Abstract
Introduction
Newly graduated nurses (NGNs) encounter difficulties in their professional development and experience high stress during the transition into practice, which may contribute to early turnover. Providing structured transition support is essential for navigating the complexities of patient care and alleviating stress.
Objective
To explore whether participation in a professional development programme (ProDeveloP) with a reflective component during the initial months of transition into practice is associated with NGNs’ perceived stress and professional development in terms of role clarity, task mastery, and social acceptance.
Methods
A quantitative intervention study with a non-randomised design. The study was conducted in a region in mid-Sweden. A total of 66 NGNs participated in the study: a control group (n = 27) in 2022 and an intervention group (n = 39) in 2023. The intervention group comprised NGNs who participated in a ProDeveloP, which builds upon a previous introduction programme consisting of eight educational days. ProDeveloP introduced four additional focus areas – role clarity, task mastery, social acceptance, and recovery – and incorporated structured reflection through six facilitated dialogue group sessions. Data were collected through surveys and analysed statistically.
Results
The intervention group, comprising NGNs who participated in ProDeveloP, had significantly lower perceived stress compared with the control group (Mann–Whitney U = 241.000, z = –3.311, p < .001), with a large effect size (Hedges’ g = .956, 95% CI [0.489, 1.575]). This difference remained statistically significant after adjusting for relevant covariates in a linear regression model. No significant differences were observed between the groups in relation to role clarity, task mastery, or social acceptance.
Conclusion
Transition support employing a reflective approach, such as ProDeveloP, may lower perceived stress among NGNs during the early transition and can be crucial for ensuring a positive transition experience.
Keywords
Introduction/Background
In Sweden, newly graduated nurses (NGNs) must have completed a three-year university education programme, which includes clinical training, to prepare them for practice. Graduating with a bachelor's degree brings considerable pressure and expectations to perform to a high standard. Previous research conducted on NGNs in Sweden indicates that they are not sufficiently supported in meeting professional responsibilities and demands (Willman et al., 2021). The phenomenon of NGNs leaving their initial workplace in Sweden is notable. In one region in mid-Sweden, 20% of NGNs left their first employment during the first year (Törnqvist, 2020). High attrition rates are also seen globally, exacerbating the ongoing challenge of a nursing shortage and jeopardising the future availability of healthcare resources (World Health Organisation [WHO], 2022). Retaining NGNs is crucial for a sustainable and high-quality, and patient-safe healthcare system globally. It is imperative for employers and governments to take urgent action to provide support for NGNs (Duchscher & Corneau, 2023). Providing transition support can counteract the high turnover rates (Miller et al., 2023; Reebals et al., 2022) and enhance patient safety (Murray et al., 2020). Therefore, it is essential to explore the support requirements of NGNs to facilitate their transition into professional practice. This will help enhance retention and ensure the sustainability of the future nursing workforce.
Review of Literature
Transitioning from student to NGN, while assuming responsibility for patient care in the dynamic and demanding hospital environment, is a complex process. This transition presents significant challenges and can be overwhelming (Reebals et al., 2022), with the initial period being emotionally and psychologically demanding (Duchscher, 2009). Heightened demands for safe performance in direct patient care can provoke anxiety due to fear of making errors that might harm patients (Kaldal et al., 2023; Murray et al., 2020). These challenges are often a source of considerable stress for NGNs (Duchscher, 2009; Labrague & McEnroe-Petitte, 2018; Murray et al., 2020). Nursing transition theory classifies NGNs’ first-year experience into three stages: “doing” (first 3–4 months), “being” (4–8 months), and “knowing” (8–12 months), representing a progressive process of professional development. The initial stage is characterised by intensive learning in a demanding work environment with limited support, where NGNs experience high stress and uncertainty in complex clinical scenarios (Duchscher, 2008).
