Abstract
Background
The novel coronavirus disease 2019 (COVID-19) pandemic restricted nursing practicums, which limited students’ clinical experience. In many programs, hands-on training was replaced with simulations, potentially affecting new nurses’ practical skills and decision-making. Consequently, preceptors guiding inexperienced nurses faced increased instructional burdens and challenges in ensuring safe and competent practice.
Objectives
This study aimed to examine how disruptions to clinical practicums due to the COVID-19 pandemic impacted the role performance of preceptors supporting newly graduated nurses in 2022 over time.
Methods
A longitudinal survey involving 426 preceptors from 39 hospitals in Hyogo Prefecture, Japan, was conducted three times in 2022 (June, September, and December). The main outcome assessed was preceptor role performance, which was measured using the 35-item Preceptor Role Self-Evaluation Scale. Secondary outcomes included participant demographics and perceived difficulties in guiding new nurses under COVID-19-related practicum restrictions, and they were assessed on a 5-point scale. Ethical and institutional approval was obtained, and the surveys were distributed online via QR codes and email. Participation was voluntary and anonymous, with responses linked over time using the participants’ email addresses.
Results and Conclusion
Seventy-six preceptors (six males and 70 females; 17.8% response rate) completed all three surveys. In June, those reporting higher instructional difficulty demonstrated significantly higher role performance, particularly in planning, evaluation, accident prevention, and cooperation between ward staff and patients. By September and December, their ability to cooperate was significantly better. These findings indicate that preceptors who perceived greater difficulty initially improved their performance, which highlights the heightened instructional demands caused by COVID-19 disruptions to clinical training.
Introduction
The first case of pneumonia caused by COVID-19 was reported in Wuhan City, Hubei Province, China, in December 2019. The infection rapidly spread, and in January 2020, the World Health Organization (WHO, 2025) declared a Public Health Emergency of International Concern (PHEIC). This unprecedented pandemic severely impacted not only healthcare settings but also nursing education.
Clinical practicums—core components of basic nursing education involving practical learning activities conducted in cooperation with hospitals and community healthcare institutions—faced significant challenges. From an infection control standpoint, many healthcare facilities suspended or restricted student placements. Consequently, nursing universities across Japan were forced to drastically revise their curricula, including canceling or shortening practicums and shifting to simulation-based training on campuses (Japan Association of Nursing Programs in Universities, 2021; Sugawara et al., 2020).
Nursing practicums were vital learning opportunities designed to help students integrate the knowledge gained from general education and foundational specialized subjects with nursing-specific knowledge, skills, and attitudes acquired in professional courses, thereby fostering the ability to apply these comprehensively in practice (Ministry of Education, Culture, Sports, Science and Technology, 2019). A lack of clinical practicum experience raises concerns about the potential impact on the development of clinical competencies and decision-making skills essential for newly graduated nurses.
Review of Literature
Ohue and Shiragami (2023) demonstrated that students who completed even 1 week of on-site practicum under COVID-19 restrictions showed superior learning in nursing problem-solving behaviors, such as individualized problem-solving and psychological support, compared with those who received only simulation-based training. Conversely, Palese et al. (2022) found no significant differences in job role performance or basic nursing skills between newly graduated nurses who attended restricted educational programs during the pandemic and those who graduated without such restrictions, a result suggesting that the effects on practical nursing abilities may not be uniform. Ohue et al. (2025) further indicated that the reduction in clinical practicums and the transition to campus-based training due to COVID-19 had led to a decline in practical nursing skills among new graduates, highlighting the ongoing challenge of ensuring both the quality and quantity of clinical experience.
Collectively, these findings suggested that the effects of the COVID-19-related practicum disruptions vary across contexts and outcomes. Newly graduated nurses entering clinical practice in 2022 often lacked sufficient clinical experience and potentially faced difficulties in skill acquisition and workplace adaptation. Supporting these nurses requires greater individualization and flexibility, which likely increases the instructional burden on preceptors and educators.
