Abstract
Background
The transition of nursing education from traditional methods to more advanced approaches is crucial for adequately preparing students to deliver competent care in tertiary care centers. Moreover, clinical faculty in nursing plays a key role in guiding nursing students through their clinical training in various healthcare settings.
Purpose
This study aims to describe the perceptions of undergraduate nursing students regarding the effectiveness of the learning environment and clinical teaching in clinical areas across various countries.
Methods
The study, conducted using a descriptive, cross-sectional research design, gathered data from 215 nursing students using the Clinical Learning Environment Inventory and Clinical Teaching Effectiveness Instrument. Data analysis included frequencies, percentages, mean, standard deviation, t-tests, analysis of variance, and correlation assessments to comprehend the impact of clinical teaching and learning environments.
Results
Nursing students’ perceptions of the clinical learning environment produced mean scores between 2.03 and 3.38 on a scale from 1 to 4, resulting in an overall mean score of 2.72 across 42 items. This indicates a general satisfaction with their clinical learning experiences. Regarding effective clinical teaching, the mean student responses varied from 3.02 to 3.40 out of a possible 5 points, with a total mean of 3.22. The study revealed notable correlations in the context of effective clinical teaching, particularly with demographic variables and the clinical learning environment. Specifically, a significant correlation with age (r = .177, p = .009) and the clinical learning environment (r = .572, p < .001) was identified.
Conclusion
The study concludes that students expressed overall satisfaction with their clinical learning experiences. They recognized the importance of participating in clinical training, fulfilling clinical responsibilities for assigned patients, exerting extra effort for learning, receiving support from preceptors in clinical settings, and being attentive to communications from staff. The collaboration between clinical preceptors and academic nursing lecturers is crucial in providing a positive learning environment for students to complete clinical tasks effectively.
Background
Nursing tudents increasingly seek clinical environments that foster the development of skills necessary for integrating theoretical knowledge into effective clinical practice (Hagqvist et al., 2020; Jamshidi et al., 2016). Various clinical areas provide opportunities for students to acquire essential skills, preparing them for clinical reasoning and professional development (Kavanagh & Szweda, 2017). While many nursing programs employ simulations to effectively facilitate learning, in some programs, simulation use is limited or unavailable, making real clinical sites the primary learning environment (Roh et al., 2019).
Literature Review
The clinical environment is a key component in nursing education, aiding students in engaging in authentic practice and enhancing the effectiveness of clinical teaching (Mackavey & Cron, 2019; Wu et al., 2020). Clinical experiences, recognized internationally as an essential component of nursing education, significantly shape both the teaching process and the learning outcomes of students, as evidenced by numerous studies (Clarke et al., 2016; Rafati et al., 2017; Rodríguez-García, 2021). Clinical settings offer students the opportunity to not only develop practical skills but also gain an understanding of the fundamental principles governing healthcare system processes (Bastable, 2021; Rafati et al., 2017). In these settings, nursing students typically work alongside a multidisciplinary healthcare team, which underscores the need for strong communication skills essential for professional nursing practice (Denneson et al., 2017; Ellis & Sevdalis, 2019). These environments are conducive to fostering therapeutic communication, thereby nurturing positive and trusting relationships during the training period (Abdolrahimi et al., 2017; Torous & Hsin, 2018). Effective communication facilitates essential interactions among students, clinical instructors, nurses, and other healthcare team members, enabling them to work collaboratively toward mutual goals and ensure optimal outcomes (Bastable, 2021; Rafati et al., 2017).
Clinical instructors are pivotal in fostering the development of students’ professional skills, emphasizing practical skill-building rather than solely theoretical knowledge acquisition (Harden & Laidlaw, 2020; Jamshidi et al., 2016). The Clinical Teaching Effectiveness Instrument (CTEI; Gallivan, 2022) has been established as an effective measure for assessing the performance of clinical educators. This tool is also instrumental in helping healthcare educators effectively assign teaching roles, foster competency development, and deliver impactful feedback for enhancement Glatz et al. (2017) and Yang et al. (2018). Nursing students, particularly at the onset of their clinical training in hospitals, often experience significant stress. Thus, understanding their perceptions of the effectiveness of the clinical teaching environment is vital to positively influencing their knowledge acquisition, safe training practices, and professional growth. When designing an optimal clinical teaching environment, it is essential to consider various factors, including curriculum objectives, the learning environment, clinical instructor experience, and the individual characteristics of students (Soroush et al., 2021). Nursing educators need to recognize the importance of exploring these elements through students’ perceptions, which can significantly impact their achievement and performance levels. Conducting these investigations is essential for equipping nursing students with the skills and knowledge needed to seamlessly integrate into healthcare systems at an early stage in their careers. This study also enables educational systems to highlight the effectiveness of clinical teaching environments and conduct further research aimed at enhancing student engagement and clinical teaching.