During the transition period, NGNs require support to overcome challenges and alleviate their stress (Frögéli et al., 2022). Transition support can facilitate socialisation and professional development in key areas: understanding the demands of the professional role (role clarity), mastering required tasks (task mastery), integrating into the group (social acceptance), and managing stress (Ellis et al., 2015). Healthcare organisations commonly use organised introduction programmes to ensure NGNs receive adequate assistance during this transition (Reebals et al., 2022). These programmes often encompass a wide range of strategies, including team and mentorship support, peer support, and workplace environmental support (Rush et al., 2019). When introduction programmes include not only technical skills training but also soft skills development, addressing the ethical and emotional aspects of care, they have been shown to ease NGNs’ transition and support their professional development (Song & McCreary, 2020). Opportunities for reflection further enable NGNs to process experiences, integrate theoretical knowledge with practice, and develop comprehensive professional understanding (Berglund & Ekebergh, 2025), particularly when undertaken in collaboration with experienced RNs and peers (Lindblom et al., 2025).
Several studies confirm that introduction programmes can enhance NGNs’ professional development and reduce turnover rates (Miller et al., 2023; Rush et al., 2019). However, there remains a paucity of research evaluating the specific components of these programmes (Rush et al., 2019). Programmes often do not include clearly defined, evidence-based core components, particularly in relation to structured reflection and soft skills development. Moreover, few studies have examined how these components relate to outcomes such as perceived stress (Kenny et al., 2021).
To address these gaps and better support NGNs in their transition into practice, a professional development programme (ProDeveloP) was designed as an extension of a previous introduction programme consisting of traditional educational sessions. ProDeveloP introduced four new focus areas – role clarity, task mastery, social acceptance, and recovery – and incorporated structured reflection in dialogue groups to address ethical and emotional challenges. The aim of this study is to explore whether participation in a ProDeveloP with a reflective component during the initial months of transition into practice is associated with NGNs’ perceived stress and professional development in terms of role clarity, task mastery, and social acceptance.
Methods
Design
This was a quantitative intervention study with a non-randomised design (Polit & Beck, 2020), comprising an intervention group and a control group.
Research Questions
Were there differences in perceived stress, role clarity, task mastery, and social acceptance between NGNs who participated in ProDeveloP and those who attended the previous introduction programme?
Was there an association between participation in ProDeveloP and perceived stress among NGNs, controlling for relevant covariates and predictors?
Setting and Sample
The study was conducted at a principal regional hospital in mid-Sweden. Inclusion criteria were NGNs who were newly employed and participated either in a previous introduction programme in 2022 or in ProDeveloP in 2023. Specifically, all eligible NGNs employed in 2022 who participated in a previous introduction programme starting in September were included in the control group, while all eligible NGNs employed in 2023 who participated in ProDeveloP, starting either in February or September, were included in the intervention group. No specific exclusion criteria were applied. All NGNs held full-time permanent positions and worked shifts.
ProDeveloP
This study was part of a larger research project that investigated whether ProDeveloP, comprising four focus areas and structured reflection, could support NGNs during their transition. ProDeveloP and the research project are further described in a study protocol (Höglander et al., 2025). ProDeveloP was implemented in 2023 through a collaboration between a university and a regional education centre and was conducted in Swedish.
Before 2023, the introduction programme consisted of eight educational days delivered over the first four months. These sessions included joint lectures on topics such as communication, work and health, leadership, patient safety, dementia, discharge processes, palliative care, pain management, pharmacological management, acid–base balance, trauma, and pre-hospital care. The programme also incorporated simulation exercises for acute and trauma situations, as well as skills training in various clinical procedures. ProDeveloP was developed based on the previous introduction programme and existing research. It included additional components such as four focus areas—role clarity, task mastery, social acceptance, and recovery—and integrated structured reflection facilitated through dialogue groups, addressing ethical and emotional challenges.
