Abstract
Introduction
Nurses are responsible for monitoring and providing nursing care to patients. The early detection of a patient who is starting to deteriorate – and the activation of critical care outreach services (CCOS) – can improve patient outcomes. However, the literature indicates that CCOS are underutilised. Self-leadership is a process whereby persons influence their own behaviour.
Objective
The purpose of this study was to develop strategies for the facilitation of self-leadership in ward nurses that will enable them to act proactively and promptly in utilising CCOS at a private hospital group in South Africa.
Methods
A sequential exploratory mixed-method research approach was followed to develop strategies for the facilitation of self-leadership in nurses that will enable them to utilise CCOS proactively when a patient starts to deteriorate. An adapted version of Neck and Milliman's self-leadership strategic framework was used as the methodological steps of the study.
Results
The quantitative analysis extracted eight factors, which were used as the departure point to develop strategies for the facilitation of self-leadership among nurses in a CCOS. Five strategies were developed that related to self-motivation, role models, patient outcome, assistance and guidance from CCOS, and the power of self-confirmation; these strategies aligned with the themes and categories extracted from the qualitative data analysis.
Conclusion
There is a need for self-leadership among nurses in a CCOS.
Keywords
Introduction and Background
Observing and monitoring patients’ health conditions is a vital responsibility of nurses and the key to identifying any deterioration in patients (Van Galen et al., 2016). Early recognition of patients whose health is deteriorating and the management of these patients in general wards can help to reduce the need to transfer these patients to a higher level of care (Subbe et al., 2017).
Review of the Literature
Critical care outreach services (CCOS) are implemented to identify patients in general wards whose health is deteriorating and to provide nurses with assistance with providing timely and appropriate nursing care for these patients. Globally, several CCOS approaches have been implemented in healthcare facilities. Although these approaches are known by diverse terms – including the ‘rapid response system’, ‘medical emergency team’ and the ‘patient-at-risk team’ – all have the same goal, namely to assist nurses with the management of patients whose health is at risk of deteriorating or is deteriorating at that moment. Prinsloo (2020) states that the diversity of CCOS approaches all share one element, namely the tracking of vital data by using a referral algorithm, for instance the modified early warning score (MEWS), to indicate when a patient needs to be referred to CCOS. CCOS assist nursing staff in implementing suitable and personalised interventions for the referred patient to prevent them from further deterioration; alternatively, CCOS assists nurses in transferring the patient to a higher level of care, if necessary. Although these services have been implemented, the literature reveals that they have not been used consistently (NCEPOD, 2015; Özdemir et al., 2021). Nurses thus need to implement self-leadership to motivate themselves to follow the guidelines in activating CCOS when a patient starts to deteriorate.
The process of self-leadership entails persons’ influencing their own behaviour by using three specific sets of strategies, namely behaviour-focused strategies, constructive thought patterns and natural reward strategies (Neck & Houghton, 2006). With behaviour-focused strategies, people manage their behaviour by using tactics such as self-observation, self-goal-setting, self-cueing, self-reward and self-correcting feedback (Neck et al., 2020). To change ineffective behaviour, nurses should be aware of their behaviour and what they need to change. Therefore, self-observation can be seen as the first step in changing ineffective behaviour, for instance when nurses determine that they are unsure when to activate the CCOS and set themselves the goal (goal-setting) of empowering themselves by learning the process to follow in activating CCOS. The nurse thus changes their behaviour by gaining knowledge of the process to follow in activating CCOS. Having a poster outlining the process of activating CCOS when needed is an example of self-cueing to remind the nurse of the process to follow. Self-reward can be either simple, such as congratulating yourself on achieving your goal, or more concrete, such as acquiring something you wanted. Self-correcting feedback means that nurses examine their ineffective behaviour introspectively, determine what they need to do to correct such behaviour and then proceed to apply effective behaviour.
