects of Head Start on mental health among low-income mothers, and only a handful have investigated effects on indicators of economic hardship or maternal employment (Landivar et al. 2022; Pihl 2022; Sabol and Chase-Landale 2015; Schiman 2022; Schochet and Padilla 2022; Wikle and Wilson forthcoming). Their results, moreover, are mixed, with some showing that Head Start participation broadly improves labor market outcomes for mothers (Landivar et al. 2022), some that the program has no impact (Sabol and Chase-Landale 2015) or possibly even deleterious effects on maternal employment (Pihl 2022), and still others demonstrating beneficial effects but only for select subpopulations (Schiman 2022; Schochet and Padilla 2022; Wikle and Wilson forthcoming).
These mixed results may reflect the complexities of treatment intensity, effect heterogeneity, and program substitution. Some Head Start centers provide care only for half days. If mothers have access to Head Start but only for a short period of time, they may still encounter difficulties with increasing their labor supply. Head Start also provides services that can be obtained in roughly comparable form through other programs or organizations. The presence of these close substitutes can complicate the task of program evaluation by obscuring evidence of positive impacts in conventional analyses of treatment effects. Finally, Head Start impacts may vary across different groups of mothers, and in the presence of effect heterogeneity, conventional analyses of treatment effects can also obfuscate improvements in maternal outcomes.
Treatment Intensity
Head Start provides only one or two years of care for children nearing the start of kindergarten, and some centers only operate part-time. When the HSIS was fielded, a Head Start center could satisfy minimum program requirements by offering as few as 3.5 hours of instruction per day, over 4 days per week, for just 128 days per year. Consequently, more than half of participating children are enrolled in Head Start for less than 35 hours per week. Such limited hours of operation may not offset the challenges of entering the labor force while raising young children, especially given the growing prevalence of irregular work schedules in the low-wage sector. These considerations suggest that the amount of time that mothers can send their children to Head Start may shape the program’s impact on their employment, and by extension, their economic and emotional well-being.
The limitations of Head Start as a form of subsidized childcare also suggest that alternative care subsidies offering greater or more flexible coverage, such as state-funded preschool or childcare fee assistance vouchers, may better serve low-income mothers. Indeed, the weight of the evidence from a large volume of research indicates that the provision of childcare vouchers, universal preschool programs, and kindergarten expansion leads to significant increases in maternal employment (e.g., Baker, Gruber, and Milligan 2008; Cascio 2009; Morrissey 2017; Tekin 2007), although results from experimental or quasi-experimental evaluations of these programs are sometimes more ambiguous (Havnes and Mogstad 2011; Michalopoulos 2010; Michalopoulos, Lundquist, and Castells 2010).
Effect Heterogeneity
The effects of Head Start on low-income mothers are likely heterogeneous. In general, we expect the largest improvements to accrue to those with the most to gain: mothers well below the federal poverty threshold or who suffer from separate but compounding sources of disadvantage.
Attention to effect heterogeneity is important when evaluating Head Start and maternal well-being because participating families often rely on several other means-tested programs for which eligibility must be recertified at regular intervals, such as Medicaid or the Supplemental Nutrition Assistance Program. If mothers increase their work hours to the point that their income exceeds certain thresholds, they may become ineligible for these programs or have their benefits reduced, which presents a disincentive to additional employment. This suggests that Head Start participation may primarily affect mothers of more limited means, for whom additional income will not place their benefit eligibility at risk.
Beyond the disincentives arising from means testing, women with children in more financially stable households may be less sensitive to Head Start because they already have higher initial labor market participation and/or reliable access to alternative childcare arrangements. In Norway, for example, the expansion of kindergarten eligibility had little effect on labor supply among mothers with higher initial earnings because most were already working, but among mothers with low initial earnings, emp-loyment increased by more than 10 percentage points (Finseraas, Hardoy, and Schøne 2017). Thus, any effects of Head Start on maternal well-being may be most pronounced among families with fewer resources prior to entering the program.