ProDeveloP consistently addressed four focus areas throughout its duration: role clarity, task mastery, social acceptance (Bauer et al., 2007; Gustavsson et al., 2020), and recovery (Frögéli et al., 2022). These focus areas were selected based on their proven impact on both immediate adaptation and long-term professional sustainability. Lecturers, teachers, facilitators, and NGNs received guidance on how to integrate these focus areas into learning and practice. To support continuous reflection, specifically designed reflection cards were used. These cards included reflection prompts such as reflecting with colleagues on the experience of being new in the professional role, seeking feedback, considering expectations and responsibilities associated with being a nurse, and exploring strategies to support recovery.
Dialogue groups have been identified as a pivotal component for facilitating professional development (Bergman et al., 2009). Six dialogue group sessions, each lasting two hours, were conducted with peers and trained facilitators over the first 10 months. The sessions were facilitated by experienced RNs who had completed a three-day training programme focused on structured group reflection. All facilitators had at least 3 years of professional experience. Facilitator manuals, inspired by Kolb's experiential learning model (Kolb, 2014), were designed to promote a safe and trustworthy learning environment in which NGNs felt encouraged to share their experiences, thoughts, and emotions. Each session began with a ‘check-in’ to acknowledge participants’ current emotional state and concluded with a ‘check-out’ to reflect on professional support and whether any emotional burdens had been released. All participants were invited to actively contribute by sharing experiences and offering mutual support. Regular opportunities for structured reflection on clinical experiences were also incorporated into the educational days. All new components introduced in ProDeveloP were designed to lower stress, support the socialisation process, and facilitate professional development. An overview of ProDeveloP, highlighting the new components compared with the previous introduction programme, is presented in Table 1. Attendance among NGNs during the educational days and the first three dialogue group sessions ranged from 90% to 100%, with full facilitator participation.
Overview of ProDeveloP.

New components compared with a previous introduction programme.
Outcome Measures
Perceived stress (primary outcome) and role clarity, task mastery, and social acceptance (secondary outcomes) were measured using 5-point Likert scales in Swedish, based on instruments previously validated in the Swedish context (Frögéli et al., 2019; Frögéli et al., 2020). Details of the specific items for each variable are summarised in Table 2. In the present study, Cronbach's α was calculated to assess the internal consistency of the scales, resulting in α = .806 for role clarity, α = .732 for task mastery, α = .790 for social acceptance, and α = .885 for stress.
Elements Affecting the Practice of NGNs with Survey Item Examples.

Data Collection
Digital surveys in Swedish, distributed via Survey and Report (Artlogic, 2022), were used to collect data on the programme's final educational day. The study's first arm (i.e., the control group) consisted of all eligible NGNs (n = 39) who participated in the previous introduction programme that started in September 2022. The survey, which included demographic questions, was administered in late November. A total of 27 NGNs in the control group agreed to participate and answered the survey. The second arm (i.e., the intervention group) consisted of all eligible NGNs (n = 62) who participated in ProDeveloP starting either in February or in September 2023, depending on their graduation date. The survey was distributed in early May or December, aligning with the same time frame as the control group. However, the participants in the intervention group had already completed a presurvey containing demographic questions before starting ProDeveloP. A total of 39 NGNs from the intervention group participated in this study survey.
Data Analysis
The SPSS Statistics version 29 (IBM Corp, 2024) was used for the analyses. The analyses were conducted by the first and last authors, with support from experienced researchers in statistical analysis and statisticians, who verified the accuracy of both the analytical procedures and the results. A visual inspection of the data indicated minor deviations from normality. Results from the Shapiro–Wilk test confirmed that the variables included in the study were not normally distributed. Consequently, non-parametric statistical tests were selected. For the scales used in this study, scores ranged from 0 to 8 for task mastery and social acceptance, and from 0 to 12 for stress and role clarity. These ranges reflected the number of items per scale and the scoring system applied, where each response option was scored from 0 to 4.
A Mann–Whitney U test was used to compare the mean scores of the study variables (stress, role clarity, task mastery, and social acceptance) to determine differences between the control and intervention groups. A two-sided significance level of p = .01 was applied, based on a Bonferroni correction to control the family-wise error rate (FWER) across four comparisons, adjusting the conventional threshold of p = .05 by dividing it by the number of tests (p = .05/4). To complement significance testing, effect sizes were calculated using Hedges’ g, which adjusts for small and unequal sample sizes.