Constructive thought patterns facilitate the formation of constructive thought beliefs to have a positive impact on nurses’ performance. Nurses identify and replace dysfunctional beliefs and disregard irrational or pessimistic self-talk in favour of more useful and positive self-talk (Neck & Houghton, 2006). Another constructive thought pattern approach is mental imagery, which involves visualising the successful execution of a task in advance of performing the task (Neck et al., 2020). This can be seen when the nurse is anxious about performing nursing care interventions on a deteriorating patient. They can imagine performing these nursing care interventions under the guidance of the CCOS, which will probably reduce their anxiety about performing these interventions.
Natural reward strategies help people to focus on the intrinsically motivating features of a given task and involve building more pleasurable features into a task or diverting attention away from the less enjoyable features (Neck & Houghton, 2006). An example is when a nurse is doing a routine task, such as measuring a patient's vital data, and then focusing on the importance of recording the patient's vital data. This results in increased feelings of competence, self-control and a sense of purpose (Ryan & Deci, 2017).
To date, there has been little research on the self-leadership of ward nurses in a CCOS. Practising self-leadership might influence ward nurses to engage in their work and activate CCOS according to the guidelines set out in the healthcare organisation. There is growing support for the possible advantages of practising self-leadership among nurses (Kayral & Dulger, 2019; Kim & Kim, 2019). The purpose of this study was to develop strategies for the facilitation of self-leadership in ward nurses that will enable them to act proactively and promptly in utilising CCOS at a private hospital group in South Africa by investigating the following research questions. (a) How do nurses experience their self-leadership in the CCOS at a private hospital in Pretoria? (b) What is the conceptual framework within which nurses lead themselves in the CCOS? (c) How will nurses lead themselves to follow the CCOS guidelines? (d) What strategies can be implemented to facilitate self-leadership among nurses in a CCOS?
Methods
Design
A sequential exploratory mixed-method research approach (Polit & Beck, 2017) was followed to achieve the purpose of the study. An adapted version of Neck and Milliman's (1994) self-leadership strategic framework was used as the methodological steps to develop strategies for the facilitation of self-leadership among nurses in a CCOS at a private hospital group in South Africa. The first step, according to Neck and Milliman's (1994) self-leadership strategic framework, was to observe, record and analyse the phenomenon of self-leadership. A qualitative exploratory descriptive contextual design was used for this purpose. The creation of a new conceptual framework for the phenomenon was the second step in the self-leadership strategy framework. The third adapted step initiated the quantitative exploratory approach of the study. Here the author explored the perceptions of nurse managers working at different private hospitals in the hospital group in Gauteng in terms of initiating self-leadership.
The fourth step was to create a work environment that is conducive to self-leadership. Strategies to facilitate self-leadership among ward nurses in CCOS were developed from the findings of the statistical analysis.
Research Questions
The research questions were as follows:
How do nurses perceive their ability to lead themselves in the current CCOS at a Gauteng's private hospital? What is the conceptual framework that nurses in the current CCOS at a private hospital in Pretoria lead themselves within? How will nurses lead themselves to implement the CCOS at a Gauteng private hospital group? What strategies can be implemented to facilitate self-leadership among ward nurses in a CCOS?
Settings and Sample
The setting for this study was a private hospital group in Gauteng, comprising several hospitals. One hospital with a bed capacity of about 500 beds was the setting for the qualitative phase. The accessible population was 203 nurses working permanently in general wards who were purposively invited to participate in focus group discussions. Nurses who worked in the intensive care units and high-care units were excluded from the sample as they were not part of the CCOS. The same applied to nurses who were not permanently employed by the hospital group, for example, agency nurses. For the quantitative part of the study, total sampling was used as the target population is small (Laerd, 2012) and 123 questionnaires were handed out to all the ward nurse managers at 12 hospitals from the private hospital group in Gauteng. Managers not working in nursing wards were excluded from the sample.
