Abstract
Background
The flipped classroom model (FC) has gained prominence in nursing education for its emphasis on active, student-centered learning. While global evidence supports its efficacy in skill-based training such as cardiopulmonary resuscitation (CPR), limited studies have evaluated its impact within Middle Eastern nursing programs, particularly in Oman.
Objective
This study aimed to assess the effectiveness of the FC approach in enhancing CPR knowledge, skills, and learner perception among first-year nursing students.
Methods
Exploratory quasi-experimental one-group pretest/post-test design was conducted among 177 first-year nursing students enrolled in the Fundamentals of Nursing I course at the University of Buraimi, Oman. Participants completed preclass materials, followed by collaborative case-based discussions and skill demonstrations. CPR knowledge was assessed through multiple-choice tests, skills through a standardized checklist, and perceptions using a validated Likert-scale questionnaire.
Results
There was a statistically significant improvement in CPR knowledge scores from pretest (M = 6.81, SD = 3.20) to post-test (M = 10.88, SD = 2.00; p < .001). Knowledge scores moderately correlated with CPR skill performance (r = .209, p = .005), though no significant correlations were found with perception scores. Female students demonstrated significantly higher CPR performance than males (p = .023). Overall, students expressed positive perceptions of the FC model.
Conclusion
The FC approach significantly improved CPR knowledge and moderately influenced skill acquisition among novice nursing students, irrespective of academic standing. These findings suggest potential benefits of integrating FC methods but should be interpreted as exploratory within a single-group design. Support the integration of active, student-centered methodologies in nursing education across the Middle East. Further research is recommended to explore long-term retention and clinical application.
Keywords
Introduction
Cardiopulmonary resuscitation (CPR) is a critical, life-saving intervention that requires both theoretical knowledge and psychomotor proficiency. For nursing students—who are often among the first responders in clinical emergencies—early mastery of CPR is essential for improving patient survival outcomes. However, research consistently indicates that traditional lecture-based instruction, while effective for knowledge transmission, often fails to provide sufficient opportunities for hands-on practice, active engagement, and critical decision-making skills necessary for high-quality CPR performance (Cheng et al., 2019; Hew & Lo, 2018). This pedagogical gap has prompted educators worldwide to seek innovative teaching strategies that optimize both cognitive and psychomotor learning outcomes.
The flipped classroom (FC) model has emerged as a promising approach in health professional education, reversing the traditional sequence of content delivery and practice. In this model, foundational learning occurs before class through digital resources—such as pre-recorded lectures and instructional videos—while in-class time is dedicated to active, collaborative learning activities and skill application (Betihavas et al., 2016; Della Ratta, 2020). By shifting passive learning outside the classroom, the FC model allows educators to use face-to-face sessions for case-based discussions, simulation exercises, and immediate feedback—elements shown to enhance both knowledge retention and skill competency (Park & Howell, 2021).
In the Middle East, nursing education has undergone rapid modernization over the last decade, integrating active learning methodologies such as problem-based learning, simulation-based training, and FCs to align with global accreditation standards and national health priorities (Aboshaiqah et al., 2018). Countries like Saudi Arabia, Jordan, and the United Arab Emirates have reported positive outcomes from FC adoption in skill-based nursing courses (Ali, 2025; Al-Qahtani et al., 2022). In Oman, the healthcare sector's expansion and the Ministry of Health's emphasis on improving emergency response capabilities have heightened the need for high-quality CPR training among novice nursing students. Yet, few studies in the Omani context have investigated the use of FC in CPR education.
Despite global evidence supporting the FC model in skill-based training, research in Oman remains scarce, especially in foundational clinical skills such as CPR. Existing regional studies—such as Joseph et al. (2021), which examined FC in anatomy and physiology courses—demonstrated improved examination performance, but the direct impact on psychomotor skills like CPR remains largely unexplored. Moreover, studies have shown mixed findings on student satisfaction and self-efficacy in FC environments (Joseph et al., 2025), highlighting the need to evaluate both objective performance outcomes and subjective learner perceptions.
