Abstract
Introduction
The current healthcare environment is very complex; thus, a healthy work environment is needed to ensure nurses’ job satisfaction and retention. Also, improving nurses’ self-efficacy became a mandate in light of the increased stressful demands of the nursing profession; therefore, implementing an effective leadership style, such as authentic leadership, has become essential because of its positive influence on various nursing outcomes. Thus, this study investigated the impact of the perceived nursing leaders’ authentic leadership on the perceived hospital nurses’ general self-efficacy, job satisfaction, and intent to stay at work.
Methods
A quantitative cross-sectional design was used, and a non-random convenience sample of 295 nurses who were working at the hospitals was recruited. The study period extended from the 1st of September to the 6th of October 2022.
Results
Hospital nurses perceived that their leaders had a moderate level of authentic leadership. The nurses perceived themselves as having sufficient general self-efficacy. They were moderately satisfied with a moderate level of intent to stay at work. Furthermore, nurses who perceived their leaders as authentic leaders had higher general self-efficacy, were more satisfied and had higher intent to stay at work than nurses who perceived their managers as non-authentic. Moreover, nurses who perceived a high sense of general self-efficacy intended to stay longer at work than their counterparts (r = .335, P < .01), and those who were satisfied at work reported higher general self-efficacy and intended to stay longer at work than less satisfied nurses. In addition, there were significant differences in the perceived nursing leaders’ authentic leadership based on educational level, shift type, and the type of hospital.
Conclusion
Higher levels of self-efficacy, job satisfaction, and intent to stay at their work were all demonstrated by nurses who thought their leaders were authentic. This high level indicates that the way leaders lead significantly influences nurses’ workplace experiences and long-term commitment. Contextual differences in leadership perception highlight the need for tailored leadership development programs that address the unique challenges of various healthcare settings.
Introduction
The global healthcare system faces complex challenges, notably a severe nursing shortage (Bandeali & Maita, 2024). The WHO's 2020 SOWN report notes 27.9 million nurses worldwide, yet a deficit of 5.9 million remains, with 17% expected to retire within a decade (Bandeali & Maita, 2024). Alarmingly, 89% of this gap—around 5.3 million nurses—is concentrated in low- and lower-middle-income countries like Jordan, where workforce growth barely keeps pace with population increases (Bandeali & Maita, 2024). This high rate underscores the urgency of addressing workforce sustainability in healthcare (Yamamoto et al., 2024).
In Jordan, the situation is exacerbated by nurse migration in pursuit of better pay and working conditions (Pattali et al., 2024). The shortage threatens patient safety, increases mortality (Nydahl et al., 2024; Pattali et al., 2024), and compromises care quality (Leary et al., 2024), as widely documented (Bandeali & Maita, 2024; Nydahl et al., 2024; Pattali et al., 2024).
Nursing administrators must prioritize job satisfaction and retention (Zhu et al., 2023), with leadership playing a key role (AbdELhay et al., 2025; Koskinen et al., 2023). This study explores how perceived authentic leadership affects nurses’ general self-efficacy, job satisfaction, and intent to stay. Low self-efficacy correlates with reduced satisfaction (Kallerhult Hermansson et al., 2024) and retention (Alshaibani et al., 2024), especially among new nurses (Holter, 2022). These factors impact absenteeism, turnover, burnout, and overall care quality (AbuAlRub et al., 2023; Metwally et al., 2025; Stemmer et al., 2022).
Relational leadership styles like authentic leadership can enhance nurses’ experiences and retention (Almutairi et al., 2025; Labrague et al., 2025). Emphasizing ethics, transparency, and self-awareness, authentic leadership may offer practical solutions. Thus, this study examines its relationship with nurses’ self-efficacy, job satisfaction, and intent to stay, contributing to effective retention strategies.
Literature Review
A healthy work environment is essential for nurses’ job satisfaction, intent to stay, and retention (Pattali et al., 2024). Addressing workplace factors and enhancing general self-efficacy is critical due to the profession's high stress and emotional demands (Labrague et al., 2025; Mrayyan et al., 2023). Nurses with strong self-efficacy manage challenges effectively and uphold care standards (Magon et al., 2023). Leadership style plays a vital role, with authentic leadership—an emerging relational style—positively influencing nurses’ outcomes and work environments (Almutairi et al., 2025; Pattali et al., 2024). Although international studies have explored the relationship between authentic leadership and job satisfaction (e.g., Wong et al., 2020), this study is the first to examine this relationship in Jordan.
Authentic leadership fosters ethics, trust, and transparency (Almutairi et al., 2025), improving nurses’ well-being (Faroque et al., 2025), psychological health, job satisfaction, performance (Metwally et al., 2025), and work conditions (Al Sabei et al., 2023). Avolio's theory, commonly used to study authentic leadership, emphasizes self-awareness, transparency, balanced processing, and moral integrity (Avolio, 2024; Avolio & Gardner, 2005), though it lacks a nursing-specific context.
To address this, Giordano-Mulligan and Eckardt (2019) developed a nursing-specific framework defining authentic leadership and strategies to foster engagement and healthy environments. Concept analyses, such as Almutairi et al. (2025), identified key attributes (e.g., caring, ethical courage), antecedents (e.g., authenticity, leadership development), and outcomes (e.g., well-being, performance, safety). Maziero et al. (2020) also found that authentic leadership enhances engagement, satisfaction, retention, and commitment.