Data Collection Qualitative Phase
Data saturation was achieved after eight focus group discussions with nurses who were employed at one of the private hospitals in the group. Participants for the focus group discussions varied between five and nine. An interview guide consisting of open-ended questions was used to explore nurses’ self-leadership experiences in CCOS. The participants were asked: ‘How is it for you to lead yourself in the outreach service in the ward where you are placed?’ The following probing questions were also asked: ‘Tell me about the outreach service?’ and ‘What do you understand around the goals of the outreach service?’
Data Collection Quantitative Phase
The conceptual framework served as the foundation for the creation of the questionnaire, converging strategies that nurses apply to lead them to implement CCOS. Participants were asked to rate how much they agreed or disagreed with each of the items on a five-point Likert scale that made up the questionnaire. The questionnaire was divided into two sections: section 1, participants’ biographical information, and section 2, statements reflecting the concepts of the conceptual framework about self-leadership, and this was divided into six headings as seen in Table 1. A total of 123 questionnaires were handed out to nurse managers at 12 different hospitals and 83 questionnaires were received back.
Questionnaire Section 2 Headings.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Data Analysis
Qualitative Phase
For the qualitative phase of the study, the data were collected and then transcribed verbatim after each focus group discussion and anonymised by removing any personal data that could identify participants. The transcribed data were analysed by means of content analysis (Friese, 2019). Trustworthiness was ensured through credibility, dependability, confirmability, transferability and authenticity (Polit & Beck, 2017).
Quantitative Phase
The questionnaires were analysed using SPSS software version 22 using descriptive and inferential statistics. Data were described and compiled using descriptive statistics, including frequency distributions (f), mean values (x) and standard deviations (SD). In this study, factor analysis was utilised to determine how the variables interacted with one another and to untangle these interactions in order to find groups of relationships (factors) that