Abstract
Introduction
Poison is a substance that can hurt or cause dysfunction in the body due to its chemical action. Poisoning related to pesticides used in agriculture is a major public health issue in developing countries. However, there is a limited epidemiological data on poisoning in Ethiopia.
Objective
The aim of this study was to determine poisoning patterns, clinical outcome, and factors associated with poisoned patients in Northwest Ethiopia.
Methods
A cross-sectional study was conducted in July 2021 to include data of 1 year period. Data of all poisoned patients were collected using a standardized checklist from the registration book and patient medical records. The association between variables and outcomes was analyzed using a multivariable logistic regression model. A p-value of < 0.05 was considered to declare a statistically significant association.
Result
Over one-third of the poisoning cases (35.9%) were seen in the spring, according to a survey of 315 patient medical data. The majority of patients were in the age group of 21–30 years (44.1%). The most common form of poison consumed was organophosphate (OP), which accounts for 61.3% of all visits, and the least common was food poisoning, which accounts for 1.9%. About 82.5% of poisoning cases survived, while the remaining 17.5% were died. Time of arrival to the hospital ≥1 h (adjusted odds ratio (AOR) = 7.02; 95% confidence interval (CI): 1.16, 11.40), lack of oxygen support (AOR = 6.64; 95% CI: 3.56–6.78), and lack of adrenaline/dopamine medication (AOR = 3.57; 95% CI: 1.17–5.78) were all substantially linked with death of poisoned cases.
Conclusions
Three-fourth of poisoning cases survived, while the remaining one-fourth died. Ingestion of OPs is the most prevalent type of poisoning, and most cases are intentional. Delayed arrival ≥1 h, lack of oxygen support, and adrenaline/dopamine treatment were all linked to death. On-time arrival, oxygen assistance, and adrenaline/dopamine treatment in a healthcare setting are all recommended.
Introduction
Poisoning is a qualitative term that refers to a chemical substance's ability to have a negative or harmful effect on the body (Pokhrel et al., 2008). It can enter the body by a multitude of routes, causing both systemic and local effects (limited to the eyes, skin, lungs, etc.). Accidental or non-intentional poisoning is the term used to describe poisoning brought on by the unintentional use of a drug or chemical substance or the use of drugs by children for no apparent reason (Pokhrel et al., 2008). Every year, over 385 million cases of unintentional, acute pesticide poisoning are reported worldwide, with approximately 11,000 deaths. Based on an estimated global farming population of 860 million, pesticide poisoning affects around 44 percent of farmers each year (Boedeker et al., 2020). In Ethiopia, the prevalence of acute poisoning was 1.7% (Tefera & Teferi, 2020). It is highly prevalent among females and age of less than 30 years old (Chelkeba et al., 2018).
Poisoning is most commonly caused by pesticides and pharmaceuticals. Pesticides used in agriculture are a major public health issue in developing countries (Ahmed et al., 2018). Medicines that affect the central nervous system are the most commonly utilized for self-harm in the developing world. Before the 1970s, there were few case series studies for anti-epileptics, benzodiazepines, or antidepressants; however, from the 1970s onward, barbiturates became a common means of self-poisoning (Khan & Reza, 1998; Singh et al., 1984; Wesseling et al., 1997). Some Asian and African tribes have serious problems with household items including kerosene oil for lighting, cleaning agents like Dettol (Chloroxylenol), bleach, and strong acids like sulfuric acid used for drain cleaning (Nhachi & Kasilo, 1994).
Poisoning is a big health and health-related issue in our country. It is a leading cause of death and morbidity in many countries. In underdeveloped countries, poisoning is growing increasingly widespread, with major hazards such as hospitalization and mortality. Thousands of people die each year as a result of poisoning, with majority of those deaths occurring in developing countries (Senanayake & Peiris, 1995). Studies support that intentional poisoning is the most common reason of poisoning (Chelkeba et al., 2018; Getie & Belayneh, 2020; Tefera & Teferi, 2020). Pesticides, notably organophosphates (OPs), have been identified as the cause of death in the majority of self-poisoning cases, particularly in rural areas. OPs compounds are a diverse group of chemicals used in both home and industrial settings. Pesticides such as malathion, parathion, diazinon, and fenthion, nerve gases such as soman, sarin, and tabu, ophthalmic agents such as echothiophate and isoflurophate, and anti-helminthic such as echothiophate and isoflurophate are examples of OPs (trichlorfon) (Ahmed et al., 2018).