To the best of our knowledge, no published studies have simultaneously explored the perceptions of effective teaching environments among undergraduate nursing students in clinical settings across multiple countries. Our research aims to unravel the views of these students in diverse national contexts. The findings are intended to guide nurse educators in formulating strategies that will strengthen these educational aspects and enrich the overall clinical teaching environment.
Research Questions
To further explore the landscape of nursing education, the following research questions were formulated:
What are undergraduate nursing students’ perceptions of the effectiveness of the learning environment in clinical areas across different countries? This question seeks to understand students’ views on the quality and impact of the clinical settings where they receive their practical training. How do undergraduate nursing students perceive the effectiveness of clinical teaching in different countries? This inquiry focuses on students’ opinions about the quality and impact of the teaching they receive during their clinical training in various geographical locations. What is the relationship between students’ perceptions of effective clinical teaching and demographic variables, as well as the clinical learning environment? This question aims to examine the connections between students’ perceptions of effective clinical teaching and the influence of their demographic backgrounds, as well as the features of the clinical learning environments they encounter.
Methodology
Study Design
The study was conducted using a descriptive, cross-sectional design from June 2020 to December 2021.
Sample and Setting
Questionnaires were distributed to undergraduate nursing students from various nursing schools across four countries. Participants were drawn from Sultan Qaboos University in Oman, Al al-Bayt University, Jordan University of Science and Technology, and Zarqa University in Jordan, as well as Taibah University in the Kingdom of Saudi Arabia and Al-Quds University in Palestine, specifically from their respective faculties of nursing. The required sample size was determined using a rule-of-thumb formula, calculated as 22 × 10 + 50, resulting in a minimum of 270 nursing students (Ab Latif & Nor, 2019; Breytenbach et al., 2017). Those deemed eligible to participate in this study were requested to complete the questionnaires. Of these, 215 students submitted their responses, a number sufficient for the intended analysis.
Eligible participants met the following criteria: (a) enrollment as a nursing student in the Adult Health Nursing (I) course; (b) voluntary expression of intent to participate; and (c) ability to read and understand English. Both bridging and regular students were included in the study.
Study Instruments
The self-reported questionnaire comprised three parts: (a) demographic characteristics, (b) Clinical Learning Environment Inventory (CLEI), and (c) CTEI. Demographic data included age, gender, nursing program type (bridging or regular students), year of study, country, nursing school, area of practice, accommodation, and GPA.
The CLEI (D. Chan, 2001, 2002; D. Chan, 2003) was utilized to measure nursing students’ perceptions of their clinical learning environment. This instrument assesses three fundamental dimensions of human environments: the relational aspect, personal development, and system maintenance. Specifically, the CLEI assesses perceptions in real clinical learning environments and categorizes students’ viewpoints across six areas concerning their psycho-social aspects during clinical practicums. The inventory comprises 42 items that characterize aspects of clinical experience, with seven items for each of the five scales. The first two scales address personalization and student involvement; the subsequent two focus on teachers’ innovation and task orientation; and the fifth measures individualization. Additionally, a student clinical learning experience satisfaction scale, introduced by D. Chan (2001), evaluates overall student satisfaction.