Self-efficacy—belief in one's ability to manage stress—is shaped by support systems and compensation (Al-Hamdan & Bani Issa, 2021), and is vital for resilience. Few studies have explored authentic leadership's impact on nurses’ self-efficacy, though Labrague et al. (2021) found moderate positive correlations in a study of 1,534 nurses in Oman.
Job satisfaction reflects nurses’ emotional connection to their work and affects performance (Metwally et al., 2025), well-being (Faroque et al., 2025; Labrague et al., 2025), and career planning. It is influenced by factors like work conditions, salary, leadership, and stress (Yasin et al., 2020). Relational leadership styles—authentic, servant, and transformational—positively impact satisfaction (Specchia et al., 2021).
Job satisfaction strongly influences intent to stay (Al Zamel et al., 2020), and leadership behaviors shape both. While international studies show a positive link between authentic leadership and job satisfaction (Labrague et al., 2025; Wong et al., 2020), this relationship remains unexplored in Jordan. Intent to stay, defined as nurses’ decision to remain in their roles, is influenced by satisfaction and environment (Al Zamel et al., 2020). Though direct studies are lacking, authentic leadership has been linked to reduced turnover intention (Alkarabsheh et al., 2022).
In summary, authentic leadership shows promise in improving nurses’ self-efficacy, job satisfaction, and retention, but further research is needed to clarify its application in specific contexts.
Theoretical Framework
The research expands upon Avolio's authentic leadership theory in conjunction with the nursing leader framework proposed by Giordano-Mulligan and Eckardt (2019). This integration lays a comprehensive foundation for understanding leadership within nursing environments. Both frameworks underscore essential attributes—self-awareness, relational transparency, balanced processing, and internalized moral perspectives (Avolio, 2024; Avolio & Gardner, 2005)—that influence nurse outcomes. 1, General Self-Efficacy: Authentic leaders cultivate psychological safety, allowing nurses to voice concerns and make assured decisions. 2, Job Satisfaction: Ethical decision-making and inclusive, balanced processing foster trust and fairness, aligning with nurses’ values. 3, Intent to Stay: Supportive leadership strengthens organizational commitment, thereby decreasing turnover. These results highlight how leadership theory plays out in actual healthcare environments.
Giordano-Mulligan and Eckardt's (2019) framework further categorizes these characteristics into personal integrity, transparency, and altruism. Elevated personal integrity and moral courage enhance self-efficacy, transparent communication improves job satisfaction, and a compassionate, altruistic approach motivates nurses to persist in their positions. Ultimately, both frameworks emphasize the vital importance of trust, ethics, and psychological safety in effective nursing leadership. Together, these frameworks reinforce the importance of authentic leadership in promoting nurses’ intent to stay at work and well-being.
Problem, Research Questions, and Significance
The healthcare environment is full of challenges that may influence nurses (Nydahl et al., 2024; Pattali et al., 2024). These challenges highlight the importance of leadership strategies that help nurses manage the complexities of their work environment. Thus, general self-efficacy, job satisfaction, and intent to stay at work are essential issues that nurse administrators should consider. As nursing leaders deal with followers from different generations, more attention is paid to their followers through a modern leadership style, such as authentic leadership (Labrague et al., 2025; Mrayyan et al., 2023). This shift in leadership priorities highlights the changing needs of a diverse nursing workforce.
Nursing leaders’ authentic leadership is a relatively new leadership style that is needed in the currently changing and complex healthcare environment. An opportunity exists for continued research regarding the associations between such leadership and staff outcomes (Raso et al., 2020). To address this gap, the present study explored key relationships and variables by answering the following research questions: (a) What are the levels of nursing leaders’ authentic leadership, nurses’ general self-efficacy, job satisfaction, and intent to stay in Jordan? (b) What are the relationships between the perceived nursing leaders’ authentic leadership, nurses’ general self-efficacy, job satisfaction, and intent to stay? (c) What are the differences in the levels of the perceived nursing leaders’ authentic leadership based on the background variables of the sample? These questions provide a comprehensive understanding of leadership dynamics in Jordanian healthcare environments.
It is worth noting that this study stems from a Master's thesis. In this paper, the authors have utilized total scores to represent the levels and correlations among the variables studied, while also comparing the perceived authentic leadership of nursing leaders. Since this topic is relatively new, using total scores helps mitigate the risk of Type II errors (Polit & Beck, 2019), which in turn strengthens the validity and reliability of the findings. The researchers will dive deeper into the analyses of individual variable levels and the differences in self-efficacy, job satisfaction, and intent to stay among nurses in future publications. Interestingly, no prior research has explored the relationship between nursing leaders’ authentic leadership and nurses’ self-efficacy, job satisfaction, and intent to stay all at once. This gap highlights the relevance of the current study. The results could provide valuable insights for nursing administrators and policymakers as they craft and implement leadership interventions aimed at promoting authentic leadership practices, which could lead to enhanced self-efficacy, job satisfaction, and retention among nurses.
Methods
Guided by the STROBE checklist, this study investigated the impact of the perceived nursing leaders’ authentic leadership on the perceived hospital nurses’ general self-efficacy, job satisfaction, and intent to stay at work.