were closely related (Grove et al., 2015, p. 343). An exploratory factor analysis was carried out because there were no predefined concepts regarding the number of dimensions in a group of variables in the questionnaire (Osborne & Banjanovic, 2016). Items that were answered by all the participants were included in the factor analysis and a Kaiser–Meyer–Olkin test was used to measure the sampling adequacy (Hinton et al., 2014). Validity and reliability were enhanced through pre-testing of the questionnaire to ensure the appropriateness of statements, face validity and construct validity. A Cronbach's alpha test for internal consistency was conducted on each factor (Polit & Beck, 2017)
Results
Research Question 1
Focus group participants’ ages ranged from 22 to 55. Three themes, five categories and 12 sub-categories were derived from the qualitative data analysis as seen in Table 2.
Themes, Categories, and Sub-Categories.
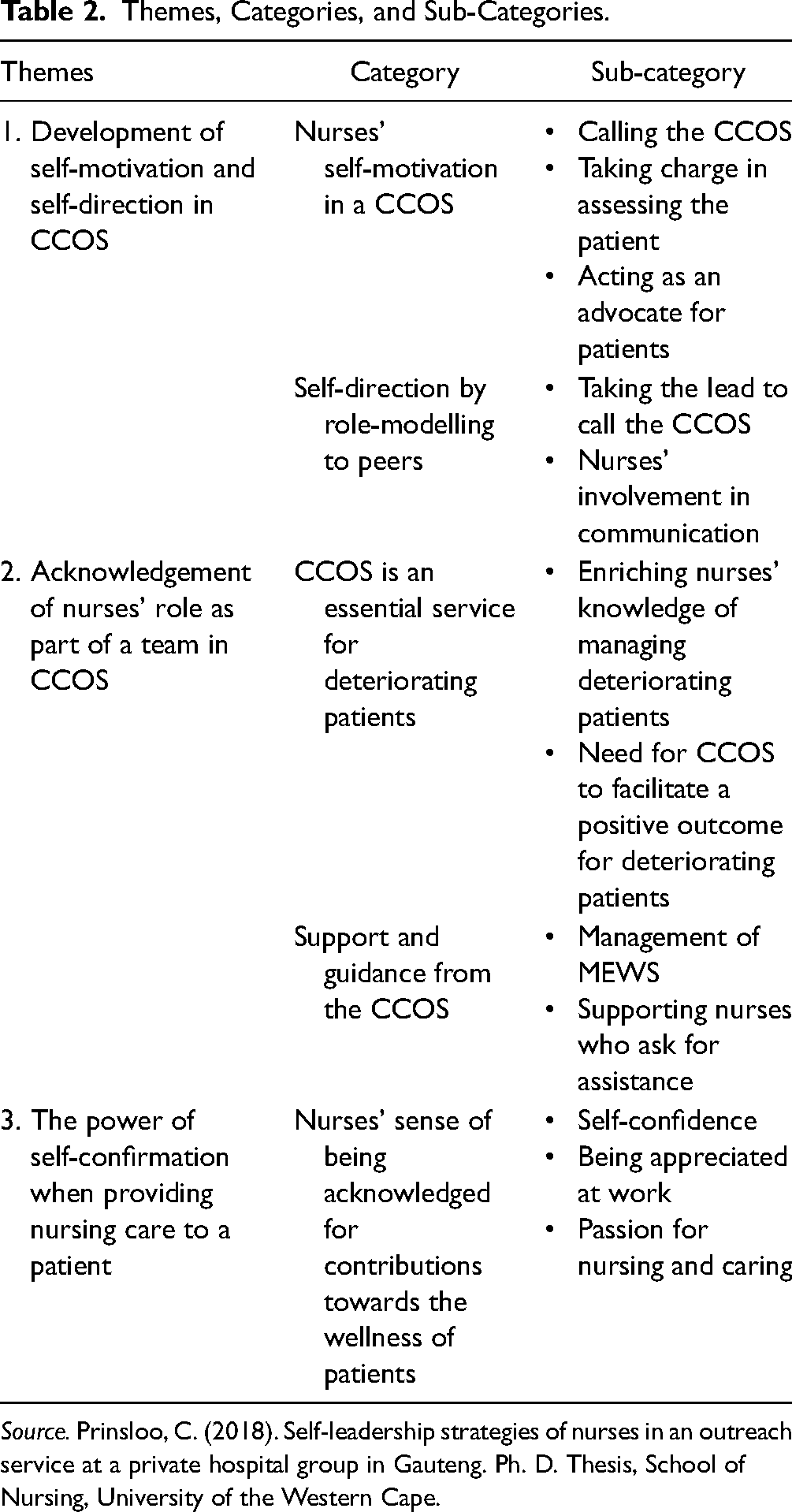
Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. Ph. D. Thesis, School of Nursing, University of the Western Cape.
Theme 1: Development of Self-Motivation and Self-Direction in CCOS
The nurses described how behaviour-focused strategies helped them to become more motivated to act on their own in contacting CCOS: ‘We’re very observant, you do observations, you monitor them, are they normal or abnormal? Then you can see what the next step is you can take …’ (Focus group discussion (FGD) 1; Participant (P) 4).
It could be concluded that the nurse is internally debating (self-evaluating) the next course of action after the calculation of a MEWS score. The nurses utilise the MEWS as a cue to decide whether the patient is in danger of worsening and whether it is necessary to contact the CCOS (Neck et al., 2020).
A participant exhibited self-leadership when she realised she lacked the skills necessary to give a deteriorating patient the proper nursing care after engaging in self-observation (behaviour). She used self-motivation when she acts as an advocate for the patient in contacting the CCOS when she required assistance in an emergency: ‘… when you don’t know any more what to do for this patient, you pick up the phone, “Sister (referring to CCOS), come help me please”. That is nice to know because you don’t know everything, you try up to a point … Then you just phone, “Sister …”’ (FGD2; P4).