Given the urgent clinical relevance of CPR competence, the dominance of traditional teaching methods in many Middle Eastern nursing programs, and the limited evidence from Oman, this study addresses a critical gap. By systematically evaluating the effect of a FC approach on CPR knowledge, skills, and perceptions among first-year nursing students, this research aims to inform curriculum design, support national educational reforms, and ultimately enhance the preparedness of future nurses in life-saving interventions.
Literature Review
Research has shown that the FC model enhances clinical and psychomotor skill development among nursing students. Hew and Lo (2018) conducted a meta-analysis of 28 studies in healthcare education, concluding that FC improves academic performance and skill mastery by fostering interactive learning. Similarly, Cheng et al. (2019) found that nursing students trained in FC performed CPR with greater accuracy and retained knowledge better than those taught through traditional lectures. Additionally, Yang et al. (2019) reported that FC students scored significantly higher in CPR assessments and expressed greater confidence in their skills, highlighting the effectiveness of this approach for skill-based learning.
The FC model promotes active learning, resulting in higher student engagement and motivation. Park and Howell (2021) found that 80% of nursing students preferred FC over traditional teaching due to its emphasis on interactive learning, peer collaboration, and hands-on practice. Similarly, Fisher et al. (2021) reported that FC led to higher participation rates, improved critical thinking skills, and a deeper conceptual understanding compared to passive learning methods. However, challenges remain, including increased student workload, difficulties in adapting to self-directed learning, and faculty resistance to new teaching approaches (Betihavas et al., 2016).
However, some challenges exist, such as increased workload for students, difficulty adapting to self-directed learning, and faculty resistance to adopting new teaching strategies (Betihavas et al., 2016).
Nursing education in the Middle East has undergone significant transformation in recent years, with universities increasingly integrating active learning methodologies such as problem-based learning (PBL), simulation training, and FCs (Aboshaiqah et al., 2018). Given the high demand for skilled nurses, particularly in emergencies and critical care, modern teaching approaches are essential for improving clinical competencies.
Research Questions
What is the effect of FC on students’ knowledge retention of CPR guidelines?
Does the FC approach improve first-year nursing students’ CPR skill proficiency?
What is the impact of FC on students’ perception of self-efficacy?
Method
Study Design
An exploratory quasi-experimental study with one group pretest and post-test design was employed to evaluate the effectiveness of a FC approach in improving CPR knowledge and skills among first-year nursing students.
Study Setting and Population
The study was conducted at the University of Buraimi, Oman, among undergraduate nursing students enrolled in the Fundamentals of Nursing course during the Spring 2025 semester.
Sample and Sampling Technique
Sample size was estimated using a 95% confidence interval (Z = 1.96), a margin of error of 5%, and an expected effect size derived from prior similar studies. The STROBE guidelines were followed in reporting. All students enrolled in the Fundamentals of Nursing I course during the Spring 2025 semester (N = 220) was invited to participate, making the sample a near-census of the cohort with voluntary participation rather than a convenience subset. Of these, 177 students consented and completed all study components (response rate 80%). First-year nursing students registered in the Fundamentals of Nursing I course during the Spring 2025 semester who volunteered to participate in the study were included. Students who were absent or those who refused to participate during the data collection period were excluded from the study.
Ethical Consideration
Ethical approval was obtained from the Research and Ethics Committee of the University and Ethics committee of the College of Health Sciences, University of Buraimi. Participation was voluntary, and written informed consent was obtained from all students. Confidentiality was ensured by assigning anonymous identification codes and securely storing all data on password-protected devices.
Data Collection Procedure
Data collection was conducted in two sequential phases over a 2-week period to capture baseline measures, intervention effects, and postintervention perceptions. The process was standardized for all participant group to ensure consistency and reliability.
Prior to the intervention, all eligible participants were invited to a scheduled orientation session. The Objectives and procedures of the study were explained, and informed consent was obtained. Participants received instructions to access the preclass learning package via the Moodle platform. This package included a Power Point lecture and the official American Heart Association (AHA) Basic Life support (BLS) instructional Video. On the second week during the class session (2 hours) the participants completed the pretest knowledge assessment using validated multiple-choice questionnaire aligned with the latest AHA BLS guidelines. Followed students were divided into smaller groups of 5 to 6 students for collaborative discussions based on clinical scenarios. Case scenarios were projected for group analysis, and responses were reviewed collectively during a class-wide discussion. The facilitators moderated the sessions and reinforced key CPR core concepts.