To further examine differences in perceived stress between the control and intervention groups, a linear regression analysis with bootstrapping was conducted. The model included covariates that were both theoretically and empirically supported (role clarity, task mastery, and social acceptance) as well as demographic factors associated with stress, such as prior clinical experience before participation in either the previous introduction programme or ProDeveloP (previous clinical education at the workplace and number of weeks worked before programme participation).
Ethical Considerations
Ethical approval for the study was obtained from the Swedish Ethical Review Board (Dnr 2022-05682-01) and adhered to throughout the research process. The NGNs received both oral and written information about the study, in accordance with the ethical principles outlined in the World Medical Association's Declaration of Helsinki (World Medical Association, 2024). Written informed consent was obtained from all participants before they participated in the study. A data management plan was implemented to ensure proper handling and secure storage of all data, in compliance with university policy and followed the European Union's General Data Protection Regulation (GDPR 2016/679, 2016). The surveys in the Survey and Report were securely transferred using digital transfer. All data were anonymised through coded identifiers, and participants were assured of full confidentiality.
Results
Sample Characteristics
The demographic characteristics of participants in both the control and intervention groups are presented in Table 3. While the groups showed overall similarities, a notable difference was observed in the number of weeks worked before the introduction programme.
Demographic Characteristics of the Participants.
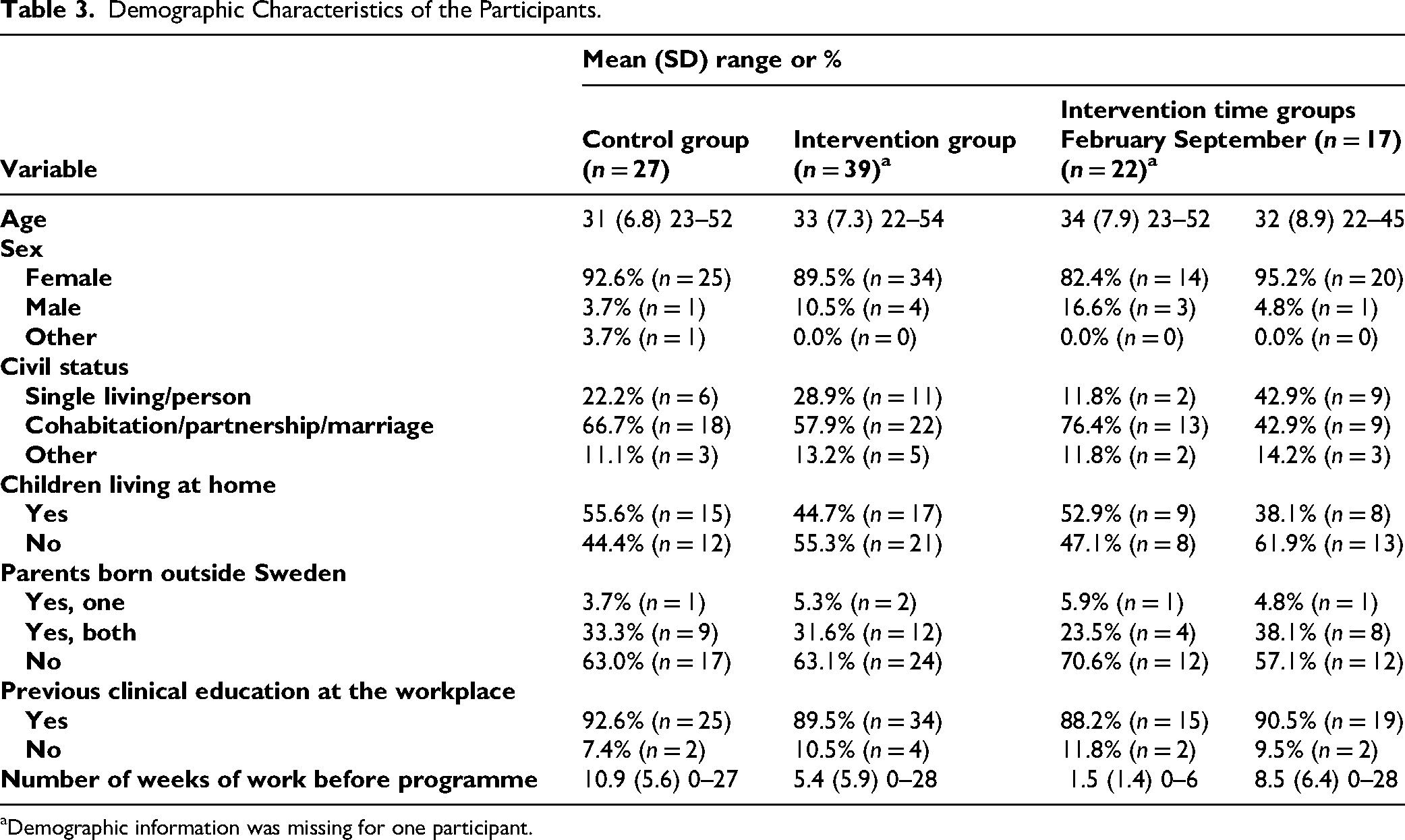
Demographic information was missing for one participant.
Missing Data
Demographic information was missing for one participant, and one item related to social acceptance was not completed by another participant; both participants were in the intervention group. Participants with missing data were excluded from analyses involving those variables by the statistical software.
Differences in Perceived Stress, Role Clarity, Task Mastery, and Social Acceptance Between Intervention and Control Groups
The results showed that the intervention group perceived lower stress in week 13 compared to the control group. A Mann–Whitney U test indicated a significant difference in perceived stress between the intervention and control groups (U = 241.000, z = –3.311, p < .001). The control group reported higher median stress scores (Md = 7) compared with the intervention group (Md = 5). The effect size was large (Hedges’ g = .956, 95% CI [0.489, 1.575]). No significant differences were observed regarding role clarity, task mastery, and social acceptance (Table 4).