The effects of Head Start may also be larger for mothers who encounter multiple, intersecting forms of disadvantage. Membership in a marginalized racial group, in particular, shapes the experience of poverty in the United States. Among low-income mothers, Hispanic and especially Black women are much more likely than their White counterparts to live in disadvantaged neighborhoods that may be isolated from employment opportunities, contain fewer potential spouses with stable incomes, or lack affordable childcare options (Reardon, Fox, and Townsend 2015; Wilson 1996). Under these compounding disadvantages, access to Head Start may generate larger improvements in maternal well-being among Black and Hispanic mothers.
Program Substitution
Head Start is not the only form of subsidized childcare and early education available to low-income families. Many areas offer public preschool programs, and these services have expanded over time (Cascio and Schanzenbach 2013). In addition, states receive federal block grants from the Child Care and Development Fund, which support vouchers for low-income families that can be redeemed at private childcare centers and preschools. Funds from Temporary Assistance for Needy Families are also commonly used for this purpose (Schumacher, Greenberg, and Duffy 2001). Thus, low-income parents may have access to several programs providing similar services.
In experimental evaluations, standard intent-to-treat analyses may understate program impacts if many participants receive similar services in the absence of the focal intervention (Heckman et al. 2000). In the HSIS specifically, about one third of participants assigned to the control group enrolled in an alternative form of center-based care, most of which were themselves heavily subsidized. Comparing outcomes among mothers who received an offer to enroll in Head Start with those who did not would therefore involve a contrast between two groups in which many members of each are receiving similar services, even if compliance with Head Start assignment were perfect.
Moreover, if compliance is imperfect, analyses aimed at recovering the impact of a program among those induced by the offer of admission to participate may also yield unduly negative assessments of program benefits in the presence of similar substitutes. For example, if a randomly assigned offer of admission to Head Start shifts participants between different types of subsidized center-based care, analyses that use treatment assignment to instrument for Head Start participation recover a weighted average of two different effects: one capturing the effect of Head Start versus home care among those who switch to Head Start from home care when offered admission, and another capturing the effect of Head Start versus an alternative form of center-based care among those induced by treatment assignment to move from center care into Head Start (Kline and Walters 2016). Because participating in one versus another form of subsidized center-based care may not appreciably affect maternal outcomes, it is important to account for this type of program substitution when evaluating effects on low-income mothers.
Method
To investigate whether Head Start improves the well-being of low-income mothers, we use data from the HSIS, a randomized controlled field experiment conducted by the U.S. Department of Health and Human Services (2018). As part of the experiment, more than 4,000 families with an eligible child were randomly assigned to either a treatment group that was offered access to Head Start or a control group that was not offered access. Baseline data were collected through surveys administered during the fall of 2002 (wave 1), when Head Start admits first entered the program. Follow-up data were then collected in the spring of 2003 (wave 2) and every year thereafter (waves 3–5) until participating children had reached first grade. Our analytic sample includes n = 3,406 identifiable mothers of a child participating in the HSIS at baseline, and inferences target the population of women with children who are eligible for the program. We exclude families in the HSIS if the mother does not live in the same household as the participating child (171 cases) or if they did not respond to the parental survey at baseline (865 cases). Parallel analyses that include these cases and multiply impute their missing data yield similar results.
Measures
We first consider a measure of treatment assignment, denoted by Z, which is coded 1 if a sample member received an offer to enroll in Head Start and 0 otherwise. Although participants were randomly assigned to these treatment and control groups at baseline, some who received a Head Start offer did not enroll in the program, while others without an offer were admitted to a different Head Start program elsewhere or they reapplied and enrolled later in the year. To account for this type of noncompliance, we also consider a measure of treatment receipt, denoted by A, which is coded 1 if a sample member’s child was actually enrolled in a Head Start program at the time of their wave 2 interview and 0 otherwise. In addition, among sample members assigned to the control group, some enrolled their children in alternative forms of subsidized, center-based care that provided services similar to Head Start. To account for this type of program substitution, we consider a sample member’s childcare arrangement, which is a polytomous variable, denoted by D ∈ {h, c, m}, indicating whether the child was in Head Start (h), another type of center-based care (c), or home care (m) at wave 2 of the HSIS. Finally, we also consider a measure of treatment intensity, which records the number of hours a sample member’s child typically spends in Head Start each week.