Study Design
A quantitative cross-sectional design was utilized in the study. This design was appropriate to describe the levels of the main variables and examine the correlations between them. This design aligns with the study's aim to capture a snapshot of variables at a single point in time (Polit & Beck, 2019). Cross-sectional studies are cost-effective and practical, offering initial insights that can inform future longitudinal research (Polit & Beck, 2019). Given these advantages, the design was suitable for exploring leadership and nurses’ outcomes in healthcare environments. Researchers utilized a cross-sectional design to explore the effects of potential causes that were beyond their control (Polit & Beck, 2019).
Settings and Sample
In Jordan, there are 68 private hospitals, 33 government hospitals, 15 military hospitals, and 2 university-affiliated hospitals (Ministry of Health, 2021). This distribution reflects the diversity of healthcare organizations. The study was conducted in three government hospitals, one university hospital, and two private hospitals. These hospitals were located in the northern region and had bed occupancy rates exceeding 100%, making them suitable for studying leadership and workforce outcomes. The research covered all nurses who worked in Jordanian hospitals. The study's accessible population comprised nurses working in the designated hospitals. This focus ensured that the sample was relevant and aligned with the study's objectives.
Nurses were recruited using a non-random approach by convenience sampling of nurses from various sectors. To determine the appropriate sample size for such a correlational study, the researchers used the G*power 3.1.10 program, aiming for a power level of 0.80 and a significance level of .05, factoring in a medium effect size of 0.30. The analysis indicated a minimum of 249 participants; to account for potential data loss, the sample size was increased to 300. Of the 300 distributed questionnaires, 297 were returned, and 295 were complete and included in the final analysis, resulting in a response rate of 98.33%. Data collection occurred across different shifts, with night shifts being particularly helpful due to the absence of managers.
For the present sample's inclusion criteria, all nurses needed to have at least a year of experience in hospital settings and at least a diploma degree (which is equivalent to an associate degree in Jordan). Nursing students, administrative nurses without direct patient contact, and junior nurses with less than 1 year of experience were excluded.
Instruments
A demographic form was used to collect information on background variables such as age, gender, educational status, marital status, nursing experience, unit, worked shift, and type of hospital. This essential data provided context for the participants’ responses and made it possible to compare different subgroups. Authentic Nurse Leadership was measured by Giordano-Mulligan's Authentic Nurse Leader Questionnaire (ANLQ) (Giordano-Mulligan & Eckardt, 2019). Permission to use and translate the scale was granted by the original authors. To make sure it was linguistically and culturally suitable, the scale went through a thorough translation process. The scale was translated into the Arabic language using the translation and back translation methods by experts in the English and Arabic languages. Further, the content validity of the Arabic version of ANLQ was assessed by a panel of three expert faculty members who are interested in the research topic, and two other experts checked the translated Arabic version with the tool's original author. These steps helped to confirm that the instrument was valid and reliable for use in the Jordanian context.
The ANLQ consists of 29 items on a 5-point Likert-type scale, ranging from 0 to 4. Items are grouped into 5 subscales, which are: (1) Self-awareness, (2) Moral Ethical Courage, (3) Relational Integrality, (4) Shared Decision Making, and (5) Caring. This framework enables a thorough evaluation of leadership qualities from various perspectives. Participants were asked to express how they perceived their leader exhibiting the authentic leader attributes on a Likert scale ranging from 0 (never) to 4 (all of the time). The overall nursing leaders’ authentic leadership score was calculated by taking the average for all items, which was classified according to Giordano-Mulligan and Eckardt (2019) as minimal to low with a mean score of 0 to 1, low with a mean score of 1 to 2, moderate with a mean score of 2 to 3, and high with a mean score of 3 to 4. In the original study, the alpha coefficient was 0.96 (Giordano-Mulligan & Eckardt, 2019). In this study, the alpha coefficient for the whole scale was 0.98. This high reliability supports the internal consistency of the instrument in the current context.
General Self-Efficacy was operationally defined by the General Self-Efficacy Scale (GSE)—the Arabic version (Schwarzer & Jerusalem, 1995). The original authors granted permission to use the scale. It consists of 10 items measured on a Likert scale ranging from 1 (not at all true) to 4 (exactly true). A 1 to 4 Likert scale is commonly classified into mild (low): 1.00 to 2, moderate: 2.01 to 3.00, and high (strong): 3.01 to 4.00. The total score ranged from 10 to 40; a higher score indicates a greater sense of self-efficacy. The alpha coefficient was between 0.76 and 0.90 (Schwarzer & Jerusalem, 1995). In the current study, the alpha coefficient for the whole scale was 0.92. This result indicates strong reliability and supports the scale's use in measuring nurses’ self-efficacy.
Available in the public domain, job satisfaction was measured by the Arabic version of McCloskey and Mueller's Satisfaction Scale (MMSS) was used to measure nurses’ job satisfaction (Mueller & McCloskey, 1990). This scale consists of 31 items on a 5-point Likert scale, where 5 indicates “very satisfied,” and 1 indicates “very dissatisfied.” The total score of all subscales was added to determine the level of nurses’ job satisfaction. A 1 to 5 Likert scale is commonly classified into mild (low): 1.00 to 2.33, moderate: 2.34 to 3.67, and high (strong): 3.68 to 5.00. Higher scores indicate greater nurses’ job satisfaction. The alpha coefficient for this scale in the original study was 0.89 (Mueller & McCloskey, 1990) and 0.96 in the current study. These results confirm the scale's reliability and appropriateness for assessing nurses’ job satisfaction.