Theme 2: Acknowledgement of Nurses’ Role as Part of a Team in CCOS
Participants describe their roles in the CCOS: ‘My concern is to take care of the patient, to make sure that the patient's condition is okay. If I see the patient is complicating and the condition is not, is unstable, then I have to report to the sister …’ (FGD8; P1).
The participant indicated how she sets goals in nursing her patients. In general, goals that are detailed, challenging, yet attainable, are helpful at controlling our immediate behaviour. The most effective and motivating goals are usually those that are realistic and attainable. Achieving such goals can be incredibly satisfying (Neck et al., 2020).
A participant described how she used MEWS as a cue to take care of her patient. Using the MEWS as a cue to guide your behaviour may improve the quality of care a patient receives and the patient's outcome: ‘I think I can say with this thing of the MEWS score; it makes our life more easier. Because you can say you can see at the chart that when the patient MEWS score is like, let's say, 5, you can see that this patient is really in serious trouble, so you need to activate CCOS’ (FGD5; P1).
Participants described their need for support from CCOS: ‘There is somebody that you can call if you really need help or support for a patient because we all are RNs, and most of us actually know really. We know what to do when we are worried about a patient, but it is always nice to have somebody that you can call that has a little bit more knowledge and can support you’ (FGD1; P4).
Nurses practice constructive thought patterns when they visualise the successful care of a deteriorating patient with the assistance of the CCOS. Van Wart (2015) states that constructive thought patterns include mental imagery of successful execution outcomes. ‘So it is very, very important for outreach sister [referring to the CCOS] to be there and to guide because if you don’t know what signs to look for, the outreach sister can always say, “Look out for this, look out for that,” so she is a very important guide for us’ (FGD 4; P1).
‘… the outreach service – very good, and it's improving, because what I am saying it improves the lives of the patients …’ (FGD6; P4).
The CCOS support and assistance in the management of deteriorating patients increase nurses’ knowledge of managing deteriorating patients. It seems that participants practised self-determination assessing their knowledge managing deteriorating patients and focused on the pleasant aspects when they take care of a deteriorating patient which can be seen as natural rewarding for them. Natural reward strategies, according to Neck et al. (2020), are intended to support feelings of competence and self-determination, which in turn promote performance-improving, task-related behaviours.
Theme 3: The Power of Self-Confirmation When Providing Nursing Care to a Patient
According to the self-confirmation theory, motivation arises from a positive self-image (Carrol et al., 2015, p. 268). The results indicated that CCOS contributed to a sense of self-confidence in nurses: ‘… and also comes a lot of confidence and passion for what you are doing when you feel that that patient, you are the one who is close to that patient, you are the one who assists the patient …’ (FGD7; P4).
According to Neck et al. (2020) natural reward strategies come after the positive experience of task completion and achieving goals.
Research Question 2
The conceptual framework was developed according to an adapted method of Jabereen (2009), while the practice-oriented theory of Dickoff et al. (1968) was used as the framework for the conceptual framework. The findings of the focus group discussions led to conclusions that were integrated into the conceptual framework. The concepts identified from the focus group findings were organised and categorised according to the main components in the survey list of Dickoff et al. (1968). This list provided answers to six key questions about self-leadership of nurses, which constituted the reasoning map for describing the conceptual framework.
Research Question 3
This conceptual framework was used to create the questionnaire, which covered the strategies that nurses apply to lead them to activate the CCOS. The nurse managers’ perceptions of nurses initiating self-leadership activities in a CCOS were explored. The participants’ ages ranged from 30 to 63. The majority were between the ages of 40 and 44. A little more than half of the participants had worked as nurse managers for more than 6 years, and 50% held a nursing management degree. Nearly a third of the nurse managers said there were no intentions to adopt the CCOS in their hospital, while just over half of them (54.1%) said that the CCOS was available in their facilities. The factor analysis extracted eight factors (Table 3).