Items in the CLEI were scored using a 4-point Likert scale, with responses ranging from 4 (strongly agree) to 1 (strongly disagree). Selected questions are scored in reverse order to ensure consistency, with all negative items adjusted to reflect the same directional interpretation. The CLEI has been applied in various studies across different countries, yielding comparable results that highlight its suitability for diverse cultural contexts (Ghahremani et al., 2022; Wong & Bressington, 2021). The instrument's validity has been established in previous research, with Cronbach's alpha values ranging from 0.6 to 0.88 (D. Chan, 2002; Wong & Bressington, 2021). An Iranian study reported Cronbach's alpha values ranging from 0.47 to 0.74, with higher values (0.63–0.76) noted in specific domains when the population was segmented by year of study (Yazdankhahfard et al., 2020). In the current study, the calculated Cronbach's alpha for the CLEI is 0.65. Permission to use the scales was sought from the primary authors.
The CTEI is a vital tool for gauging students’ perspectives on the performance of clinical educators. This 15-item self-report questionnaire enables students to evaluate factors that either facilitate or impede their clinical learning experiences. The CTEI's reliability has been established in numerous studies, with Cronbach's alpha levels ranging from 0.74 to 0.95, indicating high internal consistency (D. Chan, 2001, 2002; D. S. Chan, 2003). Additional research has also reflected this high level of internal consistency, as evidenced by a Cronbach's alpha of 0.97 (Gallivan, 2019; Smith, 2020). Moreover, the CTEI's construct validity, which ensures its precision in measuring clinical educators’ performance, has been validated by research, including Dunn et al.'s (2020) study. In the current study, the CTEI achieved a Cronbach's alpha of 0.80.
Respondents rated each item on the CTEI using a 5-point Likert scale, which ranged from 1 (never/poor) to 5 (always/superb), with an additional option for “don't know/not applicable.” This scoring approach allows for a comprehensive assessment of each item. The mean scores from all 15 items were then calculated to determine an average rating for each student. Both the CLEI and CTEI were analyzed based on the mean scores obtained for each item, enabling a nuanced interpretation of the data collected.
Data Collection Procedure
Communication letters outlining the study's details, including its title, purpose, nature, and an overview of potential benefits and risks, were sent to all nursing students at the selected sites. Following the identification of potential participants who met the eligibility criteria, written consent was obtained for their participation in the study.
To administer the questionnaires, a research assistant not affiliated with the faculty was employed to avoid potential coercion or bias in student responses. This assistant, possessing at least a BSc degree in nursing, distributed the questionnaires during the students’ free time. Number-coded forms were stored securely to ensure confidentiality and kept separate from the corresponding number-coded files. Hard copy files were kept in a locked cabinet accessible only to the principal investigator, safeguarding the data from unauthorized disclosure.
Data analysis was conducted using SPSS version 23. Statistical procedures included calculating frequencies, means, and standard deviations for demographic variables and students’ perceptions of effective clinical teaching and learning environments. The study employed t- tests and one-way analysis of variance (ANOVA) to assess the effectiveness of clinical teaching in relation to demographic variables with careful consideration of all underlying assumptions. Additionally, Pearson correlation analysis was utilized to examine the relationships between effective clinical teaching, interval-level variables, and the clinical learning environment.
Ethical Considerations
Ethical approval was granted by the Research Ethics Committee at each participating institution. After receiving these approvals, data collection was initiated. At the outset of participation, the following critical information was disclosed to the participants: (a) A clear outline of their rights as participants; (b) an explanation of the potential benefits and/or risks associated with their involvement in the study; (c) detailed information about the nature of the study; (d) assurance of participant anonymity; (e) the option to withdraw from the study at any point without repercussions; and (f) a commitment to maintaining confidentiality throughout the research process.
Researchers secured informed consent from each participant, emphasizing the voluntary nature of participation, and ensuring that the decision to participate or decline would have no impact on their academic evaluation. The research assistants then distributed the questionnaires to the participants, who completed them and returned them upon completion.