Available in the public domain, intent to stay at work was measured by the Arabic version of McCain's Intent to Stay Scale, which is a part of McCain's Behavioral Commitment Scale. This scale contains five items on a 5-point Likert-type scale, wherein 1 (strongly disagree) and 5 (strongly agree). A 1 to 5 Likert scale is commonly classified into mild (low): 1.00 to 2.33, moderate: 2.34 to 3.67, and high (strong): 3.68 to 5.00. Higher scores indicate greater nurses’ intent to remain at work. The alpha coefficient of this scale in the original study was 0.88 (McCloskey & McCain, 1987) and 0.92 in the present study. This reliability supports the scale's use in evaluating nurses’ intent to stay in their current roles.
Ethical Considerations
The study was approved by the Institutional Review Board of the Jordan University of Science and Technology, Jordan approved the study. IRB No. 40/49/2021, dated July 6th, 2022, the Ministry of Health (#MOH/REC/2/022/285, dated Sept. 14th 2022), as well as the targeted hospitals. The participants participated voluntarily and were informed that they could withdraw at any time. Anonymous questionnaires were used to maintain privacy and confidentiality. The questionnaires were completed by each participant voluntarily and submitted directly to the researchers in a sealed envelope.
Participant Recruitment and Questionnaire Distribution
The researchers approached all the targeted hospitals and obtained the necessary approvals to reach out to potential participants. After securing these permissions, they kicked off the data collection using a structured survey running from September 1st to October 6th, 2022. Before diving into this phase, they conducted a pilot study with 30 nurses, making up about 10% of the total sample, who worked in hospital settings. This pilot study was done to check how clear, reliable, and how long it would take to complete the questionnaire. Those participating in the pilot study were not included in the final sample. The findings from this pilot confirmed that the questionnaire was easy to understand and would take around 10 to 15 minutes to fill out. The reliability coefficients were impressively high for all the assessment tools: 0.98 for the Authentic Leadership Questionnaire, 0.94 for the Job Satisfaction Scale, 0.88 for the Intention to Stay Scale, and 0.89 for the General Self-Efficacy Scale.
To invite participants, the researchers provided a thorough overview of the study and its goals to each nurse, ensuring they understood everything before giving their informed consent to participate. The questionnaires, which included all the necessary study instruments, were then handed out in person by the researchers to nurses working on different units and shifts. Participation was entirely voluntary, and nurses were reminded that they could opt out at any time. To maintain confidentiality and privacy, the questionnaires were anonymous and filled out individually by each participant. Completed forms were then returned directly to the researchers in sealed envelopes.
Data Analyses
Data were analyzed using the Statistical Package of Social Sciences software (IBM Corp, Version 26, 2019). The α-level of significance was set at .05. Prior to analysis, the dataset was screened for missing values and outliers. All variables were checked for normality and outliers; no violations were detected. Questionnaires with more than 20% missing responses were excluded from the analysis; two were removed for this reason. For the remaining cases, missing values were replaced using item-level mean substitution.
Different statistics were used to answer the research questions. For this study, nursing leaders’ authentic leadership (independent variable), nurses’ general self-efficacy, job satisfaction, and intent to stay among nurses (dependent variable) were treated as continuous variables; thus, means and standard deviations were used to report the level of these variables (the first research question), and Pearson's correlation coefficient tested the relationships between these continuous variables (the second research question) (Polit & Beck, 2019). These methods were appropriate for uncovering associations within the data. The differences between continuous and two-value categorical variables, such as gender, were analyzed by an independent t-test. Also, the one-way analysis of variance (ANOVA) test was used to test the relationships between continuous and three-value categorical variables, such as the type of hospitals (private, governmental, and university-affiliated hospitals (the third research question); those tests were followed by Tukey's post hoc test to assess the source of differences (Polit & Beck, 2019). These statistical methods were selected to ensure robust analysis of relationships and group comparisons relevant to the study objectives. Different statistical methods were used to address the three research questions: descriptive statistics for variable levels (RQ1), Pearson's correlation for relationships (RQ2), and t-tests/ANOVA with Tukey's post hoc tests for group differences (RQ3).
Results
Sample Characteristics
The majority of the study participants were females (80.00%). Most of the participants were married (70.80%) and had baccalaureate degrees (70.50%). The respondents’ ages ranged from 20 to 49 years, with a mean of 31.00 years. The nursing experience ranged from 1 to 27 years, with a mean of 7.70 years. Table 1 presents detailed background data of the sample.
Demographic Characteristics of Participants (n = 295).
