Abstract
Introduction
Organizations still struggle with the best mechanisms to implement research into practice, and guideline developers need to continue to strive toward collaboration and avoidance of duplication.
Objective
To assess the utilization of evidence-based nursing practice and associated factors among nurses working in Saint Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia, 2022.
Methods
An institutional-based cross-sectional study was conducted from 10 September 2022 to 25 November 2022. The total sample size was 418, and a simple random sampling technique was used to select nurses. Data were collected through a self-administered questionnaire. Data were entered using EpiData version 4.6 and exported to SPSS version 25 for analysis. Multicollinearity was considered by using a variance inflation factor (VIF > 10). The goodness of fit test was done using the Hosmer–Lemeshow model. Binary logistic regression was done, and variables with a
Result
The utilization of evidence-based nursing practice was 58.1% [95% CI: 52.23–63.24]. Male sex [AOR 4.65, 95%CI: 2.51–8.63], work experience of >5 years [AOR 6.83, 95%CI: 2.27–20.58], head nurse role in the hospital [AOR 1.72, 95%CI: 1.02–3.18], master's degree educational status [AOR 2.78, 95%CI: 1.89–8.61], and availability of EBNP guideline in the ward [AOR 1.24, 95%CI: 1.04–5.32] were significantly associated.
Conclusion
About six in 10 nurses utilize EBNP at Saint Paul’s Hospital Millennium Medical College. Sex, experience of >5 years, head nurse role in the hospital, master's degree educational status, and availability of EBNP guidelines in the ward were significantly associated with the utilization of EBNP. Therefore, recruiting experienced nurses, learning master`s degrees, and availing the EBNP guidelines in the ward might increase the utilization of EBNP.
Keywords
Introduction
Evidence-based nursing practice (EBNP) is the use of the best research-proven assessments and treatments in our day-to-day client care and service delivery (Barton, 2014; Beglinger, 2014; Davidson & Brown, 2014; Jylha et al., 2017; Melnyk & Fineout-Overholt, 2015; Portney, 2020). It is a practice through which nurses execute their clinical duties while utilizing the current and valid research findings, clinical expertise (Beglinger, 2014; Melnyk & Gallagher-Ford, 2015; Portney, 2020), the client values and preferences (Aronsson et al., 2017; Barton, 2014; Hassien, 2016; Melnyk & Gallagher-Ford, 2015), and the available resources to make a practice decision (Melnyk et al., 2018; Shayan et al., 2019; Straus et al., 2018). Its movement begins with the identification of the research-to-practice gap and applying decision-making at different levels of the health system of professional nursing practice (Dereje et al., 2018; Jylha et al., 2017; Mariann et al., 2020). Today, EBNP is considered a key component of modern nursing care (Aronsson et al., 2017; Davidson & Brown, 2014; Mariann et al., 2020; Saunders et al., 2019).
The utilization of EBNP is an ongoing initiative that involves a broader approach to promoting acceptance of EBNP, including strategies to correct misperceptions about EBNP (Saunders & Julkunen, 2016; Zhou et al., 2016), and the development of skills (Fu et al., 2020; Reid et al., 2017; Shayan et al., 2019). It is conceptualized as clinical decision-making that considers the feasibility, appropriateness, meaningfulness, and effectiveness of healthcare practices. This may be informed by the best available evidence, the context in which care is delivered, the individual patient, and the professional judgment and expertise of the health professional (Jordan et al., 2019; Saunders et al., 2019; Stokke et al., 2014; Verloo et al., 2017). Organizations still struggle with the best mechanisms to implement research into practice, and guideline developers need to continue to strive toward collaboration and avoidance of duplication (Beglinger, 2014; Melnyk & Fineout-Overholt, 2015; Melnyk & Gallagher-Ford, 2015; Zeb et al., 2018).
Literature Review
Works of literature indicate that not having enough time, lack of institutional or financial support, insufficient support from colleagues, shortage of personnel and resources, inability to understand research reports, lack of knowledge, and the dependence of nurses on doctors and managers in making changes in clinical practice are the most common barriers that prevent nurses from the utilization of EBNP (Jordan et al., 2019; Sapkato, 2014). Training in research methods, organizing policies, and organizing evidence-based protocols are sources for the utilization of evidence-based nursing practice (Duncombe, 2018). Studies show that nurses frequently mentioned unawareness of EBNP or difficulty in reading and interpreting research papers (Higgins et al., 2019; Ubbink et al., 2011). Most of the time, nursing care practice in Ethiopia is based on experience, tradition, intuition, common sense, and untested theories. There is a lack of information on the level of EBNP utilization by nurses in Ethiopia (Berkman et al., 2013; Shayan et al., 2019). Currently, hospitals in Ethiopia are undergoing different construction to expand their services like cardiac and oncology centers. Nurses who give service in this center should expect to have a culture of searching for new evidence-based nursing practices to improve patient outcomes. As a result, this study evaluated the utilization of EBNP and associated factors among nurses working in Saint Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia.