Results
Participant Demographics
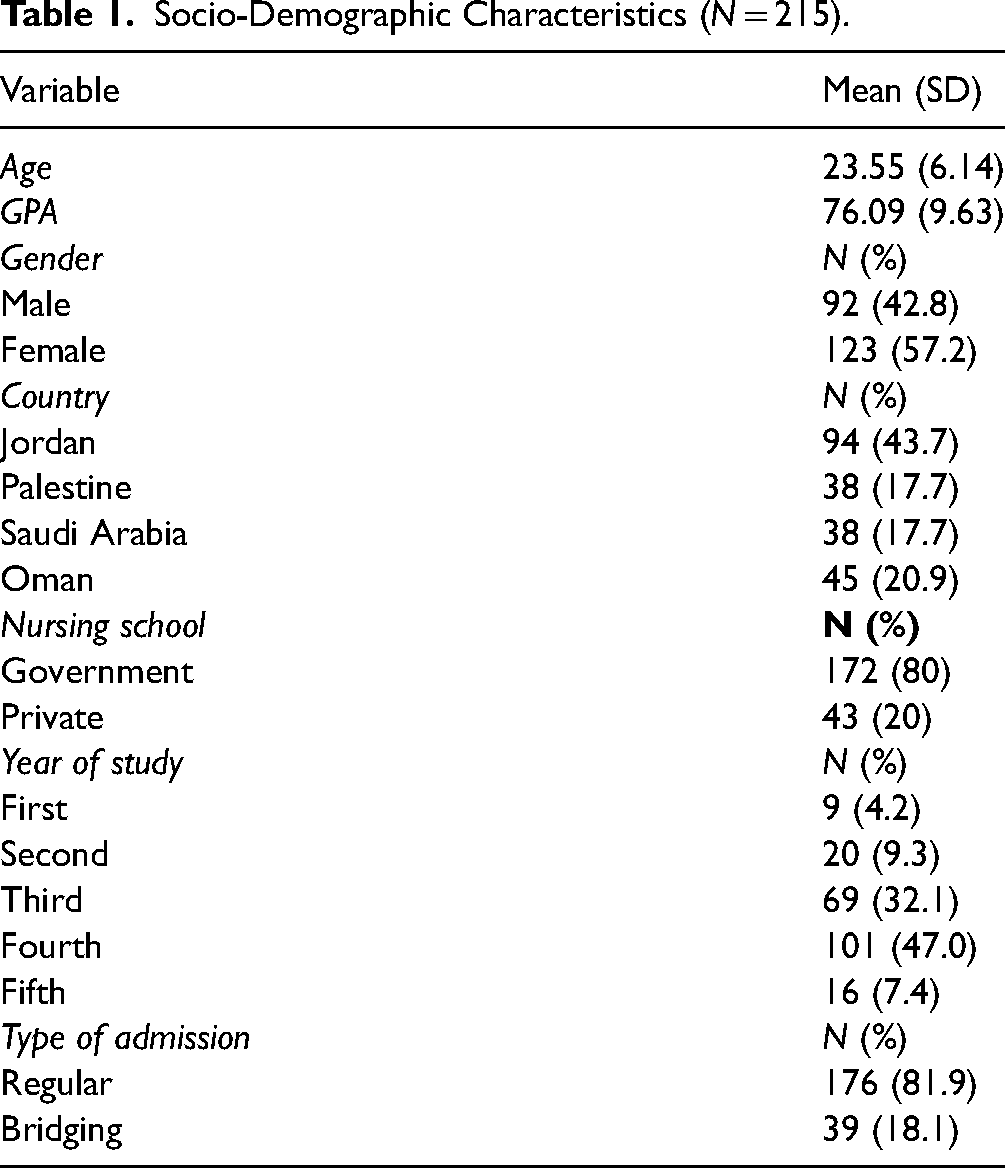
The study encompassed a total of 215 students, whose demographic characteristics are detailed in Table 1. Of these, 57.2% were female, with an average age of 23.55 years (SD = 6.14) and a GPA of 76.09 (SD = 9.63) out of 100. Most of the students (43.7%) were Jordanians, enrolled in governmental universities (80%), and in their fourth year of study (47%).
Socio-Demographic Characteristics (N = 215).
Nursing Students’ Perceptions of the Learning Environment
Students’ perceptions of their clinical learning environment were assessed using 42 items, as detailed in Table 2. Responses were recorded on a Likert scale from 4 (strongly agree) to 1 (strongly disagree). Mean scores ranged from 2.03 to 3.38, resulting in an overall mean of 2.72. Notably, most participants (2.03) disagreed with the assertion that diverse teaching methods were seldom employed. Conversely, the data indicated a strong agreement among the participants (3.38) regarding their significant investment of effort in clinical learning activities.
Students’ Perception of Their Clinical Learning Environment.