Alternative center care includes all forms of public or private childcare and preschool provided within an institutional setting. About two thirds of sample members using alternative center care report that they incurred no costs to attend, indicating that, like Head Start, this care arrangement is also highly subsidized. Home care refers to all forms of childcare provided within a private residence. Most home care—about 75 percent—is performed by a parent, while the remaining 25 percent consists of care performed by other family members or extrafamilial adults. In an ancillary analysis, we recoded home care provided by someone other than a parent as “alternative center care,” and the results were similar (see Table S1 in the Online Supplement). Among those using Head Start, children of sample members spend 25 hours per week in the program, on average, with a standard deviation of about 9 hours.
Our outcomes of interest include measures of employment, economic hardship, and depression. Maternal employment is measured with two different indicator variables. The first captures any form of employment and is coded 1 for mothers who work full-time or part-time and 0 otherwise, while the second specifically denotes that a mother is working full-time, defined as 35 or more hours per week in paid employment. We measure economic hardship using a count variable that records the number of times a sample member answered “yes” to queries about whether they had (1) difficulty paying rent, (2) difficulty paying the electricity bill, (3) difficulty buying food, or (4) difficulty buying clothes over the past three months. Maternal depression is operationalized using standardized scores on the Center for Epidemiological Studies Depression Scale (CES-D; Radloff 1977). We focus on measures of these outcomes taken at wave 2 of the HSIS.
We also adjust for a set of baseline covariates measured at wave 1 to improve the precision of our experimental estimates. These covariates include maternal race, education, marital status, and age; whether a mother’s participating child was diagnosed as having special needs; whether this child was part of the three- or four-year-old study cohort; household income and size; urban residence; whether Spanish was the primary language spoken in the household; whether there were other children younger than six years in the household besides the participating child; and finally, whether the participating child’s father was present at home. In addition, we adjust for baseline measures of all maternal outcomes after first residualizing them with respect to treatment assignment. By adjusting for a residual transformation of the baseline outcomes, we can improve the precision of our effect estimates on outcomes measured later while circumventing the possibility that we have “controlled away” any anticipatory impacts of program participation at wave 1 of the HSIS (Wodtke 2020).
Maternal education is expressed as a series of indicator variables denoting whether a sample member did not complete high school, earned a high school diploma or passed a General Educational Development test, or completed at least some college. Mothers are classified as Black, White, or Hispanic on the basis of their racial self-identification in caregiver surveys or on forms collected during the recruitment phase of the HSIS. A small number of sample members who identified as another race are pooled with White mothers. Marital status is coded 1 if a sample member is currently married and 0 otherwise. Maternal age is an indicator variable denoting whether a sample member had her first child before turning 19. Whether a mother’s participating child had been diagnosed as special needs or was part of the 3- versus 4-year-old study cohort were also coded as indicator variables. Household income refers to the amount of money income, in 2002 dollars, that accrued to the household over the previous month. Household size is a count of the total number of people living in a sample member’s home at baseline. Urban residence is coded 1 if the participating child was randomly assigned to a Head Start center located in or adjacent to a metropolitan area. Indicator variables are also used to capture whether a sample member speaks mainly Spanish at home, whether there are other children younger than 6 years in the household, and whether a participating child’s father lives in the household.
In addition to these covariates, we also account for several characteristics of the Head Start center to which a mother initially applied for admission at the time of her recruitment to the HSIS. These include an indicator variable capturing whether the Head Start center provided transportation for children, an indicator denoting whether the center provided full-time care (i.e., ≥35 hours per week), and an index of center quality constructed by combining information on the training and education of its staff, class size, frequency of math and literacy activities, availability of home visits, and the provision of health and nutrition services.