Non-Parametric Group Comparisons for Stress, Role Clarity, Task Mastery, and Social Acceptance.

Adjusted Association Between Participation in ProDeveloP and Perceived Stress
The model included covariates such as role clarity, task mastery, and social acceptance, as well as demographic factors associated with stress, including previous clinical education at the workplace and the number of weeks worked before participation in either the previous introduction programme or ProDeveloP. After adjustment, the regression coefficient was 1.736 (95% CI [0.513, 2.960], p = .005), indicating that the control group reported significantly higher average stress compared with the intervention group. In the unadjusted model, the regression coefficient was 2.927 (95% CI [1.588, 4.266], p < .001), suggesting an even greater difference before controlling for covariates.
Discussion
The aim of this study was to explore whether participation in a ProDeveloP with a reflective component during the initial months of transition into practice is associated with NGNs’ perceived stress and professional development in terms of role clarity, task mastery, and social acceptance. The findings suggest that ProDeveloP may lower stress among NGNs during their transition into practice. ProDeveloP was developed as an enhancement of a previous introduction programme, incorporating new components informed by prior research. Initial group comparisons revealed significant differences in perceived stress between the intervention and control groups, with a more favourable outcome among participants in ProDeveloP. Furthermore, linear regression analyses demonstrated that participation in ProDeveloP remained significantly associated with reduced perceived stress after adjusting for relevant covariates. This strengthens the interpretation that the observed benefits are not solely attributable to background differences between groups but may reflect an association with the programme itself.
These findings align with theoretical perspectives suggesting that NGNs require support due to demands, challenges, and intense development they experience during the initial “doing” phase of transition, which can lead to stress (Duchscher, 2008). This underscores the importance of providing NGNs with access to programmes such as ProDeveloP during their transition into professional practice. These insights can inform managers about NGNs’ need for support, reinforcing the value of structured transition programmes (Duchscher & Corneau, 2023; Murray et al., 2019).