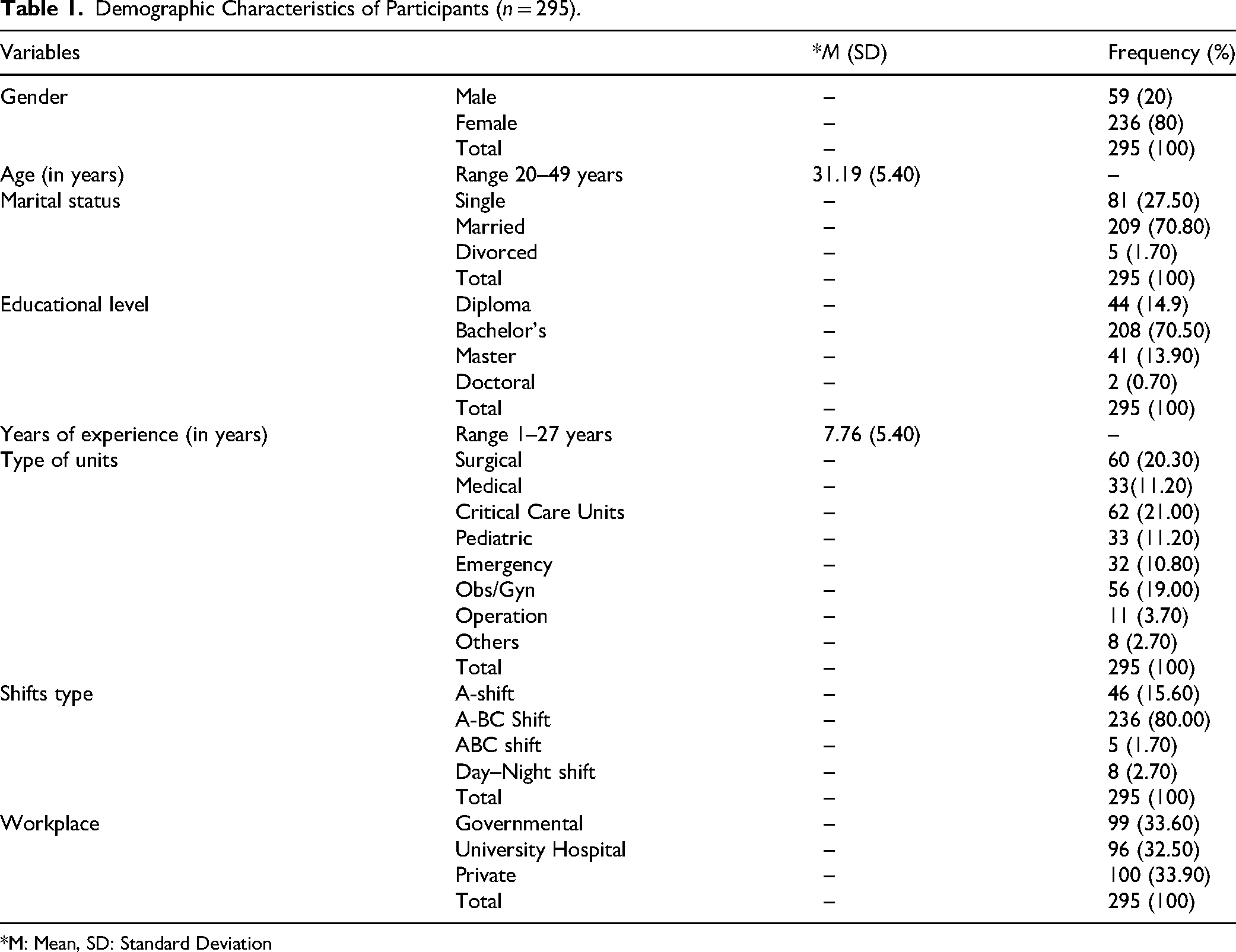
*M: Mean, SD: Standard Deviation
The Levels of the Studied Variables
According to the rules used for classifying the Likert scales in the current study, reported with the instrument, the results showed that the overall mean score of the perceived nursing leaders’ authentic leadership was 2.68 (SD = 0.91, on a scale from 0 to 4), which means that nurses perceived that their leaders had a moderate level of authentic leadership. The overall mean score of the perceived hospital nurses’ general self-efficacy was 2.94 (SD = 0.60 on a scale of 1 to 4), which is above the average level, which means that participants perceived themselves as having sufficient general self-efficacy. Moreover, the overall mean score of the perceived nurses’ job satisfaction was 2.72 (SD = 0.88, on a scale of 1 to 5), which means that the nurses were moderately satisfied. The overall mean score of the perceived nurses’ intent to stay at work was 2.81 (SD = 1.12, on a scale of 1 to 5), which means that nurses had a moderate level of intent to stay at work (Table 2).
Levels of Nursing Leaders’ Authentic Leadership, Nurses’ Job Satisfaction, Intent to Stay, and General Self-Efficacy At Work Based On Levels Total Scores (n = 295).

Likert scale ranges: Authentic leadership (0–4), Job satisfaction (1–5), Self-efficacy (1–4), Intent to stay (1–5).
The Relationships Between the Studied Variables
The results indicated a significant, moderate, positive correlation between authentic leadership and nurses’ general self-efficacy (r = .313, P < .01); a significant, strong, positive correlation was found between authentic leadership and nurses’ job satisfaction (r = .589, P < .01); and a significant, moderate, positive correlation between authentic leadership and nurses’ intent to stay at work (r = .415, P < .01). These findings highlight the influential role of authentic leadership in shaping nurses’ intent to stay. Those results indicate that nurses who perceived their leaders as authentic leaders had higher general self-efficacy, were more satisfied, and had higher intent to stay at work than nurses who perceived their managers as non-authentic. This finding suggests that authentic leadership style is a critical factor in promoting nurses’ intent to stay and job satisfaction. Nurses who perceived a high sense of general self-efficacy intended to stay longer at work than their counterparts (r = .335, P < .01), and those who were satisfied at work reported higher general self-efficacy and intended to stay longer at work (r = .563, P < .01) than less satisfied nurses (r = .433, P < .01) (Table 3). Together, these correlations reinforce the interconnectedness of nursing leaders’ authentic leadership and nurses’ general self-efficacy, job satisfaction, and intent to stay.