Methods and Materials
Study Area and Period
The study was carried out in Saint Paul’s Hospital Millennium Medical College which is found in Addis Ababa, the capital city of Ethiopia. Currently, Saint Paul’s Hospital Millennium Medical College has more than 1,000 beds. It serves about 350,000 patients per year in its outpatient department and about 49,000 in the inpatient. It trains a large number of undergraduate medical students as well as several residents. Currently, the hospital has more than 1,300 nurses; from them, 836 have bachelor's and master's degrees. The study was conducted from 10 September 2022 to 25 November 2022.
Study Population
The study population in this study was selected nurses working in Saint Paul’s Hospital Millennium Medical College. Nurses working in Saint Paul’s Hospital Millennium Medical College were included in this study. However, diploma-level nurses and nurses on leave during the data collection period were excluded. The sample size was estimated using a single population proportion formula with the following assumptions: 95% confidence level, a margin of error (0.05), and 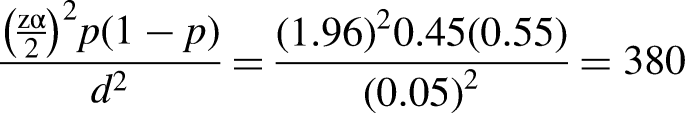
A simple random sampling technique was used to select 418 bachelor's and master's degree nurses from 836 nurses by using the human resource nurses’ registration list as a sampling frame. Then, the number of bachelor's and master's degree nurses in each working unit was identified as 202 nurses, medical ward; 152 nurses, surgical ward; 116 nurses, emergency; 108 nurses, intensive care unit; 124 nurses, pediatrics ward; 78 nurses, operation room; and 56 nurses, outpatient department. Finally, the proportional allocation was used to determine and include nurses from each nursing unit. Based on this, 101 nurses were from the medical ward, 76 nurses were from the surgical ward, 58 nurses were from the emergency, 54 nurses were from the intensive care unit, 62 nurses were from the pediatric ward, 39 nurses were from the operation room, and 28 nurses were from the outpatient department.
Study Variables
Dependent Variable
Utilization of evidence-based practice.
Independent Variables
Operational Definition
Data Collection Tool and Procedures
Data were collected using a structured self-administered and pretested questionnaire. The questionnaire was prepared in English and was adapted from different literature (AynalemI & Mignote, 2021; Dereje et al., 2018; Fu et al., 2020; Melnyk et al., 2018; Zhou et al., 2016). The tool contained sociodemographic, individual, and organizational factors, which are part of independent variables. EBNP was assessed by using 23 questions that asked about the evidence-based nursing practice of nurses for patients they care for in their work setting. The data were collected by seven bachelor's degree pharmacy technicians and supervised by one master's holder public health officer. The data collection was carried out by self-administering the questionnaire for the selected nurses in their respective wards.
Data Quality Assurance
The tool was prepared in English in collaboration with senior nursing experts, and a 2-day training was given for data collectors and supervisors. A pretest was conducted on 5% (21 nurses) of the sample size at Saint Petro's Hospital a week before the initiation of the main study. Based on the pretest result, the necessary corrections were made. To check reliability, the Cronbach's alpha reliability test was done, and it was 0.824. Continued follow-up and supervision were performed by the supervisor and researchers throughout data collection. All filled questionnaires were reviewed before data entry.
Statistical Analysis
Data were entered using EpiData software version 4.6 and exported to SPSS version 25 for analysis. Descriptive analysis was performed, and the results were presented using tables, figures, frequencies, and percentages. Multicollinearity was considered by using a variance inflation factor (VIF > 10) (El-Dereny & Rashwan, 2011). The goodness of fit test was done using the Hosmer–Lemeshow model (Hosmer & Lemeshow, 2000). Binary logistic regression was done, and variables with a
Result
Sociodemographic Characteristics
Four hundred eighteen nurses gave responses that made the overall response rate of 100%. More than half, 234 (56.0%), were females, and the age group of 193(46.2%) was 24–30 years old. Of the participants, 225 (53.8%) were married, and 351(84.0%) were bachelor’s degree holders. The work unit of 101 (24.2%) nurses was the medical ward. The religion of 146 (34.9%) nurses were Orthodox, the work experience of 286 (68.4%) nurses was less than or equal to 5 years, and the monthly income of 261 (62.4%) nurses was greater than or equal to 7,000 Ethiopian birr (Table 1).