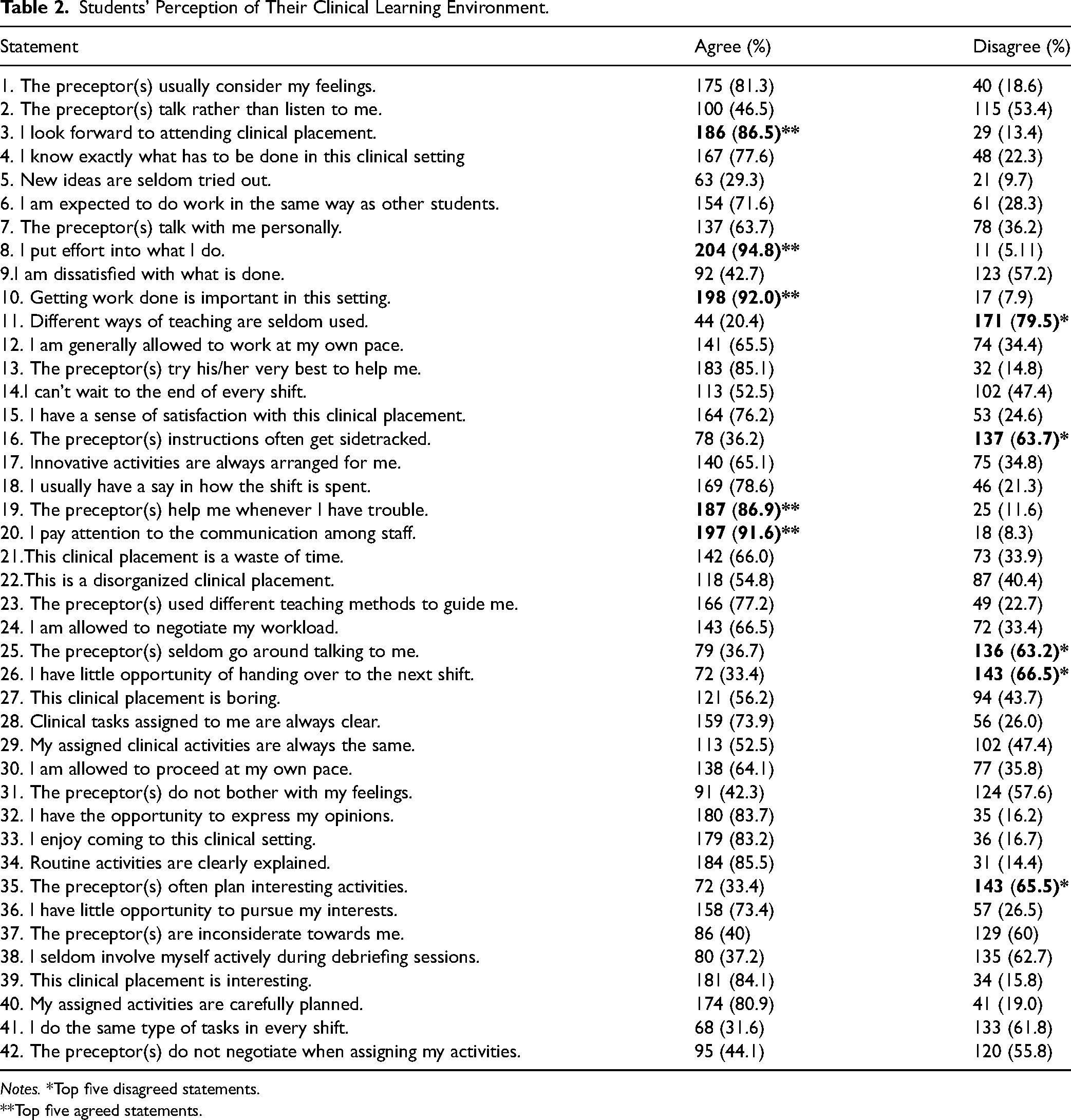
Notes. *Top five disagreed statements.
**Top five agreed statements.
Perceptions of Effective Clinical Teaching Among Nursing Students
The study also measured effective clinical teaching using 15 questions, as illustrated in Table 3. Students evaluated this aspect on a Likert scale from 1 (never/poor) to 5 (always/superb). The mean responses varied from 3.02 to 3.40, with an overall mean of 3.22.