The new components in ProDeveloP encompassed a reflective approach and four focus areas of role clarity, task mastery, social acceptance, and recovery. These elements were integrated into regular dialogue groups with peers and experienced RNs, alongside opportunities for reflection during educational days with senior staff. This finding suggests a potential mechanism through which the intervention may be associated with lower perceived stress among participants in the intervention group. Previous research has indicated that structured intervention within an introduction programme targeting role clarity, task mastery, and social acceptance can prevent stress by promoting new health behaviours and recovery (Rudman et al., 2024) and reduce the risk of early burnout (Frögéli et al., 2022). This highlights the value of including these focus areas in a programme. Moreover, previous research suggests that reflecting on experiences from patient care with peers and experienced colleagues in a programme can enhance NGNs’ confidence, help them manage uncertainty, and promote a more comprehensive understanding of how to navigate the complexities of care (Ekebergh et al., 2018; Rush et al., 2019). Such collaborative approaches can also provide emotional support (Lindblom et al., 2025) during this emotionally demanding period (Duchscher, 2009; Reebals et al., 2022).
Despite promising findings regarding lower stress, ProDeveloP showed no significant association with role clarity, task mastery, or social acceptance between the control and intervention groups. However, in a previous study, NGNs described that the reflection opportunities supported them in developing their professional role by enabling them to process caring experiences together with peers and experienced RNs who understood their situation (Lindblom et al., 2025). This affirms NGNs’ need for support from an experienced RN due to the complex professional reality that they face (Benner, 2004; Jangland et al., 2021) and for developing an understanding of the professional role in practice and ensuring patient safety (Kaldal et al., 2023; Murray et al., 2020). However, in clinical settings, opportunities for reflection are often limited, and a shortage of RNs persists (Widarsson et al., 2020). Programmes such as ProDeveloP can help ensure that necessary support is provided to participants through an organised and structured programme, in which experienced nurses are available.
Additional factors not included in this study should be considered when addressing stress and providing support for NGNs during their transition. For instance, previous research highlights that an unfavourable work environment or working conditions featuring a high workload and lack of resources may impede transition support and the effective integration of NGNs (Willman et al., 2021), which in turn may affect their perceived stress.
Overall, an enhanced socialisation process, professional development, and reduced stress may contribute to lowering turnover intentions (Ellis et al., 2015; Frögéli et al., 2022), which can contribute to decreased attrition rates (Rae et al., 2025; Reebals et al., 2022) and offer cost-effective benefits by reducing the need for new hires (Rush et al., 2019). Retaining NGNs is essential given the global ongoing nursing shortage, which threatens the sustainability of future healthcare resources (WHO, 2022). Therefore, transition support should be regarded as essential for facilitating NGNs’ professional development and ensuring the utilisation of resources.
Strengths and Limitations
One limitation of this study is the small sample size, which may have reduced statistical power and limited the generalisability of the findings. Although the study included both an intervention and a control group, baseline measurements could not be collected at the outset, restricting the ability to assess within-group changes over time. Consequently, it was not feasible to implement a randomised controlled trial. The number of eligible NGNs was constrained by the actual participation in ProDeveloP in 2023 and a previous introduction programme in 2022 at a regional hospital. While the findings provide valuable insights, they should be interpreted with caution. Future studies with larger, more diverse samples and randomised designs are needed to strengthen the evidence base and confirm the observed findings.
Despite similarities in context and demographic data of the control group and the intervention group, differences were observed in the number of weeks worked before participation, primarily due to the programme's start time and differences in graduation dates. The control group had worked for more weeks before participating in the previous introduction programme, which began in September following the summer vacation, whereas NGNs usually start work in June, immediately after graduation. The NGNs in the intervention group in February 2023 had just graduated, and the NGNs in September 2023 had the same conditions as the control group. A few individuals in each group graduated between the semesters, which explained the wider range of weeks of work before participation in the programme. Based on theoretical perspectives, clinical experience, and time in the profession may influence perceived stress among NGNs (Benner, 2004; Duchscher, 2008). To account for this, weeks worked and previous clinical education before the programme were included as covariates in the linear regression analysis to control for potential confounding effects.