Analyses
We first consider the intent-to-treat effect (ITT) of a Head Start offer on each of the maternal outcomes outlined previously, which is the policy-relevant estimand in this analysis. The ITT can be defined as follows:
where Yz denotes a sample member’s potential outcome had they been assigned to treatment z, possibly contrary to fact. It captures the expected difference in an outcome of interest if mothers in the target population had, rather than had not, received an offer to enroll in Head Start. It can be identified under the assumption that the potential outcomes, Yz, are independent of a sample member’s assigned treatment, Z, which is met by design in the HSIS because Head Start offers were randomized (Rubin 1974). It can be consistently estimated simply by comparing the sample mean of the outcome in the treatment and control groups, but to improve precision, we estimate the ITT using a linear model with the following form:
where C denotes the vector of baseline controls, Y denotes the observed outcome, and β1 captures the effect of interest.
The ITT does not account for noncompliance or program substitution. To address the problem of noncompliance, we next consider a local average treatment effect (LATE) of sending a child to Head Start rather than merely receiving an offer of admission (Angrist, Imbens, and Rubin 1996; Imbens and Angrist 1994). This effect can be formally defined as follows:
where
IV methods may be used to identify the LATE of Head Start participation on maternal outcomes under the assumptions that (1) treatment assignment, Z, is associated with the treatment obtained, A; (2) treatment assignment and each outcome of interest, Y, do not share any common causes; (3) treatment assignment does not affect these outcomes except through its influence on the treatment obtained, which is known as an exclusion restriction; and (4) treatment assignment affects the obtained treatment monotonically (Angrist et al. 1996; Imbens and Angrist 1994).
These assumptions are not all satisfied by design in the HSIS. Condition 1 can be empirically verified, and condition 2 is met because of randomization of treatment assignment, but conditions 3 and 4 are neither guaranteed nor verifiable. Nevertheless, the exclusion restriction is defensible because it is difficult to identify mechanisms other than the obtained treatment through which assignment might plausibly affect maternal outcomes. The monotonicity assumption is also reasonable, as it seems unlikely that some individuals would participate in the study with the intention to do exactly the opposite of what they are asked.
We therefore instrument A with Z and estimate the LATE using the method of two-stage least squares (2SLS), which is consistent under the assumptions outlined previously (Angrist and Pischke 2009). With this approach, A is first regressed on Z and C using a linear and additive model, which can be expressed as follows:
Then, in a second stage, the LATE is estimated from another linear model with the following form:
where
In the presence of program substitution, the LATE is a weighted average of subLATEs that capture the effects of using different types of childcare arrangements (Kline and Walters 2016). Specifically, under an additional assumption that (v) assignment of a Head Start offer does not induce mothers to switch between using alternative center care versus home care, the LATE can be reexpressed as follows:
where Yd denotes a mother’s potential outcome under childcare arrangement d, which includes Head Start (h), alternative center care (c), or home care (m), and where Dz denotes the childcare arrangement adopted under assignment to treatment z.
In this decomposition,
The weight in this decomposition,
We attempt to identify the subLATE hm using an IV approach that instruments for a mother’s childcare arrangement with Head Start assignment and interactions between treatment assignment and the baseline covariates, following Kline and Walters (2016). Specifically, we conduct 2SLS estimation, treating attendance at Head Start and enrollment in an alternative care center as separate endogenous variables and using both an indicator for Head Start assignment and interactions between this indicator, family covariates, and characteristics of the center to which a mother initially applied for admission as instruments. We expect covariate interactions with treatment assignment to generate independent variation in childcare arrangements because, for example, an admission offer at a higher quality and more easily accessible Head Start center is more appealing and therefore more likely to induce mothers to select out of home or alternative center care and into Head Start. If these and the other conditions motivating IV estimation with excluded interactions are satisfied (Kline and Walters 2016; Reardon and Raudenbush 2013), then 2SLS estimates are also consistent for the subLATE hm .