After the classroom session, students transitioned to the simulation laboratory for a 2-hour CPR practical skills session. Using medium-fidelity Resusci Anne Manikins participants individually performed the entire CPR sequence, including chest compressions, rescue breathing, and AED use. Four BLS certified instructors, each assigned to evaluate a subset of participants, used the standardized AHA CPR skills checklist to assess performance. Each student was evaluated individually, ensuring personalized observation. Immediate formative feedback was given to correct technique errors. Skill performance was repeated, if necessary, until procedural accuracy was demonstrated.
One week after completing the in class and laboratory sessions, post-test knowledge was assessed with the same validated multiple-choice questionnaire used for the pretest to measure knowledge retention and improvement. Also, a validated perception questionnaire was distributed to assess student satisfaction, perceived usefulness of FC approach, and self-reported confidence in performing CPR.
Measurements and Tools
Sociodemographic variables (age, gender, and cumulative grade point average [CGPA]) were collected using a structured questionnaire.
Knowledge assessment: A set of 10 NCLEX-style multiple-choice questions (MCQs) developed and validated by the research team.
CPR skill performance: Evaluated using standardized AHA checklist through direct observation by trained BLS instructors.
Perception survey: A 7-item Likert scale questionnaire adopted from Mengesha et al. (2024). It is a 5-point Likert scale ranging from “strongly disagree” to “strongly agree,” allowing participants to express varying levels of agreement. The instrument demonstrated validity and reliability within the target population.
All instruments demonstrated validity and reliability, with Cronbach's alpha values exceeding 0.80 for internal consistency.
Data Analysis
Data were analyzed using SPSS version 23. Descriptive statistics were used to summarize demographic data and outcome variables. Paired sample t-tests compared pre-intervention and postintervention knowledge scores. Independent sample t-tests and one-way analysis of variance (ANOVA) examined differences in knowledge, CPR performance, and perceptions of the FC approach based on gender and CGPA. Additionally, Pearson correlation assessed relationships among knowledge, skills, and perception scores. A p-value of ≤ 0.05 was considered statistically significant.
Results
Demographic Characteristics of the Participants
A total of 177 participants were included in the study. Most of the participants were female (n = 151, 85.3%), while only 14.7% (n = 26) were male. In terms of academic performance, as indicated by CGPA, 8.5% (n = 15) of participants had a CGPA of less than 2, 24.3% (n = 43) had a CGPA between 1 and 3, 37.9% (n = 67) had a CGPA between 3.1 and 3.5, and 29.4% (n = 52) had a CGPA between 3.6 and 4. The mean age of the participants was 19.42 years (SD = 1.218), indicating a relatively young population (see Table 1).
Demographic Characteristics of the Participants n = 177.

CGPA = cumulative grade point average.
Effectiveness of Flipped Classroom Approach for Learning CPR
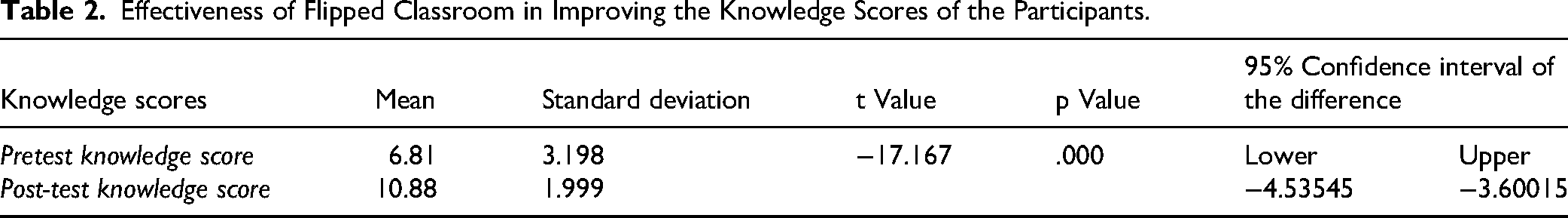
A paired sample t-test was conducted to evaluate the effectiveness of the FC approach in improving participants’ knowledge scores. The results indicated a statistically significant increase in knowledge scores from pretest (M = 6.81, SD = 3.20) to post-test (M = 10.88, SD = 2.00), t (176) = −17.17, p < 0.001. The 95% confidence interval for the mean difference ranged from −4.54 to −3.60, suggesting a meaningful improvement in knowledge following the intervention as reported in Table 2.