Pearson's Correlations Between Nursing Leaders’ Authentic Leadership, Nurses’ General Self-Efficacy, Job Satisfaction, and Intent to Stay At Work (n = 295).

** Correlation is significant at the .01 level (2-tailed). All values marked with ** indicate statistically significant correlations.
The Differences in the Perceived Nursing Leaders’ Authentic Leadership
The results showed no significant differences in the perceived nursing leaders’ authentic leadership in regard to age, experience, gender, marital status and working units. These findings suggest that background variables may not strongly influence nurses’ perceptions of authentic leadership. However, the ANOVA test indicated the presence of significant differences in the perceived nursing leaders’ authentic leadership based on educational level, shift type, and the type of hospital. This result underscores the importance of contextual factors in shaping the nurses’ perception of authentic leadership. Tukey's post hoc test indicated that nurses (a) holding master's degrees perceived a lower mean of authentic leadership than nurses holding bachelor's or diploma degrees (f (3, 291) = 6.88, P < .001); (b) working straight A-shift perceived a higher mean of the perceived nursing leaders’ authentic leadership than those working rotating A-BC and Day–Night shifts (f (3, 291) = 6.33, P < .001); and (c) working in private hospitals perceived higher levels of authentic leadership compared with nurses who worked in governmental hospitals, and university-affiliated hospitals (f (2, 292) = 15.69, P < .001) (Table 4). These results indicate the influence of work environments and organizational factors on nurses’ perceptions of authentic leadership.
The Differences in the Perceived Nursing Leaders’ Authentic Leadership Based on Background Variables Using T-Test, F-Test Followed by Tukey Post Hoc (n = 295).

M: mean; SD: standard deviation; P-value significant at ≤.05.
* Tukey's post-hoc test: Master's degree holders reported lower authentic leadership scores than Diploma and Bachelor's degree holders.
** Tukey's post-hoc test: Nurses working straight A-shifts perceived higher authentic leadership than those working A-BC and Day–Night shifts.
*** Tukey's post-hoc test: Nurses in private hospitals perceived higher authentic leadership than those in governmental and university-affiliated hospitals.
Discussion
This study investigated the impact of the perceived nursing leaders’ authentic leadership on the perceived hospital nurses’ general self-efficacy, job satisfaction, and intent to stay at work. This focus reflects the growing interest in relational leadership styles and their influence on healthcare workforce outcomes. Hospital nurses perceived that their leaders had a moderate level of authentic leadership. The nurses perceived themselves as having sufficient general self-efficacy. They were moderately satisfied with a moderate level of intent to stay at work.
The theoretical framework guiding this study integrates Avolio's authentic leadership theory (Avolio, 2024; Avolio & Gardner, 2005) and Giordano-Mulligan and Eckardt's nursing leadership framework (Giordano-Mulligan & Eckardt, 2019). These frameworks highlight key qualities like self-awareness, relational transparency, and moral courage. These traits are crucial for creating an environment where nurses feel psychologically safe, satisfied with their jobs, and motivated to stay at their jobs. The study's findings underscore this, showing that authentic leadership is positively linked to nurses’ self-efficacy, satisfaction levels, and their intention to remain in their roles or jobs.
The findings of the current study provide a baseline understanding of nurses’ perceptions of the studied variables within work environments at hospitals. Correlations indicated that nurses who perceived their leaders as authentic leaders had higher general self-efficacy, were more satisfied, and had higher intent to stay at work than nurses who perceived their managers as non-authentic. This result suggests that authentic leadership may serve as a protective factor against common workplace challenges such as job dissatisfaction and turnover. Nurses who perceived a high sense of general self-efficacy intended to stay longer at work than their counterparts, and those who were satisfied at work reported higher general self-efficacy and intended to stay longer at work than less satisfied nurses. These interconnections underscore the importance of psychological empowerment and job satisfaction in retention strategies.
The ANOVA indicated significant differences in the perceived nursing leaders’ authentic leadership based on educational level, shift type, and the type of hospital. These findings highlight the contextual nature of leadership perceptions and suggest that organizational structure and scheduling may influence how nurses experience leadership.
The Levels of the Studied Variables
More specifically, the current nurses believed that their leaders possessed moderate levels of authentic leadership. This perception aligns with existing national research and sets the stage for comparison with international findings. This finding is consistent with Jordanian research (Mrayyan et al., 2023), and other foreign studies have revealed a high degree of authentic leadership (Labrague et al., 2021, 2025; Raso et al., 2020). The moderate perception may be due to the use of transactional leadership styles in some settings, particularly in shared decision-making, which was rated lowest.
The present nurses considered themselves to have enough general self-efficacy. This self-assessment shows that nurses in the hospitals studied have a really positive psychological outlook. This finding is similar to the Jordanian research by Al-Hamdan and Bani Issa (2021). This level might be attributed to the desire to work in the nursing profession, which is a popular specialization in Jordanian culture, as well as the support nurses receive from friends, family, and coworkers. Nurses typically view themselves as possessing adequate general self-efficacy, which reflects their confidence in managing a variety of challenges encountered in their profession (Chen et al., 2025). This confidence in their skills significantly impacts their motivation, decision-making, and resilience when confronted with obstacles (Chen et al., 2025). Self-efficacy is essential for nurses in delivering high-quality care (Al-Hamdan & Bani Issa, 2021). These findings highlight just how crucial it is to nurture self-efficacy by creating supportive environments and investing in professional development.