Students’ Perception of Effective Clinical Teaching.

Relationship Between Students’ Perceptions of Effective Clinical Teaching, Demographic Characteristics, and the Clinical Learning Environment
An independent sample t-test, detailed in Table 4, revealed no significant gender-based differences in the mean scores for effective clinical teaching (t (213) = −1.37, p = .17). Similarly, the comparison between students from governmental and private universities did not yield statistically significant results (t (213) = −0.30, p = .76). However, notable distinctions were observed between regular and bridging students (t (213) = −3.76, p < .001).
Mean Differences in Effective Clinical Teaching by Gender, Type of Admission, and Type of School.

Note: * Differences in mean are significant at the 0.01 level.
Furthermore, ANOVA results indicated no substantial impact of country (F (3, 211) = 1.94, p = .12), year of study (F (3, 211) = 1.44, p = .23), or area of practice (F (3, 210) = .41, p = .79) on students’ perceptions of effective clinical teaching (see Table 5).
Mean Differences in Effective Clinical Teaching for the Country, Years of Study, and Area of Practice.

Note: * differences in means are significant at the 0.01 level.
Pearson correlation analysis was conducted to examine the relationship between effective clinical teaching and other variables, including age, GPA, and the clinical learning environment. The results showed a clear correlation between effective clinical teaching and age (r (213) = .177, p = .009), as well as a strong association with the clinical learning environment (r (213) = .572, p < .001). On the other hand, no significant correlation was found between effective clinical teaching and GPA (r (213) = −.004, p = .949; see Table 6).
Correlations Between the Effective Clinical Teaching with age, GPA, Clinical Learning Environment.

Note: *Correlation is Significant at the .01 level (two-tailed).
Discussion
The study's exploration of nursing students’ perceptions of clinical learning in four countries revealed a general sense of satisfaction. A significant majority of students recognized the importance of diverse aspects of their training. Notably, 86.5% valued attending clinical sessions, and an even higher proportion, 94.8%, emphasized the necessity of fulfilling responsibilities with assigned patients. Additionally, a strong dedication to learning was evident, with 92% of students making extra efforts and 91.6% understanding the importance of attentive communication with clinical staff. Support from preceptors in clinical settings was appreciated by 86.9% of the respondents.
The study also shed light on specific aspects of clinical education, revealing that 79.5% of students acknowledged the benefits of diverse teaching methods at clinical sites. Adherence to preceptors’ instructions was highlighted by 63.7% of students, and 63.2% underscored the need for frequent communication with preceptors. Furthermore, 66.5% of students expressed a desire for more opportunities to participate in patient handoffs, demonstrating a profound desire for practical experience. These findings align with research conducted in Oman and Jordan, which also reported positive student perceptions of clinical practice and learning, interactions with faculty, students, and staff in clinical settings, and the feedback received on clinical performance. Notably, students reported feeling significantly more motivated in-patient care when nurses in the clinical setting included them as part of the team. Additionally, they perceived the teaching faculty as role models and highly valued the professional competencies of their clinical instructors.
However, areas for improvement were also identified. Students reported negative perceptions regarding interpersonal communication with faculty, the effectiveness of clinical teaching behaviors among faculty members, student involvement during evaluations, and the adequacy of feedback from clinical instructors. Concerns were also raised about the preparedness of clinical faculty to meet students’ needs in clinical environments (Al-Dweik et al., 2021; Al-Wazzan et al., 2022; Guraya et al., 2018; Hababeh & Lalithabai, 2020; Naeem et al., 2021a). However, alongside these identified areas for improvement, the study's findings also resonate with those of similar international studies that used comparable evaluation tools. Student satisfaction with frequent interactions with clinical instructors, the consistent presence of instructors in learning settings, and effective collaboration with preceptors has been attributed to have positive effect in clinical training (Nicolaou et al., 2021)
Moreover, like the current study's results, research in other countries has highlighted concerns about the lack of clinical teaching competency among nursing instructors, identifying it as a major issue affecting students and negatively impacting the clinical learning environment (Al-Dweik et al., 2021).