To investigate effect heterogeneity across potentially compounding forms of disadvantage, we stratify the analyses outlined previously by maternal race and household income. Specifically, to examine racial heterogeneity, we perform separate analyses among Black, White, and Hispanic mothers. And to examine heterogeneity by baseline income, we separately examine mothers above versus below the sample median, which distinguishes between families closer to the poverty line and those far below it. In a set of ancillary analyses, we also considered heterogeneity by alternative income quantiles, baseline economic hardship, marital status, the presence of other young children in the household, and whether the participating child was part of the three- or four-year-old cohort. Results from these analyses gave no indication that the effects of Head Start differ across levels of these covariates.
Finally, to account for the possibility that the effects of program participation depend on treatment intensity, we repeat our analysis of the LATE, as described previously, but now limiting the estimation sample to mothers who initially applied for admission to a Head Start center that provided full-time care. In addition, we also estimate a version of the LATE that substitutes our indicator for treatment receipt with our measure for the number of hours spent per week in Head Start, which we instrument with Head Start assignment and interactions between assignment and the baseline covariates. This allows us to evaluate whether the effects of Head Start participation depend on the amount of time a mother was able to use the program.
We adjust for the bias and inefficiency that may result from missing data by simulating missing values for all variables via multiple imputation with 20 replications, and then we combine results following Rubin (1987). The proportion of missing information in this analysis is about 0.03, which is due to a combination of panel attrition and item-specific nonresponse. We use heteroscedasticity-consistent standard errors to conduct Wald tests of the null hypothesis that a focal estimand is equal to zero, and p values from these tests are interpreted as a single number summary of evidence against this possibility. We computed a set of unweighted estimates and another set of estimates that use inverse probability weights to account for the HSIS complex sample design. Because both sets of point estimates were substantively similar, we focus on the unweighted results because of their greater relative efficiency (Solon, Haider, and Woolridge 2015). All code used for this analysis is available at https://github.com/cthyeh/headstart_mothers, where we also provide instructions for accessing data from the HSIS.
Results
Table 1 presents sample characteristics from the HSIS. The first two columns of the table describe the sample separately by treatment assignment. As expected under randomization, these results show few differences between the treatment and control groups in the HSIS, indicating they are closely balanced on observed covariates. Overall, both groups are composed of mothers that are relatively disadvantaged: less than half are married, about 40 percent are teenage mothers, and their mean monthly income is only about $1,500 at baseline. The middle two columns of the table present sample characteristics separately by treatment receipt, that is, separately for mothers who enrolled their children in Head Start and those using another care arrangement. A comparison of these two groups also suggests that they differ very little on observed covariates, even though compliance with treatment assignment was imperfect in the HSIS. In the last two columns of the table, we partition mothers who did not use Head Start into those who used alternative center care and those who cared for their children at home. These two groups differ in nontrivial ways on the observed covariates, which indicates that selection into home versus alternative center care among the control group is nonrandom. For example, sample members caring for their children at home are 9 percentage points more likely to be teen mothers and 12 percentage points more likely to have less than a high school education. They are also less likely to identify as Black. Taken together, these results suggest that highly disadvantaged White and Hispanic mothers may disproportionately select into home care when their children are not admitted to Head Start.
Sample Characteristics by Treatment Assignment and Childcare Arrangement.

Note: CES-D = Center for Epidemiological Studies Depression Scale.
Overall Effects of Head Start on Mothers
Table 2 presents estimates for the overall effects of Head Start on maternal outcomes. The upper panel of the table provides estimates for the ITT of receiving a Head Start offer. Contrary to expectations, ITT estimates provide little evidence of significant impacts on maternal outcomes, as all point estimates are close to zero and their p values do not provide any indication that the data are inconsistent with the null hypothesis of no effect. In other words, it does not appear that offering access to Head Start would appreciably increase employment, reduce economic hardship, or improve mental health among low-income mothers, on average.