Although prior studies have addressed the challenges newly graduated nurses face during the pandemic, research on how these challenges affect preceptors’ instructional roles over time remains scarce. Specifically, the longitudinal effect of perceived instructional difficulty on preceptor role performance was poorly understood. Clarifying the specific difficulties encountered by preceptors and their impact on role performance provided foundational insights for improving the education of novice nurses. Notably, guidance for inexperienced nurses affected preceptors’ mental health, and experiencing mental health difficulties was considered indicative of excessive instructional burden (Ohue & Ohue, 2025).
This study addresses these gaps by longitudinally examining the relationship between preceptors’ perceived instructional difficulties and their role performance across three survey periods (June, September, and December 2022). By focusing on preceptors who supported newly graduated nurses with limited clinical practicum experience due to COVID-19, this study aimed to inform improvements in educational support systems for novice nurses when practical experience was constrained.
Hypotheses
Preceptors who perceive higher instructional difficulty exhibit higher self-evaluated role performance scores.
The relationship between perceived instructional difficulty and role performance changes with time in the three survey periods.
Methods
Study Design and Participants
This study employed a quantitative research design utilizing a longitudinal survey conducted at three time points: June, September, and December 2022.
The study targeted 426 preceptors involved with newly graduated nurses in 2022 at 39 hospitals in Hyogo Prefecture, Japan, all of which had provided consent to participate.
Survey Period
First survey: June 1 to June 30, 2022
Second survey: September 1 to September 30, 2022
Third survey: December 1 to December 31, 2022
The survey was conducted at three time points to capture changes in the preceptors’ perceived instructional difficulty, role performance, and related outcomes over time. Using a longitudinal design, this study aims to identify temporal trends and potential causal relationships that could not be observed in a single cross-sectional survey. This approach allows for a more comprehensive understanding of how preceptors’ experiences and challenges evolve and provides insights into the most effective timing and type of support.
Sampling Method and Sample Size
The participants were hospital nurses serving as preceptors for newly graduated nurses in 2022 at 39 hospitals in Hyogo Prefecture, Japan, all of whom provided consent to participate in the study. First, facility administrators were contacted, and eligible nurses were invited to participate through purposive sampling. The sample size was calculated using G*Power 3.1 software. Assuming a medium effect size (f = 0.25), α = .05, and power (1–β) = 0.80, the minimum required sample size was 52. The target sample size was increased by 30% to compensate for potential nonresponses or incomplete data, resulting in a minimum required sample size of 68 participants. A total of 76 participants, six men (7.9%) and 70 women (92.1%), responded to all three survey periods (June, September, and December), yielding a final response rate of 17.8%.
Inclusion Criteria
Registered nurses are currently working as preceptors in hospital settings.
Nurses are responsible for guiding newly graduated nurses during on-the-job training.
Nurses who provided informed consent to participate in the study.
Exclusion Criteria
Nurses who were on long-term leave (e.g., maternity or medical leave) during the study period.
Nurses with < 6 months of experience as a preceptor.
Individuals who did not complete the survey at all three time points.
Data Collection Instruments
Primary Outcome
The Preceptor Role Self-Evaluation Scale, developed by Yoshitomi and Funashima (2009), was employed to assess the role performance of nurses instructing new graduates. This scale comprises 35 items across seven subscales designed to comprehensively evaluate multiple dimensions of preceptor role performance. The seven subscales include:
Collecting diverse information about new nurses and developing individualized instructional plans reflecting their uniqueness. Providing instruction and evaluation in accordance with the instructional plan. Alleviating the new nurse's tension and compensating for deficiencies. Offering explanations of problematic phenomena and psychological support to enable continued work by new nurses. Monitoring new nurses’ conditions while aiming to achieve instructional goals and prevent accidents. Continuing instruction with cooperation from ward nurses and patients. Continuously performing duties other than new nurse instruction.
The scale's reliability and validity were confirmed at the time of development, establishing its utility as a psychometric tool. Each item is rated on a 4-point Likert scale from 1 point (hardly applies) to 4 points (fully applies), with higher scores indicating higher self-assessed role performance as a preceptor.
Secondary Outcome
The survey collected data on participants’ demographics, including gender, age, department, educational background, qualifications, and work format. Participants were asked to rate their perceived difficulties in instructing newly graduated nurses who had received insufficient clinical practicum experience due to COVID-19 restrictions (hereafter referred to as “perceived difficulty”) using a 5-point Likert scale ranging from 1 point (not difficult at all) to 5 points (very difficult).