Effectiveness of Flipped Classroom in Improving the Knowledge Scores of the Participants.
Relationship Between the Knowledge Level, CPR Performance, and Perception of Flipped Classroom Effectiveness
A Pearson correlation analysis was conducted to examine the relationships between post-test knowledge scores, CPR performance scores, and participants’ perceptions of FC effectiveness. The analysis presented in Table 3 revealed a significant positive correlation between post-test knowledge scores and CPR performance scores (mean =9.01; SD = 1.042), r = 0.209, p = 0.05, indicating that higher knowledge scores were moderately associated with better CPR performance. There was no significant correlation between CPR performance scores and perception of FC effectiveness, r = −0.049, p = 0.519. Similarly, the correlation between post-test knowledge scores and perception of FC effectiveness was not statistically significant, r = 0.053, p = 0.482. These findings suggest that while the FC approach may enhance knowledge, this improvement is only modestly linked to CPR performance and not significantly associated with students’ perceptions of the method.
Correlation Between the Knowledge, CPR Performance, and Perception of Flipped Classroom Effectiveness.

**Correlation is significant at the 0.01 level (2-tailed).
CPR=cardiopulmonary resuscitation.
Comparison of Means of Knowledge Scores, CPR Performance Scores and Flipped Classroom Effectiveness Perception Scores With the Demographic Variables of the Participants
An independent samples t-test and one-way ANOVA were conducted to compare the mean scores across gender and cumulative GPA categories. A statistically significant difference was found only in the CPR performance scores based on gender. Female students scored significantly higher (M = 9.08, SD = 0.997) compared to male students (M = 8.58, SD = 1.21), t (175) = −2.30, p = 0.023, with a 95% confidence interval of the difference ranging from −0.934 to −0.071.
Perception of Effectiveness of Flipped Classroom Approach
Students’ perceptions of the FC teaching–learning approach were generally positive. As shown in Figure 1, the mean ratings across the survey items ranged from 3.9 to 4.3, indicating a favorable evaluation and overall appreciation of the FC model.
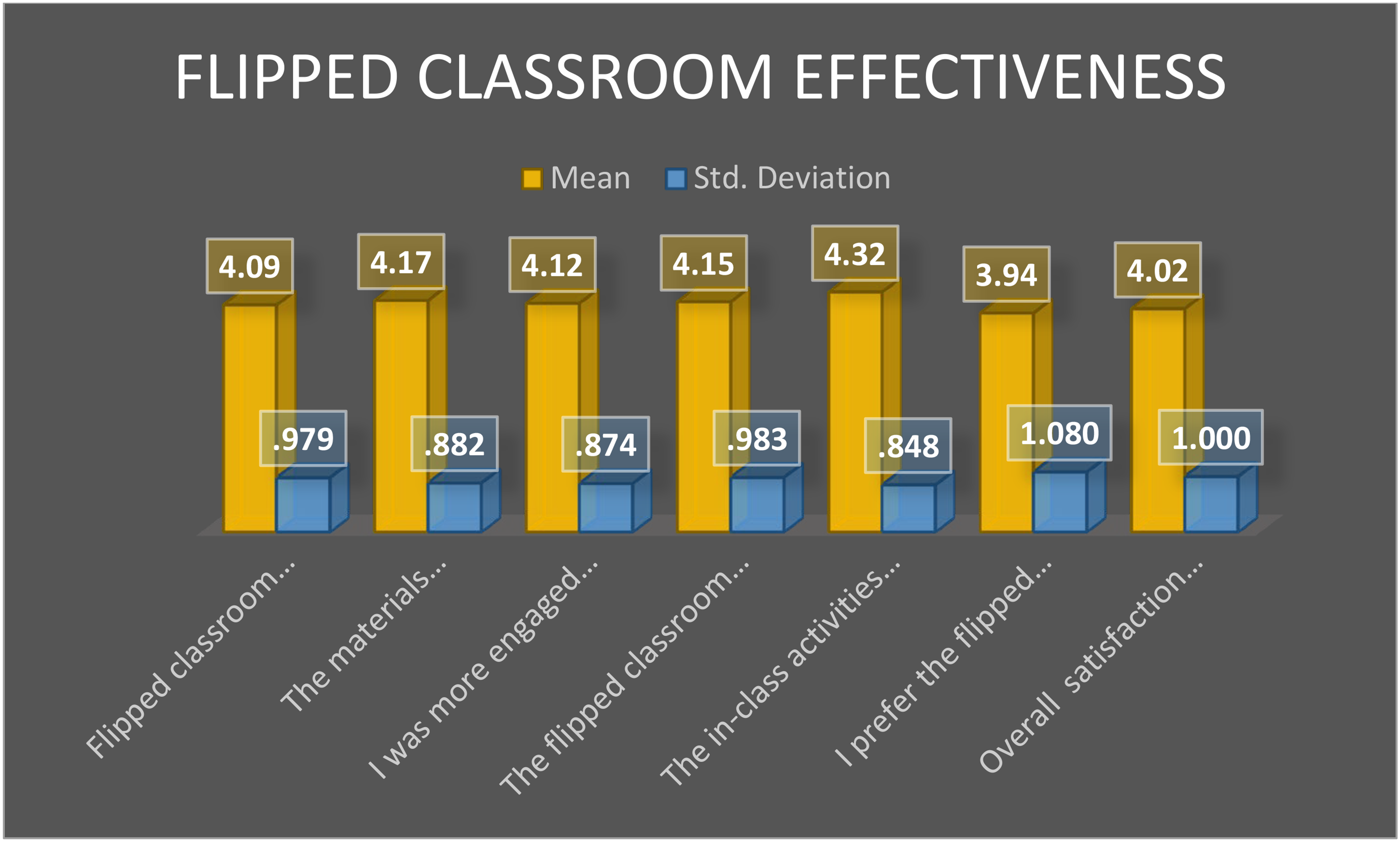
Mean SD scores of perceptions of flipped classroom effectiveness.
Discussion
This study assessed the effectiveness of a FC approach in enhancing CPR knowledge and skills among first-year nursing students at the University of Buraimi, Oman. The findings showed a significant improvement in students’ knowledge following the FC intervention, supporting the growing body of evidence favoring active and student-centered learning strategies in nursing education (Betihavas et al., 2016; Sun et al., 2025).