Estimated Effects of Head Start on Maternal Outcomes among the Head Start Impact Study Total Sample.

Note: The p values are from two-sided Wald tests of the null hypothesis that the focal effect is equal to zero. CES-D = Center for Epidemiological Studies Depression Scale; ITT = intent-to-treat effect; LATE = local average treatment effect.
The middle panel of the table presents 2SLS estimates for the LATE of sending a child to Head Start, rather than using any other care arrangement, among the subpopulation of mothers who comply with their treatment assignment. Although not shown in the table, an F test on treatment assignment in the first stage confirms that receipt of a Head Start offer is very strongly related to Head Start enrollment (F = 3,042.54, p < .001). Nevertheless, these results also provide little evidence of nontrivial effects for Head Start participation on maternal outcomes. As with the ITTs, point estimates for the LATE on maternal employment, economic hardship, and depression are all substantively small and fail to approach conventional significance thresholds.
The lower panel of Table 2 presents 2SLS estimates for the subLATE hm , which captures the effect of sending a child to Head Start, rather than caring for them at home, among mothers who are induced out of home care and into Head Start by an offer of admission to the program. Point estimates for the subLATE hm on employment are similar to those discussed previously and larger for the other outcomes, but they are also highly imprecise and thus still provide little evidence against the null hypothesis of no effect. For example, they suggest that sending a child to Head Start, rather than caring for them at home, increases the probability of full-time employment by 2.8 percentage points, but this estimate does not approach conventional thresholds for statistical significance. With a partial F statistic of 194.06 (p < .001) on treatment assignment and its interactions with covariates in the first stage, these findings do not appear to be seriously afflicted by problems related to weak instruments, but they suffer from considerable sampling variability nonetheless. In general, all subLATE hm estimates in this analysis are imprecise, indicating a high degree of uncertainty and instability, and thus must be interpreted cautiously.
In summary, the HSIS yields little evidence that Head Start increases employment, reduces economic hardship, or improves mental health among the population of eligible mothers, even after adjusting for noncompliance and program substitution.
Effects of Head Start by Race
The overall effects of Head Start on maternal outcomes may obscure heterogeneity across different racial groups. Table 3 presents estimates for the ITT, LATE, and subLATE hm separately for Black, White, and Hispanic mothers. Among Whites and Hispanics, the HSIS again provides little evidence that Head Start improves maternal outcomes, although some of these estimates suffer from considerable sampling variability and are consistent with a wide range of possible effects.
Estimated Effects of Head Start on Maternal Outcomes by Race.

Note: The p values are from two-sided Wald tests of the null hypothesis that the focal effect is equal to zero. CES-D = Center for Epidemiological Studies Depression Scale; ITT = intent-to-treat effect; LATE = local average treatment effect.
Among Blacks, however, the HSIS provides evidence that access to and enrollment in Head Start leads to meaningful improvements in employment and mental health. For example, estimates of the ITT indicate that providing access to Head Start reduces depression by nearly one fifth of a standard deviation on the CES-D, while estimates for the LATE and subLATE hm are even larger. To put the size of these effects in perspective, note that CES-D scores are about one sixth of a standard deviation lower among sample members with at least some college compared with those with only a high school diploma or General Educational Development, net of other factors.
Similarly, estimates for the ITT suggest that offering access to Head Start may increase the probability of full-time employment among Black mothers by about 7 percentage points, while estimates for the LATE and subLATE hm suggest that program participation may increase full-time employment by between 10 and 20 percentage points among Black mothers whose childcare choices respond to treatment assignment. The p values for these estimates range from .01 to .05, indicating that the data are at least somewhat inconsistent with the null hypothesis of no effect. As a comparison, sample members with at least some college are about 5 percentage points more likely than those with only a high school education to be employed full-time, net of other controls.