Sociodemographic Characteristics of Nurses in Saint Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia, 2022.

Individual and Organization-Related Factors
From a total of 418 nurses, 195 (46.7%) did take EBNP training; however, 223 (53.3%) did not take EBNP training. Similarly, 115 (27.5%) had research experience, but 303 (72.5%) did not have research experience. Less than half, 153 (36.6%), had a willingness to utilize EBNP; in contrast, 265 (63.4%) did not have a willingness to utilize EBNP.
More than half, 272 (65.1%), of the nurses reported the availability of EBNP guidelines at the workplace, but 146 (34.9%) reported the absence of EBNP guidelines at the workplace. About 104 (24.9%) nurses reported that they had enough time to utilize EBNP; however, 314 (75.1%) did not have enough time to utilize EBNP. The patient load for 63 (15.1%) was ≤3 patient to 1 nurse, but for 355 (84.9%) >3 patient to 1 nurse. Regarding the availability of computers in the work area, 231 (55.3%) worked in the ward where there was a computer, but 187 (44.3%) worked in the ward that did not have a computer.
Sources and Utilization of Evidence-Based Nursing Practice
Out of the 243 nurses who utilized evidence-based nursing practice, sources 36 (14.8%) were from previous classes, and 34 (14.0%) were from hospital protocol. About 59 (24.2%) was national guideline, 31 (12.8%) was training, 23 (9.5%) was colleague, 16 (6.6%) was personal experience, and 44 (18.1%) was internet (Figure 1).

Sources for utilization of evidence-based nursing practice in Saint Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia, 2022 (
Out of 418 nurses, 243 (58.1%) utilized EBNP; on the other hand, 175 (41.9%) not utilized EBNP (Figure 2).

Utilization of evidence-based nursing practice in Saint Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia, 2022 (
Factors Associated With the Utilization of EBNP
In bivariable analysis, sex, work experience, salary, role at the hospital, educational status, availability of EBNP guidelines in the ward, and EBNP training were significantly associated with the utilization of EBNP. Whereas, in multivariable analysis, male sex [AOR 4.65, 95%CI: 2.51–8.63], work experience of >5 years [AOR 6.83, 95%CI: 2.27–20.58], head nurse role in the hospital [AOR 1.72, 95%CI: 1.02–3.18], master's degree educational status [AOR 2.78, 95%CI: 1.89–8.61], and availability of EBNP guideline in the ward [AOR 1.24, 95%CI: 1.04–5.32] were significantly associated with utilization of EBNP (Table 2).
Bivariable and Multivariable Logistic Regression Analysis of Utilization of EBNP Among Nurses in Saint Paulo's Millennium Medical College, Addis Ababa, Ethiopia, 2022.

*
Discussion
In this study, the utilization of evidence-based nursing practice was 58.1% [95% CI: 52.23–63.24]. This finding was consistent with studies conducted in Tikur Anbessa Specialized Hospital, Ethiopia (57.6%) (Hadgu et al., 2015), in Amhara regional referral hospitals, Ethiopia (55%) (Dessie et al., 2020), in west Gondar, Ethiopia (53%) (MA. Beshir et al., 2017). However, it was higher than studies done in public hospitals of the Jimma zone, Ethiopia (51.8%) (B. Dereje et al., 2018), and South Korea 46% (Kang, 2016). This similarity among Ethiopian studies might be due to having harmonized educational sources for nursing programs, having control by a single ministry of health, a single guideline and protocol, and clinical health practice. However, the difference seen from studies done in South Korea might be due to variations in national health policy, guidelines, clinical practice care protocol, and the time difference.
This study revealed that sex was statistically associated with the utilization of EBNP. Male nurses were 4.65 times more likely to utilize EBNP compared to female nurses. This finding was consistent with research done in Jimma zone hospitals, in Ethiopia (Dereje et al., 2018). Female nurses are busy due to familial and social duties such as child rearing and caring, feeding, and familial support.