The significant gain in knowledge from pretest to post-test (from M = 6.81 to M = 10.88) suggests that the integration of online materials, such as AHA videos and PowerPoint lectures, with interactive in-class activities, contributed to deeper cognitive engagement. This aligns with regional efforts across the GCC countries—including Oman—to modernize health sciences education by adopting blended and flipped learning approaches to meet both local healthcare needs and international accreditation standards (Ashipala et al., 2024).
Although CPR knowledge and skill performance were positively correlated, the relationship was modest. This reflects earlier findings that while theoretical knowledge supports practice, mastery of psychomotor skills like CPR often requires repeated hands-on exposure and immediate feedback (Niu et al., 2023; Yang et al., 2019). In the context of Omani nursing education, simulation-based training and competency-focused curricula are still evolving, and more emphasis on practice sessions may be needed to strengthen skill retention.
Interestingly, gender was found to significantly influence CPR performance, with female students outperforming male peers (p = 0.023). While this echoes findings in other contexts where female nursing students tend to excel in structured assessments (Al-Hinai et al., 2021), in Oman this may also be influenced by broader cultural norms and gendered expectations in healthcare professions. Female students often represent the majority in nursing programs and may be more accustomed to collaborative learning environments, which align well with FC methodologies.
The significant gender imbalance in our sample (85.3% female) reflects the demographic composition of most nursing cohorts in Oman but raises questions about generalizability. Female predominance may have shaped peer interaction pattern, perception ratings, and the observed performance outcomes. Future research with more gender-balanced cohorts or stratified analyses is needed to validate whether these differences are context-specific or generalizable across nursing education programs.
No significant correlation was observed between CGPA and knowledge or performance scores, suggesting that the FC model benefits students regardless of prior academic achievement. This aligns with the inclusive goals of Oman's Vision 2040 in higher education, which advocates for equitable learning opportunities and the development of practical competencies across student populations (Ministry of Higher Education, Research and Innovation, Oman, 2020). The approach may thus serve as a valuable tool for bridging achievement gaps in large and diverse classrooms.