The HSIS therefore provides evidence that Head Start may lead to considerable improvements for Black mothers in particular. Results for other racial groups are generally consistent with those from the total sample, which suggest that access to the Head Start program may not, by itself, improve maternal outcomes. Although the subLATE hm estimates suggest that Head Start participation may actually increase economic hardship among White mothers, these results are highly imprecise and must be interpreted cautiously.
Effects of Head Start by Household Income
Table 4 presents effect estimates separately for mothers with baseline incomes above versus below the sample median. With few exceptions, estimates of the ITT and LATE for both groups of mothers are all close to zero and provide little evidence that access to or enrollment in Head Start affects maternal outcomes. Point estimates for the subLATE hm are larger in absolute terms but too imprecise to draw any meaningful inferences among mothers with different incomes at baseline. Thus, data from the HSIS provide no clear indication that mothers with especially low incomes see more pronounced improvements from Head Start participation, contrary to expectations.
Estimated Effects of Head Start on Maternal Outcomes by Household Income.

Note: The p values are from two-sided Wald tests of the null hypothesis that the focal effect is equal to zero. CES-D = Center for Epidemiological Studies Depression Scale; ITT = intent-to-treat effect; LATE = local average treatment effect.
Effects of Head Start by Treatment Intensity
Table 5 presents estimates for the effects of Head Start participation, accounting for differences in treatment intensity. The first columns of the table present estimates for the effects of participating in the program 35 hours per week, rather than not participating at all, separately for the total sample and then among each of the subpopulations for which we anticipated larger program impacts. The second set of columns present estimates for the effects of Head Start participation among mothers that initially applied for admission at a center with full-time hours. In general, these estimates closely align with those discussed previously. Even after accounting for treatment intensity, there is little evidence of program impacts among the total sample, Hispanics, or mothers with below-median incomes. Among Black mothers, by contrast, participation in Head Start on a full-time basis appears to generate substantial increases in employment and substantial decreases in economic hardship and depression.
Estimated Effects of Head Start on Maternal Outcomes Accounting for Treatment Intensity.

Note: The p values are from two-sided Wald tests of the null hypothesis that the focal effect is equal to zero. CES-D = Center for Epidemiological Studies Depression Scale; LATE = local average treatment effect.
Discussion
Although research on the effects of Head Start has focused mainly on children, we hypothesized that these programs may also affect parents, and especially low-income mothers, because the provision of affordable childcare and related services is widely thought to increase employment, reduce economic hardship, and improve mental health for caregivers living in poverty. With experimental data from the HSIS, we found that participation in Head Start generates nontrivial improvements in employment and mental health among Black mothers. There was little evidence, however, of program impacts among other groups of mothers. Because some Head Start centers operate only part-time and roughly one third of the HSIS control group sought out alternative forms of subsidized childcare, we also attempted to estimate treatment effects after accounting for program substitution and differences in treatment intensity. Results from these analyses provided suggestive evidence that Head Start leads to larger improvements in maternal outcomes specifically among Black mothers who would otherwise look after their children at home and when they could attend the program full-time.
Why might Head Start lead to larger improvements among Black mothers? We speculate that the answer may lie in the individual preferences and structural constraints that uniquely characterize this subpopulation. Historically, Black women had high rates of labor force participation, and although this pattern has faded in recent decades, there remains a strong “culture of work” among them (Boustan and Collins 2014). At the same time, however, Blacks are often perceived by employers as the least desirable job candidates (Browne and Misra 2003; Pager, Western, and Bonikowski 2009), and Black women with childcare responsibilities may face especially severe discrimination in the labor market. Black mothers also report that they prefer center care to other childcare arrangements (Fuller, Holloway, and Liang 1996), as their access to family support for child-rearing may be comparatively limited (Brewster and Padavic 2002). Thus, relative to other disadvantaged groups, Head Start may engender larger effects among Black mothers, who want to work and prefer center-based care, by attenuating structural barriers and allowing them to realize these preferences.