Procedures
The survey was administered using a paid version of Google Forms, with questionnaires and QR codes generated accordingly. After obtaining ethical approval, the study's purpose was explained both verbally and in writing to the directors of nursing at participating hospitals, and their consent was secured. Upon approval, the questionnaire and explanatory documents with QR codes were sent to each hospital's nursing department. Nurse managers then explained the study to eligible nurses and distributed the survey requests and forms. Nurses consenting to participate accessed the questionnaire via the QR code.
Responses were collected anonymously at three separate time points (June, September, and December) via the same questionnaire. The first response was submitted through paper-distributed QR codes, while for the second and third surveys, Google Forms links were sent via BCC email to protect privacy. Longitudinal linkage of responses was achieved through voluntarily provided email addresses, which were deleted after study completion.
Ethical Considerations
This study was approved by the Research Ethics Committee. Written requests for participation were sent to facility administrators, and their consent was obtained prior to initiating the study. Individual participants received detailed written explanations of the study objectives and procedures, and the study commenced after informed consent was obtained. The explanatory documents emphasized that participation was entirely voluntary, that participants could withdraw at any time without penalty, and that the data would be used exclusively for research purposes. All data were coded and statistically analyzed to ensure confidentiality and anonymity, and no personally identifiable information was disclosed. The authors declare no conflict of interest related to this study.
Data Analysis
Descriptive statistics (counts and percentages) were calculated for participant attributes.
Regarding perceived difficulty, responses of “not difficult at all,” “not very difficult,” and “neutral” were categorized as the low-difficulty group, while “somewhat difficult” and “very difficult” responses were classified as the high-difficulty group.
Normality was confirmed, and an independent t-test was conducted to compare Preceptor Role Self-Evaluation Scale scores between the low- and high-difficulty groups at each survey period. The significance level was set at 5%. IBM SPSS Statistics 26 was used for all analyses.
Results
Demographic Factors (Table 1)
A total of 76 participants responded to all three survey periods (June, September, and December), comprising six males (7.9%) and 70 females (92.1%), with a response rate of 17.8%. The majority of participants worked in general wards (n = 51, 67.1%), followed by community-based integrated care wards (n = 8, 10.5%). Intensive care units and psychiatric wards each accounted for five participants (6.6%), while obstetrics and gynecology had two participants (2.6%). One participant each (1.3%) worked in pediatrics, operating rooms, and outpatient departments. Two participants (2.6%) were classified as “other.”
Regarding educational background, the largest group consisted of university graduates (n = 39, 51.3%), followed by vocational school graduates (n = 31, 40.8%), graduate school graduates (n = 4, 5.3%), and junior college graduates (n = 2, 2.6%). In terms of qualifications, most participants were registered nurses (n = 71, 93.4%), with a small number also holding public health nurse (n = 3, 3.9%) or midwifery licenses (n = 2, 2.6%). Regarding work shifts, the majority worked in a two-shift system (n = 60, 78.9%), while day-shift-only and three-shift system workers each accounted for eight participants (10.5%).
Basic Attributes of Participants.

Preceptors’ Role Performance in On-the-Job Training of New Graduate Nurses (Table 2)
The analysis included 76 participants (six males and 70 females) who responded to all three surveys (June, September, and December), with a response rate of 17.8%. Regarding perceived instructional difficulty, two participants (2.6%) responded “not at all difficult,” 10 (13.2%) “not very difficult,” 16 (21.1%) “neutral,” 40 (52.6%) “somewhat difficult,” and seven (9.2%) “very difficult.”
Preceptors’ Role Performance in On-the-Job Training of New Graduate Nurses.

Effects of Perceived Difficulty on Role Performance Scores Across Survey Periods (Table 3)
The relationship between perceived instructional difficulties and preceptor role performance was examined by categorizing participants into a low-difficulty group (“not at all difficult,” “not very difficult,” and “neutral”) and a high-difficulty group (“somewhat difficult” and “very difficult”). Independent t-tests were employed to compare the Self-Evaluation Scale scores between the groups at the three time points.