Review of Literature
Literature indicates that pattern and magnitude of poisoning in a specific location are influenced by a number of factors. Poisoning can happen in a number of ways all over the world. Because of disparities in financial situations and cultural diversity, poisoning is not evenly distributed even within the same country. The amount of poisoning in a specific location is influenced by the availability of harmful substances, the predominant occupation in that culture, and religious and societal factors (Singh et al., 1984; Varsha et al., 2020). The growing poisoning incidence in developing countries has been blamed on inadequate drug and chemical regulation, weak surveillance systems, insufficient enforcement, and easy access to a variety of drugs and chemicals (Kumar et al., 2011; Woyessa & Palanichamy, 2020).
Poisoning has become more common as a result of the rapid expansion of industry in wealthier countries and the widespread use of pesticides in developing countries to enhance agricultural output. Similarly, as medical research evolved, a wide range of insecticides and drugs became available, many of which can cause serious harm when used incorrectly (Pokhrel et al., 2008; Varsha et al., 2020; Woyessa & Palanichamy, 2020).
A study showed in southwest Ethiopia, drug overdose was the most common patterns used by both men and women (Gesese & Ochan, 2022). According to studies conducted in Ethiopia, the factors statistically associated with poisoning incidents related to suicidal attempt include current alcohol and drug use, substance abuse, depression, anxiety, a lack of social support, being a woman, and being a patient in a mental health center (Asfaw et al., 2020; Mekonnen & Kebede, 2011; Melkam et al., 2022). Another systematic review study in Ethiopia shows that mental health problems, disputes, and addiction with substance were identified as the most common reasons for acute poisoning (Chelkeba et al., 2018). Poisoning cases are frequently underreported; the pattern and magnitude of acute poisoning cases in Ethiopia remain unclear. However, few epidemiological studies on acute poisoning have been published, and those that have been published have small sample sizes (Chelkeba et al., 2018). As a result, this research was intended to address a poisoning pattern, clinical outcome and associated factors among acute poisoning cases presented to Debre Markos Comprehensive Specialized Hospital (DMCSH) over a period of 1 year in 2021.
Method and Materials
Study Area and Period
The study was conducted at emergency outpatient department (EOPD) of DMCSH in July 2021 to include data of 1 year period (July 1, 2020 to June 30, 2021). DMCSH is under Debre Markos City Administration. Debre Markos town is located 300 Km far from Addis Ababa, the capital city of Ethiopia. According to the Central Statistical Agency of Ethiopia (CSA) 2007 national census, Debre Markos had a population of 62,497, with 29,921 males and 32,576 women (Central Statistical Agency (CSA) [Ethiopia], 2007).
Study Design and Study Population
An institutional-based cross-sectional study was conducted. All cases which were seen in EOPD of DMCSH with case of acute poisoning from July 1, 2020 to June 30, 2021 were included. Poisoned patients who died upon arrival; patients with missing data in their treatment regime and records of patients who got discharged against medical advice were excluded.
Sampling Procedure and Techniques
Data were collected from medical records of all patients admitted to the Emergency Department with a primary diagnosis of poisoning during the study period.
Data Collection Tool and Procedure
A data collection checklist containing the variables to be measured was used for data collection. After ethical letter was obtained, patients with poisoning were identified and selected from the patient registration book. Socio-demographic data (age, sex, ethnicity, residency, occupation, educational status, marital status, and living condition), poison-related data (predisposing factors: (psychiatric illness, substance abuse, social conflict), route of exposure, clinical presentation, type of poisoning (OP, 2,4-D, alcohol intoxication, aluminum phosphide, food poisoning), reasons of poising, source of poison, previous history of suicide attempt, place of poisoning, presenting complain, time elapsed to come to hospital, mode of arrival, home remedy, pre-hospital care (ambulance usage), modality of management in the hospital (general resuscitation, specific antidote administration for OP, GI decontamination only, oxygen support, and adrenaline/dopamine)), months (seasons) of poisoning and outcome of poisoning data were collected from patient medical records.
Operational Definitions
Substance use: Use of at least any one of the following substances: alcohol, khat, cigarette, shisha, hashish, or drugs that are assumed to affect level of thinking and increase risk of involving in risky behaviors.