Although students reported generally positive perceptions of the FC, these perceptions were not significantly associated with their knowledge or performance outcomes. This supports the idea that while learner satisfaction is important, it may not always predict objective learning gains (Kim et al., 2021). It also suggests that faculty training in active learning facilitation and student preparation for blended learning may be crucial to maximize the benefits of such pedagogies in the Omani context.
This study adhered to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines to ensure comprehensive and transparent reporting.
Implication for Practice
The results of this study highlight the value of adopting the FC model in nursing education, particularly for critical life-saving skills such as CPR. Integrating FC into foundational courses can enhance knowledge acquisition and provide structured opportunities for active, hands-on learning, thereby improving both cognitive and psychomotor outcomes. The model proved beneficial across different academic performance levels, suggesting its potential to promote equity in learning. Faculty training in active learning facilitation and digital pedagogy is essential to maximize the benefits of FC and ensure sustainable implementation. At a broader level, the incorporation of FC aligns with international accreditation standards and national educational reforms in Oman and the GCC region, supporting the development of practice-ready nurses equipped to respond effectively in emergency situations and contribute to improved patient safety outcomes.
Strength and Limitations
The study is one of the first in Oman to evaluate the FC model in cardiopulmonary resuscitation (CPR) training among novice nursing students. The large sample size (N = 177) enhances the robustness of the findings and provides insights from the real classroom context, increasing ecological validity. Standardized instruments and reliability (Cronbach's alpha < 0.80) were employed, and skills were assessed by certified BLS instructors using AHA checklists, ensuring rigor in measurement.
This study used convenience sampling, limiting generalizability beyond the participating cohort. Additionally, the absence of a control group precludes causal conclusions. One notable limitation of this study is the significant gender imbalance in the sample, with 85.3% of participants being female. While this reflects the actual demographic distribution of nursing students at our institution, it may have influenced the collaborative dynamics of FC sessions and the gender-related differences observed in CPR performance. This imbalance may restrict the generalizability of findings to more gender-balanced nursing cohorts. Self-reported perceptions may be subject to bias, and skill performance was assessed immediately after instruction without long-term follow up to assess retention.
The study did not include baseline assessment of psychomotor (CPR skill) performance prior to the FC intervention, as participants were novice nursing students without previous exposure to BLS training. Consequently, only postintervention skill performance was measured, which may limit the ability to evaluate individual improvement over time.
Conclusion
The FC approach significantly improved CPR knowledge among novice Omani nursing students and demonstrated a moderate association with skill performance. Female students performed better than males, while academic background (CGPA) did not affect outcomes—supporting the model's equity potential. These findings support ongoing efforts in Oman and the broader GCC region to adopt evidence-based, learner-centered strategies in nursing education. Future studies should incorporate longitudinal follow-up and multi-institutional samples to strengthen the evidence base and guide national curriculum reforms.
Footnotes
Acknowledgments
The authors would thank College of Health Sciences at the University of Buraimi for their support and cooperation during the study. Special thanks to the faculty members who facilitated the simulation sessions and to the nursing students who voluntarily participated in the research.
Ethical Approval
Ethical approval was obtained from the ethics committee at the College of Health Sciences, University of Buraimi (Approval No: AY24-25COHS-086). Ethical Approval was obtained from the College Research and Ethics Committee (SQU/CON/DF.02/2017). All participants signed the informed consent.
Authors’ Contributions
JN was involved in conceptualization, methodology, investigation, data curation, data analysis, writing & supervision, project administration—original draft; RAR in conceptualization, methodology, investigation, data curation, data analysis, and writing—original draft; WKT in methodology, writing discussion, and review & editing; SG in conceptualization, methodology, data analysis, and writing—review & editing; RPS in conceptualization, methodology, and review & editing; HAAB in conceptualization and writing—review & editing; AMKAS in writing—review & editing; VS in methodology, writing introduction, review & editing, and submitting; and JK in methodology, and review and editing. All authors meet the authorship criteria and are in the agreement with the content of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
The date for this study is available on reasonable request.