Effects of Perceived Difficulty on Role Performance Scores Across Survey Periods.
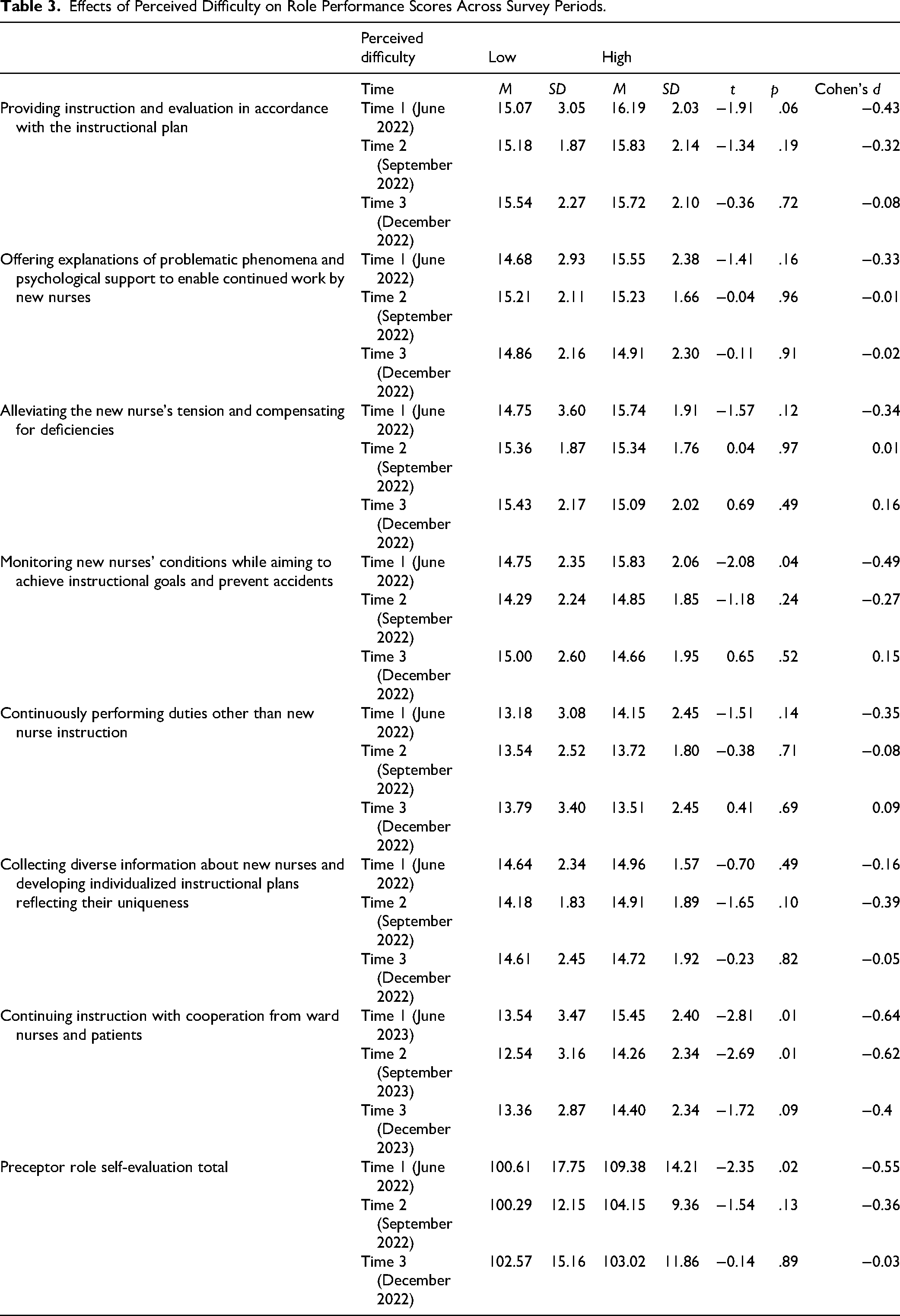
Overall, participants reporting significant difficulties tended to have slightly higher mean scores on most role performance subscales compared to those reporting slight difficulties, although most differences were not statistically significant. Significant or near-significant differences were observed in specific domains and time points as follows.