Factors Extracted.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Research Question 4
The results from the quantitative analysis were used to develop the strategies. The following criteria were used to develop the strategies:
The two items with the highest loads for each factor Agreement and total agreement of 80% or more on the items in a factor Mean values of 3.8 and lower on items in a factor Items with an SD of 1.0 or less
As mentioned in the research design, Neck and Milliman's (1994) strategic framework was adapted to develop strategies.
Five strategies were developed, relating to self-motivation, role models, patient outcomes, assistance and guidance from CCOS, and the power of self-confirmation. The objectives and activities for these strategies were derived from the findings of the quantitative data analysis, which was used to build them. Objectives concerning self-leadership, with recommended activities outlining each strategy, were developed. Each of these activities was directed at facilitating nurses’ self-leadership in CCOS with the intention of improving the deteriorating patient's outcome in a private healthcare organisation in Gauteng. Several role-players are responsible for implementing these activities, namely the healthcare organisation, human resources, managers, senior nurses and the nurse in the nurse-led CCOS.
Facilitation of Self-Motivation
The two factors of self-motivation and authority extracted from the factor analysis were used to develop objectives. Table 4 indicates objectives and suggested activities that focus on increasing self-motivation among nurses to achieve self-leadership in CCOS.
Activities to Increase Self-Motivation.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Role Models Among Nurses
This strategy aims to empower nurses to become role models and to lead by example in acquiring self-leadership in CCOS. The two factors extracted from the factor analysis, namely role modelling and knowledge, were used to develop the objectives for this strategy. Table 5 provides the objectives and activities for empowering nurses to become role models.
Activities to Empower Nurses to Become Role Models.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Improving Patient Outcomes
This strategy intends to improve patient outcomes by improving the quality of nursing care. The factors of competence and self-determination among nurses were used to develop objectives. Table 6 provides the objectives and activities to improve patient outcomes.
Activities to Improve Patient Outcome.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Assistance and Guidance from CCOS
The strategy of assistance and guidance from CCOS aims to empower nurses to engage in self-leading behaviours. Table 7 outlines the objectives and activities that stem from the assistance, guidance and responsibility extracted from the factor analysis.
Facilitation of Assistance and Guidance from CCOS.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Power of Self-Confirmation
The factor analysis yielded only one factor, namely power of self-confirmation. Table 8 outlines the objective and activities to facilitate self-confirmation among nurses.
Creating Self-Confirmation Among Nurses.

Source. Prinsloo, C. (2018). Self-leadership strategies of nurses in an outreach service at a private hospital group in Gauteng. PhD. Thesis, School of Nursing, University of the Western Cape.
Discussion
The intention of this study was to develop strategies to facilitate self-leadership among nurses in a CCOS working at a private healthcare organisation. The study drew from the definition of self-leadership namely: Self-leadership is the process of influencing oneself to establish the self-direction and self-motivation needed to perform (Neck et al., 2020). It is clearly demonstrated that self-leadership aids persons in developing personal effectiveness through three kinds of individual action, namely behaviour-focused activities, natural reward acts and constructive thought patterns (Van Wart, 2015). The themes derived from the qualitative data showed that all three forms of self-leadership actions were present. The results of the quantitative data were used to develop the strategies which related to self-motivation, role models, patient outcomes, assistance and guidance from the CCOS and the power of self-confirmation.
Pramilaa (2016) states that self-motivation is the method a person employs to find the motivation to establish goals and use strategies to keep themselves on track to follow these goals. In addition, Deci et al. (2017) state that self-motivation is the spontaneous experience of interest and enjoyment in the activity that supplies rewards. The self-determination theory indicates that the need for self-determination and competence are key processes for enhancing self-motivation derived from a task or activity (Neck et al., 2020). Positive self-talk increases motivation, effort and positive attitude (Heggebo, 2015) and is considered self-regulatory, where self-talk is used deliberately to enhance confidence (Theodarakis et al., 2008). A significant component of self-leadership is the capability to motivate oneself to do what is needed for the accomplishment of tasks, such as measuring a patient's vital data and calculating their MEWS. A nurse needs to be self-motivated to nurse a patient at risk of deteriorating, thus displaying their self-driven effort to provide such a patient with appropriate nursing care. Self-leadership provides employees with more responsibility, autonomy and control over the work process, while still permitting management guidance, such as empowering actions from the leader, to create intrinsic rewards (Kokemuller, 2018).