Student responses regarding effective teaching in clinical areas varied, with mean scores ranging from 3.02 to 3.40 out of a possible 5 points. A significant difference was observed between bridging and regular nursing students in this study. Furthermore, a correlation was found between effective clinical teaching and factors such as the age and clinical learning environment of the students. However, no statistical differences were noted in relation to the type of institution, gender, country, year of study, or area of practice in effective teaching.
Supporting these findings, studies from Oman, Jordan, Saudi Arabia, and Palestine also highlighted differences between bridging and regular nursing students (Al-Dweik et al., 2021; Hababeh & Lalithabai, 2020). In contrast, similar studies from developed countries like the United Kingdom, the United States, and Australia did not demonstrate the same results. This discrepancy may be attributed to the variation in the available technology in laboratories and clinical settings between developed and developing countries (Al-Faris et al., 2021; Hajibabaee et al., 2021). The study revealed that the prior clinical experience of bridging nursing students, particularly in their roles as staff nurses, and their familiarity with clinical settings significantly shaped their perception of teaching, contrasting with that of regular nursing students. Influential factors impacting the perceptions of regular students in clinical settings included a lack of personalized attention from clinical instructors and a noticeable discrepancy in clinical competencies between instructors and preceptors (Khairat et al., 2021). The results of this investigation align with other studies conducted in Saudi Arabia (Aboshaiqah, 2016). In terms of competency development and the accomplishment of high learning outcomes, bridging students faced fewer challenges in clinical environments than their counterparts in standard curricula.
Student nurses experience a hierarchical educational journey, with competencies progressively becoming more complex through their academic phases. Those in their junior and senior years often face greater challenges, necessitating advanced mentoring strategies in clinical teaching. After obtaining an associate degree or diploma in nursing, students typically have prior exposure to and experience in real-world clinical settings. This background tends to reduce their stress levels associated with clinical duties and challenges compared to those enrolled in bachelor's programs.
Consistent with our research findings, students emphasize the importance of communication and support from their preceptor, aligning with previous studies that highlight the significant role of clinical instructors in providing encouragement and support for continued learning (Naeem et al., 2021 b). Effective communication also plays a crucial role in fostering connections between students and clinical instructors and achieving overall learning objectives (Ekstedt et al., 2019).
Interestingly, most participants reported being assigned the same tasks during each clinical rotation day. This observation mirrors the findings by Woo and Li (2020) and Ekstedt et al. (2019), where nursing students in Singapore and North America expressed a desire for greater autonomy in their clinical experiences, which often remained unfulfilled. In contrast, students in China, as reported by Tang (2021), showed a preference for consistent supervision and hesitance toward performing tasks independently. These insights indicate that nursing students in the studied countries frequently lack the freedom to tailor their learning to their needs and preferences. Additionally, the findings imply that nursing educators may not fully recognize the importance of incorporating creative approaches in clinical training.
Strengths and Limitations
This study marks a pioneering exploration into the perceptions of nursing students regarding clinical learning environments across four distinct countries. A notable strength lies in its integration of data from culturally, economically, and socially diverse regions, thereby enhancing its applicability and potential generalizability to a global context. However, the study's cross-sectional design presents limitations, primarily in its capacity to establish causative relationships, as data collection occurred at a single point in time. Furthermore, the evolution of students’ perceptions over the course of their academic and clinical maturation remains undetermined. Future research endeavors, particularly those employing longitudinal or experimental designs, are warranted to elucidate these aspects. The insights gained here offer valuable insights for nursing educators, providing a foundation for the development and implementation of targeted interventions aimed at optimizing the clinical educational experience for nursing students.
Implications for Practice
The findings suggest that enhancing communication and feedback could significantly improve the learning environment. There is a clear need for collaborative efforts between clinicians and academic nurses to maximize the clinical educational opportunities for students in regular programs.
Conclusion
Overall, students in the current study expressed satisfaction with their clinical learning experience. They recognized the importance of participating in clinical training, fulfilling clinical responsibilities with assigned patients, exerting extra effort in learning, receiving support from preceptors, and paying attention to staff communications in clinical settings. Effective collaboration between clinical preceptors and academic nursing lecturers is vital to creating a positive learning environment for students engaged in clinical tasks.
Footnotes
Acknowledgment
The authors would like to express their gratitude to all the participants who contributed to this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