Monitoring new nurses’ conditions: high-difficulty group scored significantly higher at Time 1 (M = 15.83 vs. 14.75, t = −2.08, p = .04, d = −0.49), with no significant differences during later periods.
Continuing instruction with co-operation from ward nurses and patients showed that high-difficulty group scored significantly higher at Time 1 (M = 15.45 vs. 13.54, t = −2.81, p = .01, d = −0.64) and Time 2 (M = 14.26 vs. 12.54, t = −2.69, p = .01, d = −0.62); at Time 3, the difference approached significance (t = −1.72, p = .09).
With regard to total preceptor role self-evaluation score, the high-difficulty group scored significantly higher at Time 1 (M = 109.38 vs. 100.61, t = −2.35, p = .02, d = −0.55); no significant differences were observed at Time 2 or 3.
For other subscales, including providing instruction according to the plan, alleviating the tension of novice nurses, explaining problematic phenomena, collecting diverse information, and performing duties beyond instruction, the differences between the groups were generally small and nonsignificant across the survey periods.
Discussion
This study longitudinally analyzed preceptors’ perceptions of instructional difficulty while training newly graduated nurses and examined how these perceptions related to their role performance at three time points (June, September, and December). The findings revealed time-specific patterns in the relationship between perceived difficulty and self-evaluated preceptor role performance. Moreover, the results suggest that the COVID-19 pandemic significantly impacted the structure of novice nurse education, indirectly influencing preceptors’ role performance.
At the initial time point in June, the high-difficulty group scored significantly higher on the overall Preceptor Role Self-Evaluation Scale and on several subscales. Notably, elevated scores appeared in subscales related to practical and organizational support, including “providing instruction and evaluation based on instructional plans,” “balancing understanding of the new nurse's condition with accident prevention,” and “continuing guidance with cooperation from ward nurses and patients.” These results highlight a proactive attitude among preceptors who, despite experiencing instructional difficulties, actively engaged in supporting new nurses.
A key contextual factor underlying these findings is the reduction or suspension of clinical practicums due to the COVID-19 pandemic. As a result, many newly graduated nurses entered the workforce without sufficient clinical experience. Ohue et al. (2025) reported that the shift to online or limited practicum settings hindered the development of practical nursing competencies, particularly in areas such as information gathering, identifying nursing problems, facilitating communication, and providing individualized support. Although improvements were observed in psychological support, this variation in competency placed greater demands on preceptors, who were expected to provide more comprehensive, foundational instruction—ultimately increasing their instructional burden.
Ota and Masuda (2017) noted that insufficient preparatory education and support systems in academic settings can hinder preceptors’ ability to fulfill their roles. The findings of the present study align with this perspective. Notably, at the September and December time points, only the subscale “continuing guidance with cooperation from ward nurses and patients” showed significantly higher scores in the high-difficulty group. This suggests a shift in the preceptor's role—from direct technical instruction to more indirect, team-based support—as new nurses gradually gained independence. Preceptors who continued to experience difficulties during this later phase appeared to maintain a strong sense of responsibility and demonstrated active collaboration with other professionals, reflected in their higher self-evaluations.
Furthermore, the study found that experiencing difficulty did not necessarily correlate with lower self-evaluation scores. In fact, preceptors reporting higher difficulty often evaluated their role performance more favorably. Hirano and Koyama (2018) reported that new preceptors, while overcoming various difficulties, developed a greater sense of professional responsibility and grew through consultation and support. Similarly, Yamakawa and Miyazato (2023) showed that despite challenges such as balancing clinical duties, anxiety regarding technical skills, and a lack of support, preceptors often acquired new insights and experienced professional growth.
Ito et al. (2021) also indicated that nurses serving as preceptors for the first time experienced self-doubt and difficulty managing emotions within the first three months of their role. However, they also began to recognize the joy of teaching and personal transformation. By the sixth month, many had found a sense of fulfillment in exploring instructional methods and expressed appreciation for the support provided by their departments. These findings suggest that preceptors, while grappling with conflicting emotions, cultivate a sense of affirmation and purpose in their roles. The longitudinal nature of the current study supports this developmental process, indicating that experiencing difficulties may ultimately foster self-efficacy and professional growth.