A role model acts as an example, inspiring people with integrity, determination and compassion (Price-Mitchell, 2017). Nurses, as role models in CCOS, can motivate other nurses. Role modelling by nurses in leadership positions demonstrates the expected standards and helps build capacity in nursing practice (Christenbery, 2018). Role modelling is important to motivate nurses to behave to the best of their capability and training and to make decisions that positively affect patient outcomes (Thomas, 2018). In self-leadership behaviour, focused approaches are demonstrated when nurses, as role models for colleagues, increase the probability that their colleagues will complete tasks and face new challenges positively (Kranabetter & Niessen, 2017). As role models, nurses focus on their behaviour and may change it positively.
Nurses spend considerable time with patients in providing nursing care and they thereby influence patient outcomes. Nurses provide nursing care for patients in the form of monitoring patients’ vital data and administrating medication. Self-efficacy among nurses can be seen in their own belief that they have the required knowledge and skills to meet goals such as improving patients’ outcomes (Ayub et al., 2017). In addition, seminal authors Neck and Milliman (1994) state that self-leadership makes individual goals and tasks clear to initiate performance towards quality care. According to Neck et al. (2020), self-leadership involves the ability to develop yourself through self-influence, which leads to better performance and effectiveness in the work setting.
The CCOS assists and guides nurses in the management of patients who start to deteriorate, which, in turn, empowers nurses in the management of these patients. According to Maharaj et al. (2015), CCOS is associated with the reduction of mortality and cardiopulmonary arrest in hospitals, while Jeddian et al. (2017) state that CCOS improves nurses’ knowledge in providing nursing care to a deteriorating patient.
The data revealed that showing nurses appreciation makes them feel proud. The enjoyable and fulfilling feelings of self-confirmation experienced by nurses create feelings of competence. In self-leadership, natural reward strategies focus on the positive experience associated with a task done well (Neck et al., 2020).
Limitations
As CCOS are not widely implemented in South Africa, implementation of these strategies is limited. The study setting was limited to one private hospital group, which could affect the generalisability of the study.
Implications for Practice
Exploring nurses’ self-leadership in CCOS and developing strategies to facilitate self-leadership among ward nurses in a CCOS is a new area of research and will contribute to the literature of self-leadership and CCOS. Practising self-leadership has a positive effect on job performance (Kayral & Dulger, 2019) and may influence nurses to follow the guidelines for activating CCOS. The study offers insight into the concept of self-leadership in the context of CCOS in a private healthcare setting. The implementation of self-leadership among nurses could benefit nursing practice, as nurses would be empowered to lead themselves. The improvement of patient outcomes is another possibility, as nurses would be competent to provide quality nursing care to deteriorating patients.
Conclusions
There is a need for self-leadership among nurses. Self-leading nurses will motivate themselves to be proactive in managing deteriorating patients and will have the confidence to provide nursing care to deteriorating patients.
Institutional Review Board Approval
The study was approved by the Research Ethics Committee (ethical clearance number 12/7/6) of the institution and the Research Operational Committee of the private hospital group (approval number UNIV-2013-007B). Participants were invited to participate in the study. An informational letter about the study and a consent letter were distributed to potential participants. The participants were informed that participation was voluntary, that they had the right to withdraw at any time and that all information would be treated as confidential.
Footnotes
Acknowledgements
The author would like to thank the study participants and the private hospital group for their participation in the study. She would also like to express her gratitude to the National Research Foundation (NRF) for its financial assistance and to the University of the Western Cape for their academic support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Received funding from the National Research Foundation (NRF) South Africa.