Poisoning: This refers to the development of harmful effects following exposure to chemicals, drugs, or other xenobiotic.
Acute poisoning case: Refers to those patient charts diagnosed by the attending physician as acute poisoning cases through history, physical examination, assessment of toxidromes, and or laboratory investigations.
Intentional poisoning: This is what happens when someone who is fully aware of who they are uses drugs or gives them to someone else with the intent to harm them.
Unintentional poisoning: This refers to a person ingesting poison accidentally, due to impaired self-awareness brought on by co-occurring mental illnesses or addiction, or as a result of an unknown exposure.
General resuscitation: This refers to stabilization of airway, breathing, and circulation.
Particular antidote: an antidote which is specific and appropriate for each type of poisoning chemicals
Clinical Outcome: Is the state of poisoned patients after they have been treated in the emergency department. It is reported as either survival or death.
Data Quality Control
Four (Adnet et al., 1998) BSc nurses were recruited for data collection. One supervisor was controlling the data collection procedure and a half-day orientation was given to the data collectors. The orientation was focused on clarifying the meaning of the contents of the checklist and the criteria of incomplete patient record. The data collection checklist was prepared by English language and double checked by experts to check for consistency. The questionnaire was pre-tested on 5% of the sample size in DMCSH, and the reliability was established with a Cronbach's alpha of 0.82, to ensure that the data was reliable and of high quality. No modification was made after the pre-test because the consistency and reliability was in the acceptable range (Cronbach's alpha of > 0.7). Data collectors were directly transcribed the required information from the patient medical records to the checklist. The supervisor has been checking back some sample completed checklists to confirm accuracy of data throughout the data collection period. Data was examined for completeness, accuracy, and consistency as soon as it was collected, then properly organized, and stored for compilation and analysis.
Statistical Analysis
After being reviewed and cleaned for completeness, data was entered into EpiData version 3.1 and analyzed using Statistical Package for the Social Science (SPSS) version 25 software. Data was presented by frequency, percentages, and figures. The bi-variable and multivariable binary logistic regression models were used to investigate the relationships between outcome variables and potential related factors. Variable with p-value < 0.25 in the bi-variable logistic regression model were entered into the multivariable logistic regression model (Hosmer, 1989). Adjusted odds ratios (AORs) with 95% confidence intervals (CIs) were reported to measure the strength of association. A p-value <0.05 was used to declare a statistically significant association.
Results
Socio-Demographic Characteristics of the Study Participants
The medical records of 343 poisoned patients were evaluated. The final analysis included 315 poisoned patient records that had complete information. The majority of patients were between the ages of 21 and 30 years, accounting for 139 (44.1%) of all cases, followed by the age range of 11–20 years. A higher percentage of poisoning was seen in females 188 (59.7%) when compared to males (40.3%). Another finding was bout 135(42.9%) were not attained primary education. By their occupation, 116(36.8%) and 114(36.2%) patients were farmers and unemployed, respectively (Table 1).
Socio-Demographic Characteristics of the Participants in DMCSH, 2021.

DMCSH : Debre Markos Comprehensive Specialized Hospital.
Patterns of Poisoning by Season
In the spring months of March, April, and May, the emergency department have seen a greater number of poisoning cases 113(35.9%), while the summer months of June, July, and August have seen a relatively low percentage of cases 41(13.0%). (June, July, and August) (Table 2).
Patterns of Poisoning by Months (Season) in DMCSH, 2021 (n = 315).