The results also indicated that participants were moderately satisfied, which is comparable with recent analysis (Alsadi et al., 2025). This moderate level of satisfaction could point to some underlying issues in the healthcare environment. Other studies, like those from Korea (Lee et al., 2020), found that nurses were more satisfied with their jobs. This level may be explained by the fact that the majority of Jordan's nurses are married females who may experience work-life conflicts, as well as the presence of other work variables such as limited resources, a shortage of nurses, low salaries, a demanding workload, a restrictive work environment, high acuity patients, and long working hours (16 hours BC-shift). The combination of these factors makes it quite challenging to attain high job satisfaction among nurses in Jordan.
In this research, the level of nurses’ intent to stay at work was at a moderate level. This discovery aligns with what is happening across the country and sheds light on the persistent issues the researchers face with nurses’ intent to stay at work. These findings are consistent with earlier national surveys (Al-Hamdan et al., 2020), which found an above-average level of nurses’ intent to stay in Jordan. Higher levels were seen in foreign investigations (Lee et al., 2020). Several factors for this moderate level to stay at work include (a) the high rate of migration to better living circumstances, (b) the preference of certain employees for administrative and academic positions, and (c) the inclination to study and work in Western countries. These influences indicate that effective retention strategies need to consider not just professional goals but also the wider socioeconomic context.
The Relationships Between the Studied Variables
The study revealed a significant, moderate positive correlation between authentic leadership and nurses’ general self-efficacy, consistent with Azila-Gbettor et al. (2025), who found similar results among military officers in Ghana. This finding may be due to authentic leaders’ supportive nature and encouragement of personal growth (Giordano-Mulligan & Eckardt, 2019), as self-efficacy is shaped by interpersonal support (Saleem et al., 2023).
A strong, positive correlation was also found between authentic leadership and nurses’ job satisfaction, aligning with prior studies (Specchia et al., 2021; Wong et al., 2020; Yasin et al., 2020). Authentic leadership fosters open communication, care, and engagement, creating a work environment conducive to satisfaction. Additionally, authentic leadership showed a significant, moderate positive correlation with nurses’ intent to stay. Though underexplored, this supports findings linking authentic leadership to reduced turnover intention (Alkarabsheh et al., 2022) and aligns with Giordano-Mulligan and Eckardt's (2019) framework, which emphasizes engagement and healthy environments as retention drivers.
The study also found a novel, moderate positive correlation between nurses’ general self-efficacy and job satisfaction, suggesting intrinsic motivation and interest in nursing enhance both. Similarly, self-efficacy was moderately and positively correlated with intent to stay, indicating it may predict retention. Finally, a strong, positive correlation was observed between job satisfaction and intent to stay, consistent with previous research (Alnuaimi et al., 2020). Satisfied nurses are more likely to remain in their roles, highlighting job satisfaction as a key retention strategy.
The Differences in the Perceived Nursing Leaders’ Authentic Leadership
The study found no significant differences in perceived authentic leadership based on age, gender, experience, marital status, or work unit, suggesting these background factors may not influence nurses’ perceptions—consistent with Mrayyan et al. (2023) and Raso et al. (2020). Interestingly, nurses with master's degrees reported lower perceptions of authentic leadership than those with bachelor's or diploma degrees, indicating that educational background may shape leadership expectations. This finding contrasts with Raso et al. (2020), who found no such differences.
Nurses working straight A-shifts perceived higher levels of authentic leadership than those on rotational shifts (A-BC or Day–Night), possibly due to more frequent interaction with supervisors who typically work A-shifts. This finding differs from Raso et al. (2020), potentially due to cultural or organizational differences. Perceptions of authentic leadership were also higher in private hospitals compared to governmental and university-affiliated ones. This result may reflect differences in governance, leadership selection criteria, and the use of shared governance models in private institutions.
In summary, authentic leadership significantly enhances nurses’ experiences—including self-efficacy, job satisfaction, and intent to stay—and these findings offer valuable insights for leadership development and healthcare policy.
Strengths
This study provided a comprehensive analysis of how authentic leadership influences nurses’ general self-efficacy, job satisfaction, and intent to stay in Jordan—addressing a key gap in the literature and offering insights for healthcare organizations facing moderate levels of these challenges. As the first study of its kind in Jordan, it contributes meaningfully to nursing leadership research and offers practical guidance for leadership development and policy.
Methodologically, the study used valid, reliable tools and integrated Avolio's theory (Avolio, 2024; Avolio & Gardner, 2005) and Giordano-Mulligan and Eckardt's framework (2019), enriching the understanding of trust, ethics, and psychological safety in nursing teams.
Limitations and Directions for Future Research
This study had several limitations. (a) Self-reported data may be influenced by social desirability bias (Polit & Beck, 2019). (b) Cross-sectional design limits causal inference; longitudinal studies are recommended. (c) ANOVA analysis identified group differences but lacked depth in assessing interrelationships; future studies should use regression, SEM, or path analysis. (d) A limited scope may omit other influential organizational or personal factors. (e) Geographic focus restricts generalizability; cross-cultural research is needed to broaden applicability. Despite these limitations, the study offers valuable insights into how authentic leadership can improve nurse retention and workplace outcomes—critical for healthcare administrators and policymakers aiming to strengthen workforce stability and care quality.