The results outlined previously are partly consistent with our theoretical arguments that Head Start participation may improve the well-being of low-income mothers and that the most disadvantaged families are aided by this program more than others. Nevertheless, the weight of the evidence supporting these arguments is not overwhelming in the HSIS, and considerable uncertainty remains about whether expanding access to Head Start would, by itself, generate significant improvements in the lives of many low-income mothers who participate in the program. This population is often confronted with multiple, complex threats to their financial, familial, and emotional stability, including not only a lack of affordable childcare but also eviction, incarceration, intimate partner violence, physical health problems, and indiscriminate layoffs, among other challenges (Desmond and Western 2018; Edin and Lein 1997; Edin and Shaefer 2015). In this situation, interventions like Head Start may not be sufficiently powerful to attenuate the multidimensional hardships associated with maternal poverty, and significantly improving the lives of low-income mothers may require a combination of more robust welfare state policies (Bailey and Danziger 2013; Shaefer and Edin 2013).
Relatedly, our findings may also reflect certain limitations of Head Start as a form of subsidized childcare for low-income parents. Because Head Start only provides care relatively late in the course of early childhood, when children are already at least three years old, it does not support parents during the first several years of child-rearing, which can be among the most difficult for balancing family and work obligations.
Some Head Start centers also provide care only for half days or only for part of the year. The limited intensity of these services may not allow mothers to enter the paid workforce or otherwise increase their labor supply, thereby constraining the degree to which Head Start may help improve their financial position or reduce stressors in turn. Alternative interventions offering long-term, consistent, or flexible access to childcare and other support services may therefore have more pronounced effects for low-income mothers.
The results of this study must be interpreted cautiously, however, because of several shortcomings. The first is that the HSIS lacks data on other maternal outcomes that may be more sensitive to the type of childcare, education, and other services provided by Head Start, such as subjective well-being, anxiety, or network connections to other parents and community members. Access to Head Start may, in fact, lead to broad improvements in many maternal outcomes, just not the ones measured as part of the HSIS. A second limitation is that the HSIS was conducted nearly two decades ago, while Head Start services, the low-wage job sector, and antipoverty policies have all evolved over time, which suggests that our results are historically contingent. A third limitation is our inability to further parse the impacts of the many different care arrangements used by low-income mothers, because of the relatively small number of sample members in some of these settings and the difficultly of credibly identifying their effects. Finally, the relatively short duration of service provision in the HSIS may not be sufficient to appreciably improve maternal outcomes like economic hardship and unemployment, which often stem from persistent and seemingly unyielding structural forces in poor communities. Indeed, another set of ancillary analyses suggests that the Head Start impacts we documented while children were actively enrolled in the program largely fade away later on, after they have aged out of eligibility and their mothers can no longer use these services directly.
Its limitations notwithstanding, this study provides at least some evidence that Head Start can play a role in temporarily alleviating economic and mental health burdens among low-income mothers. Future research should investigate whether more consistent or long-term access to Head Start (e.g., through Early Head Start) yields larger improvements on a more comprehensive set of outcomes. It should also examine the effects of coupling Head Start with additional interventions that are more directly aimed at alleviating the hardships associated with maternal poverty, as identifying the precise conditions under which social programs improve maternal outcomes is essential for promoting upward mobility among low-income families and their children. The weight of the evidence from our analysis indicates that Head Start, by itself, can help certain groups of low-income mothers, but these improvements are also likely heterogeneous, dose-dependent, and may be rather small for some women.
Supplemental Material
sj-docx-1-srd-10.1177_23780231231192392 – Supplemental material for The Effects of Head Start on Low-Income Mothers
Supplemental material, sj-docx-1-srd-10.1177_23780231231192392 for The Effects of Head Start on Low-Income Mothers by Catherine T. H. Yeh and Geoffrey T. Wodtke in Socius
Footnotes
Acknowledgements
We would like to thank Fedor Dokshin as well as members of the Toronto Inequality Workshop.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.