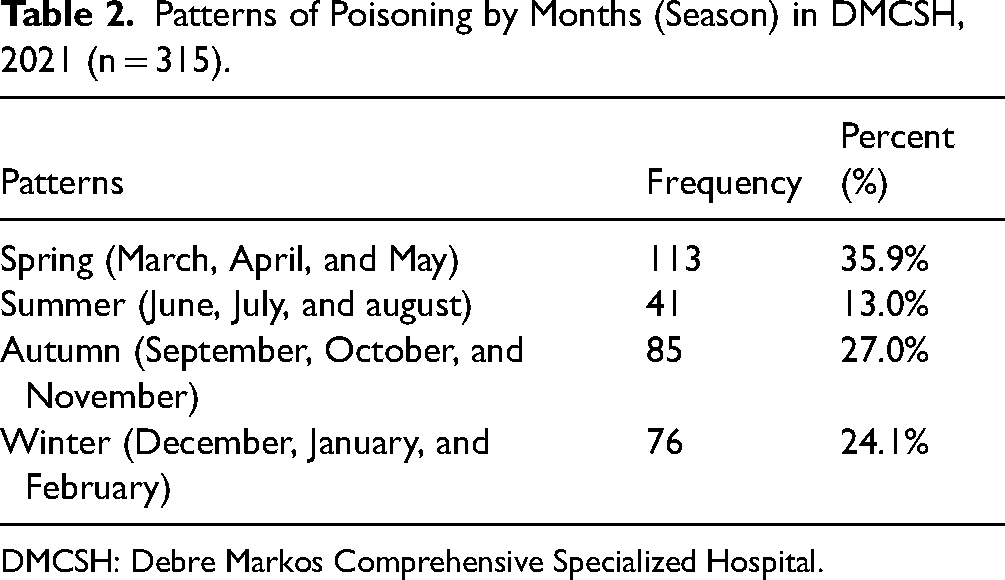
DMCSH: Debre Markos Comprehensive Specialized Hospital.
Types of Poison Ingested
In this study, OP was the most frequently consumed poison, accounting for 193 (613%), while food poisoning was the least frequently consumed poison, accounting for 6 (2.0%) (Figure 1).

Type of poison ingested in the study period at DMCSH, 2021 (n = 315).
Predisposing Factors and Route of Exposure of Poisoning
Two hundred eighty-three (89.8%) of the 315 poisoned patients took the poison intentionally. On the other hand, 20 (6.3%), 9 (2.9%), and 3 (1.0%) of the contributions were made by someone else, unintentionally and for an unexplained purpose. The biggest beginning factor for poison consumption was social conflict, which accounted for 236 (74.9%) of individuals who took the poison purposefully, and the least was other unknown factor, which accounted for 6 percent (1.9%). Only eight (2.5%) of patients who visited the EOPD had a previous history of suicidal attempt. The majority of the patients, 288 (91.4%), consumed the poison at home, while 13 (4.1%) had no idea where they ingested it. Almost all of the patients took the poison orally; 313 (99.4%) did so (Table 3).
Predisposing Factors and Route of Exposure of Poisoning at DMCSH, 2021 (n = 315).

DMCSH: Debre Markos Comprehensive Specialized Hospital.
Clinical Presentation and Outcomes of Poisoned Patients
According to the findings, the most common symptom was vomiting, which accounted for 238 (75.6%) of the patients, followed by loss of consciousness and epigastric pain, which accounted for 59 (18.7%) and 18(5.7%) of the patients, respectively. The majority of patients (227/72.1%) arrived at the hospital between 1 and 24 h after poisoning, and 24 (7.6%) arrived within 30 min of poisoning. The majority of the study participants (217, or 68.9%) arrived at the hospital by public transportation, with the rest arriving by foot or ambulance. During the study period, 315 poisoning cases visited the EOPD, with 260 (82.5%) being cured and 55 (17.5%) died as a result of poisoning (Table 4).
Clinical Presentation and Outcomes of Poisoned Patients at DMCSH, 2021 (n = 315).

DMCSH: Debre Markos Comprehensive Specialized Hospital.
Interventions Given for Poisoned Patients
Out of 315 poisoned patients, 99.4% received general resuscitation, 61.3% received particular antidotes, and 40% received oxygen (Table 5).
Management Given for Poisoned Patients in the Participants at DMCSH, 2021 (n = 315).

OP: organophosphate; DMCSH: Debre Markos Comprehensive Specialized Hospital.
Factors Associated with the Outcomes of Poisoning
Recovery from poisoning was found to be correlated with exposure time, oxygen support, and adrenaline/dopamine delivery. Patients with poisoning who arrived within an hour of exposure had a sevenfold higher chance of recovery than those who arrived between an hour and 24 h after exposure (AOR = 7.02; 95% CI: 1.16, 11.40). Furthermore, poisoned patients who received oxygen assistance were 6.64 times more likely to recover than patients who did not receive oxygen treatment (AOR = 6.64; 95% CI: 3.56–6.78). In addition, poisoned patients who received adrenaline/dopamine were 3.57 times more likely to recover than those who did not (AOR = 3.57; 95% CI: 1.17–5.78) (Table 6).