Future studies should compare authentic leadership with other styles—such as transformational, transactional, and servant leadership—to better understand its unique impact on satisfaction, retention, and performance (Adams et al., 2024; Munyon et al., 2021; Yavuz, 2020). These comparisons can clarify authentic leadership's distinct value across various organizational contexts. Research should also explore how cultural norms and organizational structures influence the effectiveness of authentic leadership. Cross-cultural studies would enhance the generalizability of findings and reveal how leadership expectations vary globally.
Advanced analytical methods—such as regression analysis, structural equation modeling (SEM), and path analysis—are recommended to identify key predictors and outcomes of authentic leadership (Walumbwa et al., 2008). While this study used Pearson's correlation, t-tests, and ANOVA, future research could benefit from multivariate approaches to uncover deeper relationships. Finally, comparative and context-sensitive studies using robust analytical tools (Legutko, 2020) will provide a clearer picture of authentic leadership's role and effectiveness in diverse healthcare settings.
Implications for Nursing
This study highlights moderate levels of authentic leadership, self-efficacy, job satisfaction, and intent to stay among nurses in Jordan—indicating an urgent need for targeted interventions. Evidence-based strategies (Alshaibani et al., 2024; Kallerhult Hermansson et al., 2024) can help improve these outcomes:
Leadership and Psychological Safety: Authentic leadership training: Promote self-awareness, transparency, and ethical decision-making to boost confidence and satisfaction. Psychological safety: Encourage open communication and reduce fear of errors to strengthen self-efficacy and retention. Professional Development: Mentorship: Pair nurses with experienced mentors to support growth. Continuous education: Provide ongoing training in clinical and leadership skills to enhance satisfaction and commitment. Workplace Well-being and Culture: Burnout prevention: Use fair scheduling to reduce stress and improve retention. Recognition: Reward contributions to foster loyalty. Inclusive decision-making: Involve nurses in policy discussions and offer flexible scheduling to boost engagement. These three strategies can help healthcare organizations create supportive environments that enhance leadership effectiveness and workforce stability.
In terms of educational practice, the advantages of authentic leadership highlight the necessity for focused training, particularly for new leaders facing transitional challenges. Equipping future nursing leaders with these competencies is essential for sustaining an effective nursing workforce. For theory, these results support the framework proposed by Giordano-Mulligan and Eckardt (2019), which connects authentic leadership characteristics with enhanced nurse outcomes. This framework, which closely aligns with Avolio's model (Avolio, 2024; Avolio & Gardner, 2005), emphasizes the importance of trust, ethical decision-making, and psychological safety. These models lay a solid theoretical background for authentic leadership development in nursing.
Conclusion
The results showed how tightly nursing leaders’ authentic leadership is linked with nurses’ self-efficacy, job satisfaction, and intent to stay at work, implying that building a culture of authentic leadership and inclusively psychological safety may increase nurses’ self-efficacy, job satisfaction, and intent to stay at work, indicating that fostering a culture of authentic leadership and psychological safety may enhance these outcomes. This connectedness underscores the importance of developing authentic leadership as a strategic priority for healthcare organizations. The significant differences in the perceived nursing leaders’ authentic leadership based on educational level, shift type, and the type of hospital suggest that contextual factors play a critical role in shaping leadership effectiveness. These findings suggest that there is no universal formula for effective authentic leadership, and it must be tailored to the unique context of each organization.
Therefore, further research is needed to study how authentic leadership can be tailored across diverse healthcare environments. These factors should be investigated further to adapt authentic leadership to different organizational contexts and countries. These findings underscore the need for different leadership interventions, such as initiating authentic leadership development programs to start with; these programs would emphasize the authenticity that is needed to boost nurses’ general self-efficacy, job satisfaction, and intent to stay at work.
Footnotes
Acknowledgments
The researchers would like to thank all participants for their input in the current study.
Ethics Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board of the Jordan University of Science and Technology, Jordan approved the study. IRB No. 40/49/2021, dated July 6th, 2022, the Ministry of Health (#MOH/REC/2/022/285, dated Sept. 14th 2022), and the targeted hospitals.
Consent to Participate
Written informed consent was obtained from all subjects involved in the study. Organizational and participant consents were obtained. Personal information that could identify individuals was not collected.
Consent for Publication
This article includes data obtained from individual participants. Written informed consent for publication was obtained from all participants. All authors hereby give their consent for the publication of the article, including all associated data published by Sage Publications.
Authors’ Contributions
Study design and data analysis were done by RA and LB.
Data collection was done by LB.
Study supervision was done by RA.
Manuscript writing was done by RA, MTM, LB.
Critical revisions for important intellectual content were done by RA, MTM.
Final approval of the version was done by RA, LB, MTM.
Authorship Statement
The authors listed meet the authorship criteria according to the latest guidelines of the International Committee of Medical Journal Editors, and the authors agree with the manuscript. The authors have approved the content before submission or resubmission.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Declaration of Generative AI and AI-Assisted Technologies in the Writing Process
During the preparation of this work, the authors used Grammarly and Copilot to edit language and condense paragraphs. After using this tool, the authors reviewed and edited the content as needed and took full responsibility for the content of the publication.
Availability of Data and Materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Patient or Public Contribution
There was no patient or public contribution, as the sample included nurses recruited from different hospitals.
Reporting Method
The authors of this manuscript have adhered to the STrengthening the Reporting of OBservational Studies in Epidemiology (STROBE) checklist was used to guide the study.