Another limitation relates to the timing of data collection across the control and intervention groups. The control group participated in autumn 2022, while the intervention groups participated in spring or autumn 2023. Seasonal variation and contextual factors may have influenced participants’ experience of stress differently depending on when the data were collected. These differences could not be fully accounted for in the analysis and should therefore be considered a potential source of confounding when interpreting the results.
Despite these limitations, this study contributes to a field where evaluations of structured introduction programmes for NGNs – programmes with clearly described, evidence-based components, including a reflective approach – and their association to outcomes such as stress remain relatively scarce (Kenny et al., 2021).
Another limitation concerns the use of shortened scales with a limited number of items, which may have restricted content coverage and posed a risk to the validity of between-group comparisons. However, the scales and items were selected based on prior validation in earlier studies (Frögéli et al., 2019; Frögéli et al., 2020), and all demonstrated acceptable internal consistency in the present study, with Cronbach's alpha values exceeding .70.
Implications for Practice
These findings suggest that structured and organised introduction programmes such as ProDeveloP, incorporating components based on previous research and addressing focus areas alongside a reflective approach in educational days and dialogue groups, may play an important role in supporting NGNs during their transition into professional practice. Future research employing randomised controlled designs with larger samples and longitudinal follow-up is warranted to confirm and extend these findings. In addition, a deeper exploration of NGNs’ stress and recovery, as well as specific aspects of group interaction, such as trust building and shared reflection, is critical for understanding the mechanisms behind the observed associations. Furthermore, examining the role of transition support in the workplace and what occurs after the first year of structured support ends could be an important direction for future studies. A clearer understanding of these mechanisms will be key to refining and tailoring interventions for NGNs and comparable professional groups within healthcare.
Conclusion
This study demonstrates that ProDeveloP lowers NGNs’ perceived stress during the initial stages of their professional development. Although the lack of randomisation and modest sample size are limitations, the inclusion of a control group and the finding of significantly lower perceived stress among NGNs in the intervention group are noteworthy. These results suggest that structured introduction programmes incorporating reflective components may help alleviate stress among NGNs, although further research with larger samples and randomised designs is needed to confirm these findings.
Supplemental Material
sj-docx-1-son-10.1177_23779608261421265 - Supplemental material for Associations Between Participation in ProDeveloP and Newly Graduated Nurses’ Stress and Professional Development When Transitioning into Practice
Supplemental material, sj-docx-1-son-10.1177_23779608261421265 for Associations Between Participation in ProDeveloP and Newly Graduated Nurses’ Stress and Professional Development When Transitioning into Practice by Magdalena Lindblom, Margareta Widarsson, Marie-Louise Södersved Källestedt, Anna Letterstål, Kent W Nilsson, Margareta Asp and Jessica Höglander in SAGE Open Nursing
Footnotes
List of Abbreviations
Acknowledgments
We would like to express our gratitude to all who participated in this study, especially the newly graduated nurses, who were invaluable to this research.
Ethical Approval and Informed Consent
Ethical approval for the study was obtained from the Swedish Ethical Review Board (Dnr. 2022-05682-01). Written informed consent was obtained from all participants involved in the study.
Authorship Contributions
Conceptualisation and methodology: ML, MW, MLSK, AL, KN, MA, and JH. Investigation: ML. Formal analysis: ML, KN, and JH. Writing–original draft: ML. Writing–review and editing: ML, MW, MLSK, AL, KN, MA, and JH. Funding acquisition: MA.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by AFA Insurance (grant number: 220065). The funder has not been involved in the study design, data collection, analysis, or interpretation of data, nor in the writing of the report or the decision to submit the article for publication.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Clinical Trial Registration
ProDeveloP was registered in ClinicalTrials.gov [clinical trial number, NCT06742047].
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