Factors Associated with the Survival in the Past 1 Year, in DMCSH, 2021 (n = 315).

*p-value < 0.05, **p-value < 0.01, ***p-value < 0.001. DMCSH: Debre Markos Comprehensive Specialized Hospital; AOR: adjusted odds ratio; CORs: crude odds ratios; CI: confidence interval.
Discussion
Of the 315 patients, 41% belonged to the 21 to 30 range of ages, which was similar to the findings from a previous study from south India which showed 50% patients who were aged between 18 and 30 (Nadeem et al., 2020; Reddy et al., 2020). Females outweighed males in this study, accounting for 59.7% of all cases. This is comparable to the findings of other studies. The same study was conducted in South India (Adnet et al., 1998), Dessie Referral Hospital (Adnet et al., 1998), and Jimma University Specialized Hospital (Melkam et al., 2022), and the results showed that the prevalence of poisoned females was 54.8%, 55.0%, and 52.4%, respectively, with age groups of 31.86% (15–24 years), 44.7% (21–30 years), and 67.9% (12–20 years).The high female to male ratio in such studies may be attributed to the fact that females more exposed to poisoning due to more stay in home (Chelkeba et al., 2018).
The emergency department received over one-third of the poisoning cases (35.9%) was in the spring months of March, April, and May, which was contrary to the findings of Dessie Referral Hospital (Getie & Belayneh, 2020) where as it received a less percentage (13.0%) of cases during the summer months of (June, July, and August). The relatively high prevalence of poisoning during this season could be attributed to the use of pesticides after harvest in spring. It is the time when insecticides were highly used for storing of cereal products in Ethiopia (Berhe et al., 2022).
OPs were the leading causes of poisoning (61.3%) followed by aluminum phosphide (25.7%), alcoholic intoxication (7%), 2, 4 dichlorophenoxy acetic acid (4.1%), and food poisoning (1.9%). OPs (45%) were identified as a common cause of poisoning in a study conducted at Dessie Referral Hospital (Adnet et al., 1998), whereas studies conducted at Jimma University Specialized Hospital (Nhachi & Kasilo, 1994) and Tikur Anbesa Hospital (Adnet et al., 1998) identified household cleaning agents as a common cause of poisoning, 40.4% and 43.1%, respectively. Majority (89.8%) of the poisonings were intentional, which was similar to the findings of Indian study (Peshin et al., 2014). Most of them were farmers followed by unemployed. This may be attributed to the lack of knowledge, poor social support, and stress related to unemployment (owing to family burden) supported by other studies done (Lekei et al., 2014; Mekonnen & Kebede, 2011; Melkam et al., 2022; Platt, 1984; Teklemariam et al., 2016). Almost all poisoning cases (99.4%) involved oral ingestion as the route of exposure, which is consistent with the finding from other studies (Al-Barraq & Farahat, 2011; Jailkhani et al., 2014; Teklemariam et al., 2016).
Vomiting, loss of consciousness, and epigastric pain were the most common presenting symptoms which accounting for 238 (75.6%), 59 (18.7%), and 18(5.7%) respectively. The victims in this study were managed using general resuscitation (99.4% of the cases). Specific antidote (Atropine sulfate) was given for all OP poisoned (61.3%) patients which is similar with a study done in eastern Ethiopia (Nigussie et al., 2022). Most of the cases were survived 260 (82.5%). The case fatality rate was 55 (17.5%). This result is a bit higher than results from Jimma University Specialized Hospital (Teklemariam et al., 2016) probably because the time of arrival of patients in DMCSH was after 1 h.
Only 27.9% of patients arrived at the hospital within 1 h after exposure with the majority (72.1%) arriving during one to 24 h. The result from Jimma University Specialized Hospital (Teklemariam et al., 2016) also revealed comparable result, 39.4% of patients arrived within 1 h of exposure but most 56.7% arrived within 1–24 h. The majority of patients arrived precisely 1 hour after being poisoned, which helps to explain this. The time between ingesting a poison and being admitted to the hospital is crucial for better care of poisoned patients. Treatment should begin as soon as a poisoning event occurs (Tripathi, 2013; Usha et al., 2017). This finding would imply that the factors associated with delays in reaching to the hospital should be identified and the health-seeking behavior of people regarding poisoning incidents should be improved (Daly et al., 2006).