In this study, work experience was statistically associated with the utilization of EBNP. Nurses whose work experience was greater than 5 years were 6.83 times more likely to utilize EBNP compared to nurses whose work experience was less than or equal to 5 years. This was supported by a study conducted in Amhara referral hospitals, in Ethiopia (AynalemI & Mignote, 2021). This might be due to work experience and increased exposure to different seminars, training, and familiarity with different database sources may increase.
In this study, the role of the hospital was statistically associated with the utilization of EBNP. Ward head nurses were 1.72 times more likely to utilize EBNP compared to staff nurses. This was supported by another study (Dereje et al., 2018). This was related to having opportunities for head nurses to take workshops and training about EBNP.
This study revealed that master's degree educational status was one of the factors statistically associated with the utilization of EBNP. Nurses whose educational status was a master's degree were 2.78 times more likely to utilize EBNP compared to nurses whose educational status was a bachelor's degree. It was similar to the study at public hospitals (Dereje et al., 2018; Melnyk et al., 2018). This designates that nurses who had higher qualifications were more likely to use EBNP than lower qualifications. This might be because the master's level was more technologically inclined, thus enhancing searching strategies, or that they are more exposed to the incorporation of EBNP in their curricula and teaching programs than a bachelor of science.
This study showed that the availability of EBNP guidelines in the ward was statistically associated with the utilization of EBNP. Nurses whose wards had the availability of EBNP guidelines were 1.24 times more likely to utilize EBNP compared to nurses whose wards did not have EBNP guidelines for the utilization of EBNP (Jylha et al., 2017; Kang, 2016). This is due to the presence of leading and guiding material that encourages performance.
Limitations of the Study
The study may be prone to information biases and recall bias and did not investigate the differences among wards. Additionally, the cross-sectional nature of the study design that did not differentiate cause and effect priority may be the limitation of the study.
Implications for Nursing Practice
Identifying the independent risk factors of the utilization of evidence-based nursing practice is imperative in aiding healthcare policymakers to design practical-based strategies, and it gives clues for healthcare workers in managing patients diagnosed with various causes. The health management strategies of developing countries should focus on evidence-based nursing practice. Working on the nurses’ capacity building regarding sex, work experience, role in the hospital, and educational status can imply the effective utilization of evidence-based nursing practice for patients. Additionally, considering and addressing the availability of EBNP guidelines in the ward can also improve the utilization of evidence-based nursing practice. The stakeholders of the healthcare system can have better utilization of evidence-based nursing practice if they implement their strategic plan in consideration of the implied independent risk factors.
Conclusion
About six in 10 nurses utilize EBNP in Saint Paul’s Hospital Millennium Medical College. Sex, work experience, role in the hospital, educational status, and availability of EBNP guidelines in the ward were important factors for the utilization of evidence-based nursing practice. Therefore, recruiting experienced nurses, learning master`s degrees, and availing the EBNP guidelines in the ward might increase the utilization of EBNP.
Footnotes
Acknowledgments
We would like to thank the study participants for the scarification of their valuable time spent filling out the questionnaires.
Abbreviations Used
AOR, adjusted odds ratio; COR, crude odds ratio; EBNP, evidence-based nursing practice; SPSS, Statistical Software Package for Social Sciences.
Authors’ Contribution
All authors have made substantial contributions to the work; participated in the conception, design, and acquisition, conducted the data analysis and interpretation; and took part in drafting, revising, and critically reviewing the article. All authors gave their final approval of the version to be published and have agreed on the journal to which the article has been submitted and have agreed to be personally accountable for all aspects of the work.
Availability of Data
The data used for this study are available from corresponding authors on secured and reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Consideration
Ethical clearance was obtained from Jigjiga University, College of Medicine and Health Sciences, Ethical Review Committee. Then this ethical clearance letter was given to Saint Paul's Hospital Millennium Medical College to obtain permission to conduct the study in the hospital. Lastly, the medical directors directed these letters to the nursing directorates, and the nursing directorate was directed to matrons and head nurses of the working units.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The fund for this study was covered by Jigjiga University (grant number JJU/CoMHS/101/13).
Informed Consent
Written informed consent was obtained from each participant's nurses, and the information obtained from them would not have been disclosed. Coding was used to eliminate respondents’ names and other personal identification to ensure anonymity, privacy, and confidentiality. All the participants’ response was kept confidential, and their right to refuse to answer the questions was respected. Thoroughly, our research required the principles of the Declaration of the Helsinki General Assembly, Seoul, Korea, in October 2008.
Recommendation for Researchers
Better to conduct observational studies, investigate the differences among wards, including rural health facilities, and focus on nursing practice and nursing implications in the future.