Livingstone (2024) emphasized the complexity of clinical learning environments and highlighted how the quality of the relationship between preceptors and nursing students significantly affects students’ learning outcomes and professional development. Nevertheless, several challenges persist, including a lack of formal recognition, structured training, and institutional support for preceptors. These deficiencies can compromise the quality of education and increase the psychological burden on preceptors. Particularly in demanding settings—such as those involving critically ill patients or strict time constraints—systematic and sustained support for preceptors is internationally recognized as essential.
Therefore, experiencing instructional difficulties should not be viewed solely as a negative phenomenon. Rather, it may present opportunities for professional development and enhanced practical competence. Instead of attributing such difficulties to individual capabilities or effort, it is advisable to address them as shared organizational challenges. Institutions should establish support systems that reflect the stages of the instructional process—for example, emphasizing individualized plans and safety during the early phase of clinical instruction, and transitioning toward team-based, sustained support in later stages.
Strengths and Limitations
This study highlighted the importance of creating an educational environment in which preceptors could stably perform their roles and continue to grow professionally. To achieve this, multifaceted support measures were required, including opportunities to acquire instructional knowledge and skills, workload adjustments, psychological support, and enhanced inter-professional collaboration. These findings provided valuable insights into the structure of preceptor support systems and offered foundational knowledge for enhancing the quality of training for newly graduated nurses.
However, this study was limited to nurses from a single prefecture, which may restrict the generalizability of our findings. Future studies should include participants from multiple regions to obtain more comprehensive data. Additionally, it was essential to develop programs that provide targeted support not only for newly graduated nurses but also for preceptors who guide them, ensuring sustainable professional development and effective mentoring.
Another potential limitation was the low response rate of 17.8%, which might have introduced response bias. This low rate could be attributed to factors such as survey timing, high participant workload, and survey fatigue. Although the characteristics of the respondents were generally comparable with those of the target population in terms of key demographics, caution was advised when generalizing the findings.
Implications for Practice
These findings highlight the need for hospitals to provide structured support for preceptors, particularly during the early period of newly graduated nurses’ training, when instructional demands are greatest. Continuous monitoring of preceptor workload and stress levels is essential, as the heightened role performance observed under perceived difficulty may not be sustainable over time. Institutions should consider implementing systematic mentoring programs, refresher training, and psychological support to help preceptors adapt effectively. Strengthening the support system for preceptors may also indirectly enhance the professional development and retention of newly graduated nurses in the post-pandemic context.
Conclusion
This study examined the relationship between perceived instructional difficulty and role performance among 76 preceptors responsible for the clinical training of newly graduated nurses, measured at three time points: June, September, and December. The results showed that, in June, preceptors reporting higher instructional difficulty tended to rate their overall role performance more highly, particularly in areas such as practical instruction, safety management, and collaborative support with ward staff and patients. By September and December, only the subscale “continuing guidance with cooperation from ward nurses and patients” remained significantly higher among those experiencing greater difficulty, indicating a shift in instructional challenges over time.
These findings highlight that changes in the educational environment, such as the suspension or reduction of clinical practicums due to COVID-19, have affected not only newly graduated nurses but also the preceptors guiding them. Importantly, perceived instructional difficulty did not equate to lower role performance. Rather, preceptors who experienced greater difficulty demonstrated stronger professional responsibility and proactive engagement in addressing challenges. From a health policy perspective, these results underscore the need for structured support systems for preceptors, including training, workload management, psychological support, and interprofessional collaboration, to strengthen the nursing workforce development and ensure high-quality patient care.
Footnotes
Acknowledgements
The author would like to express sincere gratitude to the co-researchers for their cooperation and to all the participants for their contributions to this study. Their support and participation were essential for the completion of this research.
Ethical Consideration
This study was conducted after obtaining approval from the Ethics Review Committee of the author-affiliated university. This study was conducted with approval from the Hyogo University Research Ethics Committee (Approval No. 21011).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by JSPS Grant-in-Aid for Scientific Research (KAKENHI) (24K13590).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