In poisoning cases, exposure period, oxygen assistance, and adrenaline/dopamine delivery were all found to be linked to recovery. Poisoned patients who arrived within 1 h of exposure had a sevenfold higher chance of being survived than those who arrived between 1 and 24 h after exposure. This finding is supported by the recommendation of the study which stated that patients who present with serious toxic effects, prompt action is required (Chandran & Krishna, 2019). The explanation for this could be that if they arrive early, they will get early appropriate treatments before the poison cause irreversible damage to the body.
When compared to poisoned people who did not receive oxygen treatment, poisoned cases who received oxygen support were 6.64 times more likely to survive. The necessity to secure the airway is dictated by the loss of airway-protective reflexes and worry about aspiration or the presence of respiratory failure. Rapid sequence intubation with preoxygenation and neuromuscular inhibition is the best strategy to secure the airway unless the patient is dead (Adnet et al., 1998).
Similar to this, poisoned patients who received adrenaline/dopamine had a 3.57 times greater chance of making a full recovery than those who did not. Patients who got oxygen and adrenaline/dopamine after becoming critically ill may have experienced this. As a result, the likelihood of survival increased. Stomach aspiration, artificial breathing if hypoventilation is present, intravenous or intratracheal dopamine, noradrenaline, or adrenaline administration are all recommended if cardiovascular depression or peripheral vasodilation are visible(de Jong-Straková et al., 1990).
Limitation of the Present Study
The results will not be generalized to outside of the chosen study area due to purposively chosen study area and relatively smaller sample size without performing power analysis. Also, the number of cases included during this period might vary from actual number from this region, due to underreporting. There was also possibility of misdiagnosis, since the poisonings reported were not confirmed with serum analysis or other toxicological studies, and that the only source of information about the ingested poison was provided by the patient or the patient's family member.
Implications for Practice
According to the findings of this study, the majority of poisoning cases were intentional, and the majority of patients were farmers, followed by unemployed people. This would mean that uneducated farmers’ lack of knowledge, low social support, and stress associated to unemployment (due to family load) should be given special attention in this population group. Furthermore, the majority of the poisoned victims were females. This would imply that females should be prioritized in search for factors that contribute to suicidal ideation (intentional poisoning). Furthermore, the study's findings would imply that when poisoning incidences occur, patients or patient families should be advised to arrive at neighboring health facilities as soon as possible. It is also vital to remember that when a poisoned patient arrives to a medical facility, suitable antidotes, and oxygen should be administered as soon as feasible. Lastly, it would be critical to introduce machine learning algorithms to support the quick evaluation of these poisoned individuals in a congested emergency room (Malakouti, 2023).
Conclusions
Three-fourth of poisoning cases survived, while the remaining one-fourth died. Ingestion of OPs is the most prevalent type of poisoning, and most cases are intentional. Delayed arrival ≥1 h, lack of oxygen support, and adrenaline/dopamine treatment were all linked to death. On-time arrival, oxygen assistance, and adrenaline/dopamine treatment in a healthcare setting are all recommended. Overall, the finding of this study implies that early hospital visits should be emphasized when there are poisoning incidents. In addition, it is recommended that the reason for the highest incidence of poisoning in the spring months in the area should be explored in detail.
Footnotes
Acknowledgments
We are grateful to Debre Markos University's School of Medicine for ethical approval and the DMCSH personnel for collaborating by providing the poisoned recordings.
Authors’ Contributions
AT, MM, and EF developed the study design literature review, quality assessment, data extraction, statistical analysis, and interpretation of the data. TA, FF, ET, and AAA developed drafts of the manuscript. All authors approved the final manuscript.
Availability of Data
The data used for this study are available from corresponding authors on secured and reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval and clearance were obtained from the ethical review committee of the School of Medicine, Debre Markos University with protocol number of Ref(S/R/C/58/11/2021). A formal letter of permission was written from Debre Markos University, School of medicine to DMCSH's Medical Director. After discussing the purpose and method of the study, before data collection, written permission was obtained from DMCSH medical director to access and evaluate poisoned patients medical records/ charts. The ethical review committee approved the use of patients’ medical records/ charts. The data was kept in codes instead of any personal identifiers and the confidentiality of all study participants was maintained throughout the study.
Consent for Publication
Not applicable.
